GI — MCQs

On this page
A 52-year-old man, with a history of alcoholism, presents with loss of appetite, abdominal pain, and fever for the past 24 hours. He says he consumed 12 beers and a bottle of vodka 2 days ago. He reports a 19-year history of alcoholism. His blood pressure is 100/70 mm Hg, pulse is 100/min, respirations are 20/min, and oxygen saturation is 99% on room air. Laboratory findings are significant for the following: Sodium 137 mEq/L Potassium 3.4 mEq/L Alanine aminotransferase (ALT) 230 U/L Aspartate aminotransferase (AST) 470 U/L Which of the following histopathologic findings would most likely be found on a liver biopsy of this patient?
A 25-year-old woman presents to her primary care physician complaining of several months of diarrhea. She has also had crampy abdominal pain. She has tried modifying her diet without improvement. She has many watery, non-bloody bowel movements per day. She also reports feeling fatigued. The patient has not recently traveled outside of the country. She has lost 10 pounds since her visit last year, and her BMI is now 20. On exam, she has skin tags and an anal fissure. Which of the following would most likely be seen on endoscopy and biopsy?
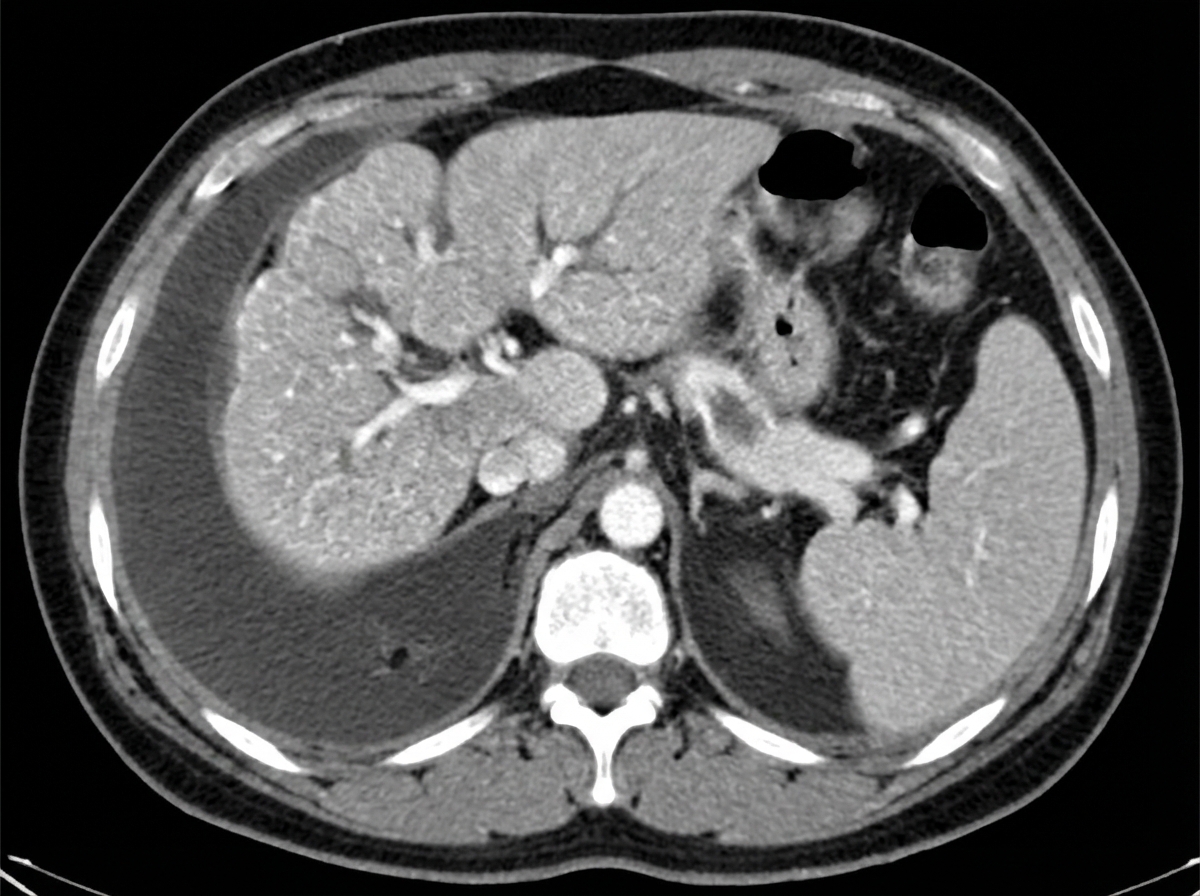
A 65-year-old man is brought to the emergency department because of a 1-day history of fever and disorientation. His wife reports that he had abdominal pain and diarrhea the previous day. He drinks 60 oz of alcohol weekly. His pulse is 110/min and blood pressure is 96/58 mm Hg. Examination shows jaundice, palmar erythema, spider nevi on his chest, dilated veins on the anterior abdominal wall, and 2+ edema of the lower extremities. The abdomen is soft and diffusely tender; there is shifting dullness to percussion. His albumin is 1.4 g/dL, bilirubin is 5 mg/dL, and prothrombin time is 31 seconds (INR = 3.3). Hepatitis serology is negative. A CT scan of the abdomen is shown. Which of the following processes is the most likely explanation for these findings?
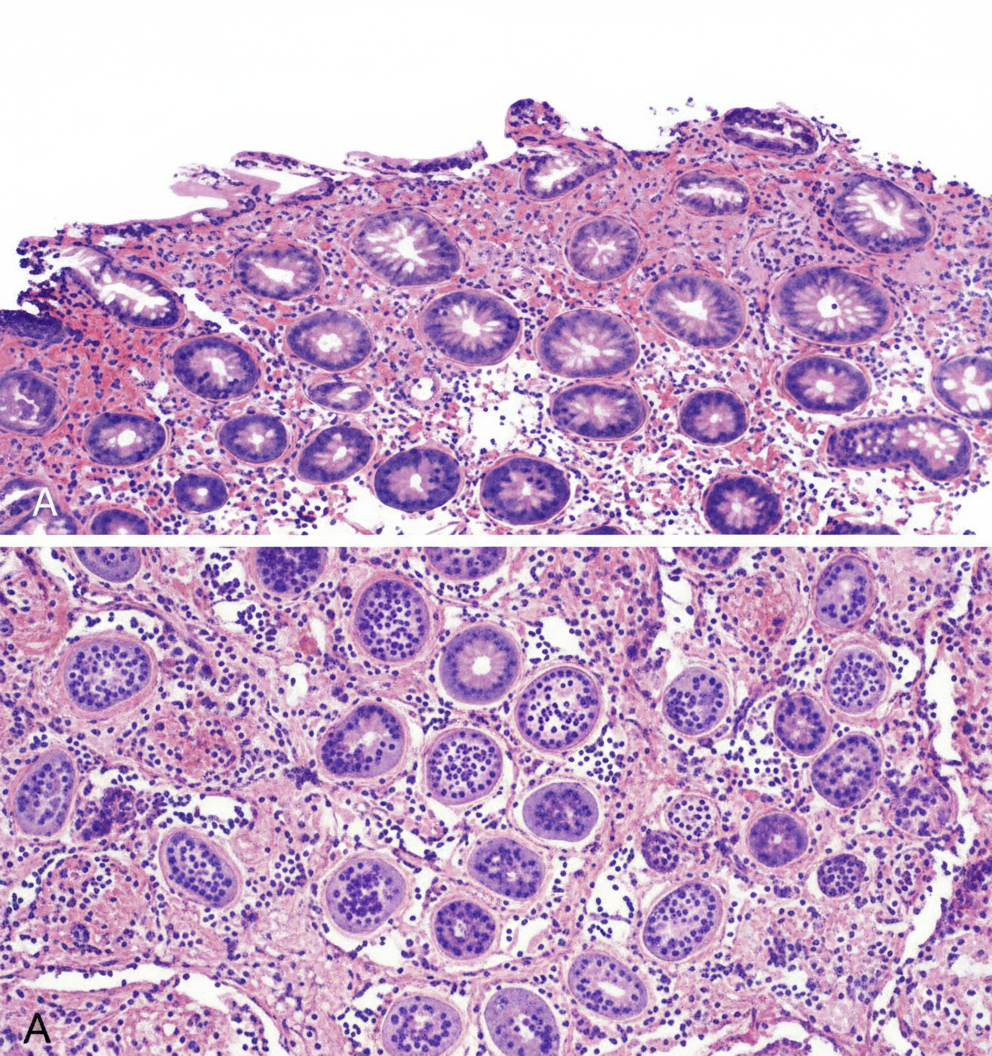
An esophageal biopsy sample from a 47-year-old male with chronic heartburn reveals intestinal metaplasia. Which of the following abnormal cell types is likely present in this patient's esophagus?
A 21-year-old man comes to the physician because of a 6-month history of severe abdominal pain, bloating, and episodic diarrhea. He has also had a 5-kg (11-lb) weight loss during this time. Physical examination shows a mildly distended abdomen, hyperactive bowel sounds, and diffuse abdominal tenderness. A biopsy specimen of the colonic mucosa shows scattered areas of inflammation with fibrosis and noncaseating granulomas. Which of the following is most likely involved in the pathogenesis of this patient's condition?
A previously healthy 35-year-old woman comes to the physician for a 3-week history of alternating constipation and diarrhea with blood in her stool. She has not had any fevers or weight loss. Her father died of gastric cancer at 50 years of age. Physical examination shows blue-gray macules on the lips and palms of both hands. Colonoscopy shows multiple polyps throughout the small bowel and colon with one ulcerated polyp at the level of the sigmoid colon. Multiple biopsy specimens are collected. These polyps are most likely to be characterized as which of the following histological subtypes?
A 27-year-old woman presents to her primary care physician for evaluation of involuntary weight loss and recurrent abdominal pain. She noticed blood in her stool several times. The medical history is significant for the polycystic ovarian syndrome. The vital signs are as follows: temperature, 38.0°C (100.4°F); heart rate, 78/min; respiratory rate, 14/min; and blood pressure, 110/80 mm Hg. The family history is notable for paternal colon cancer. A colonoscopy is performed and is presented in the picture. What findings are expected?
A 51-year-old man presents to his primary care physician's office for a 6-week history of fatigue and diarrhea. He says that the diarrhea is frequent, small volume, and contains gross blood. Review of systems is significant for subjective fever and an unintentional 5-pound weight loss. He denies recent travel outside of the United States. His past medical history is significant for IV drug abuse, HIV infection with non-compliance, and osteoarthritis. His family history is significant for Crohn disease in his mother. His temperature is 100.7°F (38.2°C), pulse is 90/min, blood pressure is 129/72 mmHg, and respirations are 16/min. His abdominal exam shows mild right and left lower quadrant tenderness with no rebound or guarding. Laboratory results are significant for a CD4 count of 42/mm^3. Colonoscopy with tissue biopsy will most likely reveal which of the following?
A 65-year-old man comes to the physician because of abdominal pain and bloody, mucoid diarrhea for 3 days. He has been taking over-the-counter supplements for constipation over the past 6 months. He was diagnosed with type 2 diabetes mellitus 15 years ago. He has smoked one pack of cigarettes daily for 35 years. His current medications include metformin. His temperature is 38.4°C (101.1°F), pulse is 92/min, and blood pressure is 134/82 mm Hg. Examination of the abdomen shows no masses. Palpation of the left lower abdomen elicits tenderness. A CT scan of the abdomen is shown. Which of the following is the most likely underlying cause of the patient's condition?
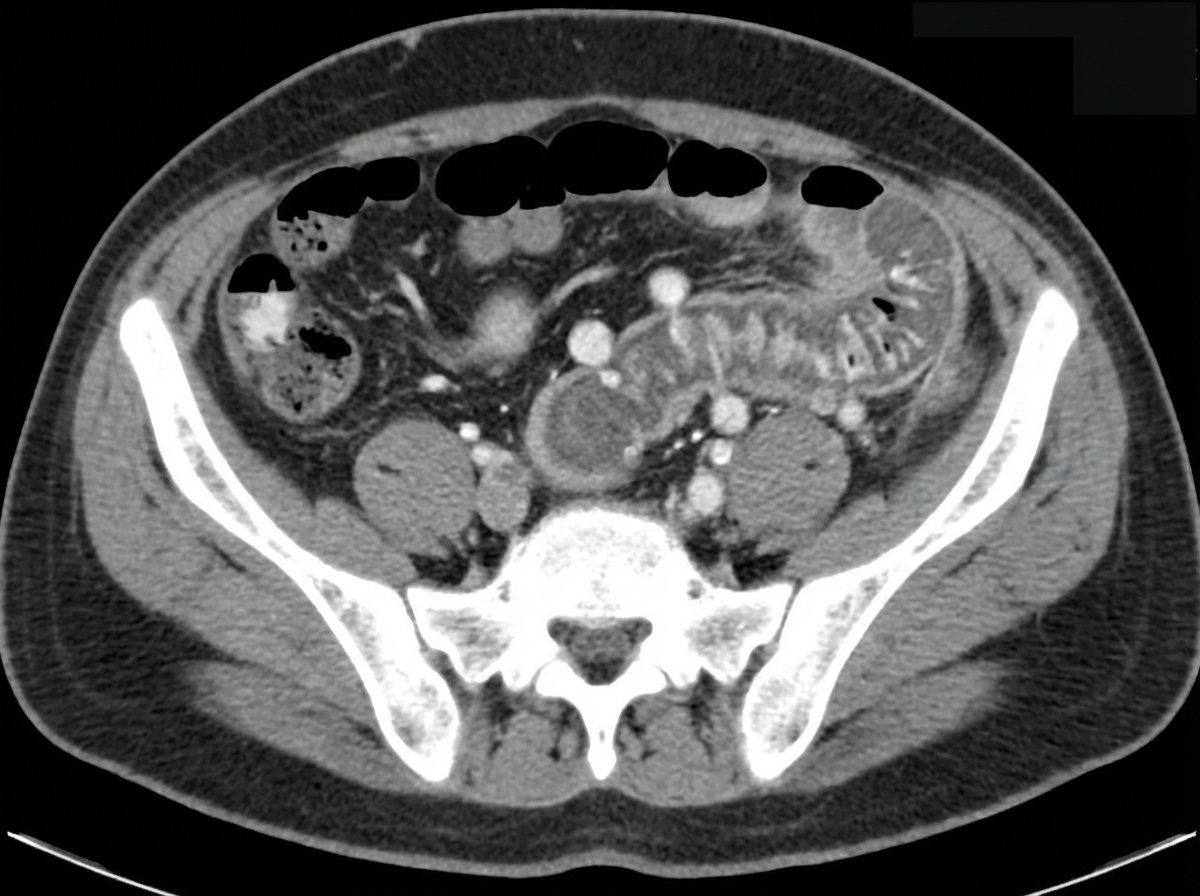
A 24-year-old woman comes to the physician because of progressively worsening episodes of severe, crampy abdominal pain and nonbloody diarrhea for the past 3 years. Examination of the abdomen shows mild distension and generalized tenderness. There is a fistula draining stool in the perianal region. Immunohistochemistry shows dysfunction of the nucleotide oligomerization binding domain 2 (NOD2) protein. This dysfunction most likely causes overactivity of which of the following immunological proteins in this patient?
Practice by Chapter
Esophageal pathology
Practice Questions
Gastritis and peptic ulcer disease
Practice Questions
Gastric tumors
Practice Questions
Malabsorption syndromes
Practice Questions
Inflammatory bowel diseases
Practice Questions
Intestinal infections
Practice Questions
Diverticular disease
Practice Questions
Vascular disorders of bowel
Practice Questions
Colon polyps and neoplasms
Practice Questions
Appendicitis
Practice Questions
Peritonitis
Practice Questions
Hernia complications
Practice Questions
Gastrointestinal stromal tumors
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
