Vascular disorders of skin — MCQs

A 76-year-old woman is brought to the physician because of lesions on her left arm. She first noticed them 3 months ago and they have grown larger since that time. She has not had any pain or pruritus in the area. She has a history of invasive ductal carcinoma of the left breast, which was treated with mastectomy and radiation therapy 27 years ago. Since that time, she has had lymphedema of the left arm. Physical examination shows extensive edema of the left arm. There are four coalescing, firm, purple-blue nodules on the left lateral axillary region and swelling of the surrounding skin. Which of the following is the most likely diagnosis?
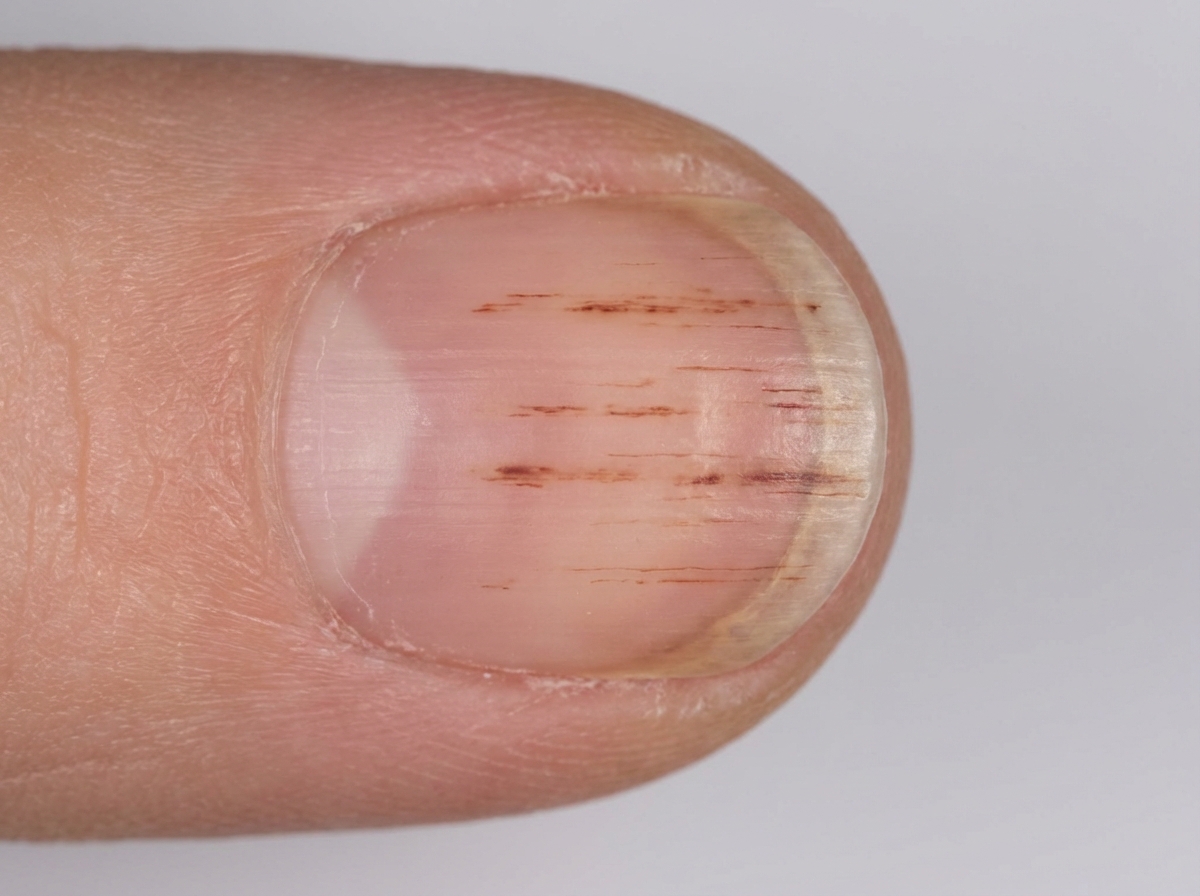
A 62-year-old man comes to the physician for a 1-month history of fever, malaise, and skin rash. He has had a 5-kg (11-lb) weight loss during this period. He does not smoke, drink alcohol, or use illicit drugs. He appears pale. His temperature is 39.1°C (102.3°F), pulse is 110/min, and blood pressure is 140/85 mm Hg. Physical examination shows nontender, erythematous macules on the palms and soles. A photograph of one of his fingernails is shown. Microscopic examination of the nail lesion is most likely to show which of the following?
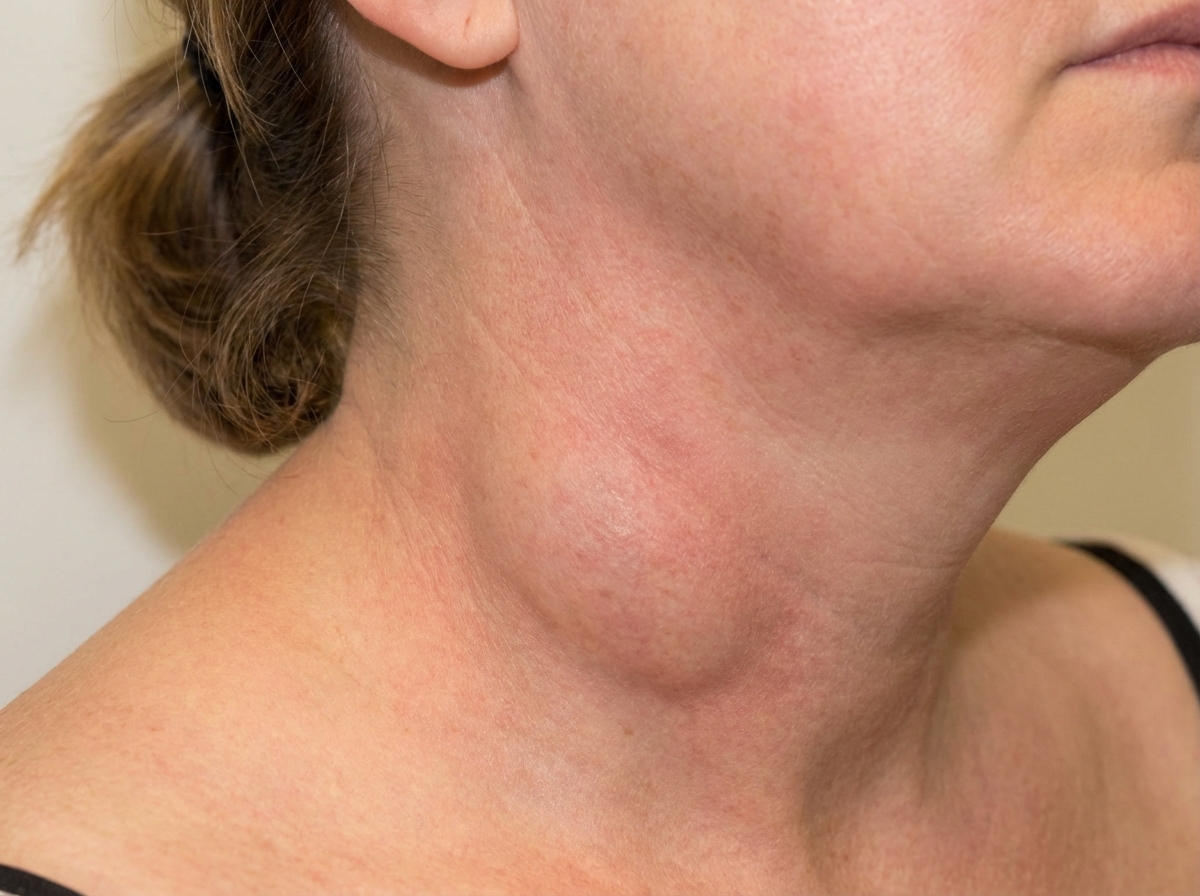
A 42-year-old woman presents because of a painful mass she first noticed on her neck 1 week ago (see image). The mass has grown over the last few days. She has no history of serious illness and takes no medications. On physical exam, her temperature is 38.0°C (100.4°F), pulse is 86/min, respirations are 12/min, blood pressure is 135/80 mm Hg. The mass is tender and relatively soft and mobile. The overlying skin is warm. On her right ear, there is a series of small and healing skin punctures left by the bite of her neighbor's kitten 3 weeks ago. No other mass is detected in the neck, supraclavicular, axillary, or inguinal regions. Oral examination reveals several discolored teeth. Her lungs are clear to auscultation and heart sounds are normal. A biopsy of the neck mass is performed. Which of the following would be most useful in establishing the diagnosis?
A 45-year-old man comes to the emergency department because of chills and numerous skin lesions for 1 week. He has also had watery diarrhea, nausea, and abdominal pain for the past 2 weeks. The skin lesions are nonpruritic and painless. He was diagnosed with HIV infection approximately 20 years ago. He has not taken any medications for over 5 years. He sleeps in homeless shelters and parks. Vital signs are within normal limits. Examination shows several bright red, friable nodules on his face, trunk, extremities. The liver is palpated 3 cm below the right costal margin. His CD4+ T-lymphocyte count is 180/mm3 (N ≥ 500). A rapid plasma reagin test is negative. Abdominal ultrasonography shows hepatomegaly and a single intrahepatic 1.0 x 1.2-cm hypodense lesion. Biopsy of a skin lesion shows vascular proliferation and abundant neutrophils. Which of the following is the most likely causal organism?
A 93-year-old woman is brought to the physician because of a purple area on her right arm that has been growing for one month. She has not had any pain or itching of the area. She has hyperlipidemia, a history of basal cell carcinoma treated with Mohs surgery 2 years ago, and a history of invasive ductal carcinoma of the right breast treated with radical mastectomy 57 years ago. She has had chronic lymphedema of the right upper extremity since the mastectomy. Her only medication is simvastatin. She lives in an assisted living facility. She is content with her living arrangement but feels guilty that she is dependent on others. Vital signs are within normal limits. Physical examination shows extensive edema of the right arm. Skin exam of the proximal upper right extremity shows three coalescing, 0.5–1.0 cm heterogeneous, purple-colored plaques with associated ulceration. Which of the following is the most likely diagnosis?
A 49-year-old man with HIV comes to the physician because of a 1-month history of intermittent diarrhea and abdominal pain. Abdominal examination shows mild, diffuse tenderness throughout the lower quadrants. His CD4+ T-lymphocyte count is 180/mm3 (normal ≥ 500/mm3). Colonoscopy shows multiple hemorrhagic nodules in the rectum and descending colon. Polymerase chain reaction of the lesions is positive for HHV-8. Histologic examination of the lesions is most likely to show which of the following findings?
Two weeks after undergoing low anterior resection for rectal cancer, a 52-year-old man comes to the physician because of swelling in both feet. He has not had any fever, chills, or shortness of breath. His temperature is 36°C (96.8°F) and pulse is 88/min. Physical examination shows a normal thyroid and no jugular venous distention. Examination of the lower extremities shows bilateral non-pitting edema that extends from the feet to the lower thigh, with deep flexion creases. His skin is warm and dry, and there is no erythema or rash. Microscopic examination of the interstitial space in this patient's lower extremities would be most likely to show the presence of which of the following?
A 28-year-old man presents for severe abdominal pain and is diagnosed with appendicitis. He is taken for emergent appendectomy. During the procedure, the patient has massive and persistent bleeding requiring a blood transfusion. The preoperative laboratory studies showed a normal bleeding time, normal prothrombin time (PT), an INR of 1.0, and a normal platelet count. Postoperatively, when the patient is told about the complications during the surgery, he recalls that he forgot to mention that he has a family history of an unknown bleeding disorder. The postoperative laboratory tests reveal a prolonged partial thromboplastin time (PTT). Which of the following is the most likely diagnosis in this patient?
A previously healthy 4-year-old boy is brought to the emergency department because of a 1-day history of pain and swelling of his left knee joint. He has not had any trauma to the knee. His family history is unremarkable except for a bleeding disorder in his maternal uncle. His temperature is 36.9°C (98.4°F). The left knee is erythematous, swollen, and tender; range of motion is limited. No other joints are affected. An x-ray of the knee shows an effusion but no structural abnormalities of the joint. Arthrocentesis is conducted. The synovial fluid is bloody. Further evaluation of this patient is most likely to show which of the following findings?
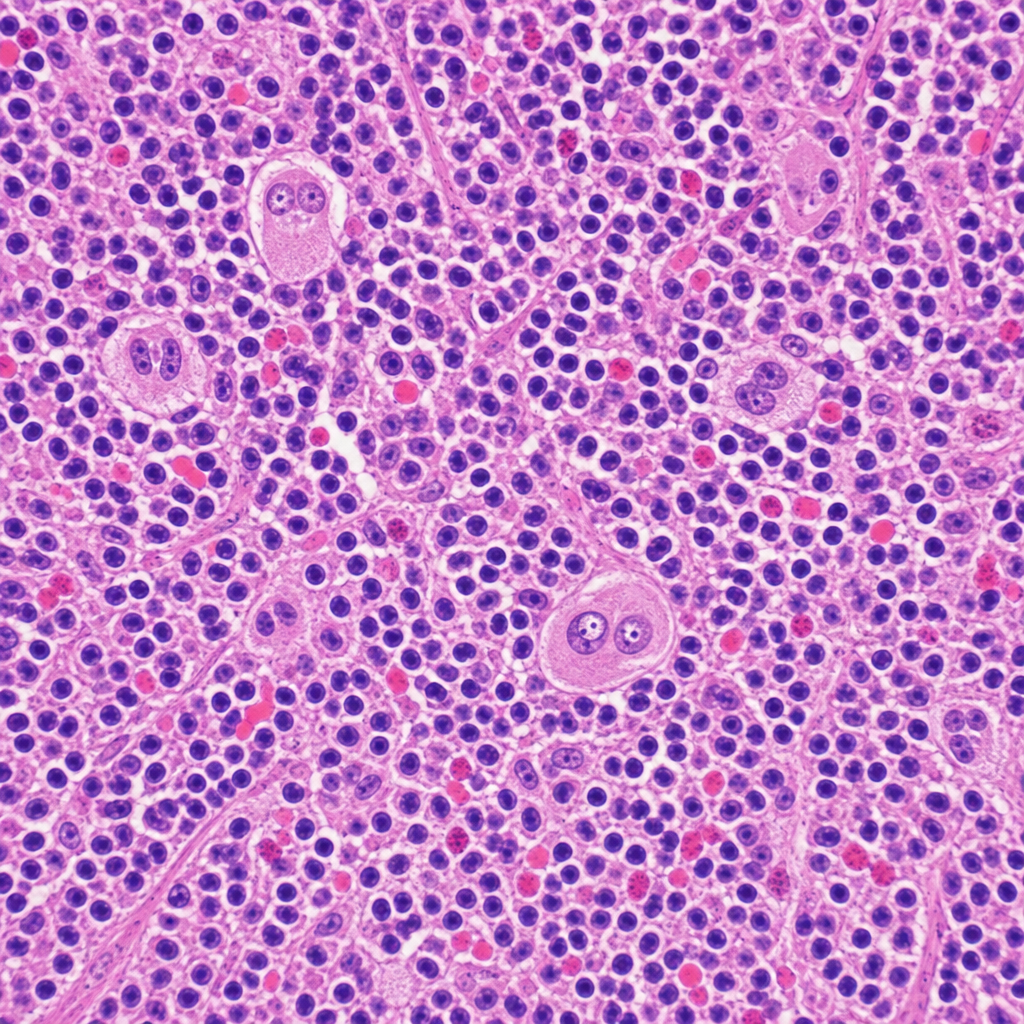
A 34-year-old woman presents with fatigue, night sweats, and a painless cervical lymph node mass for 3 months. Excisional biopsy of the lymph node is performed. The photomicrograph demonstrates a mixed cellular infiltrate with scattered large binucleated cells possessing prominent eosinophilic 'owl-eye' nucleoli, set against a background of lymphocytes, plasma cells, eosinophils, and fibroblasts. Immunohistochemical staining of the large cells is positive for CD15 and CD30 and negative for CD45. Which of the following best describes the cell of origin of the large binucleated cells seen in this lesion?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
