Panniculitis — MCQs

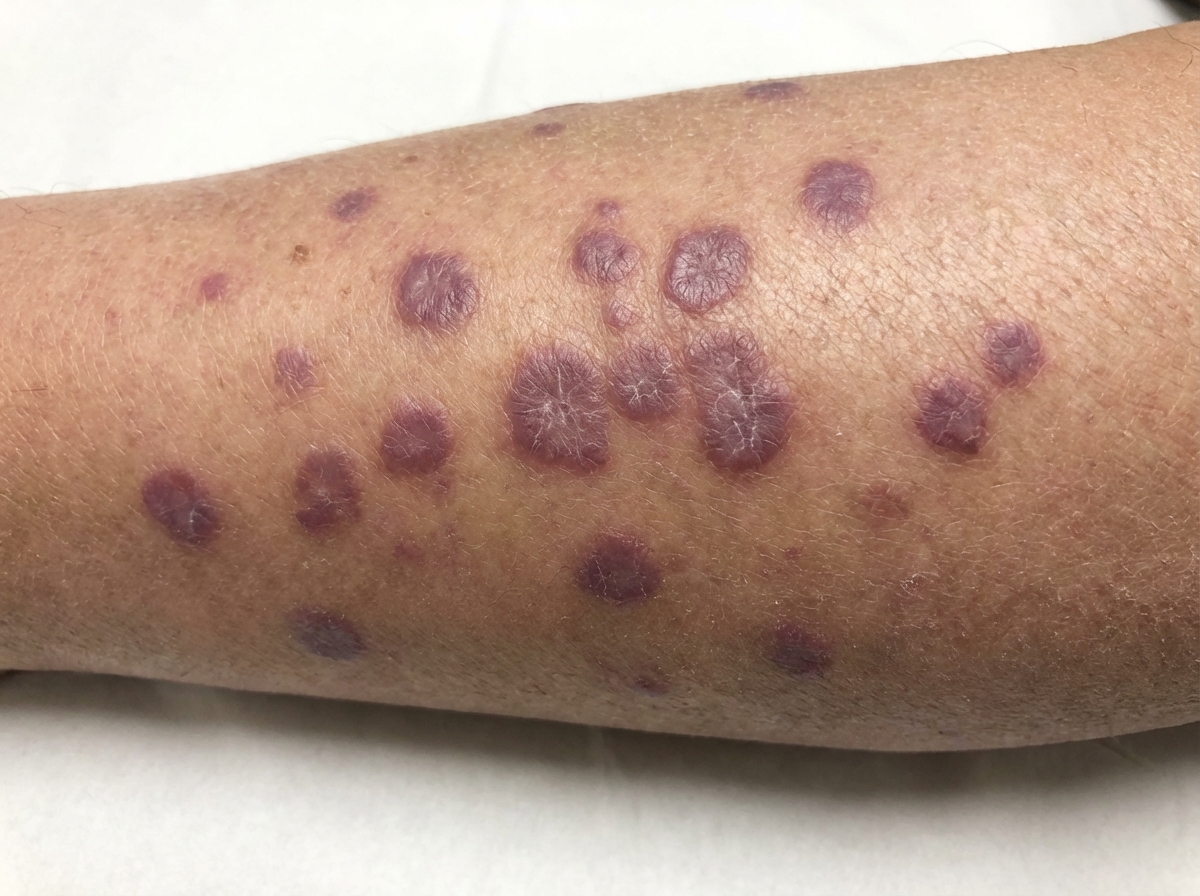
A previously healthy 46-year-old woman comes to her physician because of an itchy rash on her legs. She denies any recent trauma, insect bites, or travel. Her vital signs are within normal limits. Examination of the oral cavity shows white lace-like lines on the buccal mucosa. A photograph of the rash is shown. A biopsy specimen of the skin lesion is most likely to show which of the following?
A 55-year-old man is brought to the emergency room by his roommate due to an abdominal pain that started 2 hours ago. His pain is dull, aching, and radiates to the back. He admits to binge drinking alcohol for the past 2 days. Past medical history is significant for multiple admissions to the hospital for similar abdominal pain events, hypertension, and hyperlipidemia. He takes chlorthalidone and atorvastatin. He admits to heavy alcohol consumption over the past 10 years. He has smoked a pack of cigarettes a day for the last 20 years. In the emergency department, his temperature is 38.9℃ (102.0℉), pulse rate is 100/min, and respiratory rate is 28/min. On physical examination, he looks generally unwell and diaphoretic. Auscultation of his heart and lungs reveals an elevated heart rate with a regular rhythm. His lungs are clear to auscultation bilaterally. His abdomen is tympanitic with generalized tenderness. Evaluation of lab values reveals a leukocyte count of 28,000/mm3 with 89% of neutrophils. His amylase level is 255 U/L. A CT scan of the abdomen shows the diffuse enlargement of the pancreas. Which pathological process is most likely occurring in this patient’s peripancreatic tissue?
A 50-year-old Caucasian man is admitted to the ER with an 8-hour history of intense abdominal pain that radiates to the back, nausea, and multiple episodes of vomiting. Past medical history is insignificant. His blood pressure is 90/60 mm Hg, pulse is 120/min, respirations are 20/min, and body temperature is 37.8°C (100°F). Upon examination, he has significant epigastric tenderness, and hypoactive bowel sounds. Serum lipase and amylase are elevated and the patient rapidly deteriorates, requiring transfer to the intensive care unit for a month. After being stabilized, he is transferred to the general medicine floor with an abdominal computed tomography (CT) reporting a well-circumscribed collection of fluid of homogeneous density. Which of the following best describes the condition this patient has developed?
A 27-year-old school teacher visits her doctor because of disfiguring skin lesions that started to appear in the past few days. The lesions are mostly located on her chest, shoulders, and back. They are 2–5 mm in diameter, droplike, erythematous papules with fine silver scales. Besides a sore throat and laryngitis requiring amoxicillin several weeks ago, she has no significant medical history. What is the most likely diagnosis?
A 29-year-old man presents to the clinic complaining of fatigue and loss of sensation in his lower legs. The patient notes no history of trauma or chronic disease but states that he spends a lot of time outside and often encounters wild animals. On examination, the patient has multiple dark lesions over the skin of his face and back, as well as a decreased sensation of fine touch and vibration bilaterally in the lower extremities. What is the morphology of the etiologic agent causing this patient’s symptoms?
A 22-year-old woman presents with multiple tender, erythematous nodules on her shins that developed over the past week. She reports having a sore throat 2 weeks ago. She also complains of joint pain and fatigue. Physical examination reveals raised, red, tender nodules on the anterior surface of both legs. Her temperature is 38.2°C. Which of the following is the most likely diagnosis?
A 50-year-old female presents to her physician with vesicles and tense blisters across her chest, arms, and the back of her shoulders. Physical examination reveals that blistering is not present in her oral mucosa, and the epidermis does not separate upon light stroking of the skin. The patient most likely suffers from a hypersensitivity reaction located:
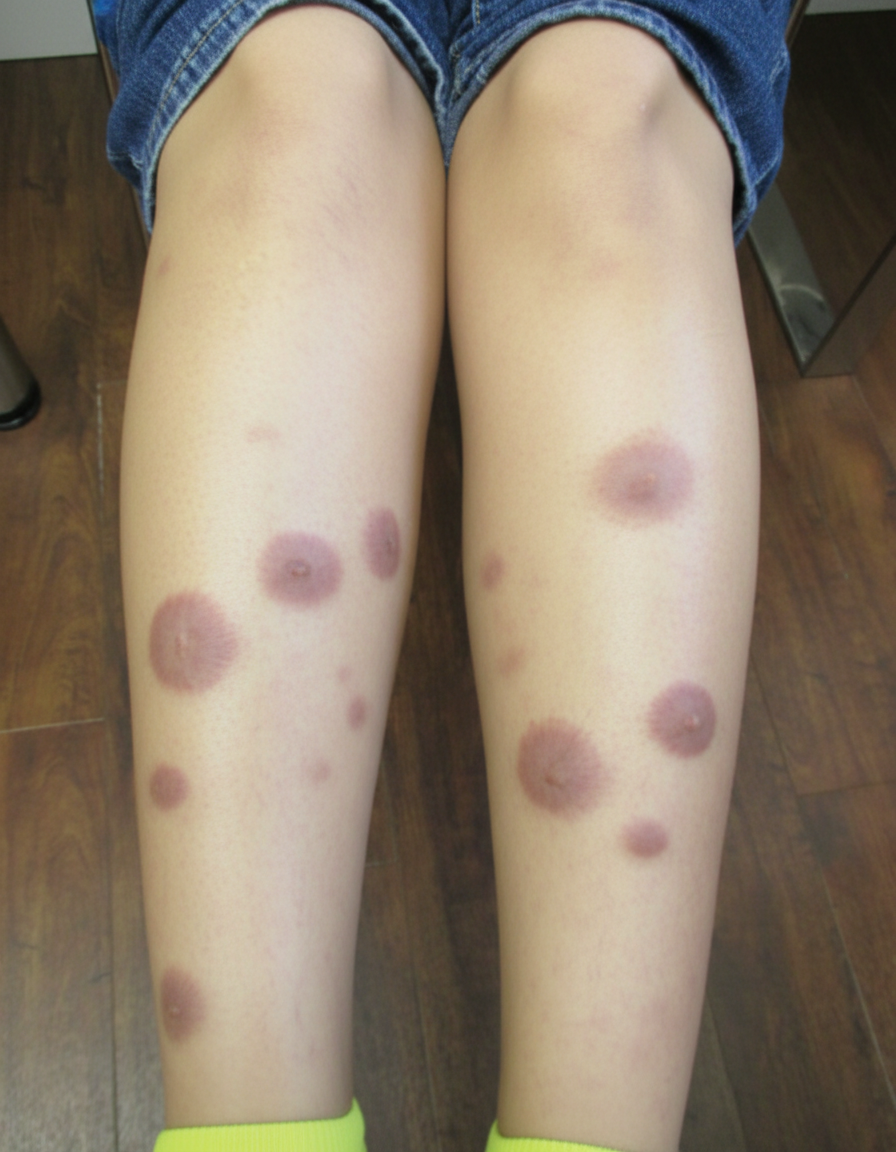
An otherwise healthy 28-year-old woman comes to the physician because of a 14-day history of painful red nodules on her legs associated with malaise and mild joint pains. She reports that the nodules were initially smaller and distinct but some have fused together over the past 3–4 days and now appear like bruises. There is no preceding history of fever, trauma, or insect bites. Her vital signs are within normal limits. A photograph of the tender lesions on her shins is shown. The remainder of the examination shows no abnormalities. Complete blood count and antistreptolysin O (ASO) titers are within the reference range. Erythrocyte sedimentation rate is 30 mm/h. Which of the following is the most appropriate next step in management ?
A 54-year-old man comes to the physician because of a cough with blood-tinged sputum for 1 week. He also reports fever and a 5-kg (11 lb) weight loss during the past 2 months. Over the past year, he has had 4 episodes of sinusitis. Physical examination shows palpable nonblanching skin lesions over the hands and feet. Examination of the nasal cavity shows ulceration of the nasopharyngeal mucosa and a depressed nasal bridge. Oral examination shows a painful erythematous gingival enlargement that bleeds easily on contact. Which of the following is the most likely cause of the patient's symptoms?
A 37-year-old woman presents to the occupational health clinic for a new employee health screening. She has limited medical records prior to her immigration to the United States several years ago. She denies any current illness or significant medical history. Purified protein derivative (PPD) is injected on the inside of her left forearm for tuberculosis (TB) screening. Approximately 36 hours later, the patient comes back to the occupational health clinic and has an indurated lesion with bordering erythema measuring 15 mm in diameter at the site of PPD injection. Of the following options, which is the mechanism of her reaction?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
