Dermatopathology — MCQs

On this page
The following skin biopsy from a patient of leprosy is diagnostic of: (Recent NEET Pattern 2016-17)
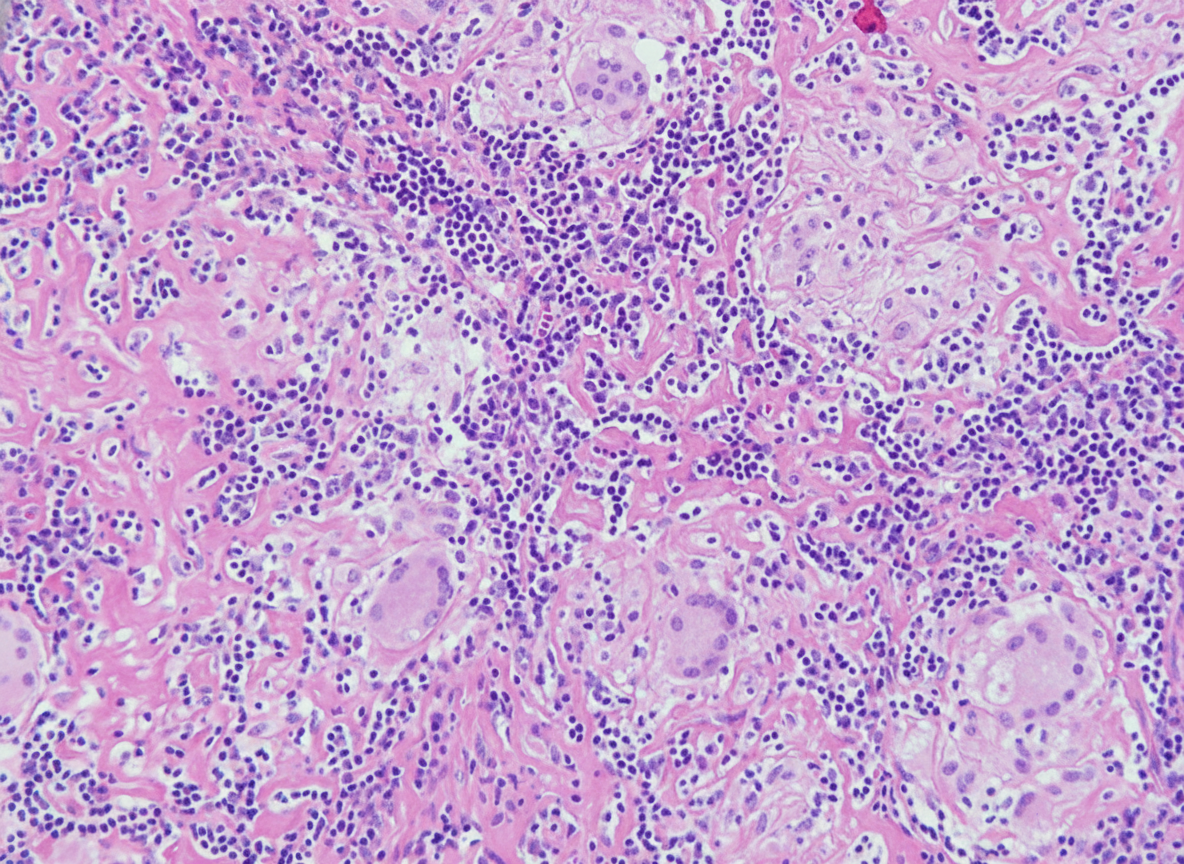
The following is a picture from scrapping of genital ulcer. Comment on the diagnosis. (AIIMS May 2017)
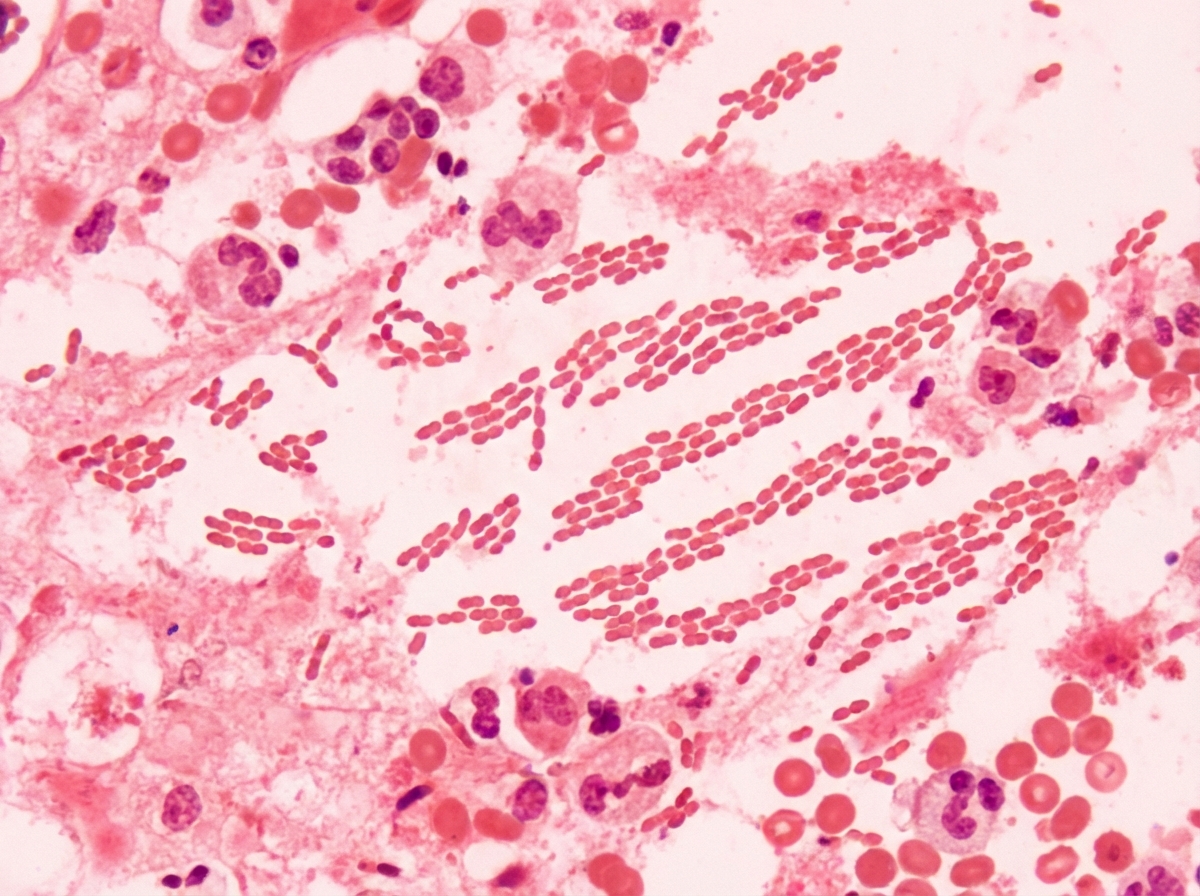
A 12-year-old boy develops multiple lumps in the skin. Biopsy of the lumps is shown below. What is the probable causative agent? (NEET Pattern 2019)
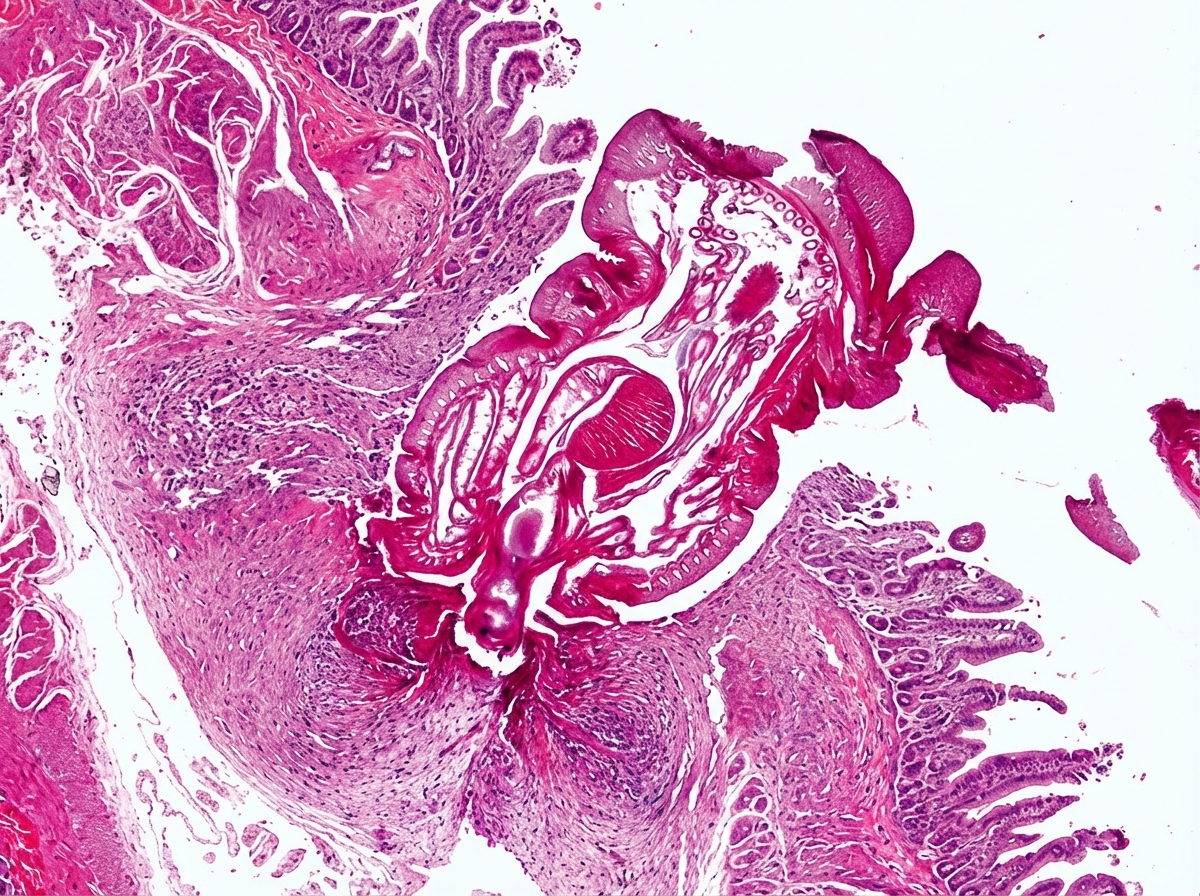
Identify the histopathological slide shown below:
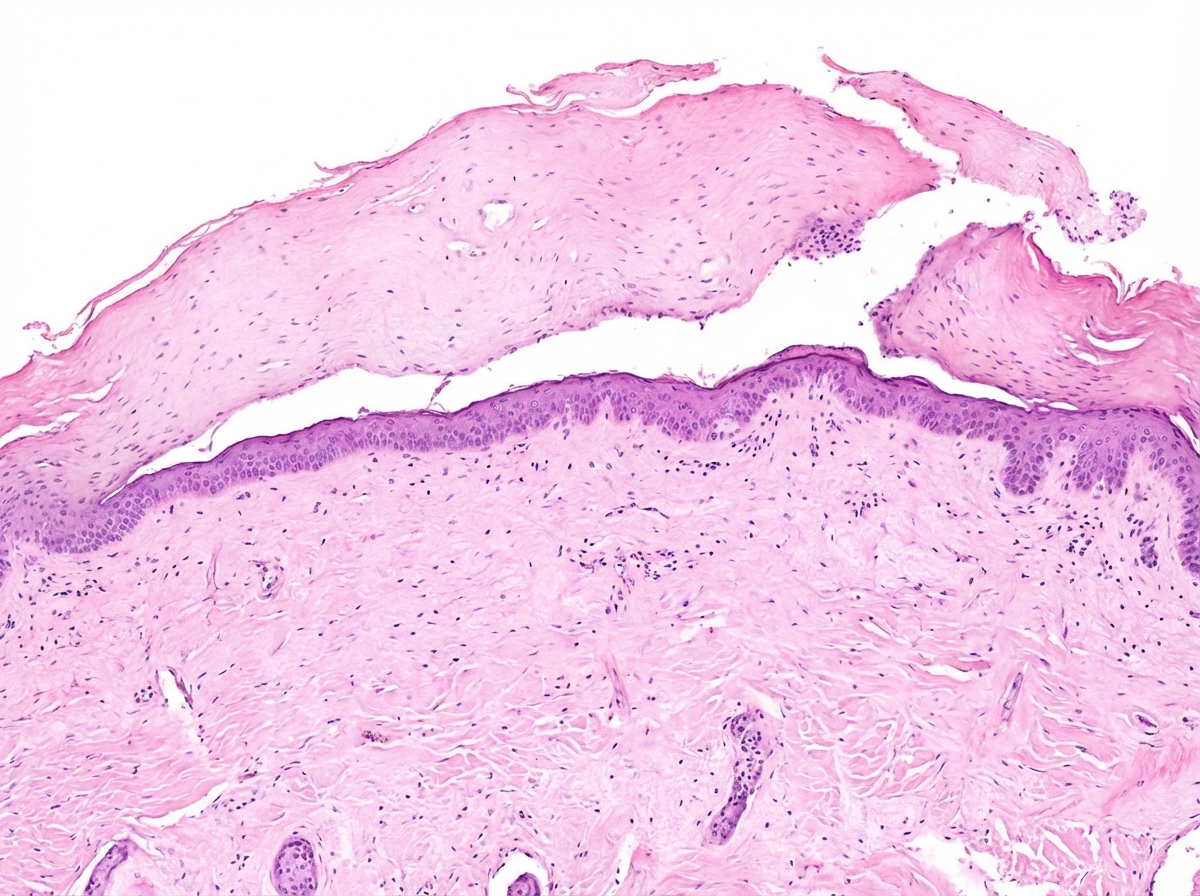
Practice by Chapter
Inflammatory dermatoses
Practice Questions
Vesiculobullous diseases
Practice Questions
Infectious skin diseases
Practice Questions
Benign epithelial tumors
Practice Questions
Premalignant skin lesions
Practice Questions
Non-melanoma skin cancers
Practice Questions
Melanocytic nevi
Practice Questions
Melanoma pathology
Practice Questions
Adnexal tumors
Practice Questions
Dermal tumors and proliferations
Practice Questions
Panniculitis
Practice Questions
Vascular disorders of skin
Practice Questions
Disorders of pigmentation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
