Types of necrosis (coagulative, liquefactive, etc.) — MCQs

An 87-year-old woman is admitted to the intensive care unit after a neighbor found her lying on the floor at her home. Her respirations are 13/min and shallow. Despite appropriate therapy, the patient dies. Gross examination of the brain at autopsy shows neovascularization and liquefactive necrosis without cavitation in the distribution of the left middle cerebral artery. Histological examination of a brain tissue sample from the left temporal lobe shows proliferation of neural cells that stain positive for glial fibrillary acidic protein. Based on these findings, approximately how much time has most likely passed since the initial injury in this patient?
A 72-year-old female is brought to the emergency department by ambulance because she was unable to walk. She says that she cut her leg while falling about a week ago. Since then, the wound has started draining fluid and become progressively more painful. She is found to have necrotizing fasciitis and is taken emergently to the operating room. Histological examination of cells along the fascial planes reveal cells undergoing necrosis. Which of the following represents the earliest sign that a cell has progressed to irreversible damage in this patient?
A 62-year-old man presents to the emergency room with an acute myocardial infarction. Twenty-four hours after admission to the cardiac intensive care unit, he develops oliguria. Laboratory tests show that his serum BUN is 59 mg/dL and his serum creatinine is 6.2 mg/dL. Renal biopsy reveals necrosis of the proximal tubules and thick ascending limb of Henle's loop. Which of the following would you most likely observe on a microscopic examination of this patient's urine?
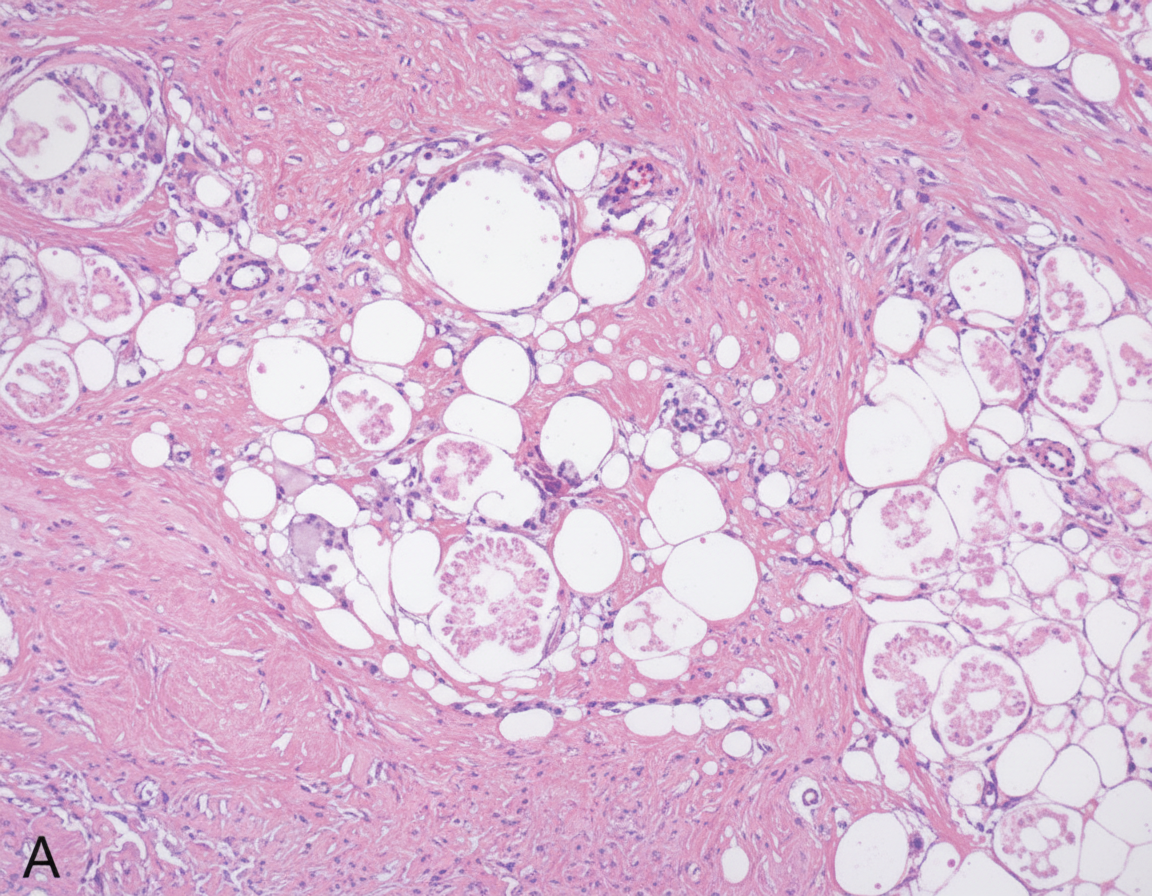
A 34-year-old woman comes to the physician a week after noticing a lump in her left breast. Three months ago, she was discharged from the hospital after treatment of multiple injuries sustained in a motor vehicle collision. Her only medication is an oral contraceptive. Her mother died of ovarian cancer. Examination shows a 2.5-cm, nontender mass in the upper outer quadrant of the left breast. Mammography shows a circumscribed radiolucent lesion with a rim of peripheral calcification. A photomicrograph of tissue from a biopsy of the mass is shown. Which of the following is the most likely cause of the breast swelling?
A patient in a phase 1 trial for a novel epoxide reductase inhibitor, being studied for stroke prophylaxis, develops pain and erythema on the right thigh two days after starting the trial. This rapidly progresses to a purpuric rash with necrotic bullae within 24 hours. Lab results show a PTT of 29 seconds, PT of 28 seconds, and INR of 2.15. What is the most likely pathogenesis of this condition?
A 38-year-old man is admitted to the hospital because of fever, yellowing of the skin, and nausea for 1 day. He recently returned from a backpacking trip to Brazil and Paraguay, during which he had a 3-day episode of high fever that resolved spontaneously. Physical examination shows jaundice, epigastric tenderness, and petechiae over his trunk. Five hours after admission, he develops dark brown emesis and anuria. Despite appropriate lifesaving measures, he dies. Postmortem liver biopsy shows eosinophilic degeneration of hepatocytes with condensed nuclear chromatin. This patient’s hepatocytes were most likely undergoing which of the following processes?
A 13-year-old African-American boy is brought to the physician because of a 4-week history of left groin and buttock pain. The pain is worse with activity but also present at rest. He has had many episodes of abdominal, back, and chest pain that required hospitalization in the past. He is at the 20th percentile for height and 25th percentile for weight. His temperature is 36.7°C (98°F), blood pressure is 115/82 mm Hg, and pulse is 84/min. Examination shows tenderness over the lateral aspect of the left hip with no swelling, warmth, or erythema. There is pain with passive abduction and internal rotation of the left hip. Leukocyte count is 8,600/mm3. Which of the following is the most likely cause of this patient's symptoms?
A 47-year-old woman with a long history of poorly controlled type 2 diabetes and recurrent urinary tract infections presents with complaints of fever, chills, and severe flank pain. On physical exam, she has left-sided costovertebral tenderness. Vitals include a temperature of 39.4°C (103.0°F), blood pressure of 125/84 mm Hg, and pulse of 84/min. She is currently taking metformin daily. Urine dipstick analysis is positive for leukocytes, nitrites, and blood. Laboratory studies show an elevated creatinine of 2.8 mg/dL (baseline 1.0 mg/dL). Urinalysis reveals fragments of tissue. What is the most likely diagnosis?
A 13-year-old boy is brought to the emergency department by his parents for severe right hip pain that suddenly started about 2 hours ago. The parents are extremely anxious and feel overwhelmed because the boy has been hospitalized several times in the past for similar episodes of pain. The boy was born at 39 weeks of gestation via spontaneous vaginal delivery. He is up to date on all vaccinations and is meeting all developmental milestones. His only medication is hydroxyurea, which he has been receiving for 3 years. His blood pressure is 125/84 mm Hg, the respirations are 23/min, the pulse is 87/min, and the temperature is 36.7°C (98.0°F). On physical examination, the patient is in distress and has severe pain (8/10) elicited by gentle palpation of the right femoral head. Which of the following conditions has the same pathophysiology as the likely diagnosis for the patient described in this case?
A 52-year-old female was found upon mammography to have branching calcifications in the right lower breast. Physical exam revealed a palpable nodularity in the same location. A tissue biopsy was taken from the lesion, and the pathology report diagnosed the lesion as comedocarcinoma. Which of the following histological findings is most likely present in the lesion?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
