Cell injury — MCQs

On this page
A 50-year-old man presents with a 3-day history of painful peeling of his skin. He says he initially noted small erythematous spots on areas of his neck, but this quickly spread to his torso, face, and buttocks to form flaccid blisters and areas of epidermal detachment involving > 40% of his total body surface area. He describes the associated pain as severe, burning, and generalized over his entire body. The patient does recall having an episode with similar symptoms 10 years ago after taking an unknown antibiotic for community-acquired pneumonia, but the symptoms were nowhere near this severe. He denies any fever, chills, palpitations, dizziness, or trouble breathing. Past medical history is significant for a urinary tract infection (UTI) diagnosed 1 week ago for which he has been taking ciprofloxacin. His vital signs include: blood pressure, 130/90 mm Hg; temperature, 37.7℃ (99.9℉); respiratory, rate 22/min; and pulse, 110/min. On physical examination, the patient is ill-appearing and in acute distress due to pain. The epidermis sloughing involves areas of the face, back, torso, buttocks, and thighs bilaterally, and its appearance is shown in the exhibit (see image). Nikolsky sign is positive. Laboratory findings are unremarkable. Which of the following is the next best diagnostic step in this patient?
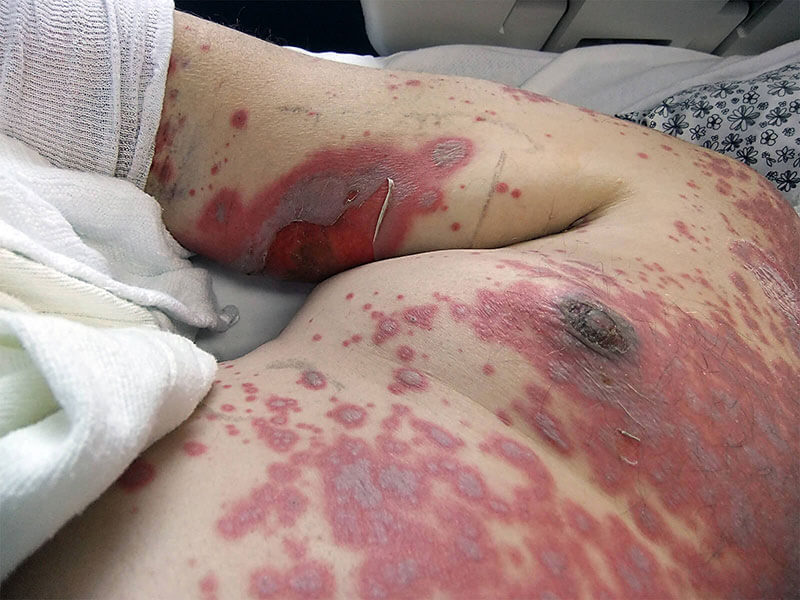
An 87-year-old woman is admitted to the intensive care unit after a neighbor found her lying on the floor at her home. Her respirations are 13/min and shallow. Despite appropriate therapy, the patient dies. Gross examination of the brain at autopsy shows neovascularization and liquefactive necrosis without cavitation in the distribution of the left middle cerebral artery. Histological examination of a brain tissue sample from the left temporal lobe shows proliferation of neural cells that stain positive for glial fibrillary acidic protein. Based on these findings, approximately how much time has most likely passed since the initial injury in this patient?
A 13-year-old boy is brought to the emergency department by his parents for severe right hip pain that suddenly started about 2 hours ago. The parents are extremely anxious and feel overwhelmed because the boy has been hospitalized several times in the past for similar episodes of pain. The boy was born at 39 weeks of gestation via spontaneous vaginal delivery. He is up to date on all vaccinations and is meeting all developmental milestones. His only medication is hydroxyurea, which he has been receiving for 3 years. His blood pressure is 125/84 mm Hg, the respirations are 23/min, the pulse is 87/min, and the temperature is 36.7°C (98.0°F). On physical examination, the patient is in distress and has severe pain (8/10) elicited by gentle palpation of the right femoral head. Which of the following conditions has the same pathophysiology as the likely diagnosis for the patient described in this case?
A 53-year-old woman is brought to the physician by her husband for the evaluation of progressive memory loss, which he reports began approximately 2 weeks ago. During this time, she has had problems getting dressed and finding her way back home after running errands. She has also had several episodes of jerky, repetitive, twitching movements that resolved spontaneously. She is oriented only to person and place. She follows commands and speaks fluently. She is unable to read and has difficulty recognizing objects. Which of the following is the most likely underlying cause of this patient's symptoms?
A 55-year-old man with atrial fibrillation is brought to the emergency department by his wife 6 hours after the acute onset of right arm weakness and slurred speech. An MRI of the brain shows a thrombus in the left middle cerebral artery. Twelve hours later, the patient develops ventricular tachycardia. Despite appropriate care, he dies. Which of the following histopathologic changes are most likely to be seen on a biopsy specimen from the affected brain tissue?
A previously healthy 24-year-old woman comes to the physician because of a 1-day history of painful rash after spending several hours in the sun. Skin examination shows well-demarcated areas of erythema with some scaling on the face, chest, upper back, and arms. The affected areas are hot and sensitive to touch. The oral mucosa appears normal. Which of the following is the most likely underlying mechanism of this patient's skin findings?
A 58-year-old man with a history of alcoholism is hospitalized with acute onset nausea and hematemesis. On admission, his vitals are as follows: blood pressure 110/70 mm Hg, heart rate 88/min, respiratory rate 16/min, and temperature 37.8℃ (100.0℉). Physical examination shows jaundice, palmar erythema, widespread spider angiomata, abdominal ascites, and visibly distended superficial epigastric veins. Abdominal ultrasound demonstrates portal vein obstruction caused by liver cirrhosis. Where in the liver would you find the earliest sign of fibrous deposition in this patient?
A 27-year-old man who recently immigrated to the United States with his family is diagnosed with an autosomal dominant disorder that causes anemia by extravascular hemolysis. The doctor explains that his red blood cells (RBCs) are spherical, which decreases their lifespan and explains that a splenectomy may be required in the future. Which of the following is most likely to be defective in this patient?
A 45-year-old man with a history of epilepsy comes to the physician for a follow-up examination. He has had trouble moving the right side of his body for 2 weeks. Three weeks ago he was admitted to the hospital for a generalized convulsive seizure. He was treated with intravenous lorazepam and phenytoin; the seizure activity resolved after 50 minutes on EEG monitoring. He was discharged 2 days later after no further epileptic activity occurred. Physical examination at discharge showed no abnormalities. He has had multiple hospitalizations for similar episodes over the past year. His only medication is lamotrigine, though he says that he sometimes forgets to take it. His temperature is 37°C (98.6°F), pulse is 70/min, and blood pressure is 130/80 mm Hg. Physical examination shows right-sided hemiparesis, right homonymous hemianopsia, and receptive aphasia. Which of the following is the most likely underlying cause of this patient's current symptoms?
An autopsy is performed on a 39-year-old man 5 days after he was found pulseless at his apartment by his neighbor. Examination of the brain shows liquefactive necrosis in the distribution of the right middle cerebral artery with surrounding edema. Immunophenotyping of a sample of the affected brain tissue shows numerous cells that express CD40 on their surface. On further histopathological evaluation, the morphology of these cells is not readily discernible with Nissl stain. These histological findings are most consistent with which of the following cell types?
Practice by Chapter
Reversible cell injury mechanisms
Practice Questions
Irreversible cell injury (necrosis)
Practice Questions
Types of necrosis (coagulative, liquefactive, etc.)
Practice Questions
Apoptosis pathways
Practice Questions
Autophagy mechanisms
Practice Questions
Cellular adaptations (atrophy, hypertrophy)
Practice Questions
Hyperplasia and metaplasia
Practice Questions
Dysplasia
Practice Questions
Intracellular accumulations
Practice Questions
Pathologic calcification
Practice Questions
Cellular aging mechanisms
Practice Questions
Ischemia-reperfusion injury
Practice Questions
Free radical injury
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
