Cell injury — MCQs

On this page
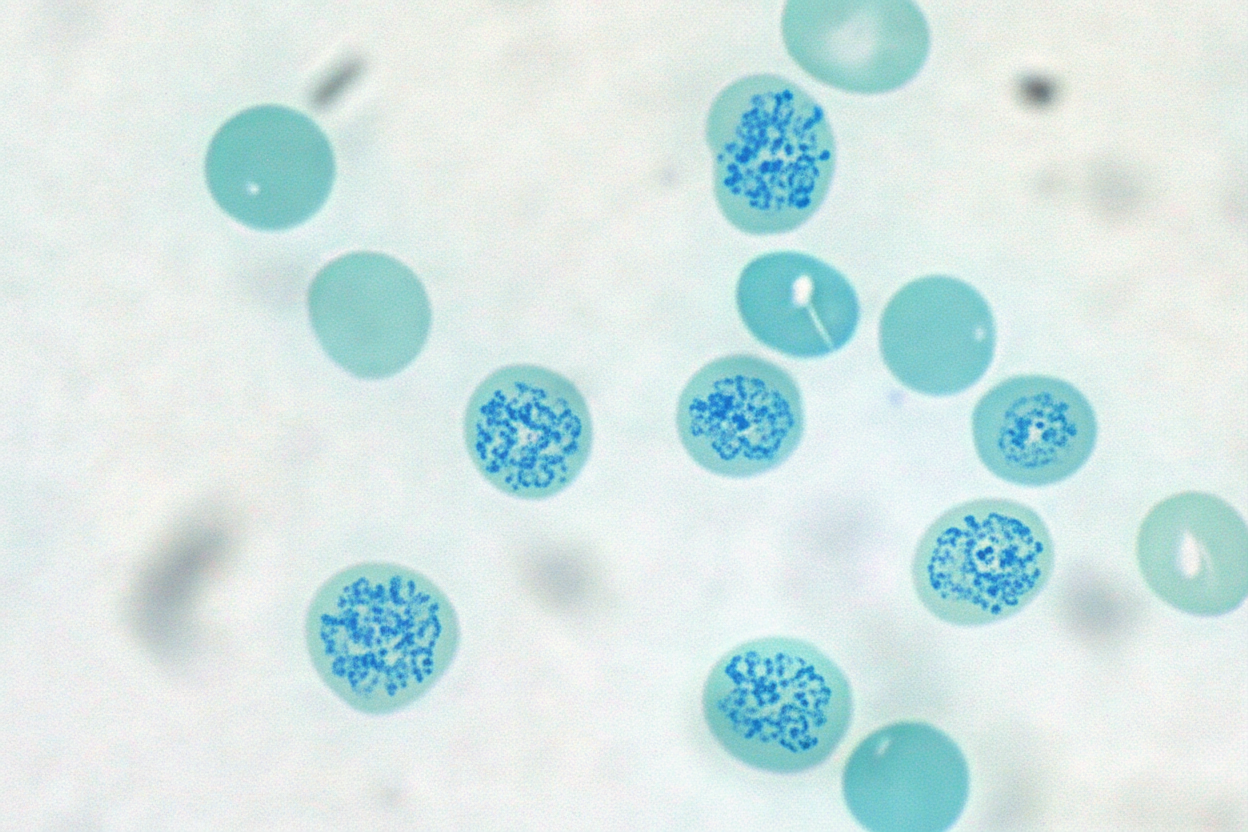
A 59-year-old woman with a history of chronic kidney disease comes to the physician for a 3-month history of easy fatiguability. Physical examination shows subconjunctival pallor. Her hemoglobin concentration is 8.9 g/dL, mean corpuscular volume is 86 μm3, and serum ferritin is 225 ng/mL. Treatment with erythropoietin is begun. A peripheral blood smear is obtained one week after treatment. A photomicrograph of the smear after specialized staining is shown. The prominent color of the intracellular structure in some of the cells is most likely the result of staining which of the following?
A 30-year-old woman presents to her physician for a routine check-up. She says she is planning to get pregnant. Past medical history is significant for arterial hypertension. Current medications are enalapril. The physician explains that this medication can be teratogenic. He changes her antihypertensive medication to methyldopa, which has no contraindications for pregnant women. A few days later, the patient is admitted to the emergency department with jaundice and dark urine. Her laboratory tests are as follows: Hemoglobin 0.9 g/dL Red blood cells 3.2 x 106/µL White blood cells 5,000/mm3 Platelets 180,000/mm3 Direct Coombs test Positive This patient is diagnosed with autoimmune hemolytic anemia (AIHA). Which of the following is correct about autoimmune hemolytic anemia in this patient?
A previously healthy 5-year-old girl is brought to the emergency department by her parents because of a severe headache, nausea, and vomiting for 6 hours. Last week she had fever, myalgias, and a sore throat for several days that resolved with over-the-counter medication. She is oriented only to person. Examination shows bilateral optic disc swelling. Serum studies show: Glucose 61 mg/dL Aspartate aminotransferase (AST) 198 U/L Alanine aminotransferase (ALT) 166 U/L Prothrombin time 18 sec Which of the following is the most likely cause of this patient's symptoms?
An autopsy is being performed on an elderly man who died from a myocardial infarction. Biopsy of the heart is likely to reveal necrosis most similar to necrosis seen in which of the following scenarios?
A 30-year-old man comes to the physician for a follow-up examination 1 month after sustaining a chemical burn over the dorsum of his right hand and forearm. Physical examination shows hyperextension of the hand at the wrist. The skin over the dorsum of the wrist is tense and there is a thick, epithelialized scar. Range of motion of the right wrist is restricted. This patient's contracture is most likely due to activity of which of the following cells?
An 8-year-old boy presents with a 7-day history of fever and abdominal pain for the past 4 days. Past medical history is significant for an exchange transfusion for neonatal hyperbilirubinemia and recurrent attacks of pallor during the course of upper respiratory tract infections. His vital signs include: blood pressure 120/70 mm Hg, pulse 105/min, respiratory rate 40/min, and temperature 37.0℃ (98.6℉). On physical examination, the patient is ill-looking. Conjunctivae are pale and the sclera is icteric. The liver is palpable 2 cm below the costal margin and the spleen is palpable 3 cm below the left costal margin. Laboratory findings show hemoglobin of 5.9 gm/dL, Hct of 20%, and haptoglobin of 28 mg/dL. A peripheral blood smear shows hypochromic anemia, polychromasia, anisocytosis, and occasional Heinz bodies. The reticulocyte count was 15%. A direct Coombs test was negative. Which of the following is the most likely diagnosis in this patient?
A 3-year-old boy is brought to the physician because of a 1-week history of yellowish discoloration of his eyes and skin. He has had generalized fatigue and mild shortness of breath for the past month. Three weeks ago, he was treated for a urinary tract infection with antibiotics. His father underwent a splenectomy during childhood. Examination shows pale conjunctivae and jaundice. The abdomen is soft and nontender; there is nontender splenomegaly. Laboratory studies show: Hemoglobin 9.1 g/dL Mean corpuscular volume 89 μm3 Mean corpuscular hemoglobin 32 pg/cell Mean corpuscular hemoglobin concentration 37.8% Hb/cell Leukocyte count 7800/mm3 Platelet count 245,000/mm3 Red cell distribution width 22.8% (N=13%–15%) Serum Bilirubin Total 13.8 mg/dL Direct 1.9 mg/dL Lactate dehydrogenase 450 U/L Which of the following is the most likely pathophysiology of these findings?
A 27-year-old African American man presents to a primary care physician for a routine checkup as a new patient. The patient states that he has been doing well lately and recently was promoted at his job. He states that 2 weeks ago he went to the ED for severe pain and was treated with morphine and oral fluids and discharged home that night. This had happened once before and he was treated similarly. The patient states that he drinks 7 to 8 alcoholic beverages per night and smokes 1 pack of cigarettes per day. The patient states that he has been gaining weight recently due to a diet consisting mostly of fast food. Basic labs are ordered as seen below. Hemoglobin: 8 g/dL Hematocrit: 28% Mean corpuscular volume: 72 um^3 Leukocyte count: 6,500/mm^3 with normal differential Platelet count: 157,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 99 mg/dL Creatinine: 1.1 mg/dL LDH: 540 U/L Ca2+: 10.2 mg/dL AST: 12 U/L ALT: 10 U/L Which of the following is the best explanation of this patient's laboratory abnormalities?
A 3-week-old male infant is brought to the physician for evaluation of poor feeding and recurrent episodes of facial grimacing. He was delivered at term after an uncomplicated pregnancy. He is at the 3rd percentile for length and 5th percentile for weight. Physical examination shows yellow discoloration of skin, a broad nasal bridge, hepatomegaly, and decreased muscle tone in the extremities. Serum studies show increased concentrations of very long-chain fatty acids. Examination of the liver cells from this neonate is most likely to show which of the following findings?
A 32-year-old woman comes to the physician because of increasing muscle weakness in her shoulders and legs for 6 weeks. She is unable to climb stairs or comb her hair. She has also had difficulty swallowing food for the past week. Her symptoms do not improve with rest. Physical examination shows normal muscle tone. There is bilateral weakness of the iliopsoas, hamstring, deltoid, and biceps muscles. Deep tendon reflexes are 2+ bilaterally. Sensation to pinprick, temperature, and vibration is intact. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 10.7 g/dL Leukocyte count 10.800/mm3 Erythrocyte sedimentation rate 100 mm/h Serum Glucose 60 mg/dL Creatine kinase 7047 U/L Lactate dehydrogenase 2785 U/L Thyroid-stimulating hormone 4.0 μU/mL Which of the following is the most appropriate next step in management?
Practice by Chapter
Reversible cell injury mechanisms
Practice Questions
Irreversible cell injury (necrosis)
Practice Questions
Types of necrosis (coagulative, liquefactive, etc.)
Practice Questions
Apoptosis pathways
Practice Questions
Autophagy mechanisms
Practice Questions
Cellular adaptations (atrophy, hypertrophy)
Practice Questions
Hyperplasia and metaplasia
Practice Questions
Dysplasia
Practice Questions
Intracellular accumulations
Practice Questions
Pathologic calcification
Practice Questions
Cellular aging mechanisms
Practice Questions
Ischemia-reperfusion injury
Practice Questions
Free radical injury
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
