Cardiovascular — MCQs

On this page
A 31-year-old Israeli male with a history of heavy smoking presents to your office with painful ulcerations on his hands and feet. Upon examination, he is found to have hypersensitivity to intradermally injected tobacco extract. Which of the following processes is most likely responsible for his condition?
A 15-year-old African-American boy is brought to the physician because of left-sided groin pain and difficulty walking for 3 weeks. He reports having pain at rest and increased pain with activity. He recently started playing flag football but does not recall any trauma. He has had many episodes of joint and bone pain that required hospitalization in the past. He is at the 25th percentile for height and 20th percentile for weight. His temperature is 37°C (98.6°F), blood pressure is 120/80 mm Hg, and pulse is 90/min. Examination shows tenderness over the lateral aspect of the hip with no swelling, warmth, or erythema. There is pain with passive internal rotation of the left hip. The remainder of the examination shows no abnormalities. Leukocyte count is 9,000/mm3. Which of the following conditions is the most likely cause of the patient's current symptoms?
A previously healthy 82-year-old man dies in a motor vehicle collision. At autopsy, the heart shows slight ventricular thickening. There are abnormal, insoluble aggregations of protein filaments in beta-pleated linear sheets in the ventricular walls and, to a lesser degree, in the atria and lungs. No other organs show this abnormality. Bone marrow examination shows no plasma cell dyscrasia. The abnormal protein aggregations are most likely composed of which of the following?
A 56-year-old male died in a motor vehicle accident. Autopsy reveals extensive atherosclerosis of his left anterior descending artery marked by intimal smooth muscle and collagen proliferation. Which of the following is implicated in recruiting smooth muscle cells from the media to intima in atherosclerotic lesions?
A 54-year-old man was brought to the emergency room due to acute onset of slurred speech while at work, after which he lost consciousness. The patient's wife says this occurred approximately 30 minutes ago. Past medical history is significant for poorly controlled hypertension and type 2 diabetes mellitus. His blood pressure is 90/50 mm Hg, respiratory rate is 12/min, and heart rate is 48/min. The patient passes away shortly after arriving at the hospital. At autopsy, bilateral wedge-shaped strips of necrosis are seen in this patient's brain in the medial temporal lobe structures. Which of the following is the most likely location of these necrotic cells?
An 18-year-old man presents with a sudden loss of consciousness while playing college football. There was no history of a concussion. Echocardiography shows left ventricular hypertrophy and increased thickness of the interventricular septum. Which is the most likely pathology underlying the present condition?
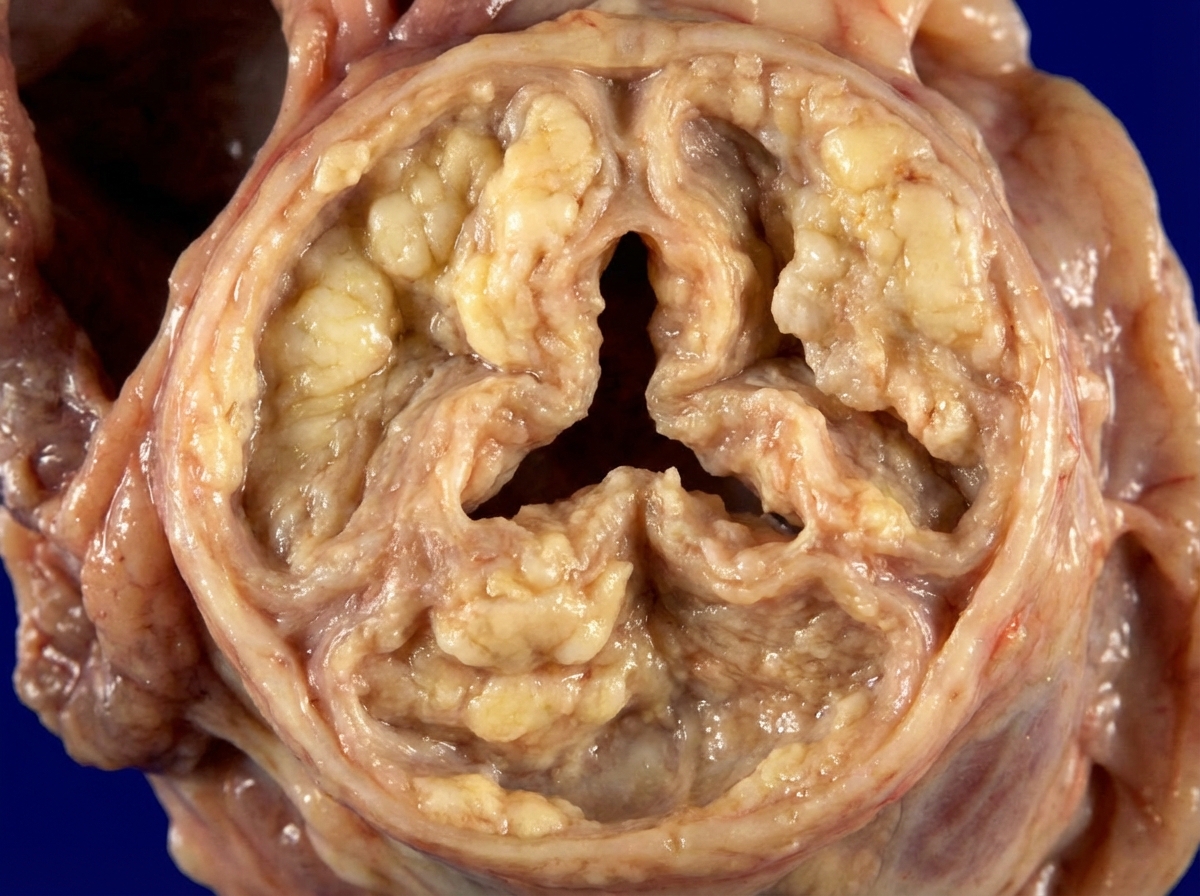
A 72-year-old man who was involved in a traffic collision is brought to the emergency room by the ambulance service. He was in shock and comatose at the time of presentation. On examination, the heart rate is 60/min, and the blood pressure is 70/40 mm Hg. The patient dies, despite resuscitative efforts. Autopsy reveals multiple internal hemorrhages and other evidence of ischemic damage affecting the lungs, kidneys, and brain. The patient’s heart shows evidence of gross anomaly similar to the picture. While acute hypovolemia is the likely cause of the ischemic changes seen in the lungs, kidneys, and brain, which of the following best explains the gross anomaly of his heart?
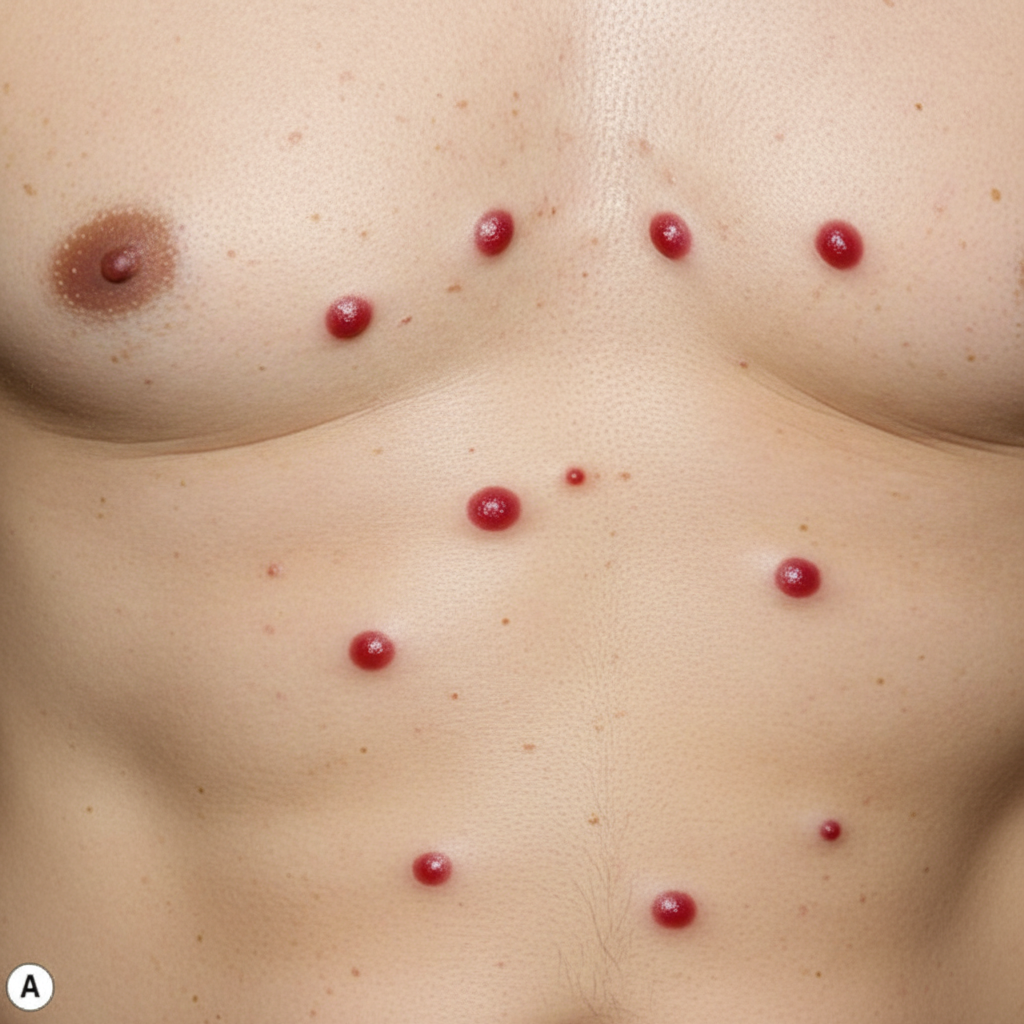
A 62-year-old man comes to the physician for evaluation of multiple red spots on his trunk. He first noticed these several months ago, and some appear to have increased in size. One day ago, he scratched one of these spots, and it bled for several minutes. Physical examination shows the findings in the photograph. Which of the following is the most likely diagnosis?
A 53-year-old man presents to the emergency department with a complaint of chest pain for 5 hours. The chest pain is continuous and squeezing in nature, not relieved by aspirin, and not related to the position of respiration. The blood pressure was 102/64 mm Hg, and the heart rate was 73/min. On physical examination, heart sounds are normal on auscultation. His ECG shows sinus rhythm with ST-segment elevation in leads II and III, aVF, and reciprocal segment depression in precordial leads V1–V6. Tissue plasminogen activator therapy is administered to the patient intravenously within 1 hour of arrival at the hospital. After 6 hours of therapy, the patient’s clinical condition starts to deteriorate. An ECG now shows ventricular fibrillation. The patient dies, despite all the efforts made in the intensive care unit. What is the most likely pathological finding to be expected in his heart muscles on autopsy?
A 59-year-old presents with right-sided hemiparesis, right-sided sensory loss, leftward eye deviation, and slurred speech. A head CT is performed which is significant for a hyperdense lesion affecting the putamen. The patient has a history of hypertension treated with hydrochlorothiazide, but is non-adherent. Which of the following is most likely associated with the cause of this patient’s neurological deficits?
Practice by Chapter
Atherosclerosis
Practice Questions
Ischemic heart disease
Practice Questions
Myocardial infarction pathology
Practice Questions
Hypertensive heart disease
Practice Questions
Congenital heart defects
Practice Questions
Valvular heart disease
Practice Questions
Rheumatic heart disease
Practice Questions
Infective endocarditis
Practice Questions
Myocarditis and cardiomyopathies
Practice Questions
Pericardial diseases
Practice Questions
Aneurysms and dissections
Practice Questions
Vasculitis
Practice Questions
Cardiac tumors
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
