Cardiovascular — MCQs

On this page
A 32-year-old woman who recently emigrated to the USA from Japan comes to the physician because of a 3-month history of night sweats, malaise, and joint pain. During this time, she has also had a 6-kg (13-lb) weight loss. Physical examination shows weak brachial and radial pulses. There are tender subcutaneous nodules on both legs. Carotid bruits are heard on auscultation bilaterally. Laboratory studies show an erythrocyte sedimentation rate of 96 mm/h. A CT scan of the chest shows thickening and narrowing of the aortic arch. Microscopic examination of the aortic arch is most likely to show which of the following findings?
A 69-year-old man is brought to clinic by his daughter for poor memory. She states that over the past two years his memory has been slowly declining though he has been able to take care of himself, pay his own rent, and manage his finances. However, two months ago she noticed a sharp decline in his cognitive functioning as well as his gait. Then one month ago, she noticed a similar decline in his functioning again that came on suddenly. The patient has a past medical history of diabetes mellitus type II, hypertension, obesity, and dyslipidemia. Current medications include hydrochlorothiazide, lisinopril, metformin, and glipizide. His blood pressure is 165/95 mmHg, pulse is 82/minute, he is afebrile, and oxygen saturation is 98% on room air. Cardiac exam reveals a crescendo-decrescendo murmur heard in the left upper sternal border that radiates to the carotids. Abdominal exam is benign, and neurologic exam reveals an unsteady gait. Which of the following findings is associated with the most likely diagnosis?
A 58-year old man comes to the emergency department because of progressively worsening shortness of breath and fatigue for 3 days. During the last month, he has also noticed dark colored urine. One month ago, he underwent mechanical aortic valve replacement for high-grade aortic stenosis. A photomicrograph of a peripheral blood smear from the patient is shown. Which of the following findings is most likely to be seen in this patient?
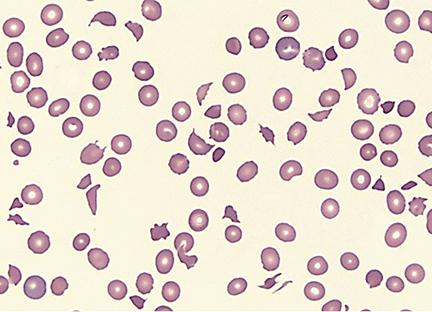
An investigator is studying genetic mutations of coagulation factors from patient samples. Genetic sequencing of one patient's coagulation factors shows a DNA point mutation that substitutes guanine for adenine. The corresponding mRNA codon forms a glutamine in place of arginine on position 506 at the polypeptide cleavage site. This patient's disorder is most likely to cause which of the following?
A 31-year-old woman comes to the physician for evaluation of worsening pain, swelling, and erythema in her left leg for the past 4 hours. She returned from a trip to Taiwan to celebrate her sister's wedding 2 days ago. She has no history of serious illness. She is sexually active with one male partner and uses a combined oral contraceptive pill (OCP). She does not smoke, drink, or use illicit drugs. Her only other medication is a multivitamin. Her temperature is 37.2°C (99°F), pulse is 67/min, respirations are 16/min, and blood pressure is 90/60 mm Hg. Examination shows swelling in her left calf and pain behind her left knee when she is asked to dorsiflex her left foot. Laboratory results show elevated D-dimers. Which of the following is the most likely cause of this patient's clinical presentation?
A 3-year-old boy is brought to the emergency department after losing consciousness. His parents report that he collapsed and then had repetitive, twitching movements of the right side of his body that lasted approximately one minute. He recently started to walk with support. He speaks in bisyllables and has a vocabulary of almost 50 words. Examination shows a large purple-colored patch over the left cheek. One week later, he dies. Which of the following is the most likely finding on autopsy of the brain?
A 41-year-old man with a history of hypertension and hyperlipidemia is brought to the emergency department by his wife for difficulty breathing after choking on food at dinner. He is unconscious and pulseless on arrival. Despite appropriate life-saving measures, he dies. Examination of the heart shows a necrotic, pale yellow plaque in the left circumflex artery. Similar lesions are most likely to be found in which of the following locations?
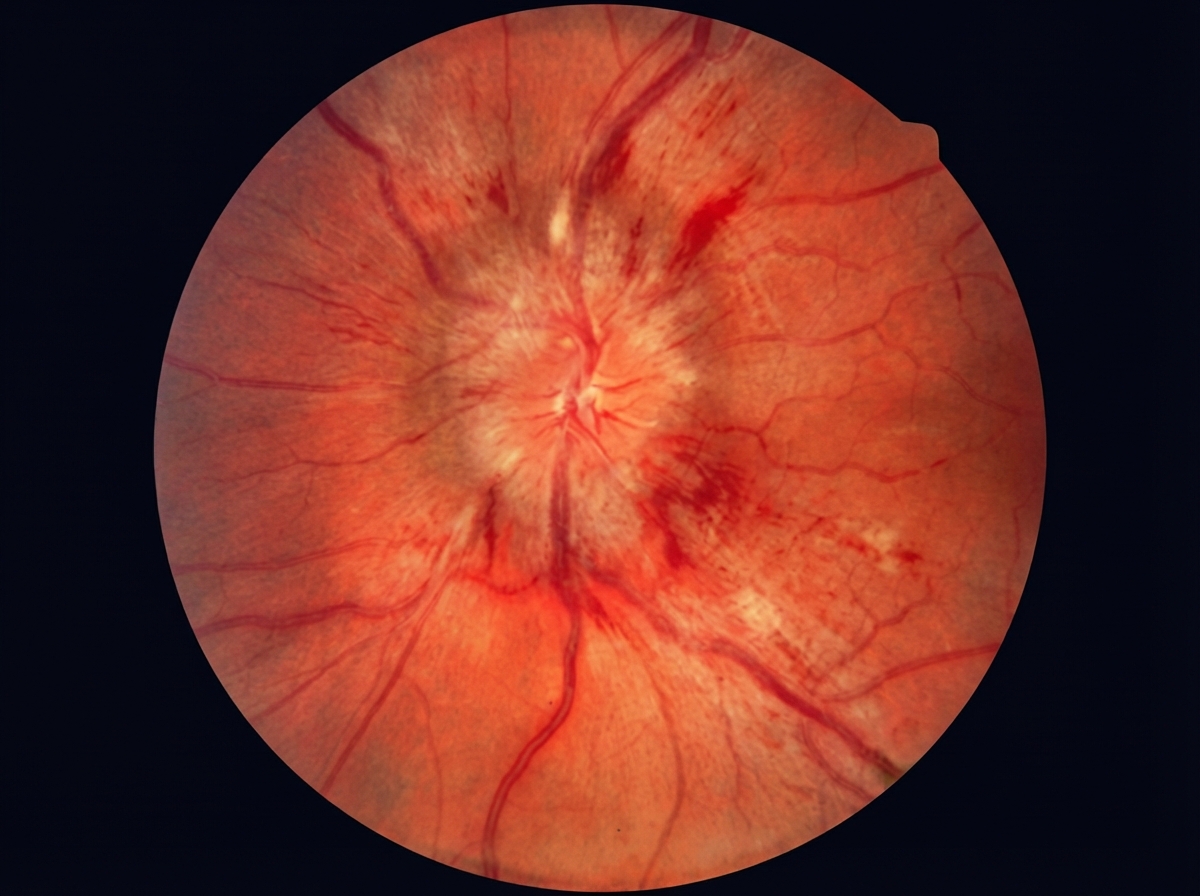
A 55-year-old man visits his primary care physician for a follow-up visit. He was diagnosed with asthma during childhood, but it has always been well controlled with an albuterol inhaler. He is hypertensive and admits that he is not compliant with his antihypertensive medication. He expresses his concerns about frequent headaches and blurry vision over the past few months. He has been taking acetaminophen for his headaches, but it has not made any difference. The blood pressure is 160/100 mm Hg, pulse rate is 77/min, and respiratory rate is 14/min. The BMI is 36.2 kg/m2. Physical examination is unremarkable. A urinalysis is notable for proteinuria. Funduscopic examination is shown on the right. Which pathologic mechanism best explains the changes seen in this patient’s fundoscopic examination?
A 65-year-old woman presents with severe abdominal pain and bloody diarrhea. Past medical history is significant for a myocardial infarction 6 months ago. The patient reports a 25-pack-year smoking history and consumes 80 ounces of alcohol per week. Physical examination shows a diffusely tender abdomen with the absence of bowel sounds. Plain abdominal radiography is negative for free air under the diaphragm. Laboratory findings show a serum amylase of 115 U/L, serum lipase 95 U/L. Her clinical condition deteriorates rapidly, and she dies. Which of the following would most likely be the finding on autopsy in this patient?
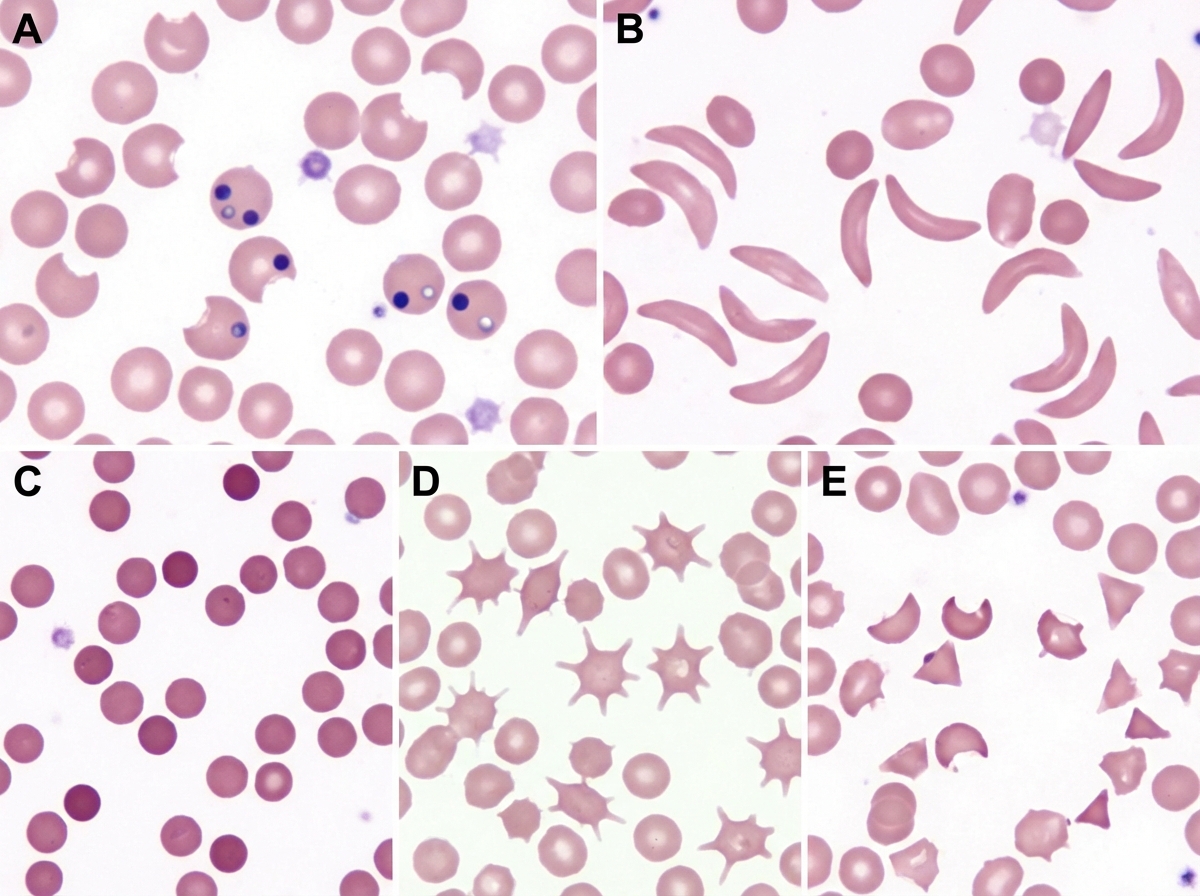
A 68-year-old man of Mediterranean descent comes to the clinic with complaints of fatigue for the past month. He reports that it is increasingly difficult for him to complete his after-dinner walks as he would get breathless and tired around 10 minutes. He endorses dizziness and an upper respiratory infection last week for which he “took a lot of aspirin.” Past medical history is significant for malaria 10 years ago (for which he was adequately treated with anti-malarial medications) and aortic stenosis status post prosthetic valve replacement 5 months ago. When asked if he has had similar episodes before, he claims, “Never! I’ve been as healthy as a horse until my heart surgery.” Physical examination is significant for mild scleral icterus bilaterally and a faint systolic murmur. Which of the following images represents a potential peripheral smear in this patient?
Practice by Chapter
Atherosclerosis
Practice Questions
Ischemic heart disease
Practice Questions
Myocardial infarction pathology
Practice Questions
Hypertensive heart disease
Practice Questions
Congenital heart defects
Practice Questions
Valvular heart disease
Practice Questions
Rheumatic heart disease
Practice Questions
Infective endocarditis
Practice Questions
Myocarditis and cardiomyopathies
Practice Questions
Pericardial diseases
Practice Questions
Aneurysms and dissections
Practice Questions
Vasculitis
Practice Questions
Cardiac tumors
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
