Cardiovascular — MCQs

On this page
A 42-year-old man with systolic heart failure secondary to amyloidosis undergoes heart transplantation. The donor heart is obtained from a 17-year-old boy who died in a motor vehicle collision. Examination of the donor heart during the procedure shows a flat, yellow-white discoloration with an irregular border on the luminal surface of the aorta. A biopsy of this lesion is most likely to show which of the following?
An 80-year-old man is admitted to the hospital after the sudden onset of sub-sternal chest pain and shortness of breath while sitting in a chair. He has hypertension and type 2 diabetes mellitus. He has smoked 1 pack of cigarettes daily for 42 years. Four days after admission, he becomes tachycardic and then loses consciousness; the cardiac monitor shows irregular electrical activity. Cardiac examination shows a new systolic murmur at the apex. Despite appropriate measures, he dies. Microscopic evaluation of the myocardium is most likely to show which of the following?
A 53-year-old woman presents with a severe headache, nausea, and vomiting for the past 48 hours. Vitals show a blood pressure of 220/134 mm Hg and a pulse of 88/min. Urinalysis shows a 2+ proteinuria and RBC casts. Which of the following renal lesions is most likely to be seen in this patient?
A 62-year-old woman is evaluated for fatigue 6 months after placement of a mechanical valve due to aortic stenosis. She does not drink alcohol or smoke cigarettes. A complete blood count reports hemoglobin of 9.5 g/dL and a reticulocyte percentage of 5.8%. Platelet and leukocyte counts are within their normal ranges. The patient's physician suspects traumatic hemolysis from the patient's mechanical valve as the cause of her anemia. Which of the following peripheral blood smear findings would most support this diagnosis?
A 72-year-old man comes to the physician because of a 6-month history of intermittent dull abdominal pain that radiates to the back. He has smoked one pack of cigarettes daily for 50 years. His blood pressure is 145/80 mm Hg. Abdominal examination shows generalized tenderness and a pulsatile mass in the periumbilical region on deep palpation. Further evaluation of the affected blood vessel is most likely to show which of the following?
A 12-year-old girl with an autosomal dominant mutation in myosin-binding protein C is being evaluated by a pediatric cardiologist. The family history reveals that the patient's father died suddenly at age 33 while running a half-marathon. What was the likely finding on histological evaluation of her father's heart at autopsy?
A 58-year-old man presents to the emergency department with severe right leg pain accompanied by tingling and weakness. His condition started suddenly 3 hours ago when he was watching a movie. His medical history is remarkable for type 2 diabetes mellitus and hypertension. He has been smoking 20–30 cigarettes per day for the past 35 years. His vital signs include a blood pressure of 149/85 mm Hg, a temperature of 36.9°C (98.4°F), and an irregular pulse of 96/min. On physical examination, his right popliteal and posterior tibial pulses are absent. His right leg is pale and cold. Which of the following is the most likely diagnosis?
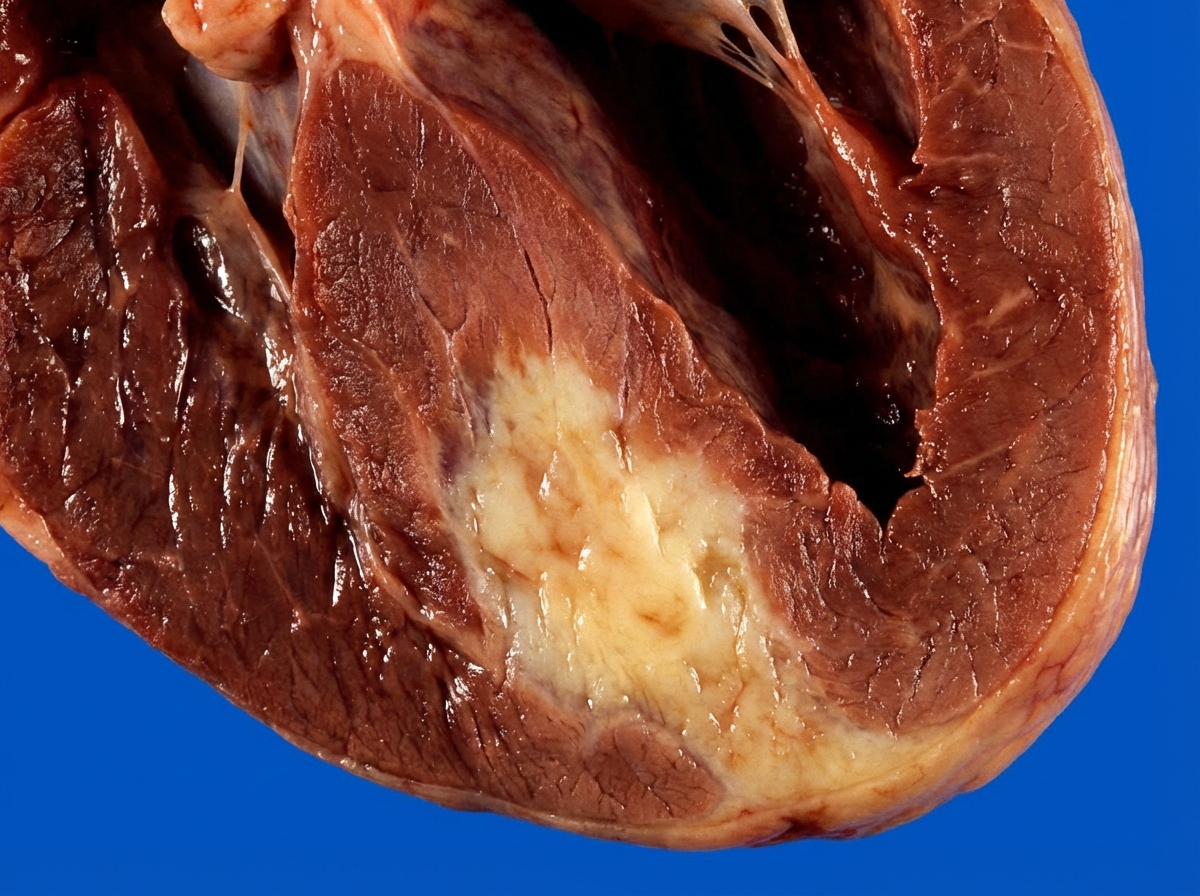
A 76-year-old man is admitted to the hospital for evaluation of sudden-onset chest pain. Three days after admission, he develops severe shortness of breath. Despite appropriate care, the patient dies. The heart at autopsy is shown. Which of the following most likely contributed to this patient's cause of death?
A 80-year-old woman is brought to the emergency department from a senior living home with a chief complaint of acute onset and severe abdominal pain with 5 episodes of bloody diarrhea. She has a history of having chronic constipation, and postprandial abdominal pain which subsides after taking nitroglycerin. The abdominal pain that she is currently experiencing did not subside using her medication. A week ago, she had a percutaneous intervention for an inferior wall STEMI. On physical examination, the patient looks pale and confused. The vital signs include: blood pressure 80/40 mm Hg, heart rate 108/min, respiratory rate 22/min, and temperature 35.6°C (96.0°F). The patient receives an aggressive treatment consisting of intravenous fluids and vasopressors, and she is transferred to the ICU. Despite all the necessary interventions, the patient dies. During the autopsy, a dark hemorrhagic appearance of the sigmoid colon is noted. What is the most likely pathology related to her death?
A 19-year-old Caucasian male collapsed from sudden cardiac arrest while playing in a college basketball game. Attempts at resuscitation were unsuccessful. Post-mortem pathologic and histologic examination found asymmetric left ventricular hypertrophy and myocardial disarray. Assuming this was an inherited condition, the relevant gene most likely affects which of the following structures?
Practice by Chapter
Atherosclerosis
Practice Questions
Ischemic heart disease
Practice Questions
Myocardial infarction pathology
Practice Questions
Hypertensive heart disease
Practice Questions
Congenital heart defects
Practice Questions
Valvular heart disease
Practice Questions
Rheumatic heart disease
Practice Questions
Infective endocarditis
Practice Questions
Myocarditis and cardiomyopathies
Practice Questions
Pericardial diseases
Practice Questions
Aneurysms and dissections
Practice Questions
Vasculitis
Practice Questions
Cardiac tumors
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
