Stages of labor — MCQs

On this page
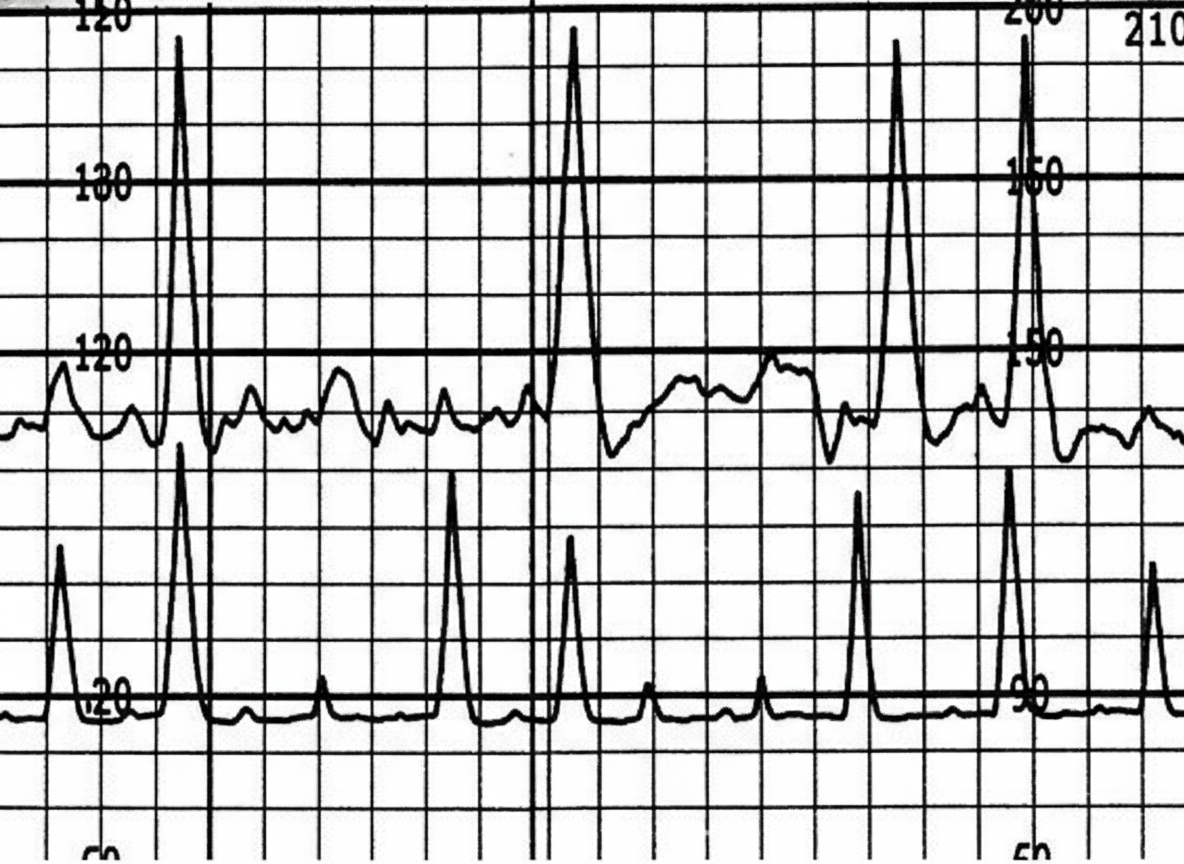
A 28-year-old woman, gravida 2, para 1, at 40 weeks of gestation is admitted to the hospital in active labor. The patient has attended many prenatal appointments and followed her physician's advice about screening for diseases, laboratory testing, diet, and exercise. Her pregnancy has been uncomplicated. She has no history of a serious illness. Her first child was delivered via normal vaginal delivery. Her vital signs are within normal limits. Cervical examination shows 80% effacement, 5 cm dilation and softening without visible fetal parts or prolapsed umbilical cord. A cardiotocograph is shown. Which of the following options is the most appropriate initial step in management?
Practice by Chapter
Physiology of parturition
Practice Questions
First stage of labor
Practice Questions
Second stage of labor
Practice Questions
Third stage of labor
Practice Questions
Fourth stage of labor
Practice Questions
Cardinal movements of labor
Practice Questions
Labor curve and Friedman curve
Practice Questions
Induction of labor indications and methods
Practice Questions
Augmentation of labor
Practice Questions
Cervical ripening methods
Practice Questions
Fetal heart rate monitoring
Practice Questions
Pain management in labor
Practice Questions
Operative vaginal delivery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
