Screening tests — MCQs

On this page
A 30-year-old woman presents to her primary care provider complaining of intermittent fever and loss of appetite for the past 2 weeks. She is also concerned about painful genital lesions. Past medical history is noncontributory. She takes oral contraceptives and a multivitamin daily. She has had two male sexual partners in her lifetime and uses condoms inconsistently. She admits to being sexually active with 2 partners in the last 3 months and only using condoms on occasion. Today, her vitals are normal. On pelvic exam, there are red-rimmed, fluid-filled blisters over the labia minora (as seen in the photograph below) with swollen and tender inguinal lymph nodes. Which of the following is the most likely diagnosis of this patient?
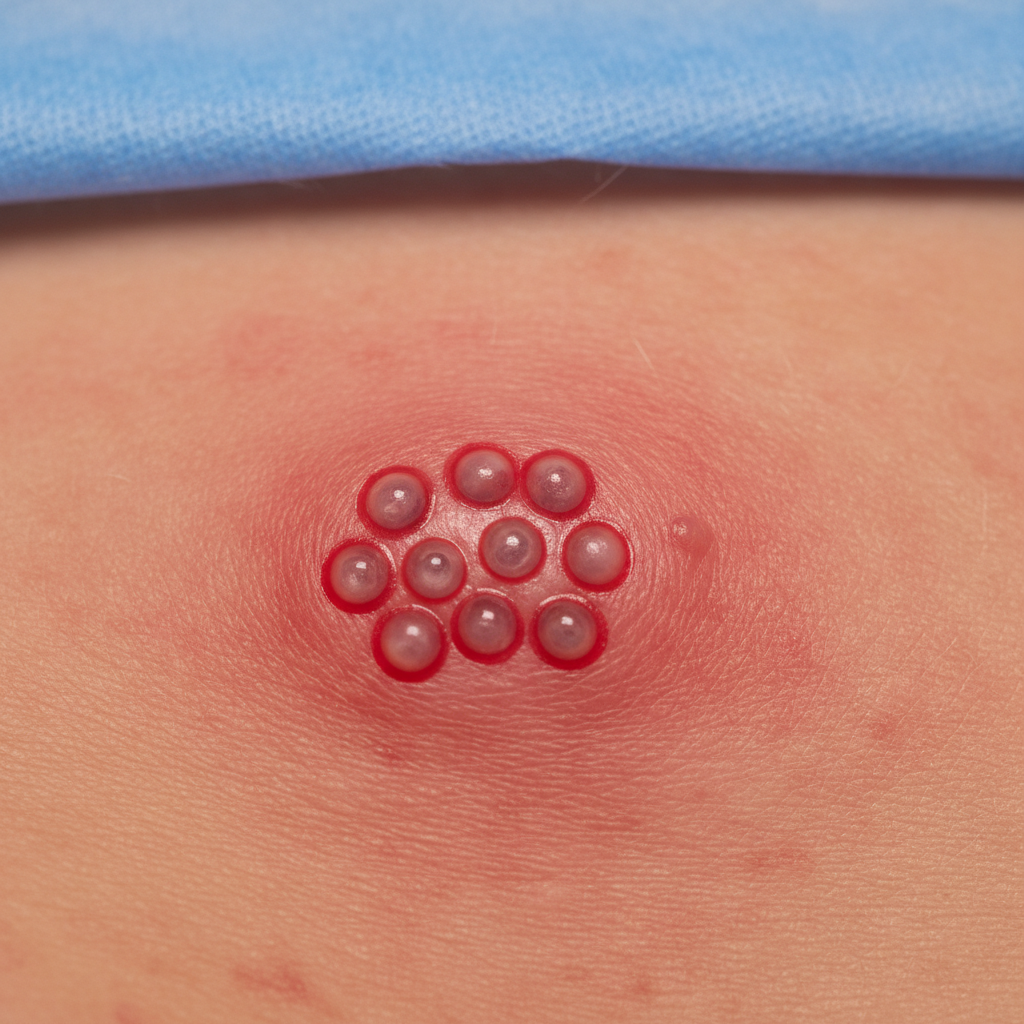
A previously healthy 19-year-old woman comes to the physician because of vaginal discharge for 3 days. She describes the discharge as yellow and mucopurulent with a foul odor. She has also noticed vaginal bleeding after sexual activity. She has not had any itching or irritation. Her last menstrual period was 2 weeks ago. She is sexually active with one male partner, and they use condoms inconsistently. A rapid urine hCG test is negative. Her temperature is 37.3°C (99.1°F), pulse is 88/min, and blood pressure is 108/62 mm Hg. Pelvic examination shows a friable cervix. Speculum examination is unremarkable. A wet mount shows no abnormalities. Which of the following is the most appropriate diagnostic test?
A 38-year-old woman makes an appointment with her family physician for a routine check-up after being away due to travel for 1 year. She recently had a screening Pap smear, which was negative for malignancy. Her past medical history is significant for a Pap smear 2 years ago that reported a low-grade squamous intraepithelial lesion (LSIL). A subsequent colposcopy diagnosed high-grade cervical intraepithelial neoplasia (CIN2). The patient is surprised by the differences in her diagnostic tests. You explain to her the basis for the difference and reassure her. With this in mind, which of the following HPV serotypes is most likely to be present in the patient?
A 38-year-old G2P2 presents to her gynecologist to discuss the results of her diagnostic tests. She has no current complaints or concurrent diseases. She underwent a tubal ligation after her last pregnancy. Her last Pap smear showed a high-grade squamous intraepithelial lesion and a reflex HPV test was positive. Colposcopic examination reveals areas of thin acetowhite epithelium with diffuse borders and fine punctation. The biopsy obtained from the suspicious areas shows CIN 1. Note the discordancy between the cytology (HSIL) and histology (CIN 1) results. Which of the following is an appropriate next step in the management of this patient?
A 19-year-old woman presents to her gynecologist for evaluation of amenorrhea and occasional dull right-sided lower abdominal pain that radiates to the rectum. She had menarche at 11 years of age and had regular 28-day cycles by 13 years of age. She developed menstrual cycle irregularity approximately 2 years ago and has not had a menses for 6 months. She is not sexually active. She does not take any medications. Her weight is 94 kg (207.2 lb) and her height is 166 cm (5.4 ft). Her vital signs are within normal limits. The physical examination shows a normal hair growth pattern. No hair loss or acne are noted. There is black discoloration of the skin in the axillae and posterior neck. Palpation of the abdomen reveals slight tenderness in the right lower quadrant, but no masses are appreciated. The gynecologic examination reveals no abnormalities. The hymen is intact. The rectal examination reveals a non-tender, mobile, right-sided adnexal mass. Which of the following management plans would be best for this patient?
A 24-year-old woman presents to her gynecologist complaining of mild pelvic discomfort and a frothy, yellowish discharge from her vagina for the past 2 weeks. She also complains of pain during sexual intercourse and sometimes after urination. Her past medical history is noncontributory. She takes oral contraceptives and a multivitamin daily. She has had two male sexual partners in her lifetime and uses condoms inconsistently. Today, her vitals are normal. On pelvic exam, she has vulvovaginal erythema and a 'strawberry cervix' that is tender to motion, with minimal green-yellow malodorous discharge. A swab of the vaginal wall is analyzed for pH at bedside. Vaginal pH is 5.8. Which of the following is the most likely diagnosis for this patient?
A 32-year-old woman, gravida 2, para 1, at 14-weeks' gestation comes to the physician for a prenatal visit. Routine first trimester screening shows increased nuchal translucency, decreased β-hCG concentration, and decreased levels of pregnancy-associated plasma protein A. Amniocentesis shows trisomy of chromosome 13. This fetus is at increased risk for which of the following?
A 42-year-old woman comes to the physician because of vaginal discharge for 3 days. She has no dysuria, dyspareunia, pruritus, or burning. The patient is sexually active with two male partners and uses condoms inconsistently. She often douches between sexual intercourse. Pelvic examination shows thin and off-white vaginal discharge. The pH of the discharge is 5.1. Wet mount exam shows a quarter of her vaginal epithelial cells are covered with small coccobacilli. Which of the following is the most appropriate next step in management?
A 32-year-old nulliparous woman with polycystic ovary syndrome comes to the physician for a pelvic examination and Pap smear. Last year she had a progestin-releasing intrauterine device placed. Menarche occurred at the age of 10 years. She became sexually active at the age of 14 years. Her mother had breast cancer at the age of 51 years. She is 165 cm (5 ft 5 in) tall and weighs 79 kg (174 lb); BMI is 29 kg/m2. Examination shows mild facial acne. A Pap smear shows high-grade cervical intraepithelial neoplasia. Which of the following is this patient's strongest predisposing factor for developing this condition?
A 34-year-old woman makes an appointment with her gynecologist because she has been having foul smelling vaginal discharge. She says that the symptoms started about a week ago, but she can't think of any particular trigger associated with the onset of symptoms. She says that otherwise she has not experienced any pain or discomfort associated with these discharges. She has never been pregnant and currently has multiple sexual partners with whom she uses protection consistently. She has no other medical history though she says that her family has a history of reproductive system malignancy. Physical exam reveals a normal appearing vulva, and a sample of the vaginal discharge reveals gray fluid. Which of the following characteristics is associated with the most likely cause of this patient's disorder?
Practice by Chapter
First trimester screening
Practice Questions
Cell-free DNA screening
Practice Questions
Second trimester serum screening
Practice Questions
Ultrasound markers and anomaly screening
Practice Questions
Carrier screening for genetic disorders
Practice Questions
Cervical cancer screening in pregnancy
Practice Questions
Diabetes screening in pregnancy
Practice Questions
Gestational diabetes management
Practice Questions
Group B streptococcus screening
Practice Questions
Screening for preeclampsia risk factors
Practice Questions
Prenatal infection screening (TORCH, HIV, STIs)
Practice Questions
Genetic counseling principles
Practice Questions
Diagnostic testing (amniocentesis, CVS)
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
