Screening tests — MCQs

On this page
A 27-year-old woman presented with a malodorous discharge in the vagina which started a week earlier. On examination, Whiff's test is positive and the gram stain shows the presence of clue cells. This infection is commonly treated with which of the following?
A female presents with postcoital bleeding. Which of the following is the most appropriate investigation?
Which of the following is a tumor marker associated with ovarian solid-cystic masses?
A 45-year-old woman presents with a history of cervical erosion and spotting for the past 2 months. What is the next best step?
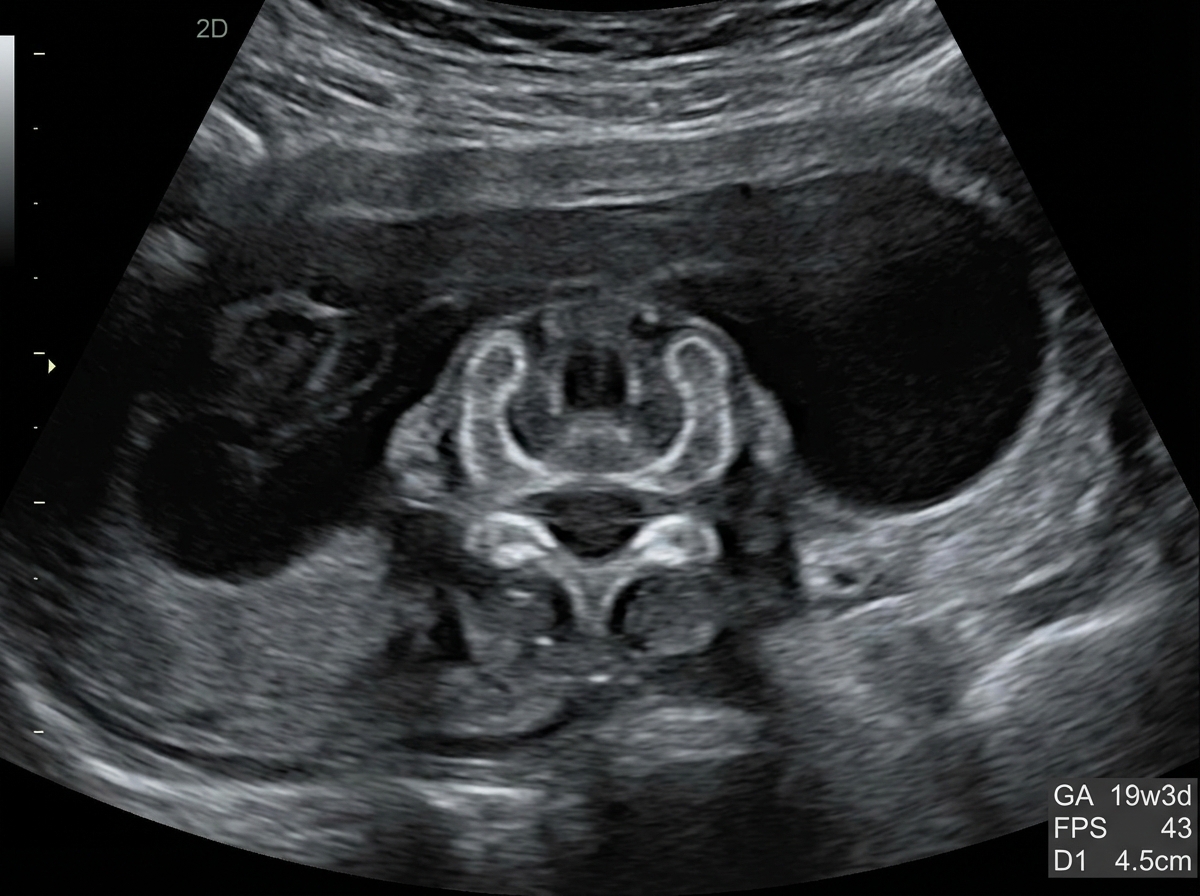
A 25-year-old pregnant woman, at 18 weeks of gestation, undergoes a routine ultrasound scan. The ultrasound images provided show below. Based on the imaging findings, what is the most likely diagnosis?
A 28-year-old married woman is anxious about conception and presents with complaints of profuse vaginal discharge. She has no history of itching. It has been 12 days since her last menstrual period (LMP). What is the most likely cause of her symptoms?
A 25-year-old woman presents with intense vaginal pruritus and pain for the past week. She says the pain is worse when she urinates. Her last menstrual period was 4 weeks ago. She is sexually active, has a single partner, and uses condoms infrequently. She denies any recent history of fevers, chills, abdominal or flank pain, or menstrual irregularities. Her past medical history is significant for systemic lupus erythematosus (SLE), diagnosed 5 years ago and managed medically. Her current medications include prednisone and oral contraceptives. The patient is afebrile and her vital signs are within normal limits. Physical examination is significant for a small amount of discharge from the vagina, along with severe inflammation and scarring. The discharge is thick, white, and has the consistency of cottage cheese. The vaginal pH is 4.1. The microscopic examination of potassium hydroxide (KOH) mount of the vaginal discharge reveals pseudohyphae. A urine pregnancy test is negative. Which of the following would be the most appropriate treatment for this patient’s condition?
A 35-year-old G0P1 female presents to her OB/GYN after 17 weeks gestation. A quad screen is performed revealing the following results: elevated inhibin and beta HCG, decreased aFP and estriol. An ultrasound was performed demonstrating increased nuchal translucency. When the fetus is born, what may be some common characteristics of the newborn if amniocentesis confirms the quad test results?
A 31-year-old G3P0020 presents to her physician for a prenatal visit at 12 weeks gestation. She does not smoke cigarettes and stopped drinking alcohol once she was diagnosed with pregnancy at 10 weeks gestation. An ultrasound examination showed the following: Ultrasound finding Measured Normal value (age-specified) Heart rate 148/min 137–150/min Crown-rump length 44 mm 45–52 mm Nasal bone visualized visualized Nuchal translucency 3.3 mm < 2.5 mm Which of the following statements regarding the presented patient is correct?
A 45-year-old primigravida woman at 13-weeks' gestation is scheduled for a prenatal evaluation. This is her first appointment, though she has known she is pregnant for several weeks. A quad screening is performed with the mother's blood and reveals the following: AFP (alpha-fetoprotein) Decreased hCG (human chorionic gonadotropin) Elevated Estriol Decreased Inhibin Elevated Ultrasound evaluation of the fetus reveals increased nuchal translucency. Which mechanism of the following mechanisms is most likely to have caused the fetus’s condition?
Practice by Chapter
First trimester screening
Practice Questions
Cell-free DNA screening
Practice Questions
Second trimester serum screening
Practice Questions
Ultrasound markers and anomaly screening
Practice Questions
Carrier screening for genetic disorders
Practice Questions
Cervical cancer screening in pregnancy
Practice Questions
Diabetes screening in pregnancy
Practice Questions
Gestational diabetes management
Practice Questions
Group B streptococcus screening
Practice Questions
Screening for preeclampsia risk factors
Practice Questions
Prenatal infection screening (TORCH, HIV, STIs)
Practice Questions
Genetic counseling principles
Practice Questions
Diagnostic testing (amniocentesis, CVS)
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
