Prenatal Care — MCQs

On this page
A 38-year-old woman, gravida 2, para 1, at 24 weeks' gestation comes to the physician for a routine prenatal evaluation. She has no history of major medical illness and takes no medications. Fetal ultrasonography shows a cardiac defect resulting from abnormal development of the endocardial cushions. This defect is most likely to result in which of the following?
A 28-year-old woman comes to the physician because she had a positive pregnancy test at home. She reports feeling nauseated and has vomited several times over the past week. During this period, she has also had increased urinary frequency. She is sexually active with her boyfriend and they use condoms inconsistently. Her last menstrual period was 5 weeks ago. Physical examination shows no abnormalities. A urine pregnancy test is positive. A pap smear is positive for a high-grade squamous intraepithelial lesion. Colposcopy shows cervical intraepithelial neoplasia grade II and III. Which of the following is the most appropriate next step in the management of this patient?
A 28-year-old woman presents with an abnormal vaginal discharge for the past week. She maintains a monogamous relationship but denies the use of barrier protection with her partner. She is 5 weeks late for her menstrual cycle. Subsequent testing demonstrates a positive pregnancy test. A wet mount demonstrates motile, pear-shaped organisms. Which of the following is the most appropriate treatment for this patient?
A 23-year-old woman gravida 2, para 1 at 12 weeks' gestation comes to the physician for her initial prenatal visit. She feels well. She was treated for genital herpes one year ago and gonorrhea 3 months ago. Medications include folic acid and a multivitamin. Vital signs are within normal limits. Pelvic examination shows a uterus consistent in size with a 12-week gestation. Urine dipstick is positive for leukocyte esterase and nitrite. Urine culture shows E. coli (> 100,000 colony forming units/mL). Which of the following is the most appropriate next step in management?
A 29-year-old woman presents to a medical office complaining of fatigue, nausea, and vomiting for 1 week. Recently, the smell of certain foods makes her nauseous. Her symptoms are more pronounced in the mornings. The emesis is clear-to-yellow without blood. She has had no recent travel out of the country. The medical history is significant for peptic ulcer, for which she takes pantoprazole. The blood pressure is 100/60 mm Hg, the pulse is 70/min, and the respiratory rate is 12/min. The physical examination reveals pale mucosa and conjunctiva, and bilateral breast tenderness. The LMP was 9 weeks ago. What is the most appropriate next step in the management of this patient?
A 16-year-old girl comes to the physician with her mother because of intermittent abdominal cramps, fatigue, and increased urination over the past 3 months. She has no history of serious illness. She reports that she has not yet had her first menstrual period. Her mother states that she receives mostly A and B grades in school and is very active in school athletics. Her mother has type 2 diabetes mellitus and her maternal aunt has polycystic ovary syndrome. Her only medication is a daily multivitamin. The patient is 150 cm (4 ft 11 in) tall and weighs 50 kg (110 lb); BMI is 22.2 kg/m2. Vital signs are within normal limits. A grade 2/6 early systolic murmur is heard best over the pulmonic area and increases with inspiration. The abdomen is diffusely tender to palpation and a firm mass is felt in the lower abdomen. Breast and pubic hair development are at Tanner stage 5. Which of the following is the most appropriate next step in management?
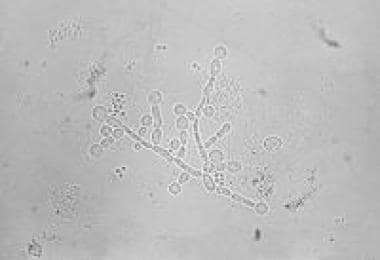
A 29-year-old woman, gravida 2, para 1, at 10 weeks' gestation comes to the physician for a prenatal visit. Over the past two weeks, she has felt nauseous in the morning and has had vulvar pruritus and dysuria that started 5 days ago. Her first child was delivered by lower segment transverse cesarean section because of macrosomia from gestational diabetes. Her gestational diabetes resolved after the child was born. She appears well. Ultrasound confirms fetal heart tones and an intrauterine pregnancy. Speculum exam shows a whitish chunky discharge. Her vaginal pH is 4.2. A wet mount is performed and microscopic examination is shown. Which of the following is the most appropriate treatment?
A 34-year-old woman, gravida 3, para 2, at 16 weeks' gestation comes to the physician because of nausea and recurrent burning epigastric discomfort for 1 month. Her symptoms are worse after heavy meals. She does not smoke or drink alcohol. Examination shows a uterus consistent in size with a 16-week gestation. Palpation of the abdomen elicits mild epigastric tenderness. The physician prescribes her medication to alleviate her symptoms. Treatment with which of the following drugs should be avoided in this patient?
A 27-year-old female in her 20th week of pregnancy presents for a routine fetal ultrasound screening. An abnormality of the right fetal kidney is detected. It is determined that the right ureteropelvic junction has failed to recanalize. Which of the following findings is most likely to be seen on fetal ultrasound:
A 23-year-old nulligravida presents for evaluation 5 weeks after her last menstrual period. Her previous menstruation cycle was regular, and her medical history is benign. She is sexually active with one partner and does not use contraception. A urine dipstick pregnancy test is negative. The vital signs are as follows: blood pressure 120/80 mm Hg, heart rate 71/min, respiratory rate 13/min, and temperature 36.8°C (98.2°F). The physical examination is notable for breast engorgement, increased pigmentation of the nipples, and linea nigra. The gynecologic examination demonstrates cervical and vaginal cyanosis. Measurement of which of the following substances is most appropriate in this case?
Practice by Chapter
Routine prenatal visit schedule
Practice Questions
Nutrition in pregnancy
Practice Questions
Weight gain recommendations
Practice Questions
Exercise in pregnancy
Practice Questions
Medication safety in pregnancy
Practice Questions
Immunizations in pregnancy
Practice Questions
Management of common pregnancy complaints
Practice Questions
Fetal growth assessment
Practice Questions
Fetal movement monitoring
Practice Questions
Antepartum fetal surveillance (NST, BPP)
Practice Questions
Anemia in pregnancy
Practice Questions
Travel during pregnancy
Practice Questions
Patient education topics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
