Prenatal Care — MCQs

On this page
A 26-year-old woman comes to the emergency department because of a 3-day history of nausea and vomiting. Her last menstrual period was 9 weeks ago. A urine pregnancy test is positive. Ultrasonography shows an intrauterine pregnancy consistent in size with a 7-week gestation. The hormone that was measured in this patient's urine to detect the pregnancy is also directly responsible for which of the following processes?
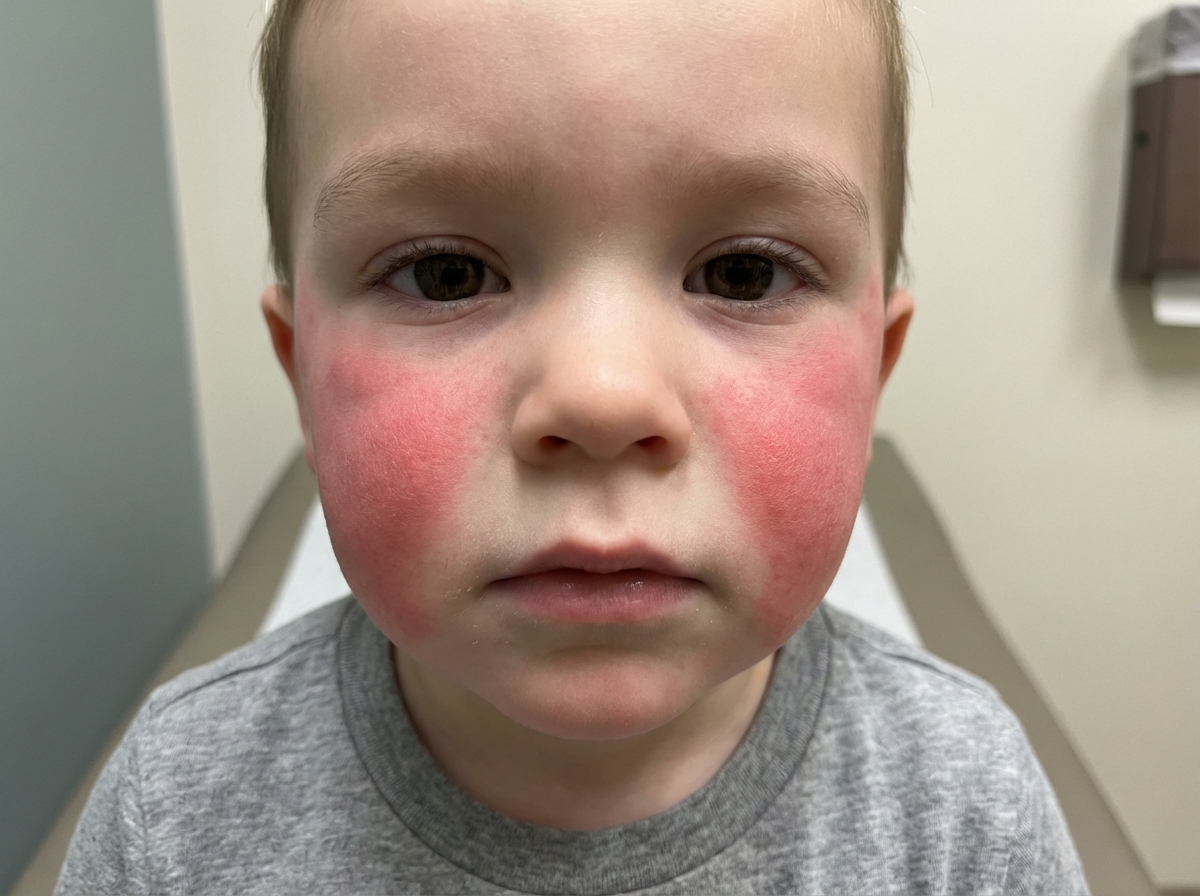
A 26-year-old woman, gravida 2, para 1, at 9 weeks' gestation comes to the physician with her 16-month-old son for her first prenatal visit. Her son has had low-grade fever, headache, and arthralgia for 5 days. He has also had a generalized rash that started on the cheeks 2 days ago and has since spread to his body. The woman has some mild nausea but is feeling well. Her first pregnancy was uneventful. Her son was delivered at 40 weeks' gestation via lower segment transverse cesarean section because of a nonreassuring fetal heart rate. Current medications include prenatal vitamins with folic acid. Preconception rubella and varicella titers were recorded as adequate. His immunizations are up-to-date. His temperature is 36.8°C (98.2°F), pulse is 85/min, respirations are 13/min, and blood pressure is 114/65 mm Hg. Pelvic examination of the woman shows a uterus consistent in size with a 9-week gestation. An image of the woman's son is shown. A complete blood cell count is within normal limits. Which of the following is the most appropriate next step in management?
A 26-year-old G1P0 woman comes to her maternal and fetal medicine doctor at 15 weeks of gestation in order to be evaluated for fetal developmental abnormalities. Her family has a history of congenital disorders leading to difficulty walking so she was concerned about her child. Amniocentesis shows normal levels of all serum proteins and circulating factors. Despite this, the physician warns that there is a possibility that there may be a neural tube abnormality in this child even though the normal results make it less likely. If this child was born with a neural tube closure abnormality, which of the following findings would most likely be seen in the child?
A 17-year-old girl comes to the physician because she had unprotected sexual intercourse the previous day. Menses have occurred at regular 28-day intervals since menarche at the age of 13 years. Her last menstrual period was 12 days ago. Physical examination shows no abnormalities. A urine pregnancy test is negative. She does not wish to become pregnant until after college and does not want her parents to be informed of this visit. Which of the following is the most appropriate step in management?
A 14-year-old girl is brought to the pediatrician by her mother. The girl's mother states that she began having her period 6 months ago. The patient states that after her first period she has had a period every 10 to 40 days. Her menses have ranged from very light flow to intense and severe symptoms. Otherwise, the patient is doing well in school, is on the track team, and has a new boyfriend. Her temperature is 98.1°F (36.7°C), blood pressure is 97/58 mmHg, pulse is 90/min, respirations are 14/min, and oxygen saturation is 99% on room air. Physical exam demonstrates an obese girl but is otherwise within normal limits. Which of the following is the most likely diagnosis?
A 26-year-old woman, G1P0, at 22 weeks of gestation presents to the clinic for a prenatal visit. Her recent pregnancy scan shows a single live intrauterine fetus with adequate fetal movements. Facial appearance shows the presence of a cleft lip. The rest of the fetal development is within normal limits. The fetal heart rate is 138/min. Her prenatal screening tests for maternal serum α-fetoprotein (MSAFP) concentration, pregnancy-associated plasma protein-A (PAPP-A), and free β-human chorionic gonadotropin (β-hCG) are within normal ranges respectively. Her past medical and surgical histories are negative. She is worried about the health of her baby. The baby is at increased risk for which of the following birth defects?
A 19-year-old female complains of abnormal facial hair growth. This has been very stressful for her, especially in the setting of not being happy with her weight. Upon further questioning you learn she has a history of type 2 diabetes mellitus. Her height is 61 inches, and weight is 185 pounds (84 kg). Physical examination is notable for facial hair above her superior lip and velvety, greyish thickened hyperpigmented skin in the posterior neck. Patient is started on a hormonal oral contraceptive. Which of the following is a property of the endometrial protective hormone found in this oral contraceptive?
A 25-year-old G1P0 woman at 22 weeks’ gestation presents to the emergency department with persistent vomiting over the past 8 weeks which has resulted in 5.5 kg (12.1 lb) of unintentional weight loss. She has not received any routine prenatal care to this point. She reports having tried diet modification and over-the-counter remedies with no improvement. The patient's blood pressure is 103/75 mm Hg, pulse is 93/min, respiratory rate is 15/min, and temperature is 36.7°C (98.1°F). Physical examination reveals an anxious and fatigued-appearing young woman, but whose findings are otherwise within normal limits. What is the next and most important step in her management?
A 28-year-old primigravid woman comes to the physician at 27 weeks' gestation with increased urinary frequency, a burning sensation when urinating, flank pain, and nausea. Her pregnancy has been uncomplicated. Glucose tolerance testing performed at 25 weeks' gestation was normal. She is sexually active with her husband. Her only medication is a prenatal vitamin. Her pulse is 90/min, respirations are 16/min, and blood pressure is 125/75 mm Hg. Physical examination shows marked tenderness in the right costovertebral area. Pelvic examination shows a uterus consistent with 27 weeks' gestation. Her urine dipstick is positive for leukocyte esterase and nitrites. The urine is sent for bacterial culture. Which of the following changes most likely contributed to this patient's condition?
A 27-year-old woman, gravida 2, para 1, at 36 weeks' gestation comes to the physician for a prenatal visit. She feels well. Fetal movements are adequate. This is her 7th prenatal visit. She had an ultrasound scan performed 1 month ago that showed a live intrauterine pregnancy consistent with a 32-week gestation with no anomalies. She had a Pap smear performed 1 year ago, which was normal. Vital signs are within normal limits. Pelvic examination shows a uterus consistent in size with a 36-week gestation. Her blood group and type is A negative. Which of the following is the most appropriate next step in management?
Practice by Chapter
Routine prenatal visit schedule
Practice Questions
Nutrition in pregnancy
Practice Questions
Weight gain recommendations
Practice Questions
Exercise in pregnancy
Practice Questions
Medication safety in pregnancy
Practice Questions
Immunizations in pregnancy
Practice Questions
Management of common pregnancy complaints
Practice Questions
Fetal growth assessment
Practice Questions
Fetal movement monitoring
Practice Questions
Antepartum fetal surveillance (NST, BPP)
Practice Questions
Anemia in pregnancy
Practice Questions
Travel during pregnancy
Practice Questions
Patient education topics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
