Prenatal Care — MCQs

On this page
A 22-year-old G1P1 woman comes to the clinic asking about “the morning after pill.” She reports that she had sexual intercourse with her boyfriend last night and she thinks the condom broke. She is not using any other form of contraception. She reports her last menstrual period was 10 days ago, and they are normally regular. The patient’s medical history is significant for obesity, asthma and allergic rhinitis. Her medications include albuterol and occasional intranasal corticosteroids. She has no history of sexually transmitted diseases and is sexually active with only her current boyfriend of 5 years. The patient denies genitourinary symptoms. Her temperature is 98°F (36.7°C), blood pressure is 112/74 mmHg, pulse is 63/min, and respirations are 12/min with an oxygen saturation of 99% O2 on room air. Physical examination, including a pelvic exam, shows no abnormalities. The patient is worried because she is back in graduate school and cannot afford another child. Which of the following is the most effective emergency contraception?
A 37-year-old woman, gravida 3, para 3, comes to the physician for a follow-up examination. She gave birth to her third child 8 months ago and now wishes to start a contraception method. Prior to her most recent pregnancy, she used a combined estrogen-progestin pill. Which of the following aspects of her history would be a contraindication for restarting an oral contraceptive pill?
A 22-year-old woman comes to the physician because of a 1-week history of nausea and vomiting. She has not had fever, abdominal pain, diarrhea, or vaginal bleeding. She does not remember the date of her last menstrual period. She uses oral contraceptive pills but occasionally forgot to take them. She had pelvic inflammatory disease 2 years ago and was treated with antibiotics. Her temperature is 37°C (98.6°F), pulse is 110/min, respirations are 16/min, and blood pressure is 118/75 mm Hg. Physical examination shows no abnormalities. Pelvic examination shows a normal appearing vagina, cervix, uterus, and adnexa. A urine pregnancy test is positive. Her serum β-human chorionic gonadotropin concentration is 805 mIU/mL. Which of the following is the most appropriate next step in diagnosis?
A healthy 31-year-old woman comes to the physician because she is trying to conceive. She is currently timing the frequency of intercourse with at-home ovulation test kits. An increase in the levels of which of the following is the best indicator that ovulation has occurred?
A 17-year-old girl comes to your outpatient clinic. She is sexually active with multiple partners and requests a prescription for oral contraceptive pills. A urine pregnancy test in your office is negative. Which of the following is the most appropriate next step?
A 28-year-old woman, gravida 1, para 0, at 10 weeks' gestation comes to the physician for her initial prenatal visit. She has no history of serious illness, but reports that she is allergic to penicillin. Vital signs are within normal limits. The lungs are clear to auscultation, and cardiac examination shows no abnormalities. Transvaginal ultrasonography shows an intrauterine pregnancy with no abnormalities. The fetal heart rate is 174/min. Routine prenatal laboratory tests are drawn. Rapid plasma reagin (RPR) test is 1:128 and fluorescent treponemal antibody absorption test (FTA-ABS) is positive. Which of the following is the most appropriate next step in management?
A 24-year-old G1P0000 presents for her first obstetric visit and is found to be at approximately 8 weeks gestation. She has no complaints aside from increased fatigue and occasional nausea. The patient is a recent immigrant from Africa and is currently working as a babysitter for several neighborhood children. One of them recently had the flu, and another is home sick with chickenpox. The patient has no immunization records and does not recall if she has had any vaccinations. She is sexually active with only her husband, has never had a sexually transmitted disease, and denies intravenous drug use. Her husband has no past medical history. Exam at this visit is unremarkable. Her temperature is 98.7°F (37.1°C), blood pressure is 122/76 mmHg, pulse is 66/min, and respirations are 12/min. Which of the following immunizations should this patient receive at this time?
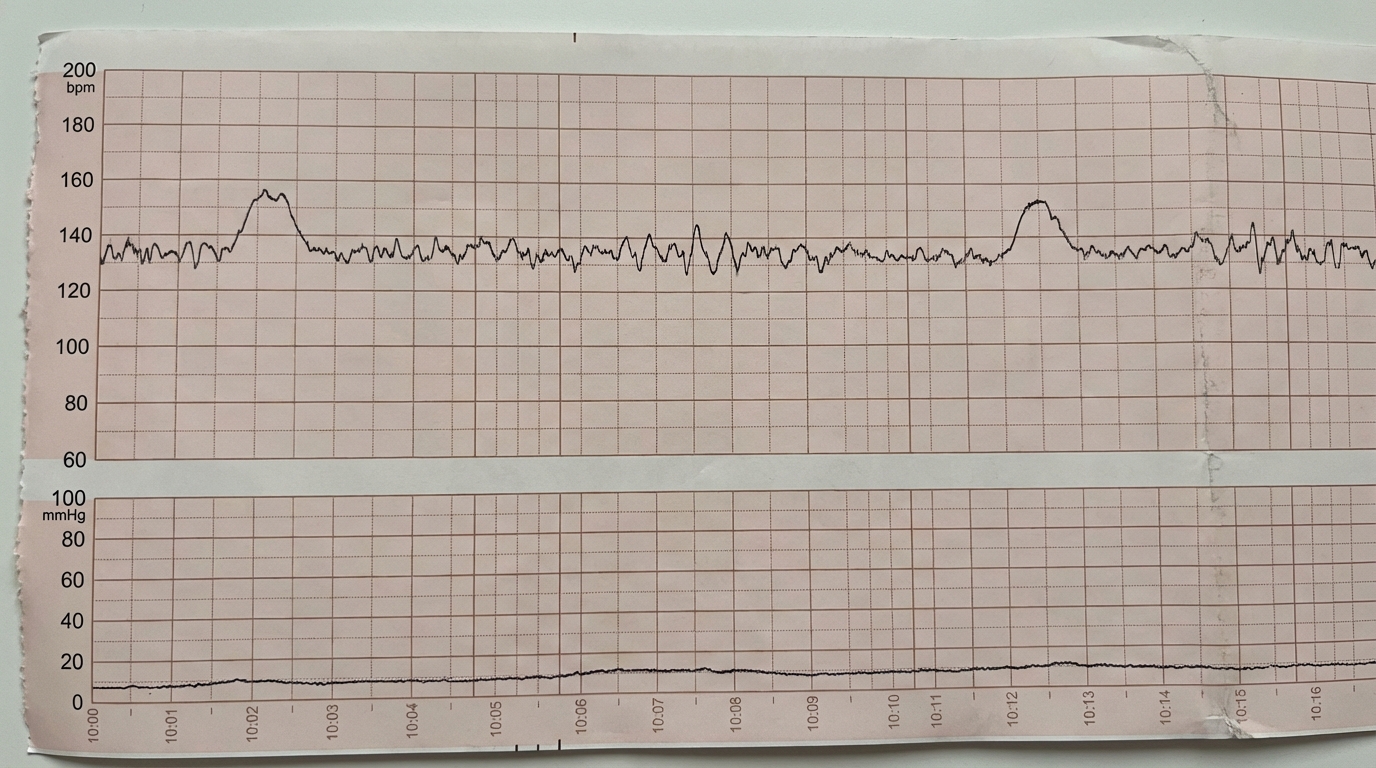
A 27-year-old woman, gravida 2, para 1, at 32 weeks' gestation comes to the physician for a prenatal visit. She feels that her baby's movements have decreased recently. She says that she used to feel 10–12 movements/hour earlier, but that it has recently decreased to about 7–8/hour. Pregnancy and delivery of her first child were uncomplicated. Medications include folic acid and a multivitamin. Her temperature is 37.2°C (99°F), and blood pressure is 108/60 mm Hg. Pelvic examination shows a uterus consistent in size with a 32-week gestation. The fetus is in a transverse lie presentation. The fetal heart rate is 134/min. A 14-minute recording of the nonstress test is shown. Which of the following is the most appropriate next step in managing this patient?
A 36-year-old woman presents with a whitish vaginal discharge over the last week. She also complains of itching and discomfort around her genitals. She says her symptoms are getting progressively worse. She has been changing her undergarments frequently and changed the brand of detergent she uses to wash her clothes, but it did not resolve her problem. Additionally, she admits to having painful urination and increased urinary frequency for the past one month, which she was told are expected side effects of her medication. The patient denies any recent history of fever or malaise. She has 2 children, both delivered via cesarean section in her late twenties. Past medical history is significant for hypertension and diabetes mellitus type 2. Current medications are atorvastatin, captopril, metformin, and empagliflozin. Her medications were changed one month ago to improve her glycemic control, as her HbA1c at that time was 7.5%. Her vital signs are a blood pressure of 126/84 mm Hg and a pulse of 78/min. Her fingerstick glucose is 108 mg/dL. Pelvic examination reveals erythema and mild edema of the vulva. A thick, white, clumpy vaginal discharge is seen. The vaginal pH is 4.0. Microscopic examination of a KOH-treated sample of the discharge demonstrates lysis of normal cellular elements with branching pseudohyphae. Which of the following is the next best step in the management of this patient?
A 23-year-old woman presented to the clinic for her first prenatal appointment with fatigue and pain in the perineum for the past 8 days. The past medical history is benign and she claimed to have only had unprotected intercourse with her husband. She had a documented allergic reaction to amoxicillin 2 years ago. The vaginal speculum exam revealed a clean, ulcerated genital lesion, which was tender and non-exudative. No lymphadenopathy was detected. A rapid plasma reagin (RPR) test revealed a titer of 1:64 and the fluorescent treponemal antibody absorption (FTA- abs) test was positive. What is the next best step in the management of this patient?
Practice by Chapter
Routine prenatal visit schedule
Practice Questions
Nutrition in pregnancy
Practice Questions
Weight gain recommendations
Practice Questions
Exercise in pregnancy
Practice Questions
Medication safety in pregnancy
Practice Questions
Immunizations in pregnancy
Practice Questions
Management of common pregnancy complaints
Practice Questions
Fetal growth assessment
Practice Questions
Fetal movement monitoring
Practice Questions
Antepartum fetal surveillance (NST, BPP)
Practice Questions
Anemia in pregnancy
Practice Questions
Travel during pregnancy
Practice Questions
Patient education topics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
