Immunizations in pregnancy — MCQs

A 21-year-old woman, gravida 1, para 0, at 39 weeks' gestation comes to the physician for a prenatal visit. She has some mild edema and tiredness but generally feels well. She recently had a nephew visiting for 1 week who became ill and was diagnosed with the chickenpox. She has no history of chickenpox and is not vaccinated against the varicella zoster virus. Current medications include folic acid supplements and a prenatal vitamin. Her temperature is 37°C (98.6°F), pulse is 82/min, respirations are 15/min, and blood pressure is 116/64 mm Hg. Pelvic examination shows a uterus consistent in size with 39 weeks' gestation. IgG antibody titers for varicella zoster virus are negative. Which of the following is the most appropriate next step in management?
A 23-year-old woman presents to her physician requesting the chickenpox vaccine. She is also complaining of nausea, malaise, and moderate weight gain. She developed these symptoms gradually over the past 2 weeks. She reports no respiratory or cardiovascular disorders. Her last menstruation was about 6 weeks ago. She has one sexual partner and uses a natural planning method for contraception. Her vital signs include: blood pressure 110/70 mm Hg, heart rate 92/min, respiratory rate 14/min, and temperature 37.2℃ (99℉). The physical examination shows non-painful breast engorgement and nipple hyperpigmentation. There is no neck enlargement and no palpable nodules in the thyroid gland. The urine beta-hCG is positive. What is the proper recommendation regarding chickenpox vaccination in this patient?
A 40-year-old pregnant woman, G4 P3, visits your office at week 30 of gestation. She is very excited about her pregnancy and wants to be the healthiest she can be in preparation for labor and for her baby. What vaccination should she receive at this visit?
A 27-year-old G2P1 woman is diagnosed with an HIV infection after undergoing routine prenatal blood work testing. Her estimated gestational age by first-trimester ultrasound is 12 weeks. Her CD4 count is 150 cells/mm^3 and her viral load is 126,000 copies/mL. She denies experiencing any symptoms of HIV infection. Which of the following is appropriate management of this patient's pregnancy?
A 34-year-old woman, gravida 2, para 0, at 28 weeks' gestation comes to the physician for a prenatal visit. She has not had regular prenatal care. Her most recent ultrasound at 20 weeks of gestation confirmed accurate fetal dates and appropriate fetal development. She takes levothyroxine for hypothyroidism. She used to work as a nurse before she emigrated from Brazil 13 years ago. She lost her immunization records during the move and cannot recall all of her vaccinations. She appears well. Vital signs are within normal limits. Physical examination shows a fundal height of 26 cm and no abnormalities. An ELISA test for HIV is negative. Serology testing shows hepatitis B surface antibody positive, hepatitis B core antibody and surface antigen negative, and hepatitis A antibody negative. Hepatitis C antibody is positive with detectable RNA. Given her incomplete vaccination history and current serologic results, which of the following vaccinations is most appropriate to recommend at this time?
A 34-year-old gravida 5, para 4 presents to the physician for prenatal care at 32 weeks of pregnancy. She comes from a rural region of Ethiopia and did not have appropriate prenatal care during previous pregnancies. She has no complaints of swelling, contractions, loss of fluid, or bleeding from the vagina. During her current pregnancy, she has received proper care and has completed the required laboratory and instrumental tests, which did not show any pathology. Her blood pressure is 130/70 mm Hg, heart rate is 77/min, respiratory rate is 15/min, and temperature is 36.6°C (97.8°F). Her examination is consistent with a normal 32-weeks’ gestation. The patient tells the physician that she is going to deliver her child at home, without any medical aid. The physician inquires about her tetanus vaccination status. The patient reports that she had tetanus 1 year after her first delivery at the age of 16, and it was managed appropriately. She had no tetanus vaccinations since then. Which of the following statements is true?
A 24-year-old newly immigrated mother arrives to the clinic to discuss breastfeeding options for her newborn child. Her medical history is unclear as she has recently arrived from Sub-Saharan Africa. You tell her that unfortunately she will not be able to breastfeed until further testing is performed. Which of the following infections is an absolute contraindication to breastfeeding?
A 29-year-old woman presents to a medical office complaining of fatigue, nausea, and vomiting for 1 week. Recently, the smell of certain foods makes her nauseous. Her symptoms are more pronounced in the mornings. The emesis is clear-to-yellow without blood. She has had no recent travel out of the country. The medical history is significant for peptic ulcer, for which she takes pantoprazole. The blood pressure is 100/60 mm Hg, the pulse is 70/min, and the respiratory rate is 12/min. The physical examination reveals pale mucosa and conjunctiva, and bilateral breast tenderness. The LMP was 9 weeks ago. What is the most appropriate next step in the management of this patient?
A 23-year-old primigravid woman comes to the physician at 36 weeks' gestation for her first prenatal visit. She confirmed the pregnancy with a home urine pregnancy kit a few months ago but has not yet followed up with a physician. She takes no medications. Vital signs are within normal limits. Pelvic examination shows a uterus consistent in size with a 36-week gestation. Laboratory studies show: Hemoglobin 10.6 g/dL Serum Glucose 88 mg/dL Hepatitis B surface antigen negative Hepatitis C antibody negative HIV antibody positive HIV load 11,000 copies/mL (N < 1000 copies/mL) Ultrasonography shows an intrauterine fetus consistent in size with a 36-week gestation. Which of the following is the most appropriate next step in management of this patient?
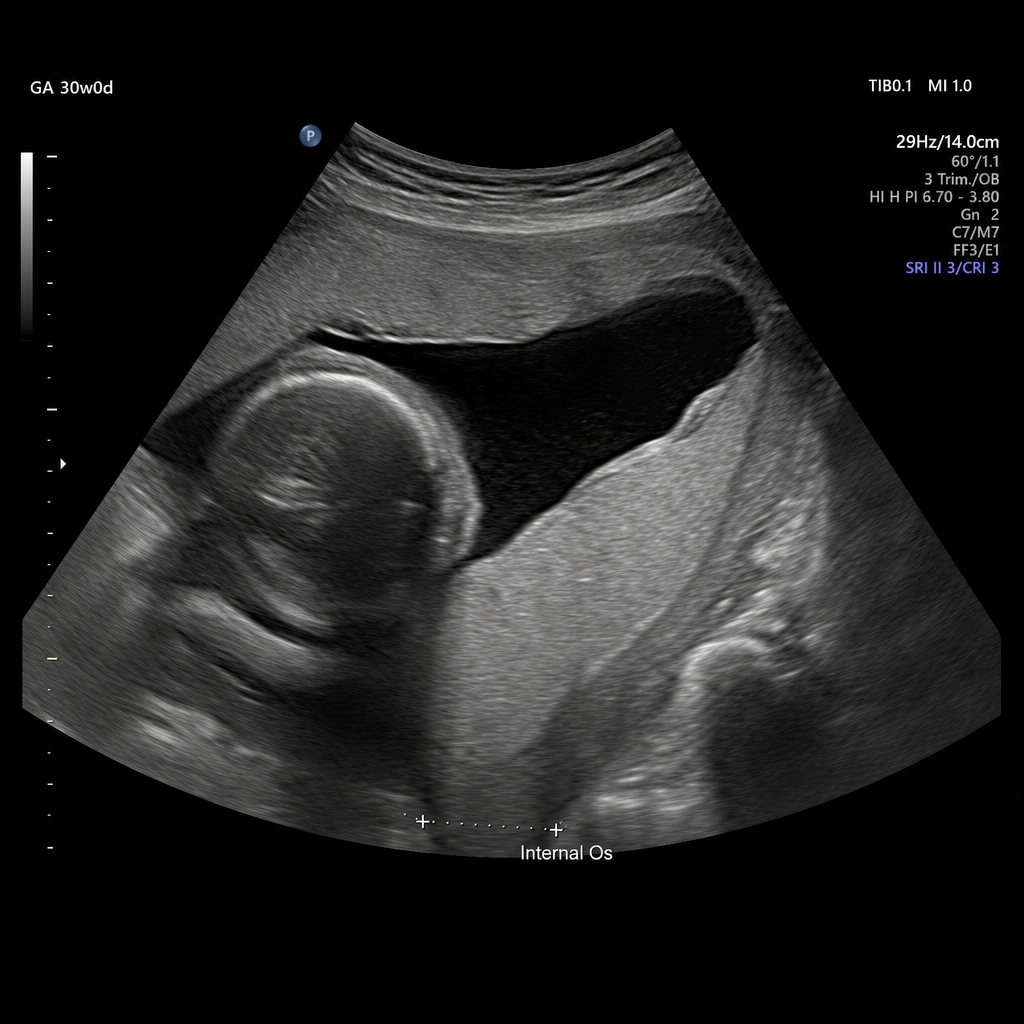
A 25-year-old woman, G1P0, at 30 weeks of gestation is brought to the emergency department with sudden-onset painless bright red vaginal bleeding. She reports two prior episodes of spotting over the past 3 weeks. Vital signs: BP 110/70 mmHg, HR 98 bpm, RR 16/min. Fetal heart rate tracing shows a baseline of 145 bpm with moderate variability and no decelerations. Transabdominal ultrasound shows placenta completely covering the internal os. Which of the following is the most appropriate immediate management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
