Postpartum hemorrhage — MCQs

On this page
A 36-year-old woman comes to the physician because of progressively worsening painful swelling of both breasts for the past 24 hours. Three days ago, she vaginally delivered a healthy 2690-g (5-lb 15-oz) girl. The patient says that breastfeeding her newborn daughter is very painful. She reports exhaustion and moodiness. She has no history of serious illness. Medications include folic acid and a multivitamin. Her temperature is 37.4°C (99.3°F). Examination shows tenderness, firmness, and fullness of both breasts. The nipples appear cracked and the areolas are swollen bilaterally. Which of the following is the most appropriate next step in management?
A 27-year-old woman, gravida 1, para 1, presents to the obstetrics and gynecology clinic because of galactorrhea, fatigue, cold intolerance, hair loss, and unintentional weight gain for the past year. She had placenta accreta during her first pregnancy with an estimated blood loss of 2,000 mL. Her past medical history is otherwise unremarkable. Her vital signs are all within normal limits. Which of the following is the most likely cause of her symptoms?
A 30-year-old woman, gravida 2, para 1, abortus 1, comes to the physician because of failure to conceive for 12 months. She is sexually active with her husband 2–3 times per week. Her first child was born at term after vaginal delivery 2 years ago. At that time, the postpartum course was complicated by hemorrhage from retained placental products, and the patient underwent dilation and curettage. Menses occur at regular 28-day intervals and previously lasted for 5 days with normal flow, but now last for 2 days with significantly reduced flow. She stopped taking oral contraceptives 1 year after the birth of her son. Her vital signs are within normal limits. Speculum examination shows a normal vagina and cervix. The uterus is normal in size, and no adnexal masses are palpated. Which of the following is the most appropriate next step in management?
A 27-year-old woman, gravida 2, para 1, at 38 weeks' gestation comes to the emergency department in active labor. She received all of her prenatal care for this pregnancy. Pregnancy and delivery of her first child were uncomplicated. The patient's blood type is Rh-negative. Four hours after arrival, a healthy 3650-g (8-lb) female newborn is delivered. Delivery of the fetus is followed by placental retention and heavy vaginal bleeding. One hour later, the placenta is manually removed and the bleeding ceases. The mother's temperature is 36.7°C (98.1°F), pulse is 90/min, and blood pressure is 110/60 mm Hg. Examination shows blood on the vulva, the introitus, and on the medial aspect of each thigh. The neonate's blood type is Rh-positive. A single dose of anti-D immune globulin is administered. Which of the following is the most appropriate next step in management?
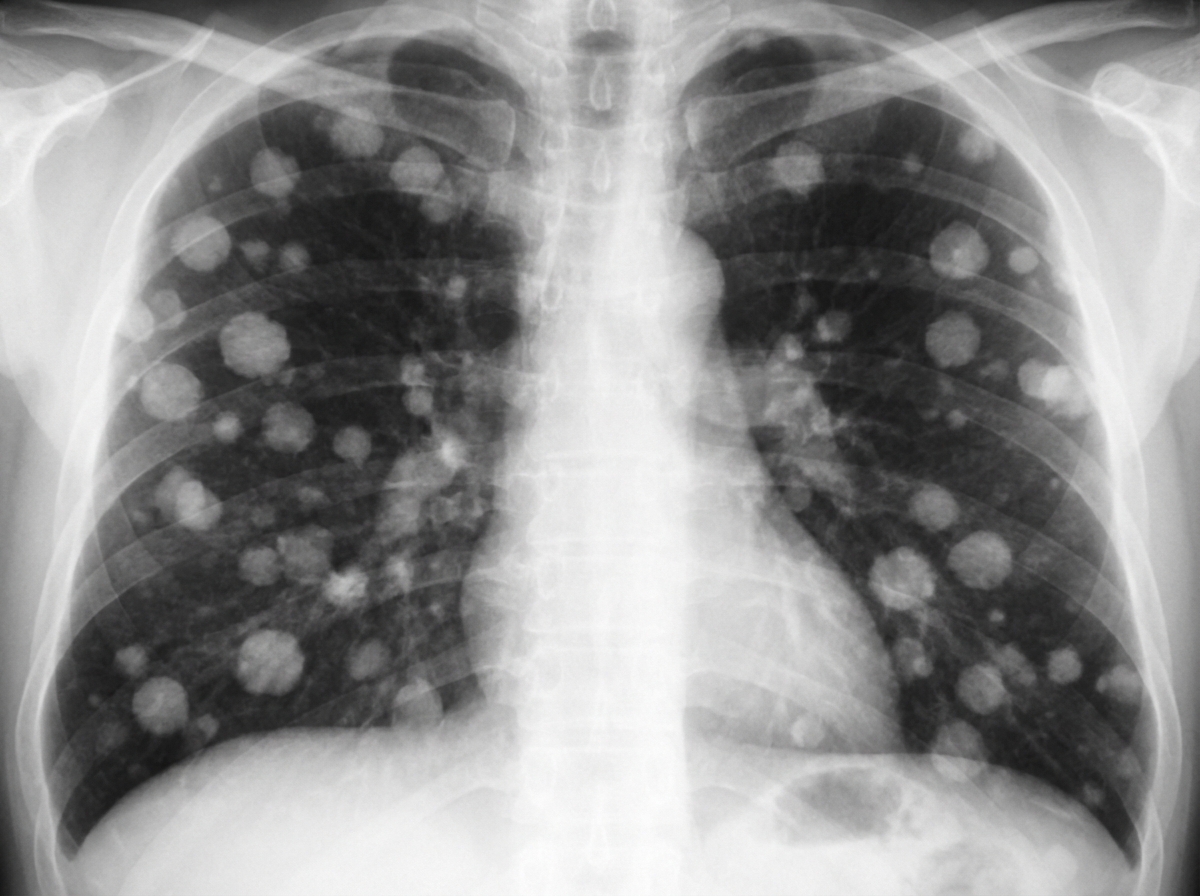
A previously healthy 32-year-old woman comes to the physician because of a 1-week history of progressively worsening cough with blood-tinged sputum, shortness of breath at rest, and intermittent left-sided chest pain. She has some mild vaginal bleeding since she had a cesarean delivery 6 weeks ago due to premature rupture of membranes and fetal distress at 38 weeks' gestation. She has been exclusively breastfeeding her child. Her temperature is 37°C (98.6°F), pulse is 95/min, respirations are 22/min, and blood pressure is 110/80 mm Hg. Breath sounds are decreased in the left lung base. The fundal height is 20 cm. Pelvic examination shows scant vaginal bleeding. Chest x-ray is shown. Further evaluation is most likely to reveal which of the following?
A 27-year-old G1P1001 is recovering in the postpartum unit three days after a Caesarean section. Her surgery was indicated for breech presentation of the infant. She was at 40 weeks and 2 days gestation at the time of delivery. The patient is now complaining of purulent discharge and continued heavy bleeding. She also notes difficulty and discomfort with urination. The patient’s prenatal course was complicated by one episode of pyelonephritis, which was treated with intravenous ceftriaxone and suppression nitrofurantoin for the remainder of the pregnancy. The patient has a medical history of generalized anxiety disorder and atopic dermatitis. On the third postpartum day, her temperature is 101.2°F (38.4°C), pulse is 112/min, blood pressure is 118/71 mmHg, and respirations are 13/min. Exam reveals that she is uncomfortable and diaphoretic. Her lochia is purulent with several blood clots, and her uterus is slightly boggy and soft. There is mild tenderness with uterine manipulation. Which of the following is the best next step in management for this patient's condition?
A 37-year-old G1P1001 presents for her 6-week postpartum visit after delivering a male infant by spontaneous vaginal delivery at 41 weeks and 5 days gestation. She notes that five days ago, her right breast began to hurt, and the skin near her nipple turned red. She also states that she has felt feverish and generally achy for 2 days but thought she was just sleep deprived. The patient’s son has been having difficulty latching for the last 2 weeks and has begun receiving formula in addition to breast milk, though the patient wishes to continue breastfeeding. She is generally healthy with no past medical history but has smoked half a pack per day for the last 15 years. Her mother died from breast cancer at the age of 62, and her father has hypertension and coronary artery disease. At this visit, her temperature is 100.6° F (38.1° C), blood pressure is 116/73 mmHg, pulse is 80/min, and respirations are 14/min. She appears tired and has a slightly flat affect. Examination reveals a 4x4 cm area of erythema on the lateral aspect near the nipple on the right breast. In the center of this area, there is a fluctuant, tender mass that measures 2x2 cm. The overlying skin is intact. The remainder of her exam is unremarkable. Which of the following is the best next step in management?
A 27-year-old woman, gravida 3, para 2, at 41 weeks' gestation is admitted to the hospital in active labor. Her pregnancy has been uncomplicated. Both of her prior children were delivered by vaginal birth. She has a history of asthma. Current medications include iron and vitamin supplements. After a prolonged labor, she undergoes vaginal delivery. Shortly afterwards, she begins to have heavy vaginal bleeding with clots. Her temperature is 37.2°C (98.9°F), pulse is 90/min, respirations are 17/min, and blood pressure is 130/72 mm Hg. Examination shows a soft, enlarged, and boggy uterus on palpation. Laboratory studies show: Hemoglobin 10.8 g/dL Hematocrit 32.3% Leukocyte Count 9,000/mm3 Platelet Count 140,000/mm3 Prothrombin time 14 seconds Partial thromboplastin time 38 seconds Her bleeding continues despite bimanual uterine massage and administration of oxytocin. Which of the following is the most appropriate next step in management?
A 26-year-old woman presents to her physician at the 3rd week postpartum with a fever and a swollen breast with redness and tenderness. She has been breastfeeding her infant since birth. The symptoms of the patient started 4 days ago. She has not taken any antibiotics for the past 12 months. She does not have any concurrent diseases. The vital signs include: blood pressure 110/80 mm Hg, heart rate 91/min, respiratory rate 15/min, and temperature 38.8℃ (101.8℉). Physical examination reveals redness and enlargement of the right breast. The breast is warm and is painful at palpation. There is purulent discharge from the nipple. No fluctuation is noted. Which of the following is a correct management strategy for this patient?
A 32-year-old woman presents to her primary care doctor complaining of increased fatigue and cold intolerance after her recent delivery. The patient delivered a healthy 39-week-old boy 3 weeks ago via spontaneous vaginal delivery. Delivery was complicated by postpartum hemorrhage requiring admission to the intensive care unit with blood transfusions. Pregnancy was otherwise uneventful, and the baby is healthy. The mother has had some difficulty with lactation, but is able to supplement her breast milk with formula feeds. On exam, her temperature is 97.7°F (36.5°C), blood pressure is 112/78 mmHg, pulse is 62/min, and respirations are 12/min. The patient does not have any neck masses or lymphadenopathy; however, her skin appears dry and rough. Which of the following serum lab abnormalities may be expected?
Practice by Chapter
Definition and classification
Practice Questions
Risk factors for postpartum hemorrhage
Practice Questions
Uterine atony management
Practice Questions
Retained placenta management
Practice Questions
Genital tract trauma repair
Practice Questions
Coagulation disorders in obstetrics
Practice Questions
Medical management of PPH
Practice Questions
Surgical management of PPH
Practice Questions
Balloon tamponade techniques
Practice Questions
Uterine compression sutures
Practice Questions
Postpartum hemorrhage protocols
Practice Questions
Blood product replacement strategies
Practice Questions
Prevention of postpartum hemorrhage
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
