Labor Complications — MCQs

On this page
A 30-year-old woman, gravida 2, para 1, at 31 weeks' gestation is admitted to the hospital because her water broke one hour ago. Pregnancy has been complicated by iron deficiency anemia and hypothyroidism treated with iron supplements and L-thyroxine, respectively. The patient followed-up with her gynecologist on a regular basis throughout the pregnancy. Pregnancy and delivery of her first child were uncomplicated. Pulse is 90/min, respirations are 17/min, and blood pressure is 130/80 mm Hg. The abdomen is nontender. She has had 8 contractions within the last hour. Pelvic examination shows cervical dilation of 3 cm. The fetal heart rate is 140/min with no decelerations. In addition to administration of dexamethasone and terbutaline, which of the following is the most appropriate next step in the management of this patient?
A 39-year-old woman, gravida 4, para 4, comes to the physician because of a 5-month history of painful, heavy menses. Menses previously occurred at regular 28-day intervals and lasted 3 days with normal flow. They now last 7–8 days and the flow is heavy with the passage of clots. Pelvic examination shows a tender, uniformly enlarged, flaccid uterus consistent in size with an 8-week gestation. A urine pregnancy test is negative. Which of the following is the most likely cause of this patient's findings?
A 46-year-old woman presents to the clinic complaining that she “wets herself.” She states that over the past year she has noticed increased urinary leakage. At first it occurred only during her job, which involves restocking shelves with heavy appliances. Now she reports that she has to wear pads daily because leakage of urine will occur with simply coughing or sneezing. She denies fever, chills, dysuria, hematuria, or flank pain. She has no significant medical or surgical history, and takes no medications. Her last menstrual period was 8 months ago. She has 3 healthy daughters that were born by vaginal delivery. Which of the following tests, if performed, would most likely identify the patient’s diagnosis?
A 68-year-old woman comes to the physician for the evaluation of loss of urine for the last year. The patient states that she loses control over her bladder when walking or standing up. She reports frequent, small-volume urine losses with no urge to urinate prior to the leakage. She tried to strengthen her pelvic muscles with supervised Kegel exercises and using a continence pessary but her symptoms did not improve. The patient is sexually active with her husband. She has type 2 diabetes mellitus controlled with metformin. She does not smoke or drink alcohol. Vital signs are within normal limits. Her hemoglobin A1c is 6.3% and fingerstick blood glucose concentration is 110 mg/dL. Which of the following is the most appropriate next step in the management of this patient?
A 37-year-old woman presents with an inability to void in the hours after giving birth to her first child via vaginal delivery. Her delivery involved the use of epidural anesthesia as well as pelvic trauma from the use of forceps. She is currently experiencing urinary leakage and complains of increased lower abdominal pressure. Which of the following is the most appropriate treatment for this patient’s condition?
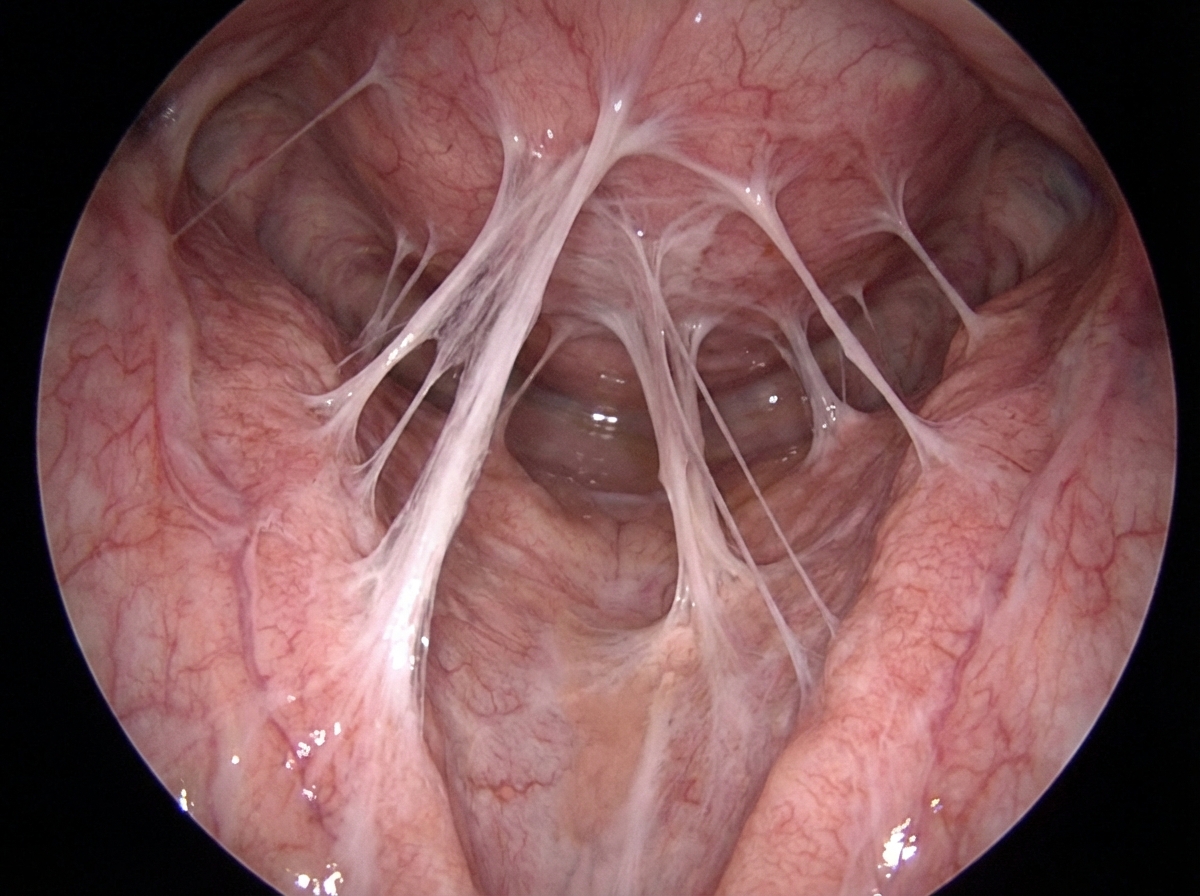
A 28-year-old woman and her husband are admitted to the office due to difficulties conceiving a child for the past year. Her menarche was at the age of 15 years, and her periods have been regular since then. Her medical history is positive for an abortion with curettage 5 years ago. A spermogram on the partner is performed, and it shows motile sperm cells. An ultrasound is performed on the patient and it is unremarkable. The laboratory results show that the FSH, LH, TSH, and prolactin levels are within normal ranges. A hysteroscopy is additionally performed and multiple adhesions are found in the uterus (refer to the image). Which of the following is the most likely composition of the scar tissue present in the uterus?
A previously healthy 29-year-old Taiwanese woman comes to the emergency department with vaginal bleeding and pelvic pressure for several hours. Over the past 2 weeks, she had intermittent nausea and vomiting. A home urine pregnancy test was positive 10 weeks ago. She has had no prenatal care. Her pulse is 80/min and blood pressure is 150/98 mm Hg. Physical examination shows warm and moist skin. Lungs are clear to auscultation bilaterally. Her abdomen is soft and non-distended. Bimanual examination shows a uterus palpated at the level of the umbilicus. Her serum beta human chorionic gonadotropin concentration is 110,000 mIU/mL. Urine dipstick is positive for protein and ketones. Transvaginal ultrasound shows a central intrauterine mass with hypoechoic spaces; there is no detectable fetal heart rate. An x-ray of the chest shows no abnormalities. Which of the following is the most appropriate next step in management?
A 17-year-old woman presents to an OBGYN clinic for evaluation of primary amenorrhea. She is a well-developed well-nourished woman who looks at her stated age. She has reached Tanner stage IV breast and pubic hair development. The external genitalia is normal in appearance. She has an older sister who underwent menarche at 12 years of age. A limited pelvic exam reveals a shortened vaginal canal with no cervix. No uterus is visualized during an ultrasound exam, but both ovaries are noted. What is the likely pathophysiology underlying this condition?
A 22-year-old woman comes to the physician for a routine health maintenance examination. She has no history of serious illness. Pelvic examination shows a pink, 2 x 2-cm, fluctuant swelling at the right posterior vaginal introitus. The swelling is most likely derived from which of the following structures?
A 27-year-old woman G2P1 at 34 weeks estimated gestational age presents with bouts of sweating, weakness, and dizziness lasting a few minutes after lying down on the bed. She says symptoms resolve if she rolls on her side. She reports that these episodes have occurred several times over the last 3 weeks. On lying down, her blood pressure is 90/50 mm Hg and her pulse is 50/min. When she rolls on her side, her blood pressure slowly increases to 120/65 mm Hg, and her pulse increases to 72/min. Which of the following best describes the mechanism which underlies this patient’s most likely condition?
Practice by Chapter
Preterm labor management
Practice Questions
Premature rupture of membranes
Practice Questions
Chorioamnionitis
Practice Questions
Abnormal labor patterns
Practice Questions
Shoulder dystocia management
Practice Questions
Umbilical cord prolapse
Practice Questions
Malpresentations (breech, face, brow)
Practice Questions
Trial of labor after cesarean
Practice Questions
Uterine rupture
Practice Questions
Placental abruption
Practice Questions
Placenta previa
Practice Questions
Amniotic fluid embolism
Practice Questions
Fetal heart rate abnormalities
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
