Amniotic fluid embolism — MCQs

A 35-year-old G3P2 woman currently 39 weeks pregnant presents to the emergency department with painful vaginal bleeding shortly after a motor vehicle accident in which she was a passenger. She had her seat belt on and reports that the airbag deployed immediately upon her car's impact against a tree. She admits that she actively smokes cigarettes. Her prenatal workup is unremarkable. Her previous pregnancies were remarkable for one episode of chorioamnionitis that resolved with antibiotics. Her temperature is 98.6°F (37°C), blood pressure is 90/60 mmHg, pulse is 130/min, and respirations are 20/min. The fetal pulse is 110/min. Her uterus is tender and firm. The remainder of her physical exam is unremarkable. What is the most likely diagnosis?
A 26-year-old primigravid woman at 39 weeks' gestation is admitted to the hospital in active labor. Pregnancy was complicated by mild oligohydramnios detected a week ago, which was managed with hydration. Her pulse is 92/min, respirations are 18/min, and blood pressure is 134/76 mm Hg. Pelvic examination shows 100% cervical effacement and 10 cm cervical dilation; the vertex is at 0 station. Cardiotocography is shown. Which of the following is the most appropriate next step in management?
A 35-year-old G1 is brought to the emergency department because of sharp pains in her abdomen. She is at 30 weeks gestation based on ultrasound. She complains of feeling a little uneasy during the last 3 weeks of her pregnancy. She mentions that her abdomen has not been enlarging as expected and her baby is not moving as much as during the earlier part of the pregnancy. If anything, she noticed her abdomen has decreased in size. While she is giving her history, the emergency medicine physician notices that she is restless and is sweating profusely. An ultrasound is performed and her blood is sent for type and match. The blood pressure is 90/60 mm Hg, the pulse is 120/min, and the respiratory rate is 18/min. The fetal ultrasound is significant for no fetal heart motion or fetal movement. Her blood work shows the following: hemoglobin, 10.3 g/dL; platelet count, 1.1*10(5)/ml; bleeding time, 10 minutes; PT, 25 seconds; and PTT, 45 seconds. Which of the following would be the best immediate course of management for this patient?
A 25-year-old woman with bipolar disorder and schizophrenia presents to the emergency room stating that she is pregnant. She says that she has been pregnant since she was 20 years old and is expecting a baby now that she is breathing much harder and feeling more faint with chest pain caused by deep breaths. Her hospital medical record shows multiple negative pregnancy tests over the past 5 years. The patient has a 20 pack-year smoking history. Her temperature is 98°F (37°C), blood pressure is 100/60 mmHg, pulse is 110/min, respirations are 28/min, and oxygen saturation is 90% on room air. Her fingerstick glucose is 100 mg/dL. She has a large abdominal pannus which is soft and nontender. Her legs are symmetric and non-tender. Oxygen is provided via nasal cannula. Her urine pregnancy test comes back positive and an initial chest radiograph is unremarkable. What is the next best step in diagnosis?
A 38-year-old primigravid woman at 34 weeks' gestation comes to the emergency department because of progressive shortness of breath for 3 hours. At a prenatal visit 2 weeks earlier, she was diagnosed with gestational hypertension. Amniocentesis with chromosomal analysis was performed at 16 weeks' gestation and showed no abnormalities. The patient has been otherwise healthy, except for a deep venous thrombosis 2 years ago that was treated with low molecular weight heparin. Her current medications include methyldopa and a multivitamin. She appears anxious. Her pulse is 90/min, respirations are 24/min, and blood pressure is 170/100 mm Hg. Crackles are heard over both lung bases. Pelvic examination shows a uterus consistent in size with a 32-week gestation. Examination of the heart, abdomen, and extremities shows no abnormalities. Which of the following is the most likely cause of this patient's shortness of breath?
A 32-year-old woman, gravida 2, para 1, at 38 weeks' gestation comes to the emergency department because of vaginal bleeding for the past hour. The patient reports that she felt contractions prior to the onset of the bleeding, but the contractions stopped after the bleeding started. She also has severe abdominal pain. Her first child was delivered by lower segment transverse cesarean section because of a nonreassuring fetal heart rate. Her pulse is 110/min, respirations are 17/min, and blood pressure is 90/60 mm Hg. Examination shows diffuse abdominal tenderness with no rebound or guarding; no contractions are felt. The fetal heart rate shows recurrent variable decelerations. Which of the following is the most likely diagnosis?
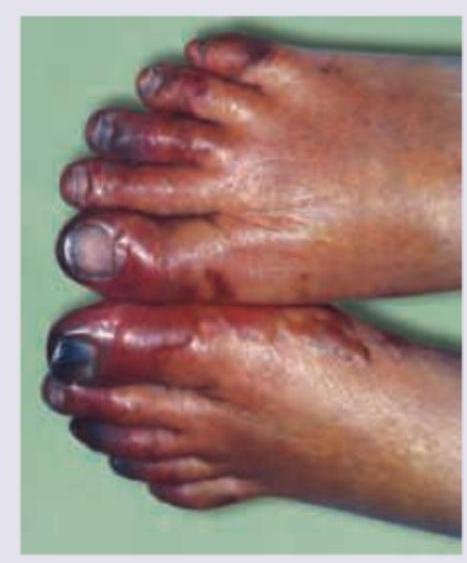
A 72-year-old man comes to the emergency department because of severe, acute, right leg pain for 2 hours. The patient's symptoms started suddenly while he was doing household chores. He has no history of leg pain at rest or with exertion. Yesterday, he returned home after a 6-hour bus ride from his grandson's home. He has hypertension treated with ramipril. He appears uncomfortable. His temperature is 37.4°C (99.3°F), pulse is 105/min and irregular, and blood pressure is 146/92 mm Hg. The right lower extremity is cool and tender to touch. A photograph of the limb is shown. Femoral pulses are palpable bilaterally; popliteal and pedal pulses are decreased on the right side. Sensation to pinprick and light touch and muscle strength are decreased in the right lower extremity. Which of the following is most likely to confirm the underlying source of this patient's condition?
A 23-year-old G1P0 woman presents to the emergency department with regular and painful contractions that occur every 3 minutes. She was at home cooking dinner when she experienced a deluge of clear fluid between her legs followed by painful contractions. The patient has a past medical history of obesity. Her pregnancy was not followed by an obstetrician, but she notes that she experienced abdominal pain and headaches frequently towards the end of her pregnancy. Her temperature is 99.5°F (37.5°C), blood pressure is 187/128 mmHg, pulse is 110/min, respirations are 17/min, and oxygen saturation is 98% on room air. The patient is started on magnesium sulfate and labetalol. The patient delivers her baby vaginally 2 hours later. On the labor and delivery floor, the patient is notably somnolent. Vitals are notable for respirations of 6 per minute. Physical exam reveals a somnolent woman who is minimally responsive. Cardiopulmonary exam is notable for hypopnea. Neurological exam reveals absent deep tendon reflexes and 3/5 strength in her upper and lower extremities. Which of the following is the next best step in management?
The patient declines the use of oxytocin or any other further testing and decides to await a spontaneous delivery. Five weeks later, she comes to the emergency department complaining of vaginal bleeding for 1 hour. Her pulse is 110/min, respirations are 18/min, and blood pressure is 112/76 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 97%. Pelvic examination shows active vaginal bleeding. Laboratory studies show: Hemoglobin 12.8 g/dL Leukocyte count 10,300/mm3 Platelet count 105,000/mm3 Prothrombin time 26 seconds (INR=1.8) Serum Na+ 139 mEq/L K+ 4.1 mEq/L Cl- 101 mEq/L Urea nitrogen 42 mg/dL Creatinine 2.8 mg/dL Which of the following is the most likely underlying mechanism of this patient's symptoms?
A 2500-g (5-lb 8-oz) female newborn delivered at 37 weeks' gestation develops rapid breathing, grunting, and subcostal retractions shortly after birth. Despite appropriate lifesaving measures, the newborn dies 2 hours later. Autopsy shows bilateral renal agenesis. Which of the following is the most likely underlying cause of this newborn's respiratory distress?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
