High-risk pregnancies — MCQs

On this page
A 20-year-old woman presents to the emergency department with painful abdominal cramping. She states she has missed her menstrual period for 5 months, which her primary care physician attributes to her obesity. She has a history of a seizure disorder treated with valproic acid; however, she has not had a seizure in over 10 years and is no longer taking medications for her condition. She has also been diagnosed with pseudoseizures for which she takes fluoxetine and clonazepam. Her temperature is 98.0°F (36.7°C), blood pressure is 174/104 mmHg, pulse is 88/min, respirations are 19/min, and oxygen saturation is 98% on room air. Neurologic exam is unremarkable. Abdominal exam is notable for a morbidly obese and distended abdomen that is nontender. Laboratory studies are ordered as seen below. Serum: hCG: 100,000 mIU/mL Urine: Color: Amber hCG: Positive Protein: Positive During the patient's evaluation, she experiences 1 episode of tonic-clonic motions which persist for 5 minutes. Which of the following treatments is most appropriate for this patient?
A 30-year-old woman, gravida 2, para 1, at 12 weeks' gestation comes to the physician for a prenatal visit. She feels well. Pregnancy and vaginal delivery of her first child were uncomplicated. Five years ago, she was diagnosed with hypertension but reports that she has been noncompliant with her hypertension regimen. The patient does not smoke or drink alcohol. She does not use illicit drugs. Medications include methyldopa, folic acid, and a multivitamin. Her temperature is 37°C (98.6°F), pulse is 80/min, and blood pressure is 145/90 mm Hg. Physical examination shows no abnormalities. Laboratory studies, including serum glucose level, and thyroid-stimulating hormone concentration, are within normal limits. The patient is at increased risk of developing which of the following complications?
A 22-year-old primigravida is admitted to the obstetrics ward with leg swelling at 35 weeks gestation. She denies any other symptoms. Her pregnancy has been uneventful and she was compliant with the recommended prenatal care. Her vital signs were as follows: blood pressure, 168/95 mm Hg; heart rate, 86/min; respiratory rate, 16/min; and temperature, 36.7℃ (98℉). The fetal heart rate was 141/min. The physical examination was significant for 2+ pitting edema of the lower extremity. A dipstick test shows 1+ proteinuria. On reassessment 15 minutes later without administration of an antihypertensive, her blood pressure was 141/88 mm Hg, and the fetal heart rate was 147/min. A decision was made to observe the patient and continue the work-up without initiating antihypertensive therapy. Which of the following clinical features would make the suspected diagnosis into a more severe form?
A 32-year-old G6P1 woman presents to the obstetrician for a prenatal visit. She is 8 weeks pregnant. She has had 4 spontaneous abortions in the past, all during the first trimester. She tells you she is worried about having another miscarriage. She has been keeping to a strictly organic diet and takes a daily prenatal vitamin. She used to smoke a pack a day since she was 16 but quit after her first miscarriage. On a previous visit following fetal loss, the patient tested positive for VDRL and negative for FTA-ABS. Labs are drawn, as shown below: Leukocyte count: 7,800/mm^3 Platelet count: 230,000/mm^3 Hemoglobin: 12.6 g/dL Prothrombin time: 13 seconds Activated partial thromboplastin time: 48 seconds International normalized ratio: 1.2 Which of the following is the best next step in management?
A 26-year-old pregnant woman (gravida 2, para 1) presents on her 25th week of pregnancy. Currently, she has no complaints. Her previous pregnancy was unremarkable. No abnormalities were detected on the previous ultrasound (US) examination at week 13 of pregnancy. She had normal results on the triple test. She is human immunodeficiency virus (HIV), hepatitis B virus (HBV), and hepatitis C virus (HCV)-negative. Her blood type is III(B) Rh+, and her partner has blood type I(0) Rh-. She and her husband are both of Sardinian descent, do not consume alcohol, and do not smoke. Her cousin had a child who died soon after the birth, but she doesn't know the reason. She does not report a history of any genetic conditions in her family, although notes that her grandfather “was always yellowish-pale, fatigued easily, and had problems with his gallbladder”. Below are her and her partner’s complete blood count and electrophoresis results. Complete blood count Patient Her husband Erythrocytes 3.3 million/mm3 4.2 million/mm3 Hb 11.9 g/dL 13.3 g/dL MCV 71 fL 77 fL Reticulocyte count 0.005 0.008 Leukocyte count 7,500/mm3 6,300/mm3 Platelet count 190,000/mm3 256,000/mm3 Electrophoresis HbA1 95% 98% HbA2 3% 2% HbS 0% 0% HbH 2% 0% The patient undergoes ultrasound examination which reveals ascites, liver enlargement, and pleural effusion in the fetus. Further evaluation with Doppler ultrasound shows elevated peak systolic velocity of the fetal middle cerebral artery. Which of the following procedures can be performed for both diagnostic and therapeutic purposes in this case?
A 34-year-old G3P2 presents at 33 weeks gestation with vaginal bleeding that started last night while she was asleep. She denies uterine contractions or abdominal pain. She had a cesarean delivery in her previous pregnancy. She also reports a 10 pack-year smoking history. The vital signs are as follows: blood pressure, 130/80 mm Hg; heart rate, 84/min; respiratory rate, 12/min; and temperature, 36.8℃ (98.2℉). The physical examination is negative for abdominal tenderness or palpable uterine contractions. The perineum is mildly bloody. On speculum examination, no vaginal or cervical lesions are seen. A small amount of blood continues to pass through the cervix. Which of the following findings would you expect on ultrasound examination?
A 29-year-old woman, gravida 2, para 1, at 30 weeks' gestation comes to the emergency department because of severe right-sided back pain for the last hour. The pain is colicky and radiates to the right groin. The patient also reports nausea and pain with urination. Pregnancy has been uncomplicated and the patient reports that she has been following up with her gynecologist on a regular basis. There is no personal or family history of serious illness. She does not smoke or drink alcohol. Medications include folic acid and a multivitamin. Temperature is 37°C (98.6°F), pulse is 90/min, and blood pressure is 130/80 mm Hg. Examination of the back shows costovertebral angle tenderness on the right side. Laboratory studies show: Urine Protein negative RBC casts negative RBC 5–7/hpf WBC casts negative WBC 1–2/hpf Which of the following is the most likely diagnosis?
A 16-year-old girl is brought to the physician because menarche has not yet occurred. She has no history of serious illness and takes no medications. She is 162 cm (5 ft 3 in) tall and weighs 80 kg (176 lb); BMI is 31.2 kg/m2. Breast and pubic hair development is Tanner stage 4. She also has oily skin, acne, and hyperpigmentation of the intertriginous areas of her neck and axillae. The remainder of the examination, including pelvic examination, shows no abnormalities. Which of the following is the most likely explanation for this patient's amenorrhea?
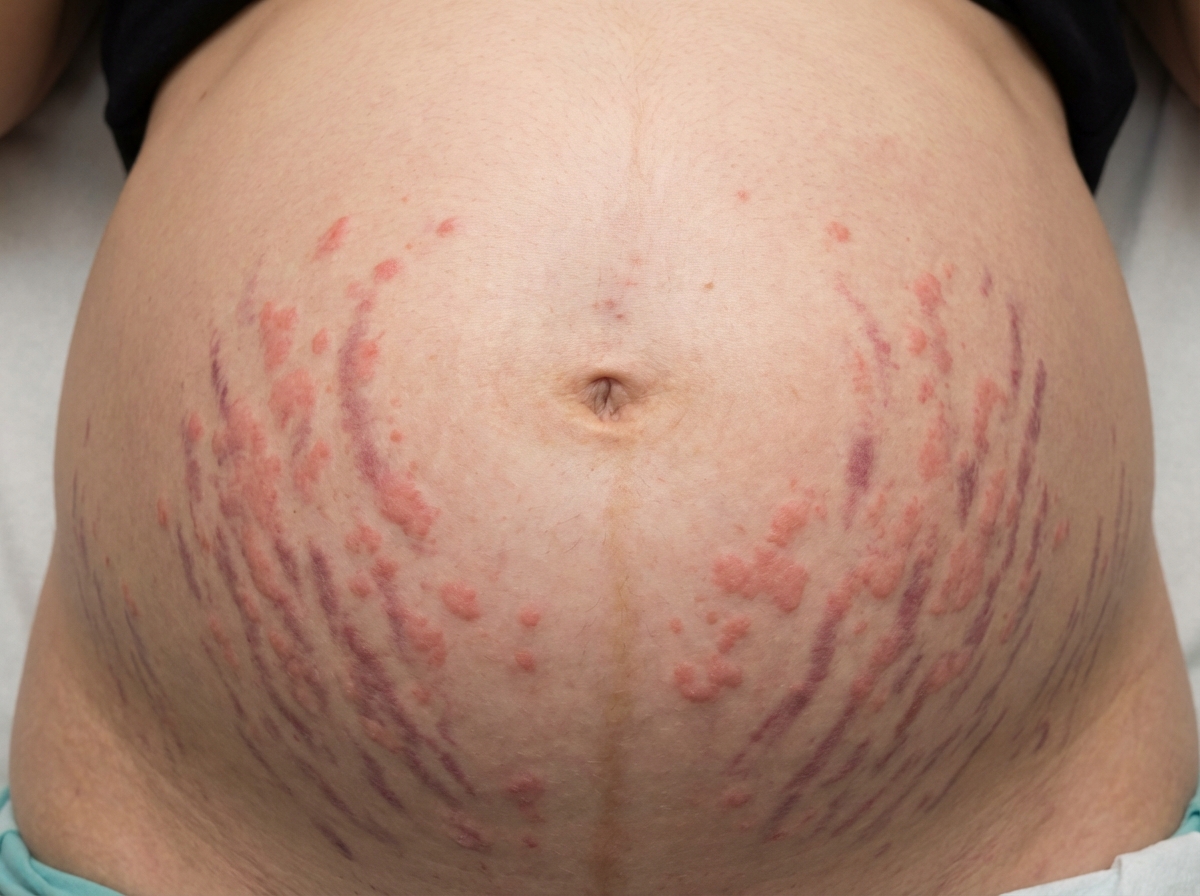
A 23-year-old primigravida pregnant patient is in her 3rd trimester with twins. She complains of itching and skin lesions. The examination shows pruritic erythematous papules and plaques on the abdomen but not on the face, palms, or soles. A picture of her abdomen is shown in the image. Her past medical history is insignificant. Her vital signs are all within normal limits. What is the next best step in management?
A 63-year-old woman, gravida 0, para 0 comes to the physician because of a 3-month history of abdominal distension, constipation, and weight loss. She has a history of endometriosis. Pelvic examination shows a nontender, irregular, left adnexal mass. Her serum level of CA-125 is elevated. Serum concentrations of human chorionic gonadotropin and alpha-fetoprotein are within the reference ranges. Microscopic examination of the mass is most likely to show which of the following findings?
Practice by Chapter
Advanced maternal age
Practice Questions
Multiple gestation management
Practice Questions
Pregestational diabetes
Practice Questions
Chronic hypertension in pregnancy
Practice Questions
Thyroid disorders in pregnancy
Practice Questions
Autoimmune disorders in pregnancy
Practice Questions
Cardiac disease in pregnancy
Practice Questions
Renal disease in pregnancy
Practice Questions
Obesity in pregnancy
Practice Questions
Substance use in pregnancy
Practice Questions
Prior preterm birth management
Practice Questions
Prior cesarean delivery management
Practice Questions
Maternal cancer in pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
