High-risk pregnancies — MCQs

On this page
Which is correct about ABO and Rh incompatibility leading to Erythroblastosis fetalis?
A USG (ultrasound) shows two babies, one of whom appears to be one month older than the other. What is the term for this condition?
A 27 -week pregnant woman with a fetus diagnosed with congenital anomalies is considering a Medical Termination of Pregnancy (MTP). Whose presence is not required for the authorization of MTP in this case?
A 32-year-old female in late pregnancy presents with seizures and high blood pressure. She is diagnosed with eclampsia and started on magnesium sulfate therapy. As part of her management, certain parameters require close monitoring to prevent magnesium toxicity. Which of the following is the MOST important parameter to monitor during magnesium sulfate therapy in this patient?
A woman at 8 weeks of gestation is diagnosed with hyperthyroidism. Which of the following is the most appropriate treatment option?
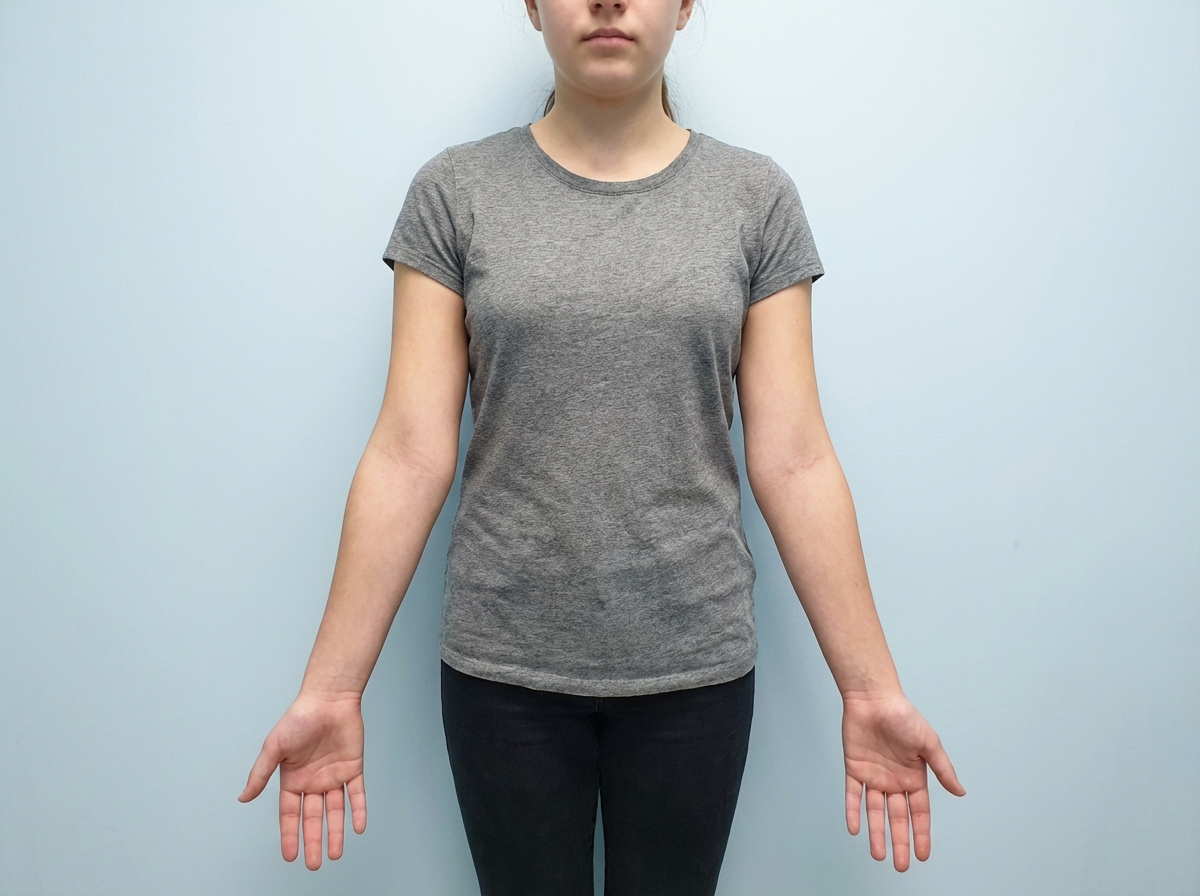
A teenage girl presents with a history of amenorrhea. Local examination is shown in the image. What karyotype analysis would you consider for further evaluation?
A 30-year-old woman presents with a history of pelvic pain and infertility. A transvaginal ultrasound is performed, and the image provided shows a tubular, fluid-filled structure with thin walls. There is no evidence of solid components or internal septations. What is the most likely diagnosis?
A mother brings her daughter with short stature, webbed neck, and other physical features. What is the most likely finding on ultrasound?
A 23-year-old primigravida lives in the same house as her school-going nephew, who contracted a varicella infection. The woman approached the medical center and was tested for varicella antibodies, with a negative result. Which of the following statements are true?
A 36-week pregnant woman with mitral stenosis has been on warfarin for anticoagulation. What is the most appropriate next step in her management?
Practice by Chapter
Advanced maternal age
Practice Questions
Multiple gestation management
Practice Questions
Pregestational diabetes
Practice Questions
Chronic hypertension in pregnancy
Practice Questions
Thyroid disorders in pregnancy
Practice Questions
Autoimmune disorders in pregnancy
Practice Questions
Cardiac disease in pregnancy
Practice Questions
Renal disease in pregnancy
Practice Questions
Obesity in pregnancy
Practice Questions
Substance use in pregnancy
Practice Questions
Prior preterm birth management
Practice Questions
Prior cesarean delivery management
Practice Questions
Maternal cancer in pregnancy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
