Viruses — MCQs

On this page
A 19-year-old woman presents to the family medical center with a 2-week history of a sore throat. She says that she has felt increasingly tired during the day and has a difficult time staying awake during her classes at the university. She appears well-nourished with a low energy level. Her vital signs include the following: the heart rate is 82/min, the respiratory rate is 14/min, the temperature is 37.8°C (100.0°F), and the blood pressure is 112/82 mm Hg. Inspection of the pharynx is depicted in the picture. Palpation of the neck reveals posterior cervical lymphadenopathy. The membrane does not bleed upon scraping. What is the most specific finding for detecting the syndrome described in the vignette?
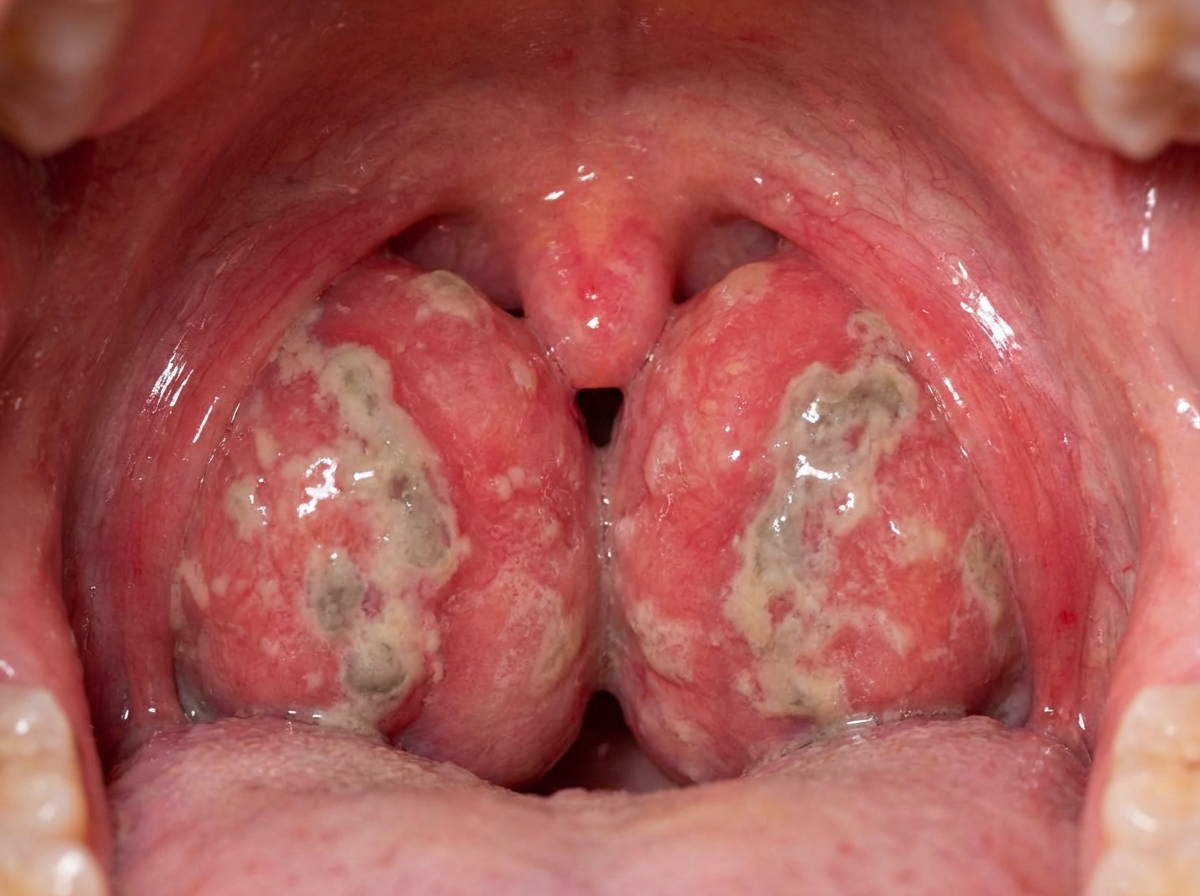
A 47-year-old male presents to the emergency department with facial swelling and trouble breathing. These symptoms began this morning and progressively worsened over the past several hours. Vital signs are as follows: T 37.7, HR 108, BP 120/76, RR 20, and SpO2 96%. Physical examination reveals nonpitting swelling of the face, hands, and arms as well as edema of the tongue and mucus membranes of the mouth and pharynx. The patient reports several episodes of mild facial swelling that occurred during childhood between the ages of 5-18, but he does not recall seeing a physician or receiving treatment for this. His medical history is otherwise negative, except for mild hypertension for which his primary care physician initiated lisinopril 2 weeks ago. This patient most likely has which of the following underlying abnormalities?
A 23-year-old woman presents with progressively worsening headache, photophobia, and intermittent fever that have lasted for 6 days. She says her headache is mostly frontal and radiates down her neck. She denies any recent history of blood transfusions, recent travel, or contact with animals. Her past medical history is unremarkable. She is sexually active with a single partner for the past 3 years. Her temperature is 38.5°C (101.3°F). On physical examination, she appears pale and diaphoretic. A fine erythematous rash is noted on the neck and forearms. A lumbar puncture is performed and CSF analysis reveals: Opening pressure: 300 mm H2O Erythrocytes: None Leukocytes: 72/mm3 Neutrophils: 10% Lymphocytes: 75% Mononuclear: 15% Protein: 100 mg/dL Glucose: 70 mg/dL Which of the following is the most likely diagnosis in this patient?
A 5-year-old boy presents with bilateral conjunctivitis and pharyngitis. The patient’s mother says that symptoms acutely onset 3 days ago and include itchy red eyes, a low-grade fever, and a sore throat. She says that the patient recently attended a camp where other kids were also ill and were completely healthy before going. No significant past medical history. Which of the following is the most likely cause of this patient’s symptoms?
A previously healthy 10-year-old girl is brought to the physician because of severe malaise, pink eyes, cough, and a runny nose for 3 days. She recently immigrated from Sudan and immunization records are unavailable. Her temperature is 40.1°C (104.1°F). Examination shows bilateral conjunctival injections. There are multiple bluish-gray lesions on an erythematous buccal mucosa and soft palate. This patient is at increased risk for which of the following complications?
A parent presents to her pediatrician requesting information about immunizations for her newborn. The pediatrician explains about basic principles of immunization, types of vaccines, possible adverse effects, and the immunization schedule. Regarding how immunizations work, the pediatrician explains that there are mainly 2 types of vaccines. The first type of vaccine provides stronger and more lasting immunity as it induces both cellular and humoral immune responses. The second type of vaccine produces mainly a humoral response only, and its overall efficacy is less as compared to the first type. Which of the following vaccines belongs to the first type of vaccine that the pediatrician is talking about?
A 17-year-old boy is admitted to the emergency department with a history of fatigue, fever of 40.0°C (104.0°F), sore throat, and enlarged cervical lymph nodes. On physical examination, his spleen and liver are not palpable. A complete blood count is remarkable for atypical reactive T cells. An examination of his tonsils is shown in the image below. Which of the following statements is true about the condition of this patient?
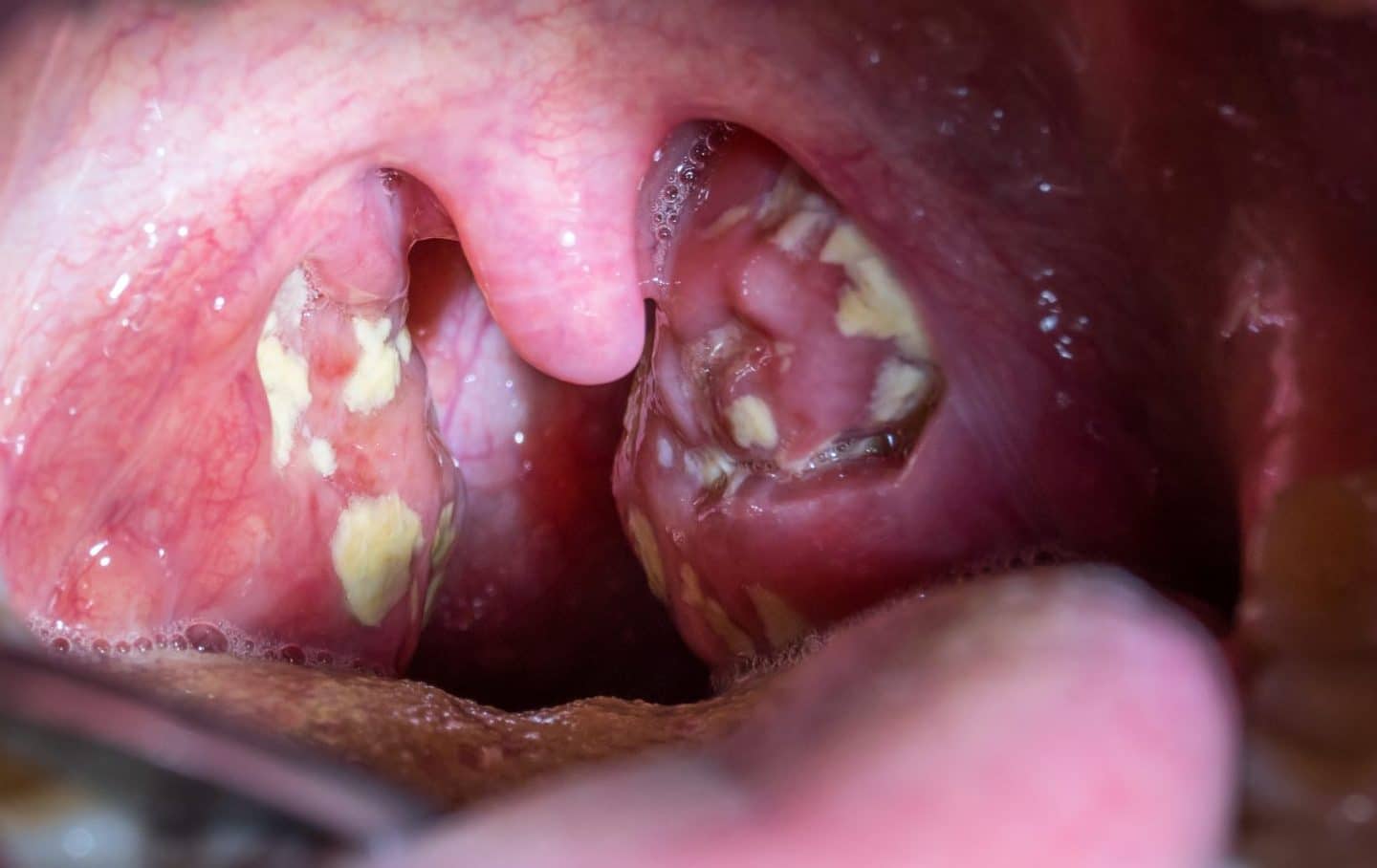
A 5-year-old boy presents to your office with his mother. The boy has been complaining of a sore throat and headache for the past 2 days. His mother states that he had a fever of 39.3°C (102.7°F) and had difficulty eating. On examination, the patient has cervical lymphadenopathy and erythematous tonsils with exudates. A streptococcal rapid antigen detection test is negative. Which of the following is the most likely causative agent?
A 30-year-old man presents with fever, malaise, and severe pain in his right wrist and left knee for the last 2 days. He describes the pain as 8/10 in intensity, sharp in character, and extending from his right wrist to his fingers. He denies any recent inciting trauma or similar symptoms in the past. His past medical history is unremarkable. He is sexually active with multiple partners and uses condoms inconsistently. The vital signs include blood pressure 120/70 mm Hg, pulse 100/min, and temperature 38.3°C (101.0°F). On physical examination, the right wrist and left knee joints are erythematous, warm, and extremely tender to palpation. Both joints have a significantly restricted range of motion. A petechial rash is noted on the right forearm. An arthrocentesis is performed on the left knee joint. Which of the following would be the most likely finding in this patient?
An 82-year-old woman is brought to the physician by her daughter because of a 3-day history of a runny nose, headache, and cough. The patient's grandson recently had similar symptoms. Her vital signs are within normal limits. Pulse oximetry on room air shows an oxygen saturation of 99%. Lungs are clear to auscultation. Testing of nasal secretions is performed to identify the viral strain. Electron microscopy shows a non-enveloped RNA virus with an icosahedral capsid. Binding to which of the following is responsible for the virulence of this virus?
Practice by Chapter
Viral structure and classification
Practice Questions
Viral replication cycles
Practice Questions
Herpesviruses (HSV, VZV, CMV, EBV, HHV-6/7/8)
Practice Questions
Respiratory viruses (influenza, RSV, parainfluenza)
Practice Questions
Enteroviruses and parechoviruses
Practice Questions
Gastroenteritis viruses (norovirus, rotavirus)
Practice Questions
Arboviruses (dengue, Zika, chikungunya)
Practice Questions
Viral hemorrhagic fevers
Practice Questions
Rabies virus
Practice Questions
Poxviruses
Practice Questions
Antiviral agents and mechanisms
Practice Questions
Viral vaccines
Practice Questions
Viral diagnostics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
