Viruses — MCQs

On this page
A 6-year-old female from a rural village in Afghanistan presents with her mother to a local health center complaining of leg weakness. Her mother also reports that the patient had a fever, fatigue, and headache a week prior that resolved. The patient has not received any immunizations since being born. Her temperature is 98.6°F (37°C), blood pressure is 110/70 mmHg, pulse is 90/min, and respirations are 18/min. Physical examination reveals 1/5 strength in right hip and knee actions and 0/5 strength in left hip and knee actions. Tone is notably decreased in both lower extremities. Sensation to touch, temperature, and vibration is intact. Patellar and Achilles reflexes are absent bilaterally. The most likely cause of this patient’s condition has which of the following characteristics?
A 15-year-old girl presents to her primary care physician with her parents. She is complaining of fever and a sore throat for the past 4 days. She was born at 39 weeks gestation via spontaneous vaginal delivery and is up to date on all vaccines and is meeting all developmental milestones. Her boyfriend at school has the same symptoms including fever and sore throat. Today, her heart rate is 90/min, respiratory rate is 17/min, blood pressure is 110/65 mm Hg, and temperature is 38.2°C (100.8°F). Examination revealed cervical lymphadenopathy and mild hepatosplenomegaly. Oral exam reveals focal tonsillar exudate. A monospot test is positive. This patient is most likely infected with which of the following viruses?
A previously healthy 32-year-old male comes to the emergency department because of a high-grade fever and malaise for 3 days. He has severe generalized joint and body pains refractory to acetaminophen. He also has a severe stabbing pain behind his eyes. He returned from a trip to Taiwan 1 week ago. He is sexually active and uses condoms inconsistently. His temperature is 38.7°C (101.7°F), pulse is 102/min, and blood pressure is 100/70 mm Hg. Examination shows nontender inguinal lymphadenopathy. There is a maculopapular rash over the trunk and extremities with some sparing of the skin over his back and groin. Abdominal examination shows no abnormalities. Laboratory studies show: Hemoglobin 13.3 g/dL Leukocyte count 3,900/mm3 Platelet count 90,000/mm3 Serum Na+ 136 mEq/L Cl- 103 mEq/L K+ 4.2 mEq/L Urea nitrogen 15 mg/dL Creatinine 1.2 mg/dL Bilirubin Total 0.4 mg/dL Direct 0.1 mg/dL Alkaline phosphatase 40 U/L AST 130 U/L ALT 60 U/L Urinalysis is normal. An ELISA test for HIV is negative. Which of the following measures is most likely to have prevented this patient’s condition?
A researcher is studying the mammalian immune response with an unknown virus. A group of mice are inoculated with the virus, and blood is subsequently drawn from these animals at various intervals to check immunoglobulin levels. Which of the following is a critical step in the endogenous pathway of antigen presentation for the virus model presented above?
A 36-year-old woman is brought to the emergency room for altered mental status and rapid twitching of her left hand 3 hours ago. The patient is a poor historian given her current mental status, and her husband provided most of the history. He reports that the patient started demonstrating bizarre behavior about 2 weeks ago. She would be up until late into the night working on a “genius project” she had and had elaborate plans to double their joint investments. This morning, she began having speech difficulties, and her left hand jerked uncontrollably for the 10 minutes. He denies loss of consciousness, urinary incontinence, vision changes, or sick contacts. Her past medical history is significant for an adequately treated syphilis infection 10 years ago. Her temperature is 101°F (38.3°C), blood pressure is 118/70 mmHg, pulse is 103/min, respirations are 18/min, and oxygen saturation is 99% on room air. A physical examination demonstrates a lethargic individual with neck stiffness. A computed tomography of the head is unremarkable, and a cerebral spinal fluid (CSF) study is shown below. Cell count: 760/mm3 Cell type: Lymphocytes Glucose: 60 mg/dL Pressure: 100 mmH2O Proteins: 35 mg/dL Erythrocytes: 130/mm^3 What is the most likely explanation for this patient’s symptoms?
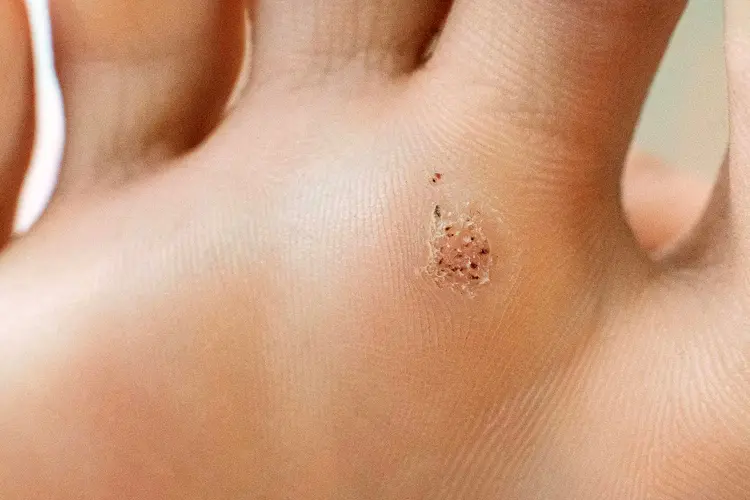
A 16-year-old boy comes to the physician because of a painful lesion on the sole of his right foot for 1 month. It has become progressively larger and more painful, making it difficult for him to walk. He does not have any personal or family history of serious illness. Three years ago he was hospitalized for an ankle fracture that required open reduction and internal fixation. He has moderate facial acne for which he is not receiving any treatment right now. His immunizations are up-to-date. Examination shows a 1-cm lesion on the sole of his foot. The remainder of the examination is unremarkable. A photograph of his sole is shown below. Which of the following is the most likely cause of the lesion?
A 33-year-old woman, gravida 2, para 1, at 24 weeks' gestation is brought to the emergency department by her husband for lethargy, nausea, and vomiting for 4 days. She returned from a trip to South Asia 2 weeks ago. Her immunizations are up-to-date and she has never received blood products. Her temperature is 38.9°C (102°F). She is not oriented to person, place, and time. Examination shows jaundice and mild asterixis. Her prothrombin time is 18 sec (INR=2.0), serum alanine aminotransferase is 3911 U/L, and serum aspartate aminotransferase is 3724 U/L. This patient's current condition is most likely associated with increased titers of which of the following serum studies?
A 4-year-old boy presents to the emergency department with diarrhea. Several days ago, he experienced a fever which has progressed to vomiting and diarrhea. He has had multiple episodes of non-bloody diarrhea and states that he feels fatigued. He is not up to date on his vaccinations and takes many different herbal supplements from his parents. His temperature is 101°F (38.3°C), blood pressure is 100/55 mmHg, pulse is 111/min, respirations are 19/min, and oxygen saturation is 100% on room air. Physical exam is notable for dry mucous membranes and a fatigued appearing child. Which of the following is the most likely etiology of this patient’s symptoms?
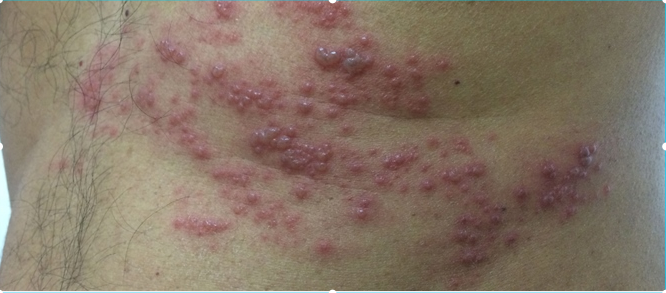
A 9-year-old boy with a history of acute lymphoblastic leukemia is brought to the clinic by his mother because of pruritic vesicles that appeared on the left side of his torso 12 hours ago. One day earlier, before the appearance of the vesicles, the patient's mother notes that he had been complaining of a burning sensation in that area. The boy has been receiving chemotherapy consisting of methotrexate, cytarabine, and cyclophosphamide for 1 month. He received the last treatment 2 days ago. He has no other past medical history. The patient is afebrile and vital signs are within normal limits. Upon physical examination, painful vesicles are localized to the left C7 skin dermatome (see image). Which of the following is the most likely etiology of the skin lesions in this patient?
A scientist is studying the influenza A virus. He focuses on two strains – one from humans (H7N1) and one from horses (H3N8). He takes cells from chickens and coinfects these cells with both influenza strains. From these chicken cells, the scientist isolates a new strain and finds that this new strain can infect human cells. He further characterizes the new strain’s hemagglutinin and neuraminidase description as H7N8. What term best describes the process that underlies these experimental results?
Practice by Chapter
Viral structure and classification
Practice Questions
Viral replication cycles
Practice Questions
Herpesviruses (HSV, VZV, CMV, EBV, HHV-6/7/8)
Practice Questions
Respiratory viruses (influenza, RSV, parainfluenza)
Practice Questions
Enteroviruses and parechoviruses
Practice Questions
Gastroenteritis viruses (norovirus, rotavirus)
Practice Questions
Arboviruses (dengue, Zika, chikungunya)
Practice Questions
Viral hemorrhagic fevers
Practice Questions
Rabies virus
Practice Questions
Poxviruses
Practice Questions
Antiviral agents and mechanisms
Practice Questions
Viral vaccines
Practice Questions
Viral diagnostics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
