Parasites/Fungi — MCQs

On this page
A 61-year-old man is brought to the emergency department by his wife because of increasing confusion over the past 12 hours. His wife reports that he has a history of type 1 diabetes mellitus. His temperature is 38.8°C (101.8°F). He is confused and oriented only to person. Examination shows left periorbital swelling that is tender to palpation, mucopurulent rhinorrhea, and a black necrotic spot over the nose. There is discharge of the left eye with associated proptosis. A photomicrograph of a specimen obtained on biopsy of the left maxillary sinus is shown. Which of the following is the most likely causal organism?
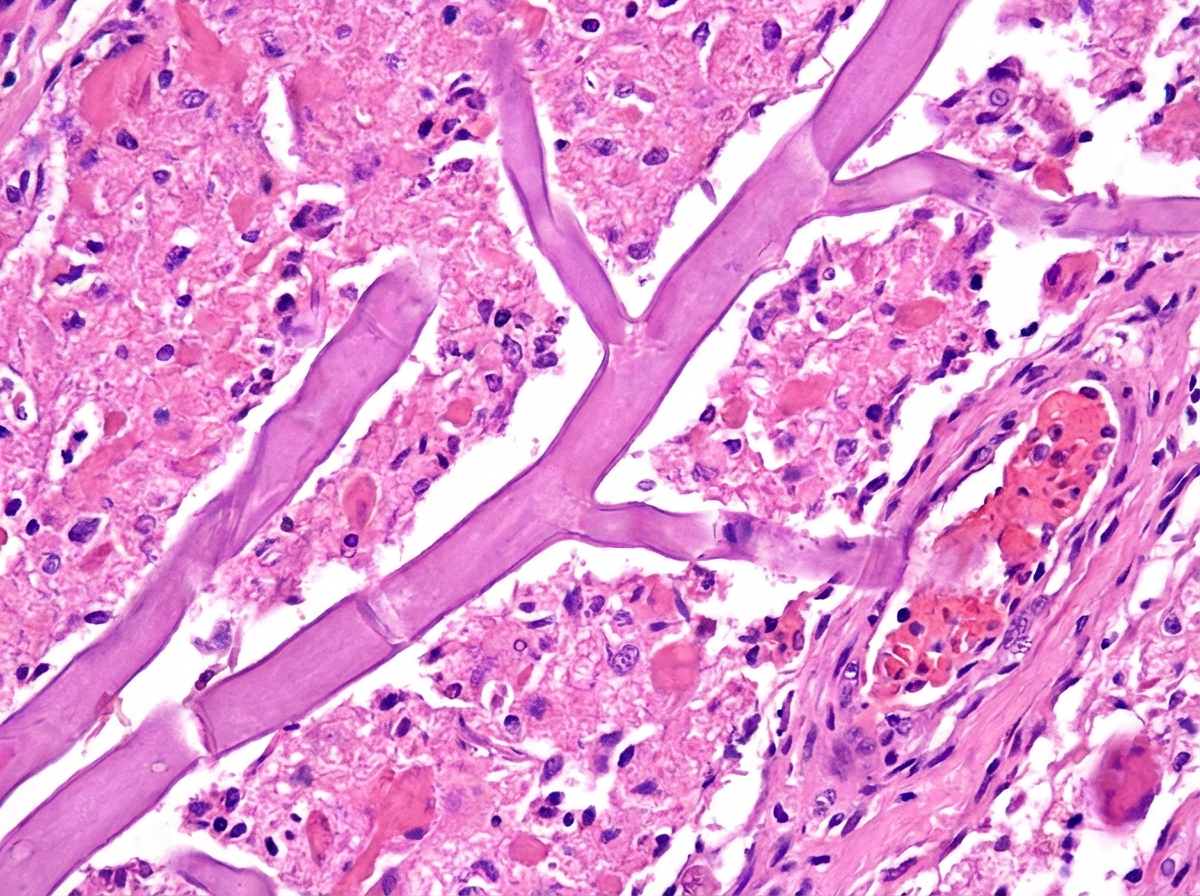
A 16-year-old boy is brought to the physician by his host parents for evaluation of a progressively pruritic rash over his shoulders and buttocks for the past 6 months. He recently came to the United States from Nigeria to attend a year of high school. He reports that it has been increasingly difficult for him to read the whiteboard during classes. Physical examination shows symmetrically distributed papules 4–8 mm in diameter, excoriation marks, and patchy hyperpigmentation over his shoulders, waist, and buttocks. There is nontender inguinal lymphadenopathy and several firm, nontender subcutaneous nodules along the right iliac crest. Six skin snip biopsies are taken from the pelvic girdle, buttocks, and thigh, and are then incubated in saline. After 24 hours, microscopic examination shows motile microfilariae. Which of the following is the most likely diagnosis?
A 67-year-old male presents to his primary care physician for evaluation of fever and an unintended weight loss of 25 pounds over the last 4 months. He also has decreased appetite and complains of abdominal pain located in the right upper quadrant. The patient has not noticed any changes in stool or urine. He emigrated from Malaysia to the United States one year prior. Social history reveals that he smokes half a pack per day and has 5-7 drinks of alcohol per day. The patient is up to date on all of his vaccinations. Physical exam findings include mild jaundice as well as an enlarged liver edge that is tender to palpation. Based on clinical suspicion, biomarker labs are sent and show polycythemia and an elevated alpha fetoprotein level but a normal CA 19-9 level. Surface antigen for hepatitis B is negative. Ultrasound reveals a normal sized gallbladder. Given this presentation, which of the following organisms was most likely associated with the development of disease in this patient?
A 45-year-old man presents to the emergency department with abdominal distension. The patient states he has had gradually worsening abdominal distension with undulating pain, nausea, and vomiting for the past several months. The patient does not see a physician typically and has no known past medical history. He works as a farmer and interacts with livestock and also breeds dogs. His temperature is 98.7°F (37.1°C), blood pressure is 159/90 mmHg, pulse is 88/min, respirations are 15/min, and oxygen saturation is 99% on room air. Physical exam is notable for mild abdominal distension and discomfort to palpation of the upper abdominal quadrants. Laboratory values are ordered and are notable for a mild eosinophilia. A CT scan of the abdomen demonstrates multiple small eggshell calcifications within the right lobe of the liver. Which of the following is the most likely etiology of this patient's symptoms?
A 29-year-old woman comes to the military physician because of a 2-day history of fever, joint pain, dry cough, chest pain, and a painful red rash on her lower legs. Two weeks ago, she returned from military training in Southern California. She appears ill. Her temperature is 39°C (102.1°F). Physical examination shows diffuse inspiratory crackles over all lung fields and multiple tender erythematous nodules over the anterior aspect of both legs. A biopsy specimen of this patient's lungs is most likely to show which of the following?
A 42-year-old man comes to the physician because of a 3-week history of rash that began on his right ankle and gradually progressed up his calf. The rash is itchy and mildly painful. He has type 2 diabetes mellitus and hypertension. He does not smoke or drink alcohol. His current medications include metformin, glipizide, and enalapril. He returned from a trip to Nigeria around 5 weeks ago. He works on a fishing trawler. His temperature is 37°C (98.6°F), pulse is 65/min, and blood pressure is 150/86 mm Hg. Other than the rash on his calf, the examination shows no abnormalities. A picture of the rash is shown. Which of the following is the most likely cause of this patient's symptoms?
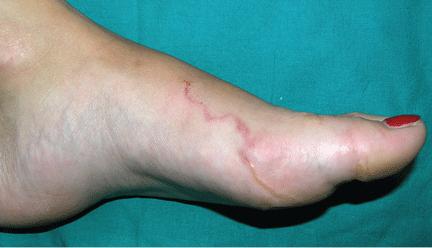
A 16-year-old male with no significant past medical, surgical, or family history presents to his pediatrician with new symptoms following a recent camping trip. He notes that he went with a group of friends and 1 other group member is experiencing similar symptoms. Over the past 5 days, he endorses significant flatulence, nausea, and greasy, foul-smelling diarrhea. He denies tenesmus, urgency, and bloody diarrhea. The blood pressure is 118/74 mm Hg, heart rate is 88/min, respiratory rate is 14/min, and temperature is 37.0°C (98.6°F). Physical examination is notable for mild, diffuse abdominal tenderness. He has no blood in the rectal vault. What is the patient most likely to report about his camping activities?
A 55-year-old man comes to the physician because of fever, fatigue, dry cough, headache, and myalgia over the past week. Two days ago, he developed several painful oral lesions and difficulty swallowing. He underwent kidney transplantation 3 years ago. His temperature is 38.2°C (100.7°F). Physical examination shows bilateral rales, hepatosplenomegaly, and multiple 1–2 cm ulcerative lesions with raised borders in the oral mucosa. A photomicrograph of a liver biopsy specimen is shown. Which of the following is the most likely causal pathogen?
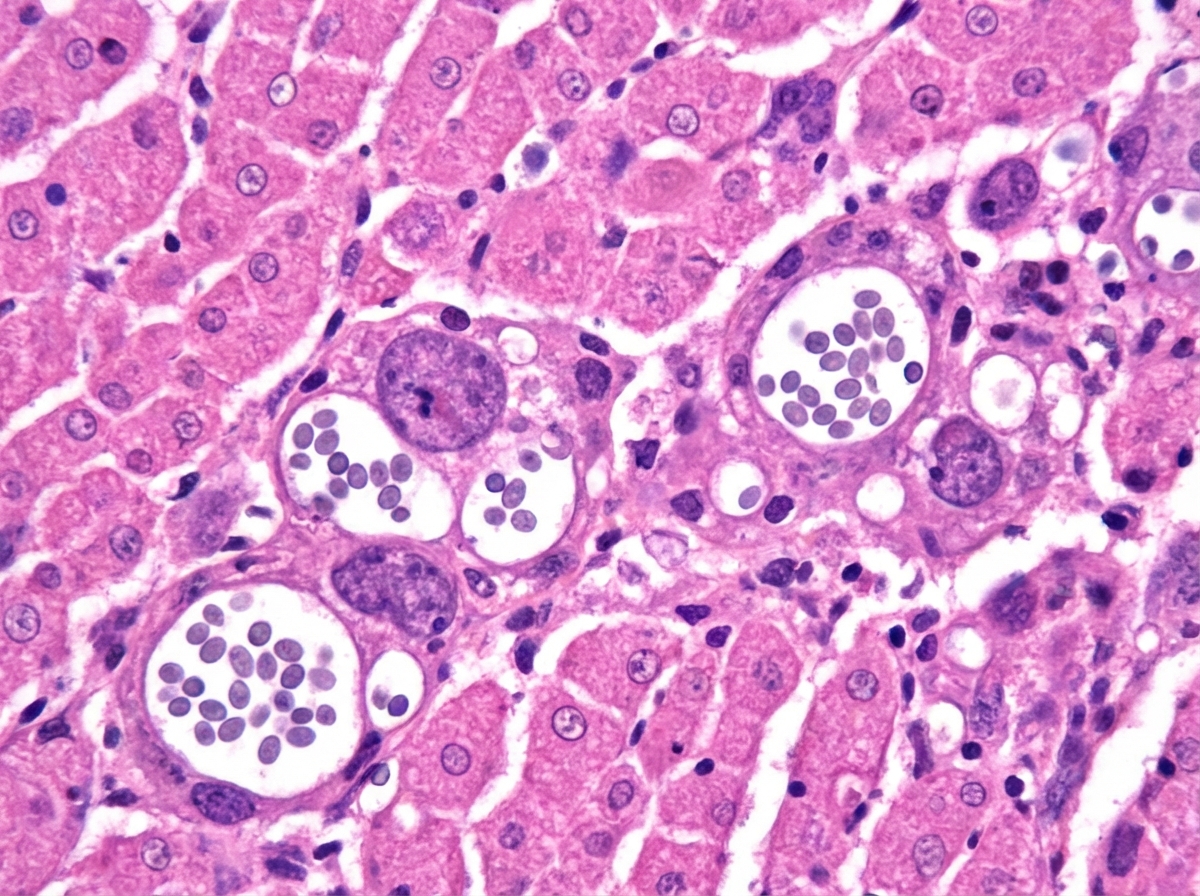
A 47-year-old woman comes to the physician because of a 3-day history of fever, fatigue, loss of appetite, cough, and chest pain. Physical examination shows diffuse inspiratory crackles over the left lung field. An x-ray of the chest shows hilar lymphadenopathy and well-defined nodules with central calcifications. Urine studies show the presence of a polysaccharide antigen. A biopsy specimen of the lung shows cells with basophilic, crescent-shaped nuclei and pericellular halos located within macrophages. This patient's history is most likely to show which of the following?
A 13-year-old boy is brought to the physician because of a 5-day history of a rash on his chest and back. His mother initially noticed only a few lesions on his back, but since then the rash has spread to his chest. His family returned from a trip to the Caribbean 2 weeks ago. His mother started using a new laundry detergent 8 days ago. He has type 1 diabetes mellitus controlled with insulin. His mother has Hashimoto thyroiditis and his brother has severe facial acne. His temperature is 37.2°C (99°F), pulse is 81/min, and blood pressure is 115/74 mm Hg. Examination of the skin shows multiple, nontender, round, white macules on the chest and trunk. There is fine scaling when the lesions are scraped with a spatula. There are no excoriation marks. The remainder of the examination shows no abnormalities. Which of the following is the most likely underlying mechanism of this patient's symptoms?
Practice by Chapter
Candida species
Practice Questions
Aspergillus species
Practice Questions
Cryptococcus neoformans/gattii
Practice Questions
Pneumocystis jirovecii
Practice Questions
Mucormycoses
Practice Questions
Dermatophytes
Practice Questions
Antifungal agents
Practice Questions
Opportunistic fungal infections
Practice Questions
Parasitic life cycles
Practice Questions
Soil-transmitted helminths
Practice Questions
Filarial nematodes
Practice Questions
Schistosomiasis
Practice Questions
Echinococci and other tissue helminths
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
