Parasites/Fungi — MCQs

On this page
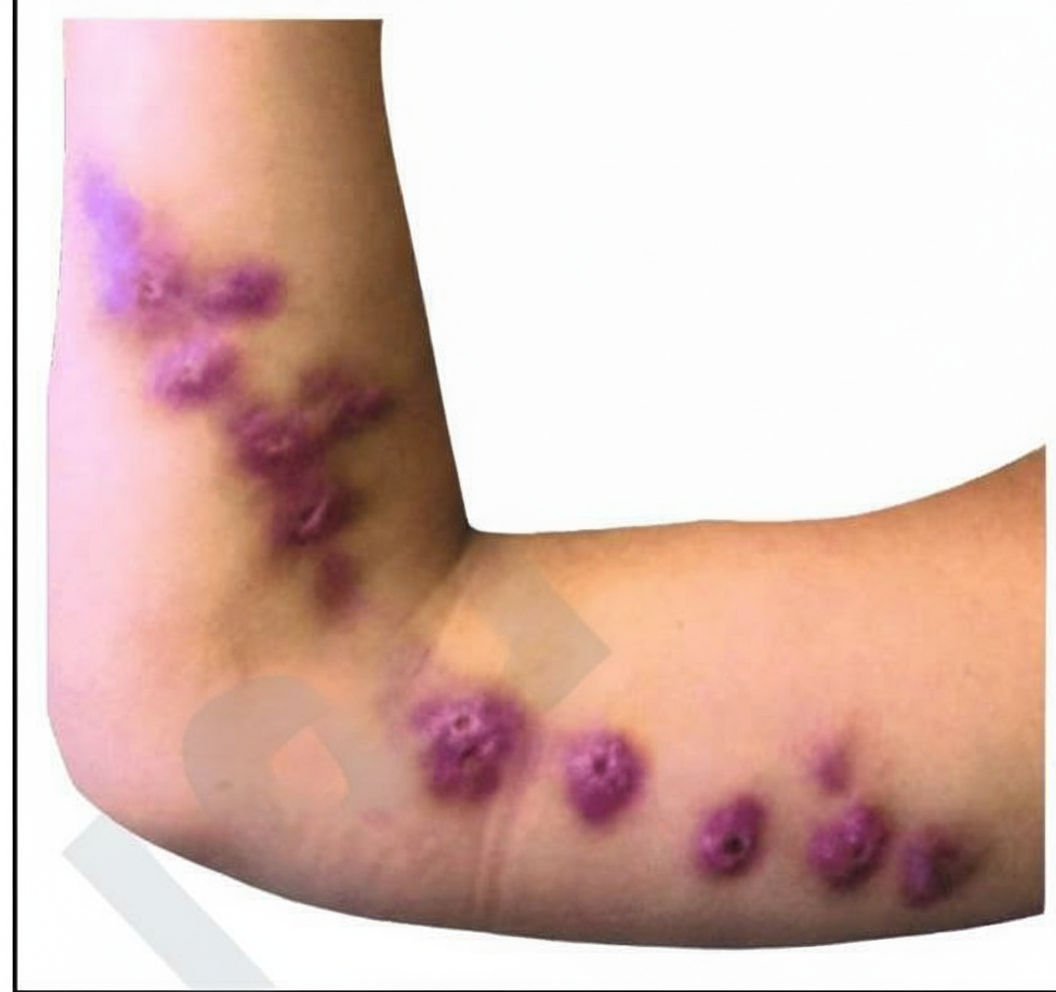
A previously healthy 48-year-old man comes to the physician because of a 2-week history of a nonpruritic rash on his right forearm. The rash began as pustules and progressed to form nodules and ulcers. He works as a gardener. Physical examination shows right axillary lymphadenopathy and the findings in the photograph. Which of the following is the most likely causal organism?
Practice by Chapter
Candida species
Practice Questions
Aspergillus species
Practice Questions
Cryptococcus neoformans/gattii
Practice Questions
Pneumocystis jirovecii
Practice Questions
Mucormycoses
Practice Questions
Dermatophytes
Practice Questions
Antifungal agents
Practice Questions
Opportunistic fungal infections
Practice Questions
Parasitic life cycles
Practice Questions
Soil-transmitted helminths
Practice Questions
Filarial nematodes
Practice Questions
Schistosomiasis
Practice Questions
Echinococci and other tissue helminths
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
