HIV — MCQs

On this page
Four scientists were trying to measure the effect of a new inhibitor X on the expression levels of transcription factor, HNF4alpha. They measured the inhibition levels by using RT-qPCR. In short they converted the total mRNA of the cells to cDNA (RT part), and used PCR to amplify the cDNA quantifying the amplification with a dsDNA binding dye (qPCR part). Which of the following group characteristics contains a virus(es) that has the enzyme necessary to convert the mRNA to cDNA used in the above scenario?
A 44-year-old with a past medical history significant for human immunodeficiency virus infection presents to the emergency department after he was found to be experiencing worsening confusion. The patient was noted to be disoriented by residents and staff at the homeless shelter where he resides. On presentation he reports headache and muscle aches but is unable to provide more information. His temperature is 102.2°F (39°C), blood pressure is 112/71 mmHg, pulse is 115/min, and respirations are 24/min. Knee extension with hips flexed produces significant resistance and pain. A lumbar puncture is performed with the following results: Opening pressure: Normal Fluid color: Clear Cell count: Increased lymphocytes Protein: Slightly elevated Which of the following is the most likely cause of this patient's symptoms?
A 27-year-old man interested in pre-exposure therapy for HIV (PrEP) is being evaluated to qualify for a PrEP study. In order to qualify, patients must be HIV- and hepatitis B- and C-negative. Any other sexually transmitted infections require treatment prior to initiation of PrEP. The medical history is positive for a prior syphilis infection and bipolar affective disorder, for which he takes lithium. On his next visit, the liver and renal enzymes are within normal ranges. HIV and hepatitis B and C tests are negative. Which of the following about the HIV test is true?
A 32-year-old HIV positive male presents to the office complaining of difficulty swallowing and bad breath for the past couple of months. Upon further questioning, he says, "it feels like there’s something in my throat". He says that the difficulty is sometimes severe enough that he has to skip meals. He added that it mainly occurs with solid foods. He is concerned about his bad breath since he has regular meetings with his clients. Although he is on antiretroviral medications, he admits that he is noncompliant. On examination, the patient is cachectic with pale conjunctiva. On lab evaluation, the patient’s CD4+ count is 70/mm3. What is the most likely cause of his symptoms?
A 33-year-old man with HIV comes to the physician because of a nonproductive cough and shortness of breath for 3 weeks. He feels tired after walking up a flight of stairs and after long conversations on the phone. He appears chronically ill. His temperature is 38.5°C (101.3°F), and pulse is 110/min. Pulse oximetry on room air shows an oxygen saturation of 95%. Upon walking, his oxygen saturation decreases to 85%. Cardiopulmonary examination is normal. Laboratory studies show a CD4+ T-lymphocyte count of 176/mm3 (N > 500). Results of urine Legionella antigen testing are negative. A CT scan of the chest shows diffuse, bilateral ground-glass opacities. Microscopic examination of fluid obtained from bronchoalveolar lavage will most likely show which of the following findings?
A 41-year-old HIV-positive male presents to the ER with a 4-day history of headaches and nuchal rigidity. A lumbar puncture shows an increase in CSF protein and a decrease in CSF glucose. When stained with India ink, light microscopy of the patient’s CSF reveals encapsulated yeast with narrow-based buds. Assuming a single pathogenic organism is responsible for this patient’s symptoms, which of the following diagnostic test results would also be expected in this patient?
A 24-year-old male presents to the emergency room with a cough and shortness of breath for the past 3 weeks. You diagnose Pneumocystis jiroveci pneumonia (PCP). An assay of the patient's serum reveals the presence of viral protein p24. Which of the following viral genes codes for this protein?
A 45-year-old man presents with a 2-week history of night sweats, cough, and a fever. Past medical history includes HIV infection diagnosed 10 years ago, managed with HAART. He says he hasn’t been compliant with his HAART therapy as prescribed because it is too expensive and he is currently unemployed without insurance. A chest radiograph is performed and reveals a cavity in the right upper lobe of his lung. Which of the following lung infections is most likely causing this patient’s symptoms?
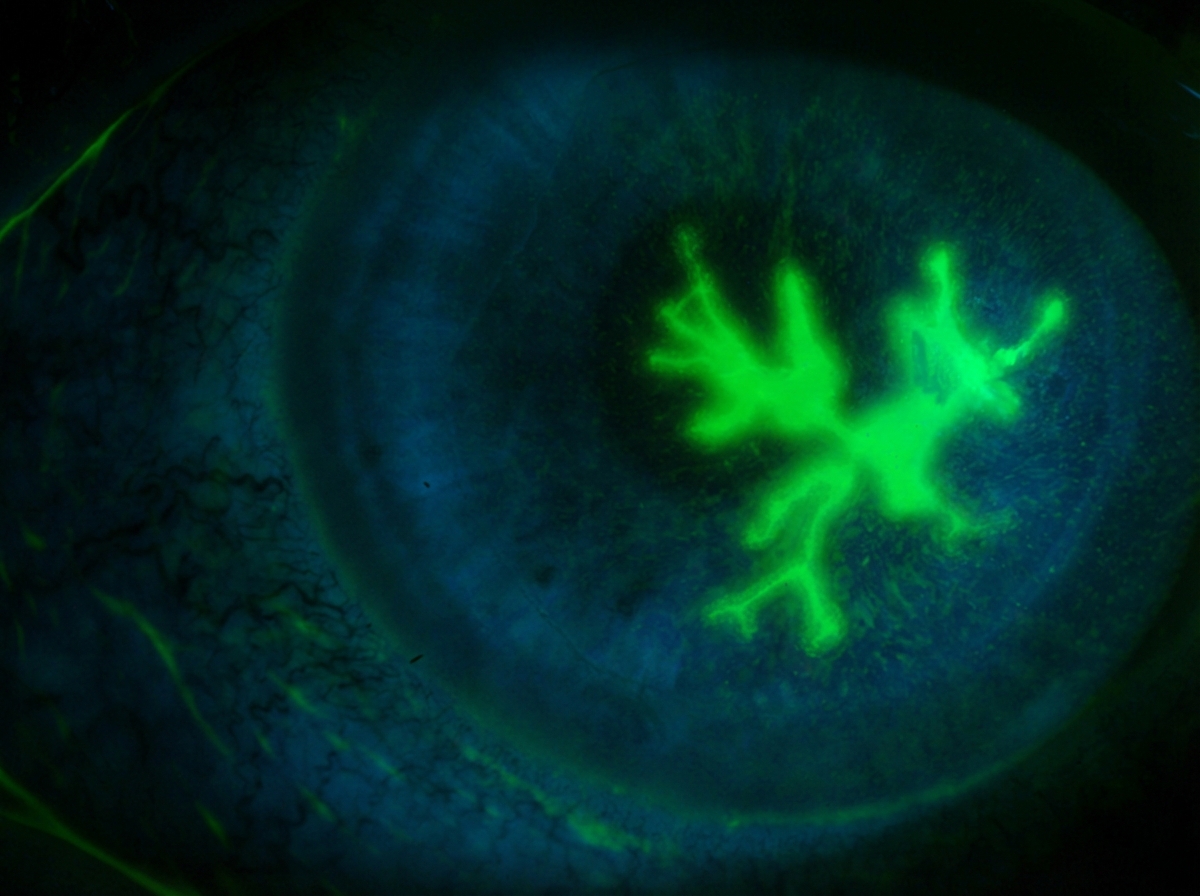
A 36-year-old woman with HIV comes to the physician because of a 3-day history of pain and watery discharge in her left eye. She also has blurry vision and noticed that she is more sensitive to light. Her right eye is asymptomatic. She had an episode of shingles 7 years ago. She was diagnosed with HIV 5 years ago. She admits that she takes her medication inconsistently. She wears contact lenses. Current medications include abacavir, lamivudine, efavirenz, and a nutritional supplement. Her temperature is 37°C (98.6°F), pulse is 89/min, and blood pressure is 110/70 mm Hg. Examination shows conjunctival injection of the left eye. Visual acuity is 20/20 in the right eye and 20/80 in the left eye. Extraocular movements are normal. Her CD4+ T-lymphocyte count is 90/mm3. A photograph of the left eye after fluorescein administration is shown. Which of the following is the most likely diagnosis?
A 23-year-old male with a homozygous CCR5 mutation is found to be immune to HIV infection. The patient’s CCR5 mutation interferes with the function of which viral protein?
Practice by Chapter
HIV structure and replication cycle
Practice Questions
HIV transmission and epidemiology
Practice Questions
Acute HIV infection
Practice Questions
CD4 monitoring and viral load
Practice Questions
Opportunistic infections in HIV/AIDS
Practice Questions
Antiretroviral therapy principles
Practice Questions
NRTI, NNRTI, PI, INSTI, and entry inhibitors
Practice Questions
HIV resistance testing
Practice Questions
HIV prevention strategies
Practice Questions
HIV-associated malignancies
Practice Questions
HIV in pregnancy and vertical transmission
Practice Questions
HIV co-infections (HBV, HCV, TB)
Practice Questions
HIV cure research
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
