Gram-positive — MCQs

On this page
A 23-year-old man comes to the physician because of a painless swelling on the left side of his jaw for 2 months. It has been progressively increasing in size and is draining thick, foul-smelling fluid. He had a molar extracted 3 months ago. Examination shows a 4-cm, tender, erythematous mass in the left submandibular region with purulent drainage. There is submandibular lymphadenopathy. A culture of the purulent material shows catalase-negative, gram-positive filamentous rods that do not stain with carbol fuchsin. Which of the following is the most likely causal pathogen?
A 16-year-old girl is brought to the emergency department by her parents because of fever, vomiting, rash, and worsening confusion since this morning. On questioning, her mother reports that her last menstrual period was 1 week ago and that she recently started using tampons. She appears lethargic and is only oriented to person. Her temperature is 40.4°C (104.7°F), pulse 174/minute, and blood pressure is 62/44 mm Hg. Examination shows oropharyngeal hyperemia and diffuse macular erythroderma. Which of the following is the most likely cause of this patient's condition?
A 7-year-old boy is brought to the emergency department by his parents. They state that he has had trouble walking the past day and this morning refuses to walk at all. The child has a past medical history of asthma, which is treated with albuterol. His temperature is 102°F (38.9°C), blood pressure is 77/48 mmHg, pulse is 150/min, respirations are 17/min, and oxygen saturation is 98% on room air. Laboratory tests are drawn and shown below. Hemoglobin: 10 g/dL Hematocrit: 36% Leukocyte count: 13,500/mm^3 with normal differential Platelet count: 197,000/mm^3 An MRI of the thigh and knee is performed and demonstrates edema and cortical destruction of the distal femur. Which of the following is the most likely infectious agent in this patient?
A previously healthy 57-year-old man is brought to the emergency department because of a 3-day history of fever and headache. He also has nausea and vomited twice in the past 24 hours. His temperature is 39.1°C (102.4°F). He is lethargic but oriented to person, place, and time. Examination shows severe neck rigidity with limited active and passive range of motion. A lumbar puncture is performed; cerebrospinal fluid analysis shows a neutrophilic pleocytosis and a decreased glucose concentration. A Gram stain of the patient's cerebrospinal fluid is most likely to show which of the following?
A 7-year-old Caucasian male presents with a temperature of 38°C. During the physical exam, the patient complains of pain when his femur is palpated. The patient's parents state that the fever started a few days after they noticed a honey-colored crusting on the left upper lip of the child's face. Culture of the bacteria reveals a catalase-positive, gram-positive cocci. Which of the following bacteria is most likely to be found in a biopsy of the child's left femur?
A 5-year-old child is brought to a pediatric clinic by his mother for a rash that started a few days ago. The mother adds that her son has also had a fever and sore throat since last week. His immunizations are up to date. On examination, a rash is present over the trunk and upper extremities and feels like sandpaper to touch. An oropharyngeal examination is suggestive of exudative pharyngitis with a white coat over the tongue. The physician swabs the throat and uses the swab in a rapid antigen detection test kit. He also sends the sample for microbiological culture. The physician then recommends empiric antibiotic therapy and tells the mother that if the boy is left untreated, the likelihood of developing a complication later in life is very high. Which of the following best explains the mechanism underlying the development of the complication the physician is talking about?
A 60-year-old woman with ovarian cancer comes to the physician with a 5-day history of fever, chills, and dyspnea. She has a right subclavian chemoport in which she last received chemotherapy 2 weeks ago. Her temperature is 39.5°C (103.1°F), blood pressure is 110/80 mm Hg, and pulse is 115/min. Cardiopulmonary examination shows jugular venous distention and a new, soft holosystolic murmur heard best in the left parasternal region. Crackles are heard at both lung bases. Echocardiography shows a vegetation on the tricuspid valve. Peripheral blood cultures taken from this patient are most likely to show which of the following findings?
A 4-year-old boy is presented to the clinic by his mother due to a peeling erythematous rash on his face, back, and buttocks which started this morning. Two days ago, the patient’s mother says his skin was extremely tender and within 24 hours progressed to desquamation. She also says that, for the past few weeks, he was very irritable and cried more than usual during diaper changes. The patient is up to date on his vaccinations and has been meeting all developmental milestones. No significant family history. On physical examination, the temperature is 38.4°C (101.1°F) and the pulse is 70/min. The epidermis separates from the dermis by gentle lateral stroking of the skin. Systemic antibiotics are prescribed, and adequate fluid replacement is provided. Which of the following microorganisms most likely caused this patient’s condition?
A 9-year-old boy who recently emigrated from sub-Saharan Africa is brought to the physician because of a 2-day history of fever, chills, and productive cough. His mother reports that he has had several episodes of painful swelling of his fingers during infancy that resolved with pain medication. His immunization status is unknown. His temperature is 39.8°C (103.6°F). Examination shows pale conjunctivae and yellow sclerae. There are decreased breath sounds and inspiratory crackles over the left lower lung fields. His hemoglobin concentration is 7 g/dL. Blood cultures grow optochin-sensitive, gram-positive diplococci. A deficiency in which of the following most likely contributed to this patient's infection?
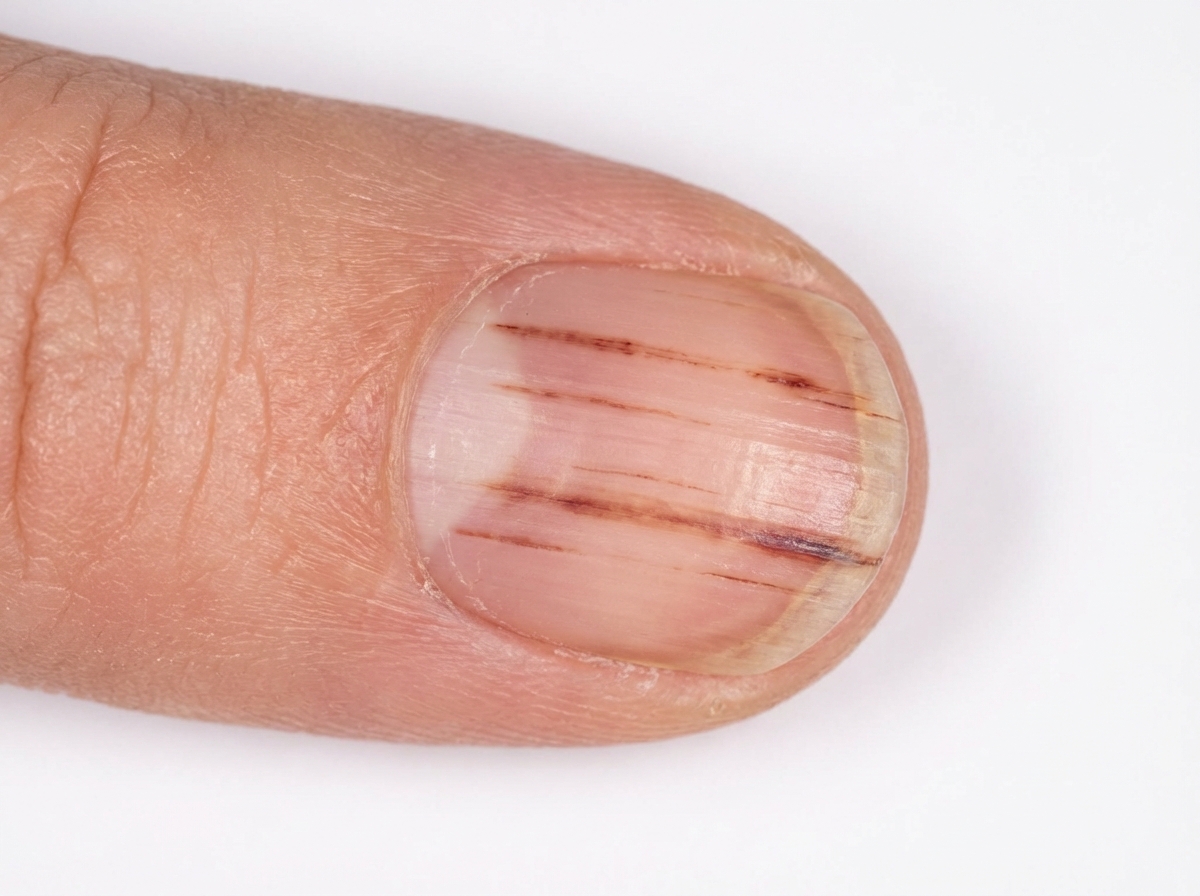
A 63-year-old man comes to the physician for evaluation of fever and a nonproductive cough for the past 2 weeks. During this period, he has also had fatigue, myalgia, and difficulty breathing. Five weeks ago, he underwent an aortic prosthetic valve replacement due to high-grade aortic stenosis. The patient has a history of hypertension, asthma, and type 2 diabetes mellitus. A colonoscopy 2 years ago was normal. The patient has smoked one pack of cigarettes daily for the past 40 years. He has never used illicit drugs. Current medications include aspirin, warfarin, lisinopril, metformin, inhaled albuterol, and a multivitamin. The patient appears lethargic. Temperature is 38.6°C (101.5°F), pulse is 105/min, and blood pressure is 140/60 mm Hg. Rales are heard on auscultation of the lungs. A grade 2/6, diastolic blowing murmur is heard over the left sternal border and radiates to the right sternal border. A photograph of his right index finger is shown. Laboratory studies show a leukocyte count of 13,800/mm3 and an erythrocyte sedimentation rate of 48 mm/h. Which of the following is the most likely causal organism?
Practice by Chapter
Staphylococcus aureus
Practice Questions
Coagulase-negative staphylococci
Practice Questions
Streptococcus pneumoniae
Practice Questions
Group A streptococci
Practice Questions
Group B streptococci
Practice Questions
Viridans group streptococci
Practice Questions
Enterococci
Practice Questions
Bacillus species
Practice Questions
Listeria monocytogenes
Practice Questions
Corynebacterium species
Practice Questions
Clostridium species
Practice Questions
Actinomyces and Nocardia
Practice Questions
MRSA and VRE
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
