Bacteria — MCQs

On this page
An 87-year-old male nursing home resident is currently undergoing antibiotic therapy for the treatment of a decubitus ulcer. One week into the treatment course, he experiences several episodes of watery diarrhea. Subsequent sigmoidoscopy demonstrates the presence of diffuse yellow plaques on the mucosa of the sigmoid colon. Which of the following is the best choice of treatment for this patient?
A 4-year-old male presents to the pediatrician with a one week history of fever, several days of bloody diarrhea, and right-sided abdominal pain. The mother explains that several other children at his son's pre-K have been having similar symptoms. She heard the daycare owner had similar symptoms and may have her appendix removed, but the mother claims this may just have been a rumor. Based on the history, the pediatrician sends for an abdominal ultrasound, which shows a normal vermiform appendix. She then sends a stool sample for culturing. The cultures demonstrate a Gram-negative bacteria that is motile at 25 C but not at 37 C, non-lactose fermenter, and non-hydrogen sulfide producer. What is the most likely causative agent?
A 22-year-old sexually active female presents to the emergency department in severe pain. She states that she has significant abdominal pain that seems to worsen whenever she urinates. This seems to have progressed over the past day and is accompanied by increased urge and frequency. The emergency room physician obtains a urinalysis which demonstrates the following: SG: 1.010, Leukocyte esterase: Positive, Protein: Trace, pH: 7.5, RBC: Negative. Nitrite: Negative. A urease test is performed which is positive. What is the most likely cause of UTI in this patient?
A 20-year-old man presents to his physician with diarrhea, vomiting, and fever for the past 2 days. After laboratory evaluation, he is diagnosed with bacterial gastroenteritis. The man is a microbiology major and knows that the human gastrointestinal tract, respiratory tract, and skin are lined by epithelia which act as a barrier against several infective microorganisms. He also knows that there are specific T cells in these epithelia that play a part in innate immunity and in recognition of microbial lipids. Which of the following types of T cells is the man thinking of?
A 27-year-old man presents to the emergency department with unrelenting muscle spasms for the past several hours. The patient’s girlfriend states that he started having jaw spasms and soreness last night but now his neck, back, and arms are spasming. She also states that he stepped on a nail about 1 week ago. Past medical history is noncontributory. The patient's vaccination status is unknown at this time. Today, the vital signs include temperature 39.1°C (102.4°F), heart rate 115/min, blood pressure 145/110 mm Hg, and respiratory rate 10/min. On exam, the patient is in obvious discomfort, with a clenched jaw and extended neck. Labs are drawn and a basic metabolic panel comes back normal and the white blood cell (WBC) count is moderately elevated. Which of the following is the most likely etiology of this patient’s symptoms?
A previously healthy 3-year-old boy is brought to the physician by his mother because of a headache, fever, and facial pain that started 10 days ago. The symptoms initially improved but have gotten significantly worse over the past 2 days. Immunizations are up-to-date. His temperature is 39.1°C (102.3°F). Physical examination shows tenderness to palpation over both cheeks. Gram stain of a nasal swab shows small, gram-negative coccobacilli. Which of the following most likely accounts for this patient's infection with the causal pathogen?
A 23-year-old man presents to student health for a cough. The patient states he has paroxysms of coughing followed by gasping for air. The patient is up to date on his vaccinations and is generally healthy. He states he has felt more stressed lately secondary to exams. His temperature is 101.0°F (38.3°C), blood pressure is 125/65 mmHg, pulse is 105/min, respirations are 14/min, and oxygen saturation is 98% on room air. Laboratory values are notable for the findings below. Hemoglobin: 12 g/dL Hematocrit: 36% Leukocyte count: 13,500/mm^3 with a lymphocytosis Platelet count: 197,000/mm^3 Physical exam is notable for clear breath sounds bilaterally. Which of the following is the best next step in management?
A 19-year-old male is found to have Neisseria gonorrhoeae bacteremia. This bacterium produces an IgA protease capable of cleaving the hinge region of IgA antibodies. What is the most likely physiological consequence of such a protease?
A patient is infected with a pathogen and produces many antibodies to many antigens associated with that pathogen via Th cell-activated B cells. This takes place in the germinal center of the lymphoid tissues. If the same patient is later re-infected with the same pathogen, the immune system will respond with a much stronger response, producing antibodies with greater specificity for that pathogen in a shorter amount of time. What is the term for this process that allows the B cells to produce antibodies specific to that antigen?
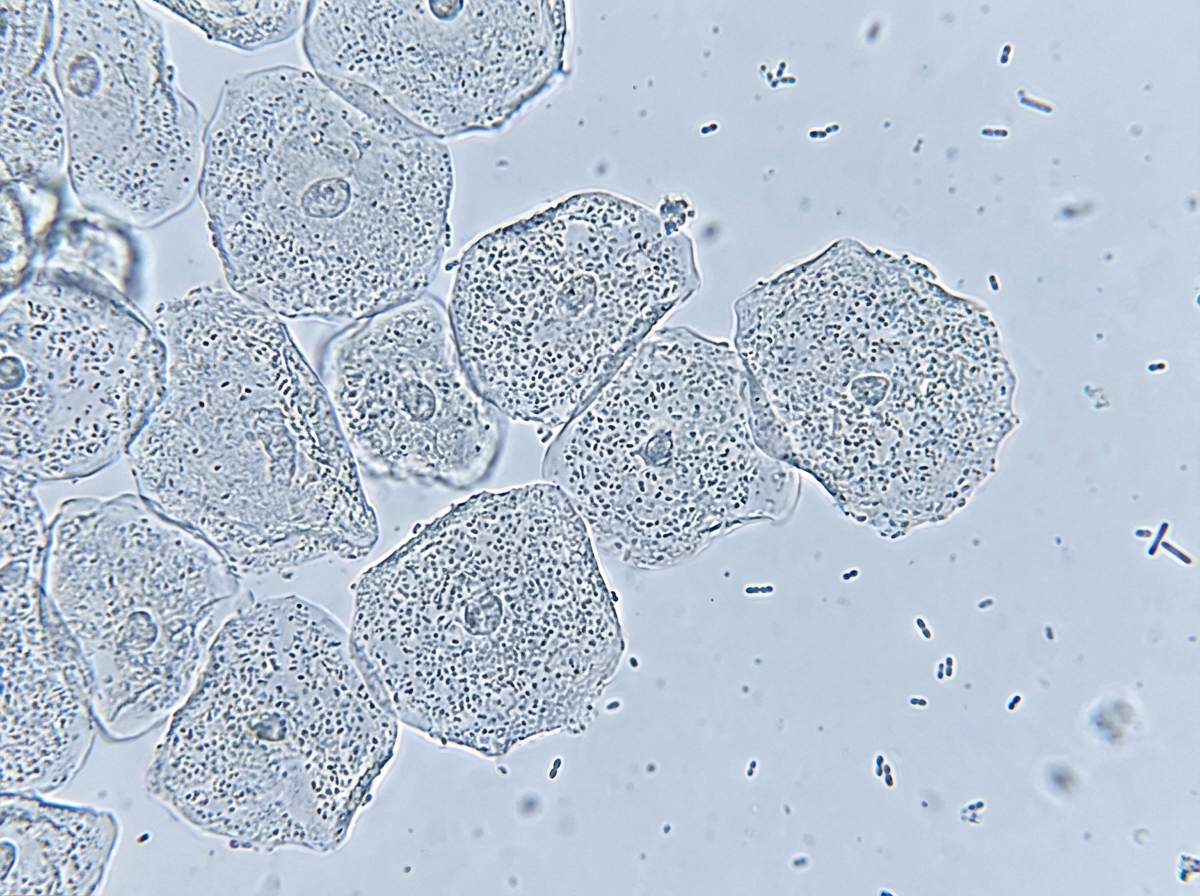
A 25-year-old woman comes to the physician because of vaginal discharge for 4 days. She has no pain or pruritus. Menses occur at regular 27-day intervals and last 5 days. Her last menstrual period was 2 weeks ago. She is sexually active with two male partners and uses a diaphragm for contraception. She had a normal pap smear 3 months ago. She has no history of serious illness and takes no medications. Her temperature is 37.3°C (99°F), pulse is 75/min, and blood pressure is 115/75 mm Hg. Pelvic examination shows a malodorous gray vaginal discharge. The pH of the discharge is 5.0. Microscopic examination of the vaginal discharge is shown. Which of the following is the most likely causal organism?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
