Bacteria — MCQs

On this page
Which of the following patient presentations would be expected in an infant with defective LFA-1 integrin (CD18) protein on phagocytes, in addition to recurrent bacterial infections?
A 6-year-old girl is brought to the physician for intermittent fevers and painful swelling of the left ankle for 2 weeks. She has no history of trauma to the ankle. She has a history of sickle cell disease. Current medications include hydroxyurea and acetaminophen for pain. Her temperature is 38.4°C (101.2°F) and pulse is 112/min. Examination shows a tender, swollen, and erythematous left ankle with point tenderness over the medial malleolus. A bone biopsy culture confirms the diagnosis. Which of the following is the most likely causal organism?
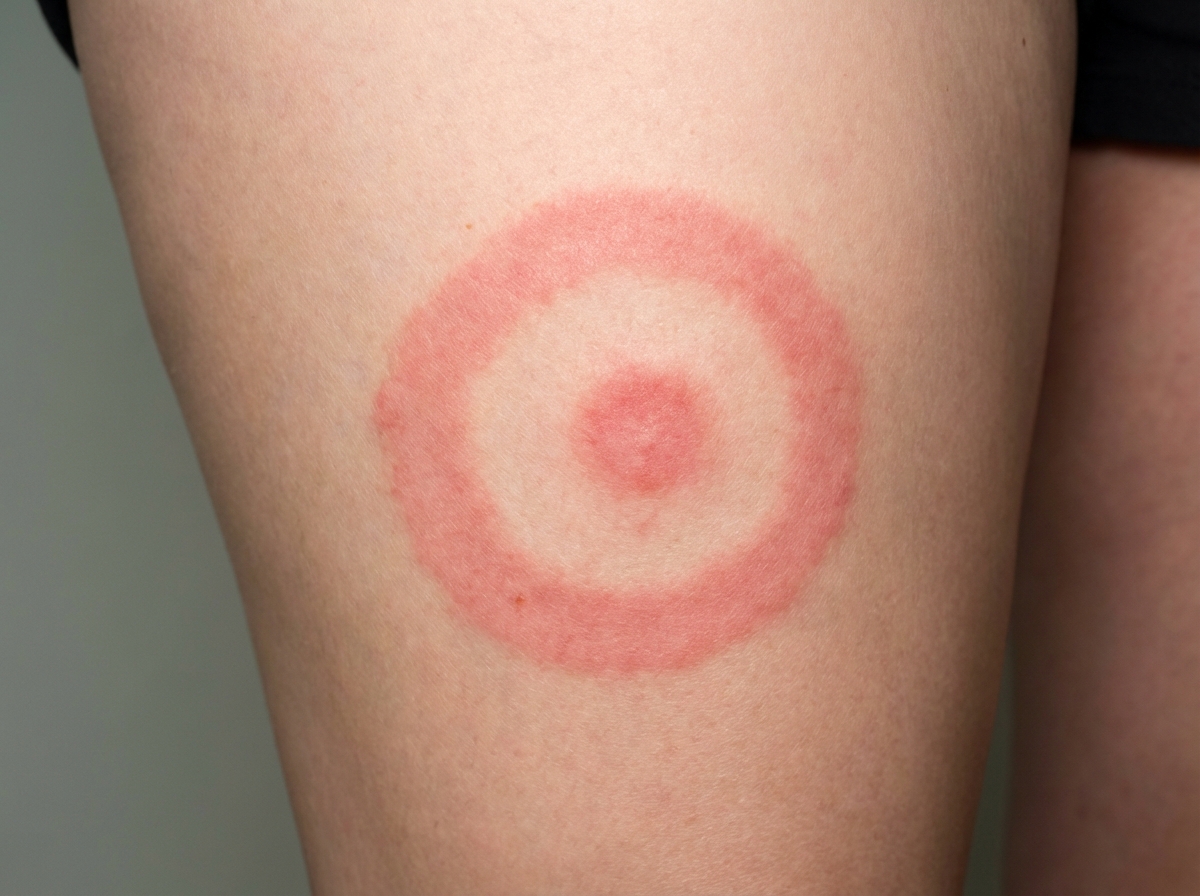
A 14-year-old girl presents with fever, headache, and muscle aches that have lasted for 2 days. She also complains of malaise and pain in her joints. She says she just returned from a camping trip in Delaware. Her past medical history is not significant. The patient denies any recent sick contacts. Her temperature is 38.3°C (101.0°F), pulse is 87/min, respirations are 17/min, and blood pressure is 120/78 mm Hg. On physical examination, there is a 3-inch-diameter, red, erythematous, round rash with central clearing on the right leg (see image). Antibodies against Proteus vulgaris OX-19 are absent. Which of the following is the most likely cause of this patient’s symptoms?
A young infant is brought to an immunologist because of recurrent infections, which have not resolved despite appropriate medical treatment. On reviewing her medical history, the immunologist notes that the child has had frequent disseminated mycobacterial infections. He suspects a possible immunodeficiency. What is the most likely cause of this patient's immunodeficiency?
An 18-year-old male in his first year of college presents to the emergency room with a fever and a severe headache. He reports having unprotected sex with several partners over the past few weeks. Upon examination, the male demonstrates nuchal rigidity and photophobia. His past medical history is notable for a lack of vaccinations beginning from infancy due to his parents' belief that vaccinations may cause autism. The bacteria causing these symptoms would most likely demonstrate which of the following?
A 15-year-old boy is brought to the emergency department by ambulance after his mother found him having muscle spasms and stiffness in his room. His mother stated he scraped his foot on a rusty razor on the bathroom floor 2 days prior. On presentation, his temperature is 102.0°F (38.9°C), blood pressure is 108/73 mmHg, pulse is 122/min, and respirations are 18/min. On physical exam, he is found to have severe muscle spasms and rigid abdominal muscles. In addition, he has a dirty appearing wound on his right foot. The patient's mother does not recall any further vaccinations since age 12. Finally, he is found to have difficulty opening his mouth so he is intubated. Which of the following treatment(s) should be provided to this patient?
A 27-year-old woman visits your office with a 3-day complaint of fever, malaise, myalgias, and headaches associated with vulvar itching, vulvar soreness, dysuria, and urethral discharge. The pain when urinating is so severe that she has attempted to avoid the use of the toilet. She just returned from a spring break in the tropics and explains that she had multiple unprotected sexual encounters with men and women. Upon physical examination, the temperature was 38.7°C (101.6°F) and the heart rate was 90/min. The pelvic examination revealed vulvar ulcers, vulvar excoriations, erythema, vaginal mucosa edema, and ulcerative cervicitis. Which of the following will best aid you in the identification of the specific organism causing the above symptoms?
An 11-year-old boy is brought to his pediatrician by his mother after he has complained of worsening left thumb pain for the last two weeks. The mother reports that the patient was previously healthy. Approximately 2 weeks ago, the family cat bit the patient’s thumb. The area around the bite wound then became red, hot, and slightly swollen and never healed. Earlier this week, the patient also started developing fevers that were recorded at home to be as high as 103.6°F. On exam, the patient's temperature is 102.2°F (39.0°C), blood pressure is 112/72 mmHg, pulse is 92/min, and respirations are 14/min. The patient’s left thumb is tender to touch over the proximal phalanx and the interphalangeal joint, but there is no obvious erythema or swelling. A radiograph performed in clinic is concerning for osteomyelitis at the proximal phalanx. Which of the following is the most likely cause of this patient’s condition?
A 14-year-old male is brought to the Emergency Department by his mother. She is worried because his face has become puffy and his urine has turned a tea-color. Patient history reveals the child recently suffered from a sore throat. The physician suspects a bacterial infection. Which of the following describes the likely bacteria responsible?
A 24-year old G1P0 mother with no prenatal screening arrives to the hospital in labor and has an uneventful delivery. The infant is full term and has no significant findings on physical exam. Shortly after birth, an erythromycin ophthalmic ointment is applied to the newborn in order to provide prophylaxis against infection. Which of the following is the most common mechanism of resistance to the ointment applied to this newborn?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
