Bacteria — MCQs

On this page
A 24-year-old woman presents to her primary care doctor with a lesion on her labia. She first noticed the lesion 2 days ago. It is not painful. She denies vaginal discharge or dysuria. She has no past medical history and takes no medications. She has had 4 sexual partners in the past 8 months and uses the pull-out method as contraception. She drinks 12-16 alcoholic beverages per week and is a law student. Her temperature is 97.8°F (36.6°C), blood pressure is 121/81 mmHg, pulse is 70/min, and respirations are 16/min. On exam, she has an indurated non-tender ulcer on the left labia majora. There is no appreciable inguinal lymphadenopathy. Multiple tests are ordered and pending. This patient's condition is most likely caused by a pathogen with which of the following characteristics on microscopic examination?
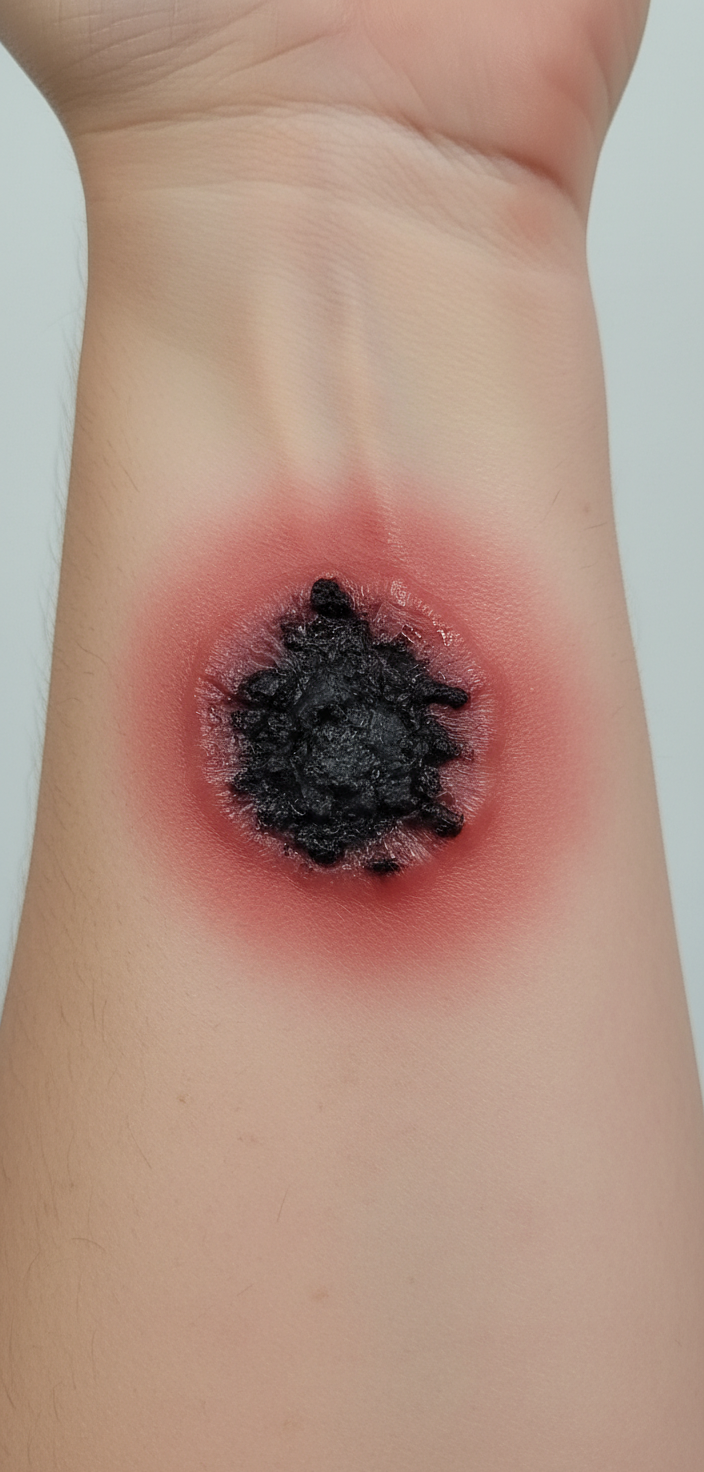
A 49-year-old man comes to the physician for evaluation of several painless, pruritic lesions on his left forearm that he first noticed 4 days ago. They were initially pink marks that progressed into blisters before ulcerating. He has also had a headache for 1 week. His temperature is 38.1°C (100.6°F). A photograph of one of the lesions is shown. There is pronounced edema of the surrounding skin and painless swelling of the left axillary lymph nodes. Which of the following is the greatest risk factor for this patient's condition?
A 36-year-old woman with a past medical history of diabetes comes to the emergency department for abdominal pain. She reports that a long time ago her gynecologist told her that she had “some cysts in her ovaries but not to worry about it.” The pain started last night and has progressively gotten worse. Nothing seems to make it better or worse. She denies headache, dizziness, chest pain, dyspnea, diarrhea, or constipation; she endorses nausea, dysuria for the past 3 days, and chills. Her temperature is 100.7°F (38.2°C), blood pressure is 132/94 mmHg, pulse is 104/min, and respirations are 14/min. Physical examination is significant for right lower quadrant and flank pain with voluntary guarding. What is the most likely pathophysiology of this patient’s condition?
A 24-year-old woman presents with fever, abdominal pain, and bloody bowel movements. She says her symptoms onset 2 days ago and have not improved. She describes the abdominal pain as moderate, cramping in character, and poorly localized. 1 week ago, she says she was on a camping trip with her friends and had barbecued chicken which she thought tasted strange. The patient denies any chills, hemoptysis, hematochezia, or similar symptoms in the past. The vital signs include: pulse 87/min and temperature 37.8°C (100.0°F). Physical examination is significant for moderate tenderness to palpation in the periumbilical region with no rebound or guarding. Stool is guaiac positive. Which of the following is a complication associated with this patient’s most likely diagnosis?
A 47-year-old woman presents to a local medical shelter while on a mission trip with her church to help rebuild homes after a hurricane. She has been experiencing severe nausea, vomiting, and diarrhea for the last 2 days and was feeling too fatigued to walk this morning. On presentation, her temperature is 99.2°F (37.3°C), blood pressure is 95/62 mmHg, pulse is 121/min, and respirations are 17/min. Physical exam reveals decreased skin turgor, and a stool sample reveals off-white watery stools. Gram stain reveals a gram-negative, comma-shaped organism that produces a toxin. Which of the following is consistent with the action of the toxin most likely involved in the development of this patient's symptoms?
A 67-year-old woman comes to the physician because of fever, chills, myalgias, and joint pain 1 month after undergoing aortic prosthetic valve replacement due to high-grade aortic stenosis. She does not drink alcohol or use illicit drugs. Her temperature is 39.3°C (102.8°F). She appears weak and lethargic. Physical examination shows crackles at both lung bases and a grade 2/6, blowing diastolic murmur over the right sternal border. Laboratory studies show leukocytosis and an elevated erythrocyte sedimentation rate. The causal organism is most likely to have which of the following characteristics?
A 28-year-old man comes to the physician for a pre-employment examination. He has no history of serious illness and takes no medications. A screening blood test is performed in which peptides are added to the sample to stimulate in vitro production of interferon-gamma, which is then measured using an enzyme-linked immunosorbent assay. This test is most likely to be helpful in diagnosing infection with which of the following pathogens?
A 27-year-old man who recently emigrated as a refugee from Somalia presents with fever, weight loss, fatigue, and exertional chest pain. He says his symptoms began 3 weeks ago and that his appetite has decreased and he has lost 3 kg (6.6 lb) in the last 3 weeks. He denies any history of cardiac disease. His past medical history is unremarkable. The patient admits that he has always lived in poor hygienic conditions in overcrowded quarters and in close contact with cats. His vital signs include: blood pressure 120/60 mm Hg, pulse 90/min, and temperature 38.0°C (100.4°F). Physical examination reveals generalized pallor. A cardiac examination reveals an early diastolic murmur loudest at the left third intercostal space. Abdominal examination reveals a tender and mildly enlarged spleen. Prominent axillary lymphadenopathy is noted. Laboratory investigations reveal a WBC count of 14,500/μL with 5% bands and 93% polymorphonuclear cells. An echocardiogram reveals a 5-mm vegetation on the aortic valve with moderate regurgitation. Three sets of blood cultures are taken over 24 hours followed by empiric antibiotic therapy with gentamicin and vancomycin. The blood cultures show no growth after 5 days. Following a week of empiric therapy, the patient continues to deteriorate. Which of the following would most likely confirm the diagnosis in this patient?
A 39-year-old woman presents to the emergency department with fever, cough, and shortness of breath. She reports developing flu-like symptoms 7 days ago but progressively worsened to the point where she experiences dyspnea on exertion. Her cough is accompanied by a mild amount of yellow sputum. Past medical history is notable for a previous admission to the hospital for pneumonia 4 months ago and an admission for bacteremia 6 weeks ago. She additionally has a history of IV heroin abuse, but her last use of heroin was 3 years ago. Temperature is 101.2°F (38.4°C), blood pressure is 104/70 mmHg, pulse is 102/min, and respirations are 20/min. Physical examination demonstrates coarse upper airway breath sounds over the right lower lung field. A faint 1/6 non-radiating systolic flow murmur is auscultated at the first right intercostal space. Abdominal examination is significant for moderate splenomegaly. Tenderness of the wrists and fingers is elicited on palpation, and range of motion is restricted. The patient comments that her range of motion and pain usually improve as the day goes on. Which of the following laboratory abnormalities is most likely to be found in this patient?
A 10-month-old boy is referred to the hospital because of suspected severe pneumonia. During the first month of his life, he had developed upper airway infections, bronchitis, and diarrhea. He has received all the immunizations according to his age. He failed to thrive since the age of 3 months. A month ago, he had a severe lung infection with cough, dyspnea, and diarrhea, and was unresponsive to an empiric oral macrolide. Upon admission to his local hospital, the patient has mild respiratory distress and crackles on auscultation. The temperature is 39.5°C (103.1°F), and the oxygen saturation is 95% on room air. The quantitative immunoglobulin tests show increased IgG, IgM, and IgA. The peripheral blood smear shows leukocytosis and normochromic normocytic anemia. The chloride sweat test and tuberculin test are negative. The chest X-ray reveals bilateral pneumonia. The bronchoalveolar lavage and gram stain report gram-negative bacteria with a growth of Burkholderia cepacia on culture. The laboratory results on admission are as follows: Leukocytes 36,600/mm3 Neutrophils 80% Lymphocytes 16% Eosinophils 1% Monocytes 2% Hemoglobin 7.6 g/dL Creatinine 0.8 mg/dL BUN 15 mg/dL Which of the following defects of neutrophil function is most likely responsible?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
