Bacteria — MCQs

On this page
During a humanitarian medical mission in rural Vietnam, a medical resident encounters a 50-year-old man with a year-long history of a pruritic rash on his upper body and face, along with numbness and tingling sensation of both of his palms. He mostly works on his family’s rice farm, where he also takes care of livestock. A physical examination revealed multiple erythematous macules and papules on the face, arms, chest, and back, as well as thinning of the eyebrows and loss of some eyelashes. Additional findings include hypopigmented macules around the elbows, which are insensitive to light touch, temperature, and pinprick. The grip strength is slightly diminished bilaterally with the conservation of both bicipital reflexes. What is the most likely diagnosis?
A previously healthy 5-year-old boy is brought to the physician with a recurring fever and malaise for 3 weeks. He has also had fatigue and loss of appetite. He initially presented 2 weeks ago with a maculopapular rash that has since resolved. At the time, he was given a prescription for amoxicillin-clavulanate. He denies sore throat or myalgias. He is home-schooled and has had no sick contacts. There are no pets at home, but he often visits a feline animal shelter where his mother volunteers. His temperature is 38.4°C (101.2°F). Physical examination shows a 1-cm papular lesion on the back of the right hand. He also has tender, bulky lymphadenopathy of the axillae and groin. Which of the following is the most appropriate next step in management?
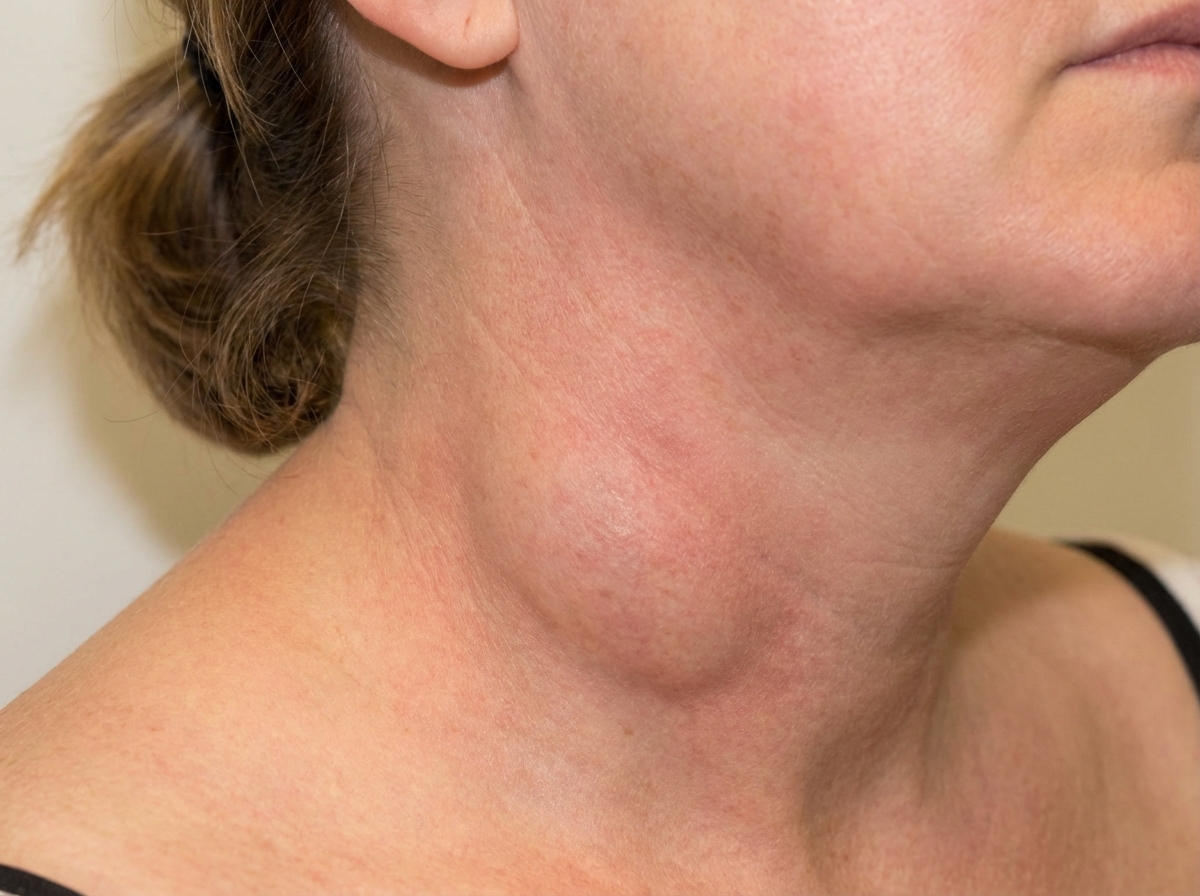
A 42-year-old woman presents because of a painful mass she first noticed on her neck 1 week ago (see image). The mass has grown over the last few days. She has no history of serious illness and takes no medications. On physical exam, her temperature is 38.0°C (100.4°F), pulse is 86/min, respirations are 12/min, blood pressure is 135/80 mm Hg. The mass is tender and relatively soft and mobile. The overlying skin is warm. On her right ear, there is a series of small and healing skin punctures left by the bite of her neighbor's kitten 3 weeks ago. No other mass is detected in the neck, supraclavicular, axillary, or inguinal regions. Oral examination reveals several discolored teeth. Her lungs are clear to auscultation and heart sounds are normal. A biopsy of the neck mass is performed. Which of the following would be most useful in establishing the diagnosis?
A 28-year-old man presents with a draining abscess on his left jaw. The patient states that he had a “bad tooth” a few weeks ago which has progressed to his current condition. His vital signs include: blood pressure 110/80 mm Hg, heart rate 85/min, and temperature 37.9°C (100.3°F). On physical examination, the patient has a 4 cm abscess on the left maxillary line that is draining a granulous, purulent material. Which of the following is the most likely causative organism of this abscess?
A 21-year-old U.S. born first year medical student with no prior hospital or healthcare work presents to the physician for a routine physical exam. The patient is HIV negative, denies drug use, and denies sick contacts. The physician places a purified protein tuberculin test in the patient's right forearm intradermally. What is the proper time to read the test and induration diameter that would indicate a positive test result?
A 43-year-old Caucasian male spent the past month on a business trip in the Caribbean. Two weeks following his return, he began experiencing diarrhea, pain in his abdomen, and a headache. He presents to the hospital and is noted to be febrile with prominent rose-colored spots on his chest and abdomen. Following recovery, the patient may become a carrier of the bacteria with the bacteria heavily localized to the:
Three days after undergoing coronary bypass surgery, a 67-year-old man becomes unresponsive and hypotensive. He is intubated, mechanically ventilated, and a central line is inserted. Vasopressin and noradrenaline infusions are begun. A Foley catheter is placed. Six days later, he has high unrelenting fevers. He is currently receiving noradrenaline via an infusion pump. His temperature is 39.6°C (102.3°F), pulse is 113/min, and blood pressure is 90/50 mm Hg. Examination shows a sternal wound with surrounding erythema; there is no discharge from the wound. Crackles are heard at both lung bases. Cardiac examination shows an S3 gallop. Abdominal examination shows no abnormalities. A Foley catheter is present. His hemoglobin concentration is 10.8 g/dL, leukocyte count is 21,700/mm3, and platelet count is 165,000/mm3. Samples for blood culture are drawn simultaneously from the central line and peripheral IV line. Blood cultures from the central line show coagulase-negative cocci in clusters on the 8th postoperative day, and those from the peripheral venous line show coagulase-negative cocci in clusters on the 10th postoperative day. Which of the following is the most likely diagnosis in this patient?
A group of microbiological investigators is studying bacterial DNA replication in E. coli colonies. While the cells are actively proliferating, the investigators stop the bacterial cell cycle during S phase and isolate an enzyme involved in DNA replication. An assay of the enzyme's exonuclease activity determines that it is active on both intact and demethylated thymine nucleotides. Which of the following enzymes have the investigators most likely isolated?
A 3-year-old girl is brought to the emergency department for 2 days of abdominal pain and watery diarrhea. This morning her stool had a red tint. She and her parents visited a circus 1 week ago. The patient attends daycare. Her immunizations are up-to-date. Her temperature is 38°C (100.4°F), pulse is 140/min, and blood pressure is 80/45 mm Hg. Abdominal examination shows soft abdomen that is tender to palpation in the right lower quadrant with rebound. Stool culture grows Yersinia enterocolitica. Exposure to which of the following was the likely cause of this patient's condition?
A 44-year-old Caucasian male presents with a fever, recent weight loss, and a cough productive of bloody sputum. A chest X-ray and CT scan were performed, revealing cavities near the apex of his lungs. The patient is started on rifampin, isoniazid, ethambutol and pyrazinamide. Formation of the cavities in the patient's lungs is mainly mediated by:
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
