Bacteria — MCQs

On this page
A 35-year-old patient with no significant past medical history arrives to the ED with abdominal cramps, nausea, and vomiting. He has had no recent travel or chemical exposures; however, three other members of his family also arrived concurrently to the ED with abdominal cramps, nausea, and vomiting. When asked about their recent activities, they recall that they had shared a lunch of leftover fried rice and soft boiled eggs about 5 hours earlier. The patients are otherwise afebrile and deny any history of diarrhea. Which of the following toxins is the most likely to have caused these symptoms?
A 4-year-old male is brought by his mother to the emergency room with dyspnea and fever. His mother reports a two-day history of progressive shortness of breath, malaise, and a fever with a maximum temperature of 101.6°F (38.7°C). The child has visited the emergency room three times over the past two years for pneumonia and otitis media. His family history is notable for sarcoidosis in his mother, diabetes in his father, and an early childhood death in his maternal uncle. His temperature is 101.2°F (38.4°C), blood pressure is 110/90 mmHg, pulse is 110/min, and respirations are 24/min. Physical examination reveals scant lymphoid tissue. A serological analysis reveals decreased levels of IgA, IgG, and IgM. This patient most likely has a defect in a protein that is active in which of the following cellular stages?
An 8-month-old boy is brought to his pediatrician by his parents with a 12-hour history of fever and coughing. He has also been experiencing intermittent diarrhea and skin abscesses since birth. Otherwise, he has been meeting developmental milestones as expected. Analysis of this patient's sputum reveals acute angle branching fungi, and culture shows gram-positive cocci in clusters. A flow cytometry reduction test was obtained that confirmed the diagnosis. Which of the following processes is most likely defective in this patient?
A 32 year-old African American man with a past medical history of sickle cell anemia presents to his primary care physician for a routine check-up. He has no complaints. His physician notes that he likely has an increased susceptibility to infections with certain organisms. Which of the following patient groups has a similar pattern of increased susceptibility?
A 7-year-old boy presents with difficult left eye-opening in the morning, eye discharge, and irritation. These symptoms developed gradually over the past week. He attends a primary school where recently an outbreak of tonsillitis took place. He had otitis media 2 weeks ago treated with ampicillin. At the presentation, the patient’s vital signs are within normal limits. Eye examination reveals bulbar conjunctival injection, mild eyelid edema, and a moderate mucopurulent discharge with crusts on the lower eyelid. There is no corneal or eyelid ulceration. No lymphadenopathy is noted. Which of the following investigations should be performed to establish a diagnosis before the treatment?
A family doctor in a rural area is treating a patient for dyspepsia. The patient had chronic heartburn and abdominal pain for the last 2 months and peptic ulcer disease due to a suspected H. pylori infection. For reasons relating to affordability and accessibility, the doctor decides to perform a diagnostic test in the office that is less invasive and more convenient. Which of the following is the most likely test used?
To protect against a potentially deadly infection, a 19-year-old female receives a vaccine containing capsular polysaccharide. This vaccine will stimulate her immune system to produce antibodies against which organism?
A 42-year-old woman presents to a medical office with complaints of fatigue, weight loss, and low-grade fever for 1 week. She noticed bleeding spots on her feet this morning. The past medical history is significant for a recent dental appointment. She is a non-smoker and does not drink alcohol. She does not currently take any medications. On examination, the vital signs include temperature 37.8°C (100.0°F), blood pressure 138/90 mm Hg, respirations 21/min, and pulse 87/min. Cardiac auscultation reveals a pansystolic murmur in the mitral area with radiation to the left axilla. Laboratory studies show hemoglobin levels of 17.2 g/dL, erythrocyte sedimentation rate (ESR) of 25 mm/h, and a white blood cell (WBC) count of 12,000 cells/mm3. An echocardiogram reveals valvular vegetations on the mitral valve with mild regurgitation. Blood samples are sent for bacterial culture. Empiric antibiotic therapy is initiated with ceftriaxone and vancomycin. The blood cultures most likely will yield the growth of which of the following organisms?
A 68-year-old man presents to the physician with fever, cough, weakness, night sweats, and poor appetite for the past 6 months. Medical records suggest that he has lost 7.5 kg (16.5 lb) of weight during this period. There is no history of breathlessness, nasal discharge, nasal obstruction, palpitations, chest pain, or symptoms related to digestion. He was released from prison 9 months ago after serving a 2-year sentence. His temperature is 38.1°C (100.6°F), pulse is 84/min, respirations are 16/min, and blood pressure is 122/80 mm Hg. Physical examination shows hepatomegaly and generalized lymphadenopathy, and auscultation of the chest reveals diffuse crackles throughout the lung fields bilaterally. On direct ophthalmoscopy, three discrete, yellow-colored, 0.5 mm to 1.0 mm lesions with indistinct borders are seen in the posterior pole. A chest X-ray is shown in the image. Tuberculin skin test with purified protein derivative is negative. What is the most likely diagnosis?
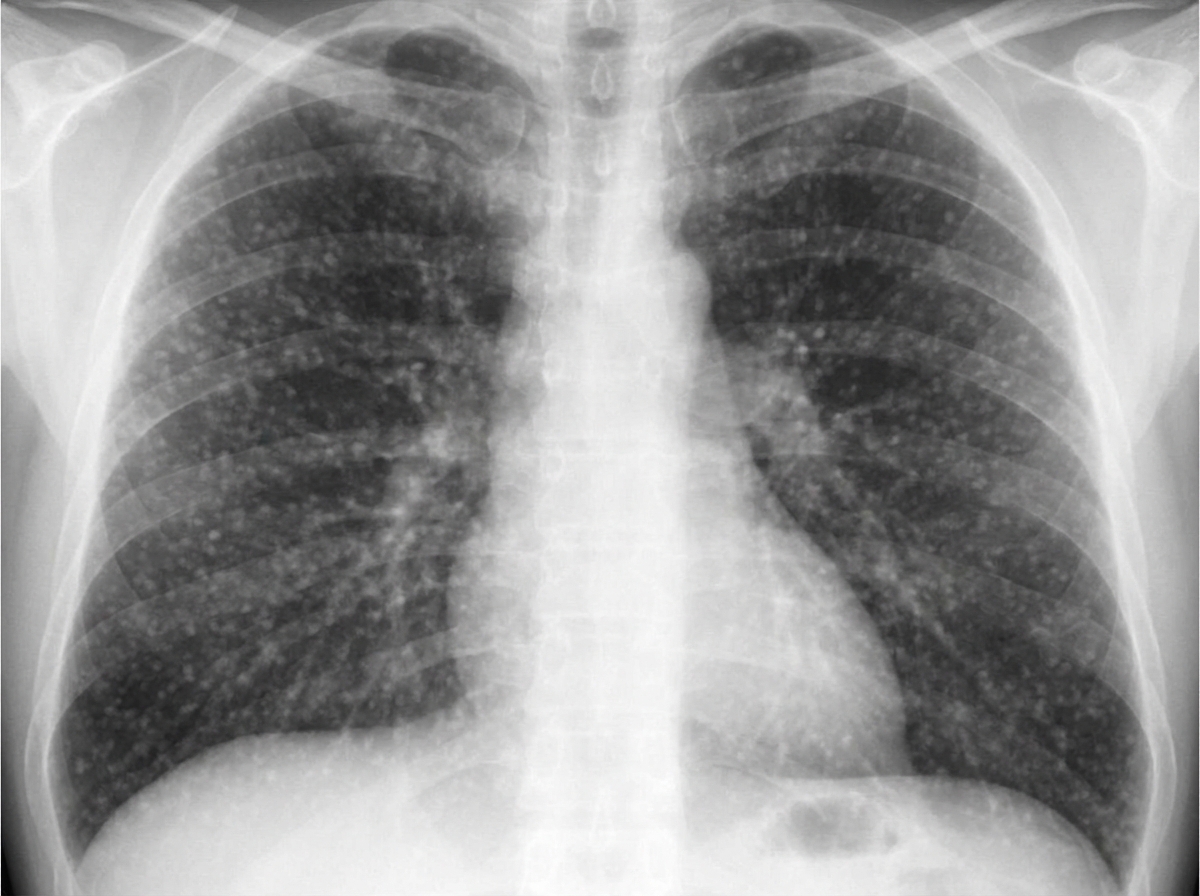
A 47-year-old alcoholic man presents to the office for a 72-hour history of intense right hemithorax pain. He also complains of fever, chills, and sweating that started 10 days ago, as well as persistent coughing with abundant malodorous sputum. Chest radiography shows a round consolidation with air-fluid levels in the middle third of the right hemithorax. Sputum samples for a direct exam, culture, and acid-fast bacilli (AFB) are sent. What is the correct diagnosis?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
