Bacteria — MCQs

On this page
A 25-year-old patient comes to the physician with complaints of dysuria and white urethral discharge. He is sexually active with 4 partners and does not use condoms. The physician is concerned for a sexually transmitted infection and decides to analyze the nucleic acid sequences present in the discharge to aid in diagnosis via DNA amplification. Which of the following is responsible for the creation of the nucleic acid copies during the elongation phase of the technique most likely used in this case?
A 32-year-old man comes to the physician because of low-grade fever and progressive painful lumps in his right groin for 6 days. The lumps have been discharging purulent fluid since the evening of the previous day. He had a shallow, painless lesion on his penis 3 weeks ago, but was too embarrassed to seek medical attention; it has resolved in the meantime. There is no personal or family history of serious illness. He has smoked one pack of cigarettes daily for 12 years. He is sexually active with multiple male partners and uses condoms inconsistently. His temperature is 38.0°C (100.4°F). Examination of his groin shows multiple masses discharging pus. The remainder of the examination shows no abnormalities. Which of the following is the most likely causal organism?
An outbreak of diphtheria has occurred for the third time in a decade in a small village in South Africa. Diphtheria is endemic to the area with many healthy villagers colonized with different bacterial strains. Vaccine distribution in this area is difficult due to treacherous terrain. A team of doctors is sent to the region to conduct a health campaign. Toxigenic strains of C. diphtheria are isolated from symptomatic patients. Which of the following best explains the initial emergence of a pathogenic strain causing such outbreaks?
A previously healthy 10-day-old infant is brought to the emergency department by his mother because of episodes of weakness and spasms for the past 12 hours. His mother states that he has also had difficulty feeding and a weak suck. He has not had fever, cough, diarrhea, or vomiting. He was born at 39 weeks' gestation via uncomplicated vaginal delivery at home. Pregnancy was uncomplicated. The mother refused antenatal vaccines out of concern they would cause side effects. She is worried his symptoms may be from some raw honey his older sister maybe inadvertently fed him 5 days ago. He appears irritable. His temperature is 37.1°C (98.8°F). Examination shows generalized muscle stiffness and twitches. His fontanelles are soft and flat. The remainder of the examination shows no abnormalities. Which of the following is the most likely causal organism?
A group of medical students is studying bacteria and their pathogenesis. They have identified that a substantial number of bacteria cause human disease by producing exotoxins. Exotoxins are typically proteins, but they have different mechanisms of action and act at different sites. The following is a list of exotoxins together with mechanisms of action. Which of the following pairs is correctly matched?
A 9-month-old girl is brought in by her father for a scheduled check-up with her pediatrician. He states that over the past 4-5 months she has had multiple ear infections. She was also hospitalized for an upper respiratory infection 2 months ago. Since then she has been well. She has started to pull herself up to walk. Additionally, the patient’s medical history is significant for eczema and allergic rhinitis. The father denies any family history of immunodeficiencies. There are no notable findings on physical exam. Labs are remarkable for low IgG levels with normal IgA, IgE, and IgM levels. Which of the following is the most likely etiology for the patient’s presentation?
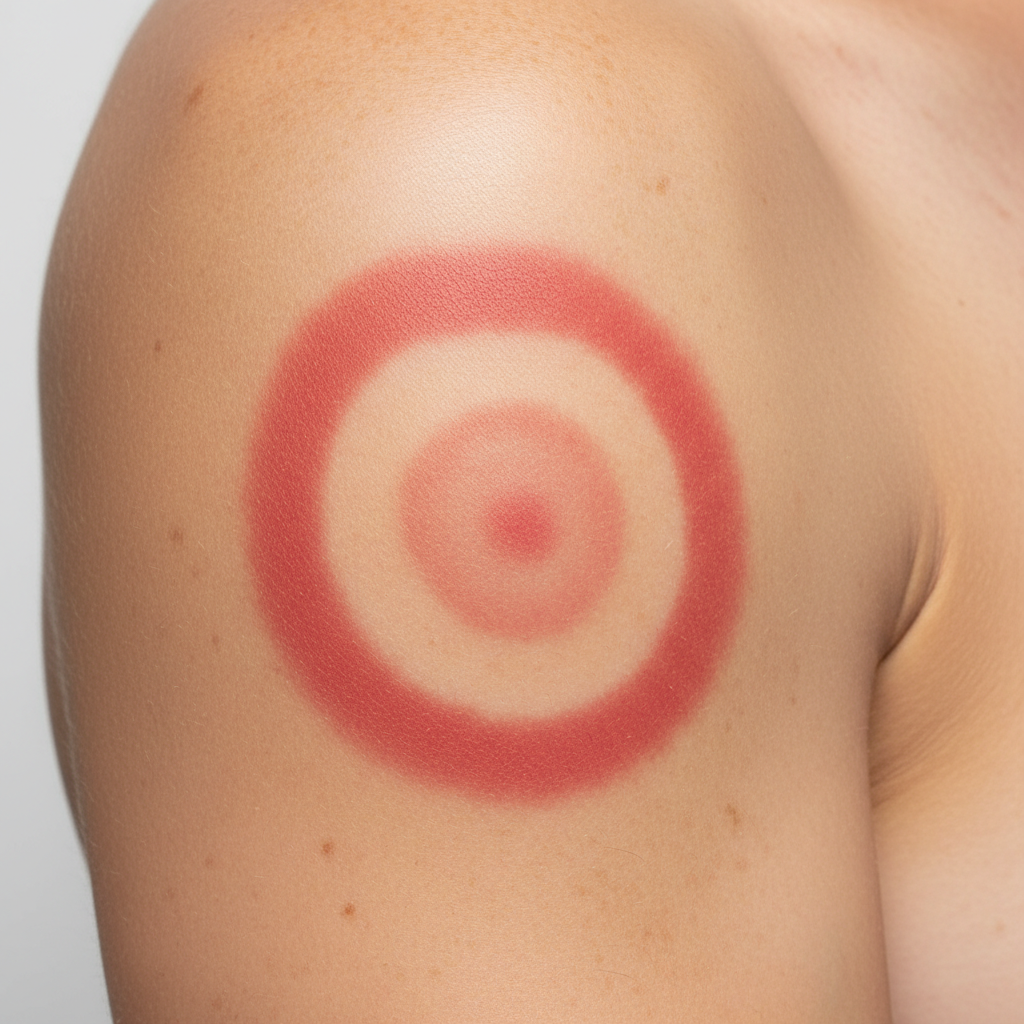
A 12-year-old girl presents to the pediatric dermatologist with an expanding, but otherwise asymptomatic erythematous patch on her right shoulder, which she first noticed 3 days ago. The girl states the rash started as a small red bump but has gradually progressed to its current size. No similar lesions were observed elsewhere by her or her mother. She has felt ill and her mother has detected intermittent low-grade fevers. During the skin examination, a target-like erythematous patch, approximately 7 cm in diameter, was noted on the right shoulder (as shown in the image). Another notable finding was axillary lymphadenopathy. On further questioning it was revealed that the patient went camping with her grandfather approximately 11 days ago; however, she does not recall any insect bites or exposure to animals. The family has a pet cat living in their household. Based on the history and physical examination results, what is the most likely diagnosis?
A 54-year-old woman comes to the physician because of lower back pain, night sweats, and a 5-kg (11-lb) weight loss during the past 4 weeks. She has rheumatoid arthritis treated with adalimumab. Her temperature is 38°C (100.4°F). Physical examination shows tenderness over the T10 and L1 spinous processes. Passive extension of the right hip causes pain in the right lower quadrant. The patient's symptoms are most likely caused by an organism with which of the following virulence factors?
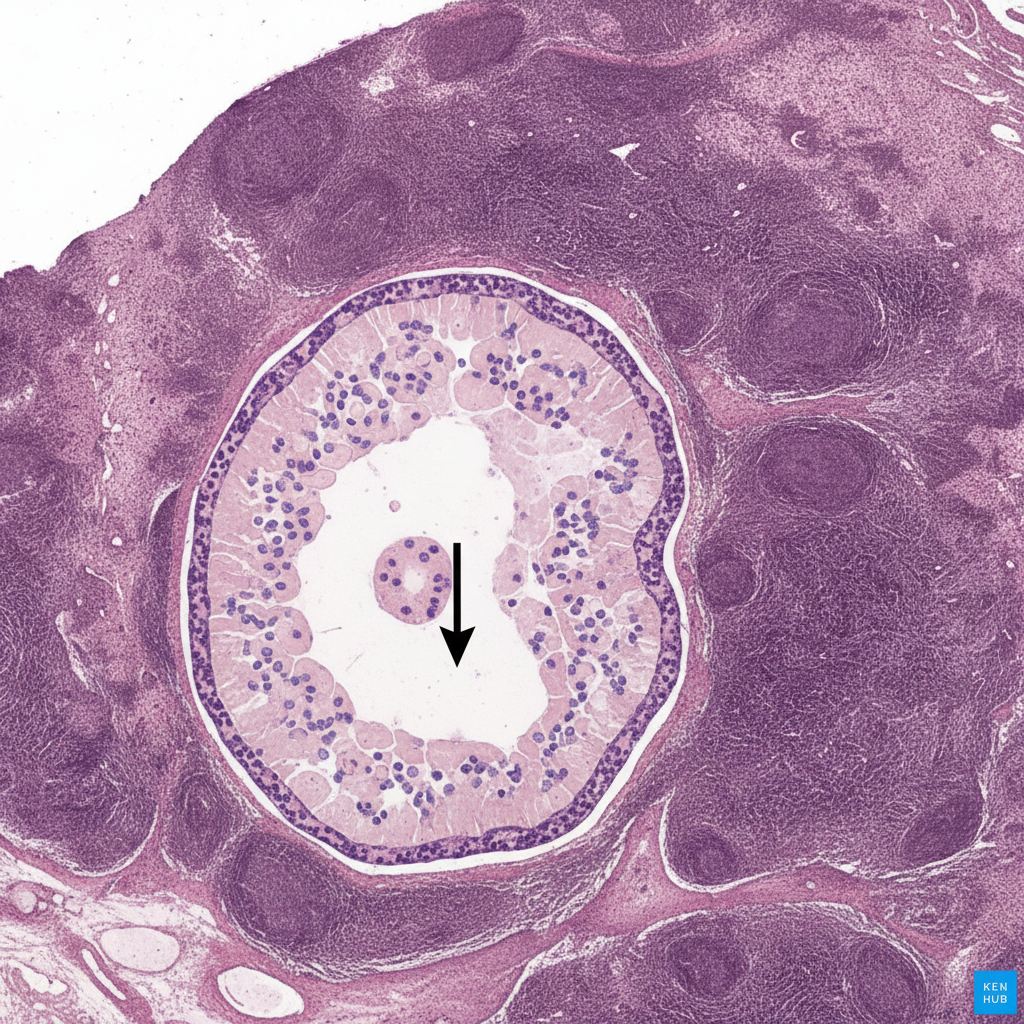
A study is designed to assess the functions of immune components. The investigator obtains a lymph node biopsy from a healthy subject and observes it under a microscope. A photomicrograph of the cross-section of this lymph node is shown. Which of the following immunologic processes most likely occurs in the region labeled with an arrow?
A 3-year-old recent immigrant is diagnosed with primary tuberculosis. Her body produces T cells that do not have IL-12 receptors on their surface, and she is noted to have impaired development of Th1 T-helper cells. Which of the following cytokines would benefit this patient?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
