Bacteria — MCQs

On this page
A group of scientists studied the effects of cytokines on effector cells, including leukocytes. They observed that interleukin-12 (IL-12) is secreted by antigen-presenting cells (APCs) in response to bacterial lipopolysaccharide. When a CD4+ T cell is exposed to this interleukin, which of the following responses will it have?
A 23-year-old man comes to the physician because of progressive pain, redness, and swelling of his left forearm. The symptoms began after he scratched his arm on a metal table 4 days ago. Examination of the left forearm shows a 2-cm, tender, erythematous, fluctuant lesion at the site of trauma. Incision and drainage of the lesion is performed and a small amount of thick, white liquid is expressed. Which of the following cytokines is involved in the recruitment of the primary cell type found in this liquid?
A 16-year-old female presents to her pediatrician complaining of 2 weeks of fever and 1 week of swollen lumps in her left armpit. Upon examination of the left upper extremity, her physician notes the presence of a single papule which the patient claimed appeared one week ago. The patient started her first job at a pet store 2.5 weeks ago. Which of the following is the vector of transmission of the causative agent?
A 3-year-old boy is brought to the physician for evaluation of a generalized, pruritic rash. The rash began during infancy and did not resolve despite initiating treatment with topical corticosteroids. Three months ago, he was treated for several asymptomatic soft tissue abscesses on his legs. He has been admitted to the hospital three times during the past two years for pneumonia. Physical examination shows a prominent forehead and a wide nasal bridge. Examination of the skin shows a diffuse eczematous rash and white plaques on the face, scalp, and shoulders. Laboratory studies show a leukocyte count of 6,000/mm3 with 25% eosinophils and a serum IgE concentration of 2,300 IU/mL (N = 0–380). Flow cytometry shows a deficiency of T helper 17 cells. The patient’s increased susceptibility to infection is most likely due to which of the following?
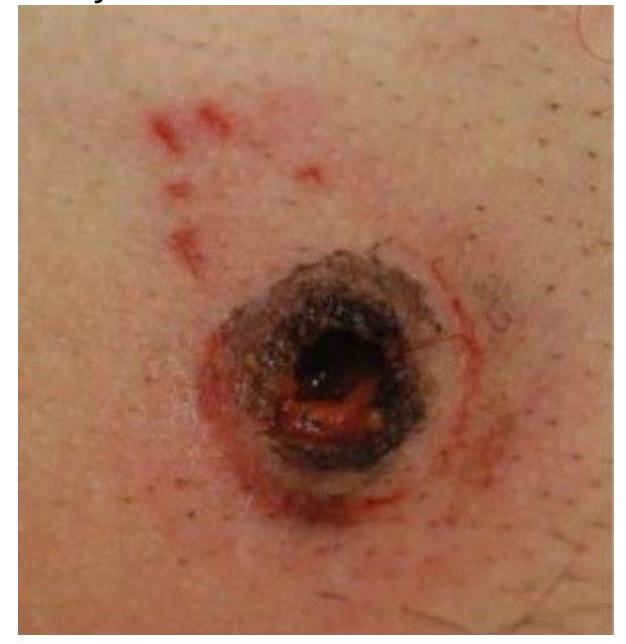
A 62-year-old woman with metastatic breast cancer comes to the physician because of a 2-day history of fever, chills, and new gluteal lesions. The lesions began as painless red macules and evolved into painful ulcers overnight. She received her fourth course of palliative chemotherapy 2 weeks ago. Her temperature is 38.2°C (100.8°F). Laboratory studies show a leukocyte count of 2,000/mm3 (20% segmented neutrophils). A photograph of one of the skin lesions is shown. Which of the following virulence factors is most likely involved in the pathogenesis of this patient's skin finding?
A 27-year-old man presents to the emergency department with general weakness and fatigue. He states that he has not felt well for several days and can't take care of himself anymore due to fatigue. The patient has a past medical history of IV drug abuse, alcohol abuse, and multiple minor traumas associated with intoxication. His temperature is 104°F (40°C), blood pressure is 127/68 mmHg, pulse is 120/min, respirations are 19/min, and oxygen saturation is 98% on room air. A murmur is heard on cardiac exam. The patient is treated appropriately and transferred to the inpatient floor and recovers over the next several days. The patient has been unable to eat solids, though he has been drinking large amounts of juice. On day 5 of his stay, the patient states he feels much better. He is no longer febrile. His only concern is profuse and watery diarrhea and severe abdominal pain which he has been experiencing since yesterday. The patient is started on IV fluids and given oral fluid replacement as well. Which of the following is associated with the most likely underlying diagnosis?
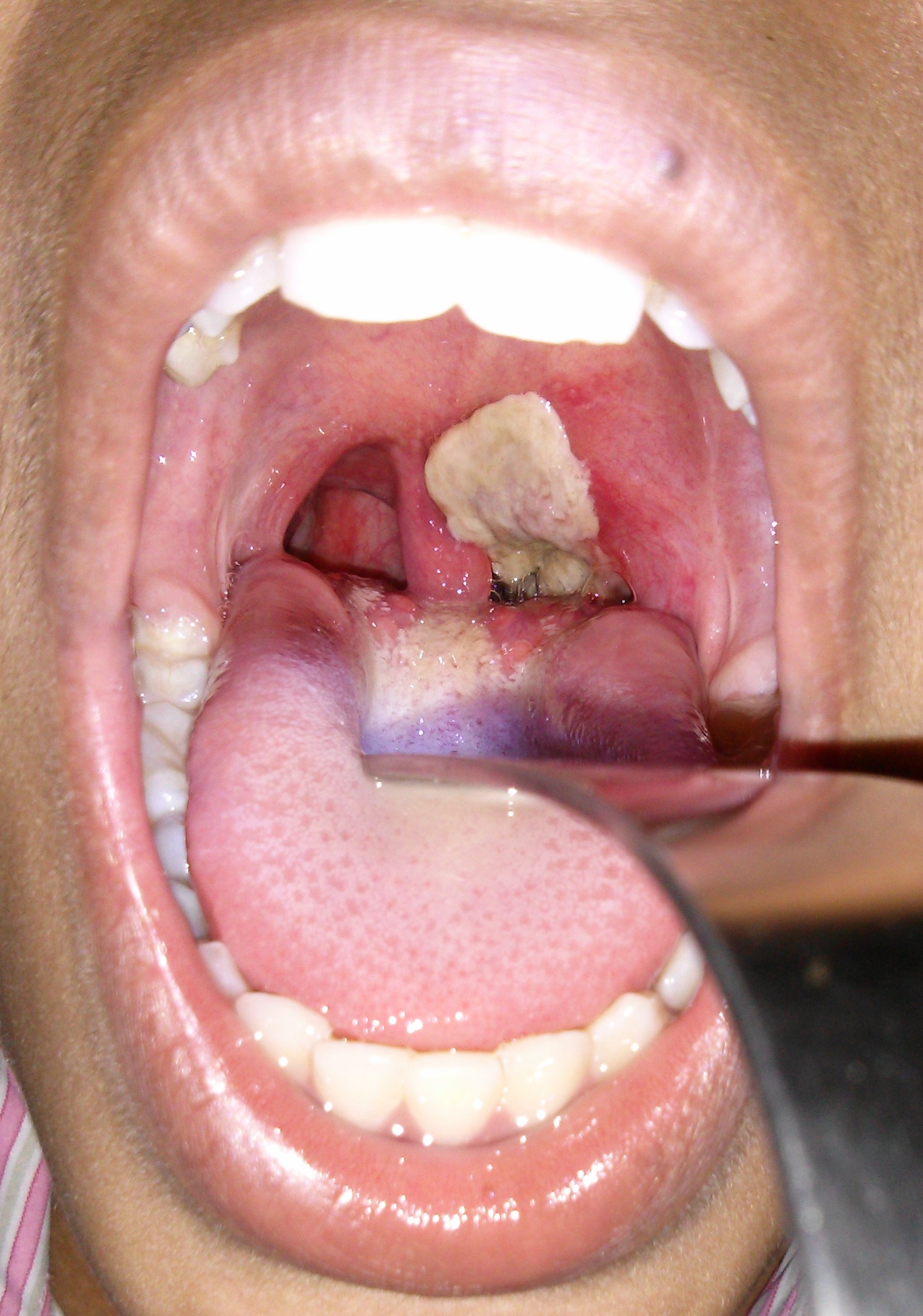
A young immigrant girl presents with low-grade fever, sore throat, painful swallowing, and difficulty in breathing. Her voice is unusually nasal and her swollen neck gives the impression of “bull's neck”. On examination, a large gray membrane is noticed on the oropharynx as shown in the picture. Removal of the membrane reveals a bleeding edematous mucosa. Culture on potassium tellurite medium reveals several black colonies. What is the mechanism of action of the bacterial toxin responsible for this condition?
An investigator studying immune response administers a 0.5 mL intradermal injection of an autoclaved microorganism to a study volunteer. Four weeks later, there is a 12-mm, indurated, hypopigmented patch over the site of injection. Which of the following is the most likely explanation for the observed skin finding?
A bacterial isolate obtained from a hospitalized patient is found to be resistant to amikacin. The isolated bacteria most likely has which of the following characteristics?
A 32-day-old boy is brought to the emergency department because he is found to be febrile and listless. He was born at home to a G1P1 mother without complications, and his mother has no past medical history. On presentation he is found to be febrile with a bulging tympanic membrane on otoscopic examination. Furthermore, he is found to have an abscess around his rectum that discharges a serosanguinous fluid. Finally, the remnants of the umbilical cord are found to be attached and necrotic. Which of the following processes is most likely abnormal in this patient?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
