Bacteria — MCQs

On this page
A previously healthy 13-year-old girl is brought to the physician by her parents because of a 2-day history of low-grade fever, headache, nausea, and a sore throat. Examination of the oral cavity shows enlarged, erythematous tonsils with exudates and palatal petechiae. There is cervical lymphadenopathy. Her parents agree to her participating in a study of microbial virulence factors. A culture of the girl's throat is obtained and an organism is cultivated. The physician finds that the isolated organism is able to withstand phagocytosis when placed in fresh blood. The most likely explanation for this finding is the expression of which of the following?
A 55-year-old man presents with fever, chills, fatigue, cough, sore throat, and breathlessness for the past 7 days. He describes the cough as productive and says he is fatigued all the time. He says he is a farmer with daily contact with rabbits, horses, sheep, pigeons, and chickens and reports cleaning the barn 3 days before his symptoms started. The patient denies any history of tick bites. Past medical history is irrelevant. His temperature is 39.4°C (103.0°F), pulse is 110/min, and respirations are 26/min. On physical examination, there are decreased breath sounds on the right side. A large tender node is palpable in the right axilla. A chest radiograph reveals multiple homogenous opacities in the lower lobe of the right lung and a right-sided pleural effusions. Gram staining of a sputum sample is negative for any organism. Serology tests are negative. Which of the following is the most likely causative organism for this patient’s condition?
A 4-year-old boy presents with bloody diarrhea. The patient’s mother states that he was fine this morning, but around midday, she received a call from his daycare center stating that the patient had a single bloody bowel movement. His mother states that there have been no recent changes in his diet, although they did attend a barbecue over the weekend. The patient has no recent history of fever, chills, or similar symptoms in the past. No significant past medical history. Initial laboratory studies show an elevated white blood cell (WBC) count, anemia, and a blood urea nitrogen (BUN)/creatinine ratio of 40. Stool examination shows 3+ blood but no fecal leukocytes. Which of the following tests would be diagnostic for this patient’s most likely condition?
A 10-month-old boy is brought to the emergency department by his parents because he has a high fever and severe cough. His fever started 2 days ago and his parents are concerned as he is now listless and fatigued. He had a similar presentation 5 months ago and was diagnosed with pneumonia caused by Staphylococcus aureus. He has been experiencing intermittent diarrhea and skin abscesses since birth. The child had an uneventful birth and the child is otherwise developmentally normal. Analysis of this patient's sputum reveals acute angle branching fungi and a throat swab reveals a white plaque with germ tube forming yeast. Which of the following is most likely to be abnormal in this patient?
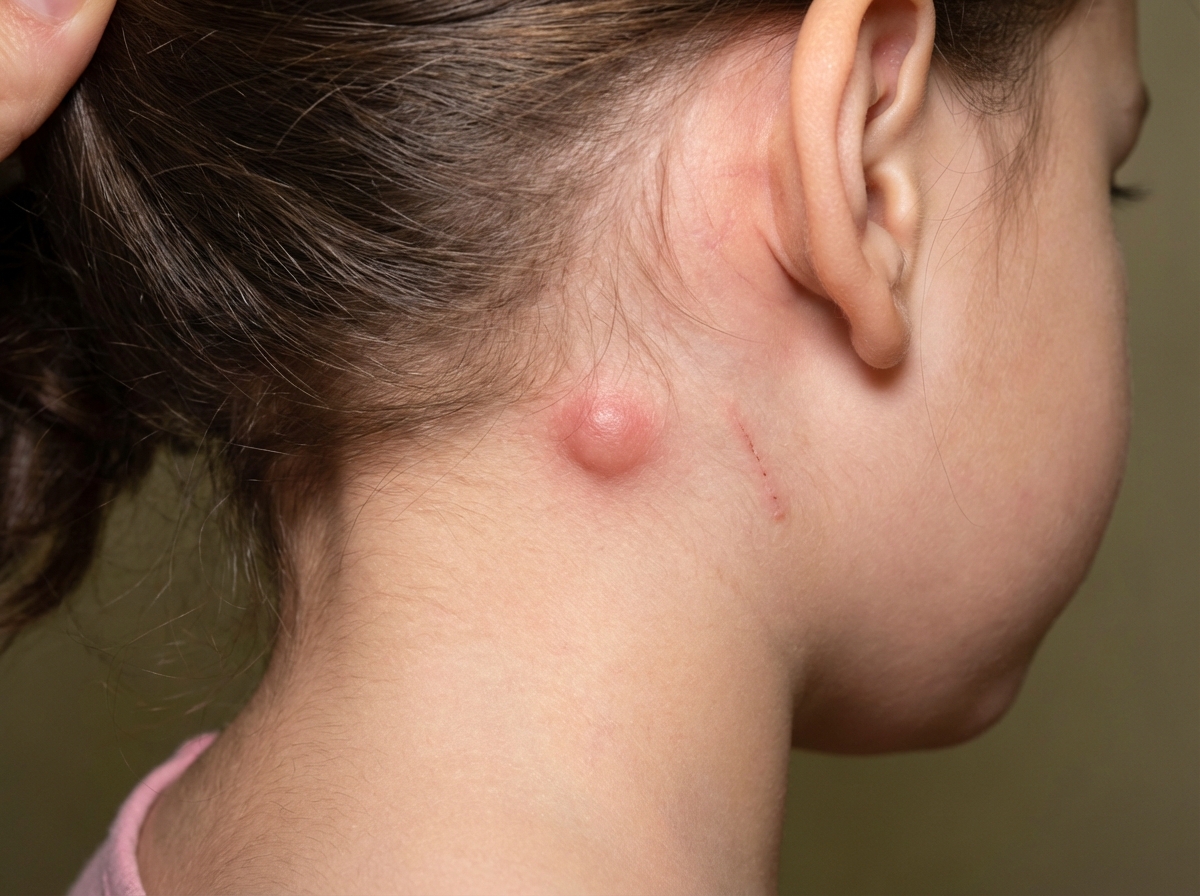
An 8-year-old girl is brought into your clinic with a 5 day history of decreased oral intake, body aches and lymphadenopathy. She has no significant medical history. Upon further questioning you find that the patient frequently plays outside, where she enjoys chasing the neighborhood cats and dogs. She has had no recent sick contacts or travel to foreign countries. The patients vital signs are: temperature 100.4F, HR 80, BP 105/75 and RR 15. Physical exam is significant for a 1-cm erythematous and tender lymph node in the right posterior cervical area (Figure 1). There is a nearly healed scratch in the right occipital region. What is the most likely diagnosis for this patient?
A scientist is studying the process by which innate immune cells are able to respond to damage and pathogen infiltration. Specifically, she examines patients with an immunodeficiency where they are unable to respond to local infections. She notices that these patients do not produce pustulant fluid and do not have recruitment of immune cells in the first several hours of inflammation. Examining neutrophils within these patients reveals that they are able to slow their movement in a flow chamber by loosely attaching to purified vessel tissues. Subsequently, she shows that the neutrophils attach tightly to these vessel walls and move across the walls to the other side. Finally, when different levels of pathogenic proteins are placed on two sides of a purified vessel wall, the neutrophils from this patient do not exhibit a preference between the two sides. The step of neutrophil recruitment that is most likely defective in this patient involves which of the following mediators?
A 46-year-old man is brought to the emergency room by police after being found passed out on the sidewalk. He is intermittently alert and smells strongly of alcohol. He is unable to provide a history, but an electronic medical record search reveals that the patient has a history of alcohol abuse and was seen in the emergency room twice in the past year for alcohol intoxication. Further review of the medical record reveals that he works as a day laborer on a farm. His temperature is 98.8°F (37.1°C), blood pressure is 122/78 mmHg, pulse is 102/min, and respirations are 14/min. On examination, he is somnolent but arousable. He has vomitus on his shirt. He is given intravenous fluids and provided with supportive care. He vomits twice more and is discharged 6 hours later. However, 6 days after discharge, he presents to the emergency room again complaining of shortness of breath and fever. His temperature is 102°F (38.9°C), blood pressure is 100/58 mmHg, pulse is 116/min, and respirations are 24/min. The patient is actively coughing up foul-smelling purulent sputum. Which of the following is the most likely cause of this patient’s current symptoms?
An autopsy of a 75-year-old man reveals obliterating endarteritis of the vasa vasorum of the aorta. Which of the following investigations will most likely be positive in this patient?
A group of scientists is studying various methods of bacterial reproduction. They find out that bacteria also exchange genetic material via these reproductive processes. They are about to study one such method known as bacterial conjugation. Which of the following occurs through bacterial conjugation?
Ten days after undergoing left hip replacement, a 73-year-old hospitalized man develops a fever, dyspnea, cough productive of yellow sputum, confusion, nausea, and diarrhea. Several patients in the hospital report similar symptoms. Physical examination shows decreased breath sounds on the left side and inspiratory crackles over the left lung. An x-ray of the chest shows opacities in the lower lobe of the left lung. Treatment with ampicillin does not improve his symptoms. Subsequent evaluation of the patient's urine detects a pathogen-specific antigen, confirming the diagnosis. Which of the following sources of infection is most likely responsible for this local disease outbreak?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
