Bacteria — MCQs

On this page
A 33-year-old man presents to the emergency department with a fever and fatigue. He states that he has not felt well since he returned from a hiking trip in Alabama. He is generally healthy and has no other medical conditions. His temperature is 101°F (38.3°C), blood pressure is 127/85 mmHg, pulse is 108/min, respirations are 14/min, and oxygen saturation is 99% on room air. Physical exam including a full dermatologic inspection is unremarkable. Laboratory studies are ordered as seen below. Hemoglobin: 13 g/dL Hematocrit: 39% Leukocyte count: 2,200/mm^3 with normal differential Platelet count: 77,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 24 mEq/L BUN: 19 mg/dL Glucose: 98 mg/dL Creatinine: 1.3 mg/dL Ca2+: 10.2 mg/dL AST: 92 U/L ALT: 100 U/L Which of the following is the most likely diagnosis?
A 42-year-old man presents to the emergency department with a 3-day history of fever and severe back pain. The fever is high-grade, continuous, without chills and rigors. The back pain is severe, localized to the thoracic region, and aggravated by deep breathing. The patient tried taking ibuprofen with little improvement. Past medical history is significant for essential hypertension, dyslipidemia, hyperuricemia, and bronchial asthma. Current medicines include allopurinol, amlodipine, atorvastatin, clopidogrel, montelukast, and a corticosteroid inhaler. The patient reports a 25-pack-year smoking history and drinks alcohol only socially. His vital signs include: blood pressure 152/94 mm Hg, pulse 101/min, temperature 39.5°C (103.1°F). BMI 36.8 kg/m2. On physical examination, the patient is alert and oriented. Multiple injection marks are visible around the left-sided cubital fossa and hand veins. The neck is supple on head flexion. Point tenderness is present in the thoracic region at the midline. Motor and sensory examinations are unremarkable with normal deep tendon reflexes. Laboratory findings are significant for the following: Hemoglobin 14.5 mg/dL White blood cell 24,500/mm3 Platelets 480,000/mm3 BUN 28 mg/dL Creatinine 1.1 mg/dL ESR 45 mm/hr C-reactive protein 84 mg/dL Sodium 144 mEq/L Potassium 4.1 mEq/L Calcium 9.7 mEq/L A contrast MRI of the spine reveals a peripherally enhancing dorsal epidural process compressing the thecal sac and causing a mild leftwards displacement. Which of the following is the most likely risk factor for this patient’s condition?
A 24-year-old man presents with a painless genital ulcer for the past 2 weeks. He reports that he recently has been having unprotected sex with multiple partners. Past medical history is unremarkable. On physical examination, a single ulcer is present on the dorsal shaft of the penis which is circumscribed, indurated, and partially healed. There is moderate inguinal lymphadenopathy but no buboes. Which of the following tests would confirm the most likely diagnosis in this patient?
A 1-year-old girl is brought to the physician for a well-child examination. She has no history of serious illness. She receives a vaccine in which a polysaccharide is conjugated to a carrier protein. Which of the following pathogens is the most likely target of this vaccine?
A 10-year-old girl presents to your office with a fever and rash. Her mother first noticed the rash 2 days ago after a camping trip. The rash began on her wrists and ankles and has now spread to her palms and the soles of her feet. This morning, she was feeling unwell and complaining of a headache. She had a fever of 102°F (39°C) prompting her mother to bring her to your office. She is otherwise healthy and does not take any medications. Her medical history is significant for a broken arm at age 8. On physical exam her blood pressure is 120/80 mmHg, pulse is 110/min, and respirations are 22/min. You notice a petechial rash on the palms, soles, ankles, and wrists. Which of the following findings would confirm the most likely cause of this patient's symptoms?
A 45-year-old woman comes to the emergency department because of abdominal cramping, vomiting, and watery diarrhea for the past 4 hours. One day ago, she went to a seafood restaurant with her family to celebrate her birthday. Three of the attendees have developed similar symptoms. The patient appears lethargic. Her temperature is 38.8°C (101.8°F). Which of the following organisms is most likely responsible for this patient's current symptoms?
A child is brought into the emergency room by her mother. Her mother states that the 7-year-old child was playing with their dog, who is up to date on his vaccinations. When the dog started playing more aggressively, the child suffered a bite on the hand with two puncture wounds from the dog's canines. The child is up-to-date on her vaccinations and has no medical history. Her vitals are within normal limits. If this bite becomes infected, what is the most likely organism to be the cause of infection?
A 25-year-old G1P0 female of Middle Eastern descent gives birth to a male infant at 38 weeks' gestation. The child is in the 15th percentile for both height and weight. Over the course of the first six months of the child's life, he develops multiple severe skin and mucosal infections characterized by dramatically elevated white blood cell counts. The patient also demonstrates mental retardation soon after birth. A thorough hematologic analysis via flow cytometry reveals that the child's neutrophils lack Sialyl-Lewis X. Which of the following processes is likely deficient in this patient?
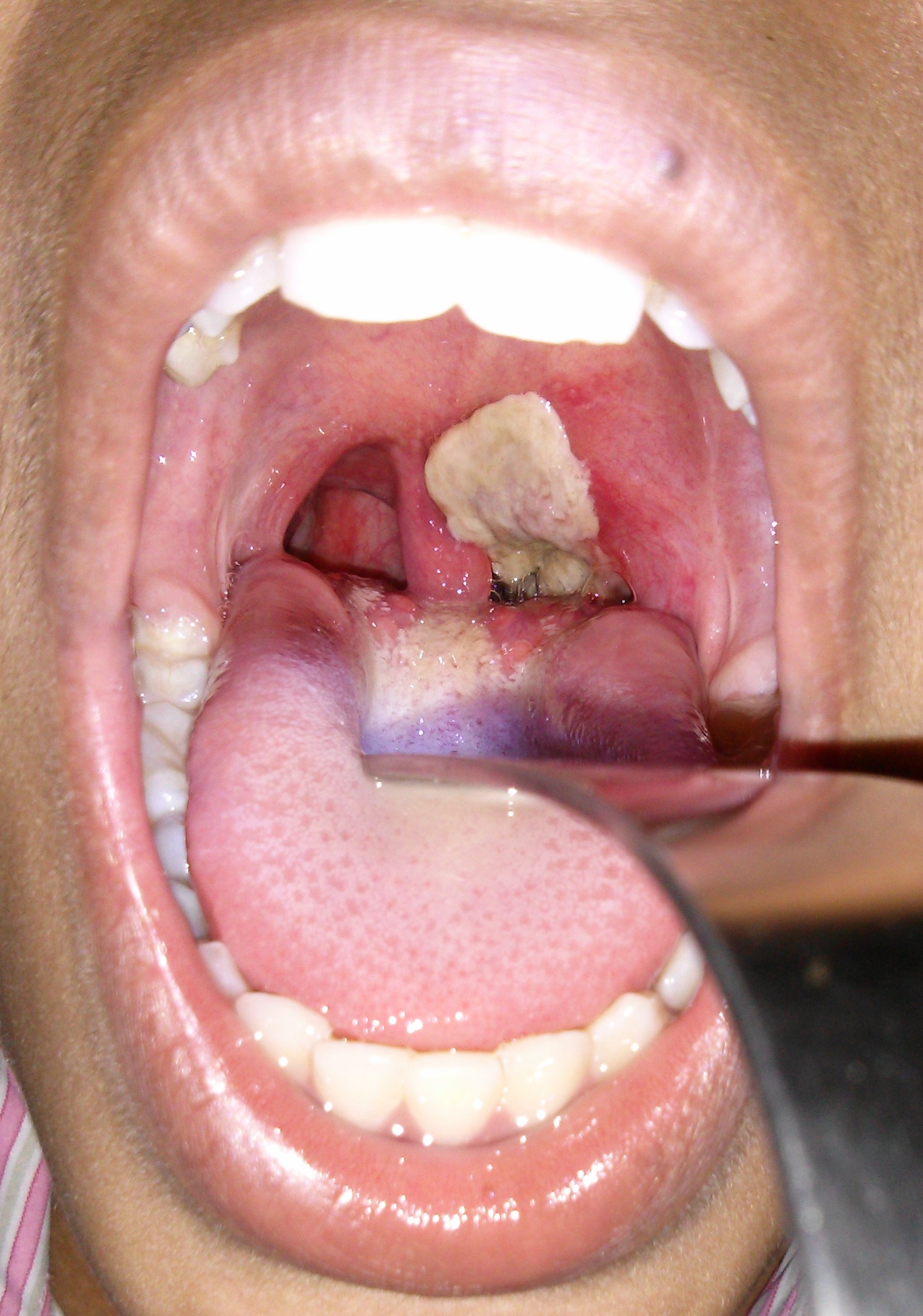
A 12-year-old boy presents to the emergency room with difficulty breathing after several days of severe sore throat. Further history reveals that his family immigrated recently from Eastern Europe and he has never previously seen a doctor. Physical exam shows cervical lymphadenopathy with extensive neck edema as well as the finding shown in the image provided. You suspect a bacteria that causes the disease by producing an AB type exotoxin. Which of the following is the proper medium to culture the most likely cause of this infection?
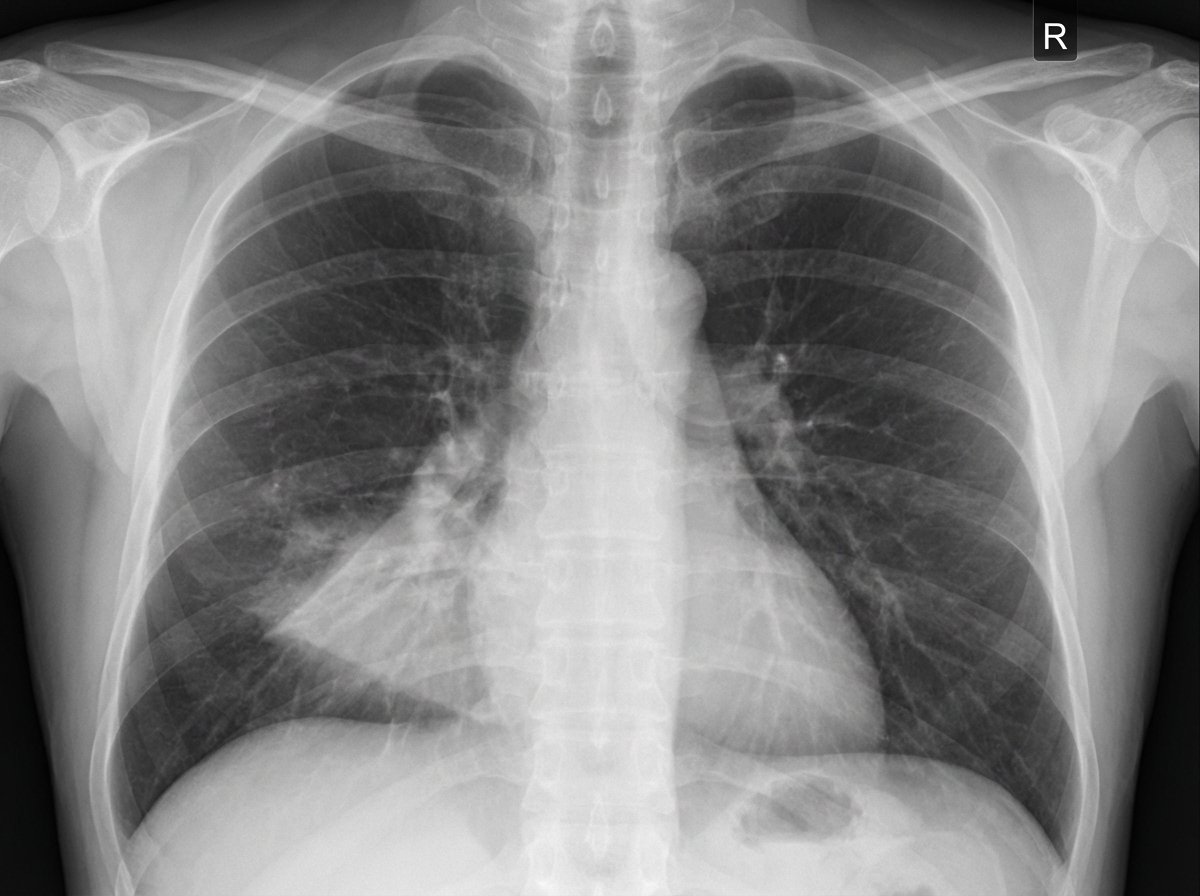
A previously healthy 46-year-old woman comes to the physician with a one-week history of productive cough and fatigue. Two weeks ago, she had fever, nasal congestion, rhinorrhea, and myalgias that resolved with supportive care. She has not traveled out of the United States. Pulmonary examination shows dullness to percussion and increased fremitus at the right middle lobe. An x-ray of the chest is shown. A sputum sample is most likely to show which of the following findings?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
