Bacteria — MCQs

On this page
A 24-year-old man presents to the emergency department for bloody stools. The patient states that he has had bloody diarrhea for the past 3 days without improvement. He recently returned from a camping trip where he drank stream water and admits to eating undercooked meats which included beef, chicken, pork, and salmon. The patient's father died at age 40 due to colon cancer, and his mother died of breast cancer at the age of 52. The patient lives alone and drinks socially. The patient has unprotected sex with multiple male partners. His temperature is 98.3°F (36.8°C), blood pressure is 107/58 mmHg, pulse is 127/min, respirations are 12/min, and oxygen saturation is 99% on room air. Laboratory values are ordered as seen below. Hemoglobin: 9.2 g/dL Hematocrit: 29% Leukocyte count: 9,500/mm^3 with normal differential Platelet count: 87,000/mm^3 Lactate dehydrogenase: 327 IU/L Haptoglobin: 5 mg/dL Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 5.9 mEq/L HCO3-: 19 mEq/L BUN: 39 mg/dL Glucose: 99 mg/dL Creatinine: 1.1 mg/dL Ca2+: 10.2 mg/dL Which of the following is the most likely cause of this patient's presentation?
A 39-year-old man comes to the emergency department because of a 2-day history of fever, chills, dyspnea, and a non-bloody productive cough. He was diagnosed with HIV infection 4 years ago and has been on highly active antiretroviral therapy since then. His temperature is 38.8°C (101.8°F). Examination shows crackles over the left lower lung base. His CD4+ T-lymphocyte count is 520/mm3 (N ≥ 500). An x-ray of the chest shows an infiltrate in the left lower lobe. Sputum cultures grow colonies with a narrow zone of green hemolysis without clearing on blood agar. The most likely causal pathogen of this patient's condition produces which of the following virulence factors?
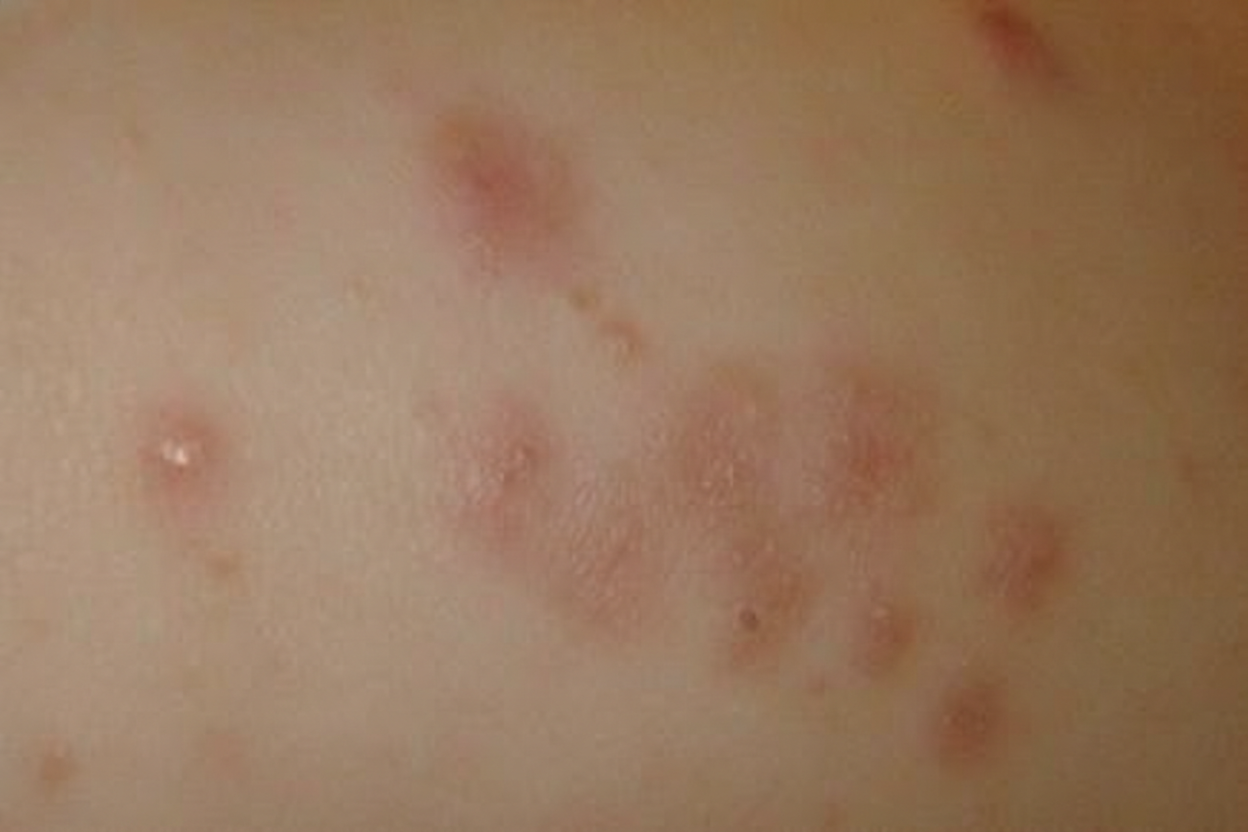
A 36-year-old man comes to the physician because of a 2-day history of malaise and a painful, pruritic rash on his lower back and thighs. His temperature is 37.8°C (100°F). Physical examination shows the findings in the photograph. Skin scrapings from the thigh grow neutral colonies on MacConkey agar. The colony-producing bacteria are oxidase-positive. Which of the following is the greatest risk factor for the patient's condition?
A 49-year-old male complains of abdominal discomfort that worsens following meals. A gastric biopsy reveals a 2 cm gastric ulcer, and immunohistochemical staining demonstrates the presence of a rod-shaped bacterium in the gastric mucosa. Which of the following is used by the infiltrating pathogen to neutralize gastric acidity?
A 35-year-old female presents to the emergency room complaining of diarrhea and dehydration. She has been experiencing severe watery diarrhea for the past 3 days. She reports that she has been unable to leave the bathroom for more than a few minutes at a time. The diarrhea is profuse and watery without visible blood or mucus. She recently returned from a volunteer trip to Yemen where she worked at an orphanage. Her past medical history is notable for psoriasis for which she takes sulfasalazine. The patient drinks socially and does not smoke. Her temperature is 99°F (37.2°C), blood pressure is 100/55 mmHg, pulse is 130/min, and respirations are 20/min. Mucous membranes are dry. Her eyes appear sunken. Capillary refill is 4 seconds. The patient is started on intravenous fluid resuscitation. Which of the following processes is capable of transmitting the genetic material for the toxin responsible for this patient's condition?
A 72-year-old woman comes to the physician because of a 3-day history of redness and swelling of her right leg and fever. She says the leg is very painful and the redness over it has become larger. She appears ill. Her temperature is 39.3°C (102.7°F), pulse is 103/min, and blood pressure is 138/90 mm Hg. Cardiopulmonary examination shows no abnormalities. Examination shows an area of diffuse erythema and swelling over her anterior right lower leg; it is warm and tender to touch. Squeezing of the calf does not elicit tenderness. There is swelling of the right inguinal lymph nodes. Pedal pulses are palpable bilaterally. Which of the following is the strongest predisposing factor for this patient's condition?
A 20-year-old woman presents to student health for a 7-day history of sinus congestion. She has also had fever, sore throat, and infectious gastroenteritis. Upon further questioning, she has had similar problems 2 or 3 times a year for as long as she can remember. These have included sinus infections, ear infections, and lung infections. At the clinic, her temperature is 38.6°C (101.4°F), heart rate is 70/min, blood pressure is 126/78 mm Hg, respiratory rate is 18/min, and oxygen saturation is 98% on room air. Physical examination is notable for mucopurulent discharge from both nares and tenderness to palpation over her bilateral maxillae. Sputum gram stain shows gram-positive diplococci. Which of the following best describes the levels of immunoglobulins that would most likely be found upon testing this patient's serum?
A 6-month-old girl presents with recurring skin infections. Past medical history is significant for 3 episodes of acute otitis media since birth. The patient was born at 39 weeks via an uncomplicated, spontaneous transvaginal delivery, but there was delayed umbilical cord separation. She has met all developmental milestones. On physical examination, the skin around her mouth is inflamed and red. Which of the following is most likely responsible for this child’s clinical presentation?
A 46-year-old obese man comes to the emergency room because of paresthesias in his feet and a hypopigmented skin lesion on his knee that he first noticed 6 weeks ago. He has also had fever, fatigue, and malaise for the last week. He has a history of chronic autoimmune thyroiditis for which he takes levothyroxine. He immigrated from Indonesia 3 years ago to join his family in the United States. His temperature is 38.7°C (101.7°F) and blood pressure is 122/84 mm Hg. Physical exam shows a well-defined hypopigmented skin lesion approximately 3 cm in diameter over the anterior aspect of the right knee. The area has no hair growth and remains dry although he is diaphoretic. There is diminished sensation to light touch and pinprick in the skin lesion when compared to surrounding skin. There is reduced light touch sensation in the big toes bilaterally. After obtaining a skin biopsy of the lesion to confirm the diagnosis, which of the following is the most appropriate initial pharmacotherapy?
A 41-year-old woman presents to the emergency room with a fever. She has had intermittent fevers accompanied by malaise, weakness, and mild shortness of breath for the past 2 weeks. Her past medical history is notable for recurrent bloody diarrhea for over 3 years. She underwent a flexible sigmoidoscopy several months ago which demonstrated contiguously granular and hyperemic rectal mucosa. She has a distant history of intravenous drug use but has been sober for the past 15 years. Her temperature is 100.8°F (38.2°C), blood pressure is 126/76 mmHg, pulse is 112/min, and respirations are 17/min. On exam, she appears lethargic but is able to answer questions appropriately. A new systolic II/VI murmur is heard on cardiac auscultation. Subungual hemorrhages are noted. Multiple blood cultures are drawn and results are pending. Which of the following pathogens is most strongly associated with this patient's condition?
Practice by Chapter
Bacterial cell structure and physiology
Practice Questions
Bacterial genetics
Practice Questions
Bacterial metabolism
Practice Questions
Bacterial virulence factors
Practice Questions
Exotoxins and endotoxins
Practice Questions
Bacterial culture methods
Practice Questions
Antimicrobial susceptibility testing
Practice Questions
Bacterial identification methods
Practice Questions
Bacterial taxonomy and classification
Practice Questions
Zoonotic bacterial infections
Practice Questions
Foodborne bacterial pathogens
Practice Questions
Waterborne bacterial pathogens
Practice Questions
Emerging bacterial pathogens
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
