Hemorrhagic stroke management — MCQs

A 67-year-old man presents to the emergency department for a headache. The patient states his symptoms started thirty minutes ago. He states he experienced a sudden and severe headache while painting his house, causing him to fall off the ladder and hit his head. He has also experienced two episodes of vomiting and difficulty walking since the fall. The patient has a past medical history of hypertension, obesity, and atrial fibrillation. His current medications include lisinopril, rivaroxaban, atorvastatin, and metformin. His temperature is 99.5°F (37.5°C), blood pressure is 150/105 mmHg, pulse is 90/min, respirations are 15/min, and oxygen saturation is 98% on room air. On physical exam, the patient localizes his headache to the back of his head. Cardiac exam reveals a normal rate and rhythm. Pulmonary exam reveals minor bibasilar crackles. Neurological exam is notable for minor weakness of the muscles of facial expression. Examination of cranial nerve three reveals a notable nystagmus. Heel to shin exam is abnormal bilaterally. The patient's gait is notably ataxic. A non-contrast CT scan of the head is currently pending. Which of the following is the most likely diagnosis?
A 48-year-old man presents to the ER with a sudden-onset, severe headache. He is vomiting and appears confused. His wife, who accompanied him, says that he has not had any trauma, and that the patient has no relevant family history. He undergoes a non-contrast head CT that shows blood between the arachnoid and pia mater. What is the most likely complication from this condition?
A 72-year-old woman is brought to the emergency department by her son after he noticed that she was slurring her speech. He also noticed that she appeared to have difficulty using her fork about halfway through dinner when the speech problems started. He brought her to the emergency department immediately and he estimates that only 1 hour has passed since the beginning of the symptoms. An immediate exam is conducted. A medication is administered to ameliorate the effects of this patient's condition that would not be available for use if the patient had presented significantly later. An hour later the patient's condition becomes significantly worse and new deficits are found. Which of the following agents should be used at this point?
A 69-year-old male presents to the emergency department for slurred speech and an inability to use his right arm which occurred while he was eating dinner. The patient arrived at the emergency department within one hour. A CT scan was performed of the head and did not reveal any signs of hemorrhage. The patient is given thrombolytics and is then managed on the neurology floor. Three days later, the patient is recovering and is stable. He seems depressed but is doing well with his symptoms gradually improving as compared to his initial presentation. The patient complains of neck pain that has worsened slowly over the past few days for which he is being given ibuprofen. Laboratory values are ordered and return as indicated below: Serum: Na+: 130 mEq/L K+: 3.7 mEq/L Cl-: 100 mEq/L HCO3-: 24 mEq/L Urea nitrogen: 7 mg/dL Glucose: 70 mg/dL Creatinine: 0.9 mg/dL Ca2+: 9.7 mg/dL Urine: Appearance: dark Glucose: negative WBC: 0/hpf Bacterial: none Na+: 320 mEq/L/24 hours His temperature is 99.5°F (37.5°C), pulse is 95/min, blood pressure is 129/70 mmHg, respirations are 10/min, and oxygen saturation is 98% on room air. Which of the following is the best next step in management?
A new treatment for hemorrhagic stroke, which is a life-threatening clinical condition that occurs when a diseased blood vessel in the brain ruptures or leaks, was evaluated as soon as it hit the market by an international group of neurology specialists. In those treated with the new drug, a good outcome was achieved in 30%, while those treated with the current standard of care had a good outcome in just 10% of cases. The clinicians involved in this cohort study concluded that the newer drug is more effective and prompted for urgent changes in the guidelines addressing hemorrhagic stroke incidents. According to the aforementioned percentages, how many patients must be treated with the new drug to see 1 additional good outcome?
A 74-year-old man presents to the emergency department by paramedics for slurred speech and weakness in the left arm and leg for 1 hour. The patient was playing with his grandson when the symptoms started and his wife immediately called an ambulance. There is no history of head trauma or recent surgery. The patient takes captopril for hypertension. The vital signs include: pulse 110/min, respiratory rate 22/min, and blood pressure 200/105 mm Hg. The physical examination shows that the patient is alert and conscious, but speech is impaired. Muscle strength is 0/5 in the left arm and leg and 5/5 in the right arm and leg. A non-contrast CT of the head shows no evidence of intracranial bleeding. The lab results are as follows: Serum glucose 90 mg/dL Sodium 140 mEq/L Potassium 4.1 mEq/L Chloride 100 mEq/L Serum creatinine 1.3 mg/dL Blood urea nitrogen 20 mg/dL Cholesterol, total 240 mg/dL HDL-cholesterol 38 mg/dL LDL-cholesterol 100 mg/dL Triglycerides 190 mg/dL Hemoglobin (Hb%) 15.3 g/dL Mean corpuscular volume (MCV) 83 fL Reticulocyte count 0.8% Erythrocyte count 5.3 million/mm3 Platelet count 130,000/mm3 Partial thromboplastin time (aPTT) 30 sec Prothrombin time (PT) 12 sec Although he is within the time frame for the standard therapy of the most likely condition, the treatment cannot be started because of which of the following contraindications?
A 23-year-old man presents with a blunt force injury to the head from a baseball bat. He is currently unconscious, although his friends say he was awake and speaking with them en route to the hospital. He has no significant past medical history and takes no current medications. The vital signs include: temperature 37.0°C (98.6°F), blood pressure 165/85 mm Hg, pulse 50/min, and respiratory rate 19/min. On physical examination, there is a blunt force injury to the left temporoparietal region approximately 10.1–12.7 cm (4–5 in) in diameter. There is anisocoria of the left pupil, which is unresponsive to light. The patient is intubated and fluid resuscitation is initiated. A noncontrast computed tomography (CT) scan of the head is acquired and shown in the exhibit (see image). Which of the following is the most appropriate medical treatment for this patient?
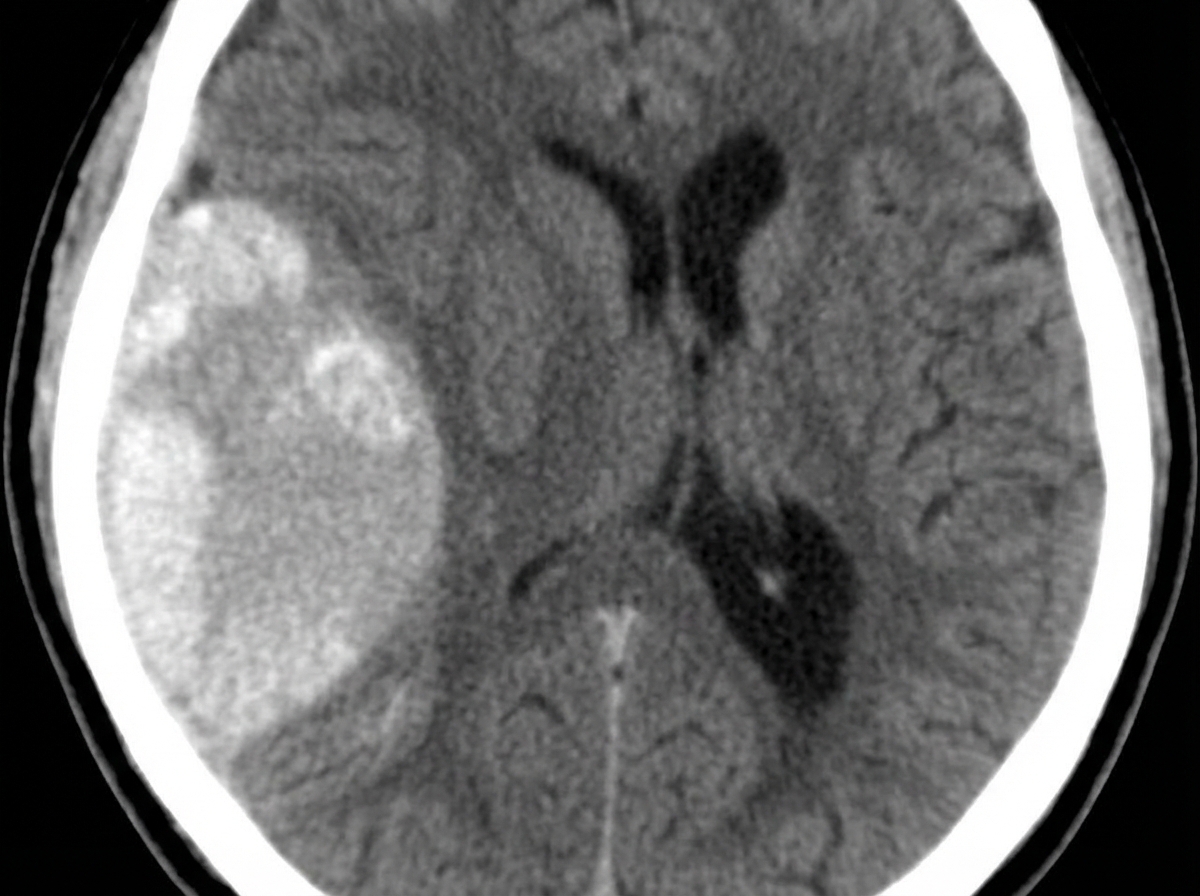
A 44-year-old man comes to the emergency department because of a severe headache and blurry vision for the past 3 hours. He has hypertension treated with hydrochlorothiazide. He has missed taking his medication for the past week as he was traveling. He is only oriented to time and person. His temperature is 37.1°C (98.8°F), pulse is 92/min and regular, and blood pressure is 245/115 mm Hg. Cardiopulmonary examination shows no abnormalities. Fundoscopy shows bilateral retinal hemorrhages and exudates. Neurologic examination shows no focal findings. A complete blood count and serum concentrations of electrolytes, glucose, and creatinine are within the reference range. A CT scan of the brain shows no abnormalities. Which of the following is the most appropriate pharmacotherapy?
A 48-year-old woman is brought to the emergency department because of a 1-hour history of sudden-onset headache associated with nausea and vomiting. The patient reports she was sitting at her desk when the headache began. The headache is global and radiates to her neck. She has hypertension. She has smoked one pack of cigarettes daily for the last 10 years. She drinks alcohol occasionally. Her father had a stroke at the age 58 years. Current medications include hydrochlorothiazide. She is in severe distress. She is alert and oriented to person, place, and time. Her temperature is 38.2°C (100.8°F), pulse is 89/min, respirations are 19/min, and blood pressure is 150/90 mm Hg. Cardiopulmonary examination shows no abnormalities. Cranial nerves II–XII are intact. She has no focal motor or sensory deficits. She flexes her hips and knees when her neck is flexed while lying in a supine position. A CT scan of the head is shown. Which of the following is the most appropriate intervention?
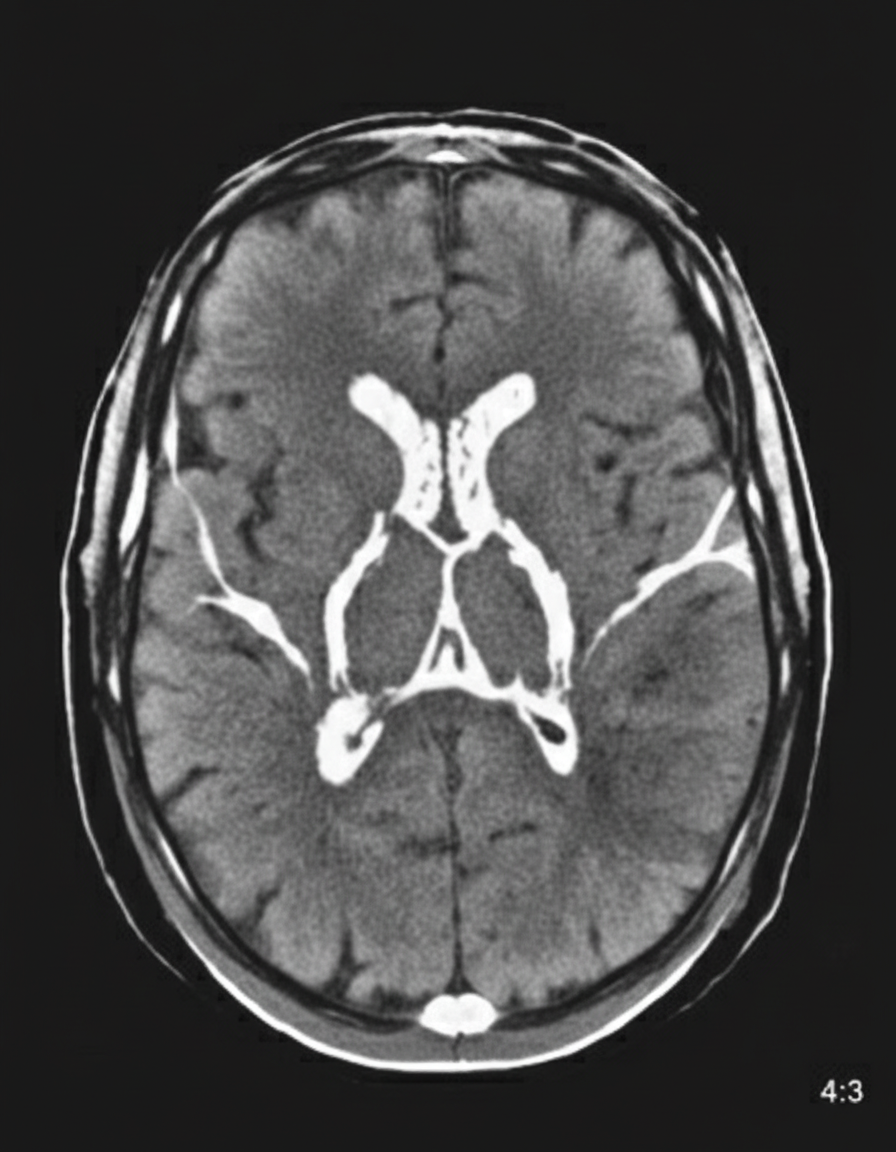
A 65-year-old man presents to the emergency department for sudden weakness. He was doing mechanical work on his car where he acutely developed right-leg weakness and fell to the ground. He is accompanied by his wife, who said that this has never happened before. He was last seen neurologically normal approximately 2 hours prior to presentation. His past medical history is significant for hypertension and type II diabetes. His temperature is 98.8°F (37.1°C), blood pressure is 177/108 mmHg, pulse is 90/min, respirations are 15/min, and oxygen saturation is 99% on room air. Neurological exam reveals that he is having trouble speaking and has profound weakness of his right upper and lower extremity. Which of the following is the best next step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
