Fluid resuscitation strategies — MCQs

A 61-year-old female with congestive heart failure and type 2 diabetes is brought to the emergency room by her husband because of an altered mental status. He states he normally helps her be compliant with her medications, but he had been away for several days. On physical exam, her temperature is 37.2 C, BP 85/55, and HR 130. Serum glucose is 500 mg/dL. Which of the following is the first step in the management of this patient?
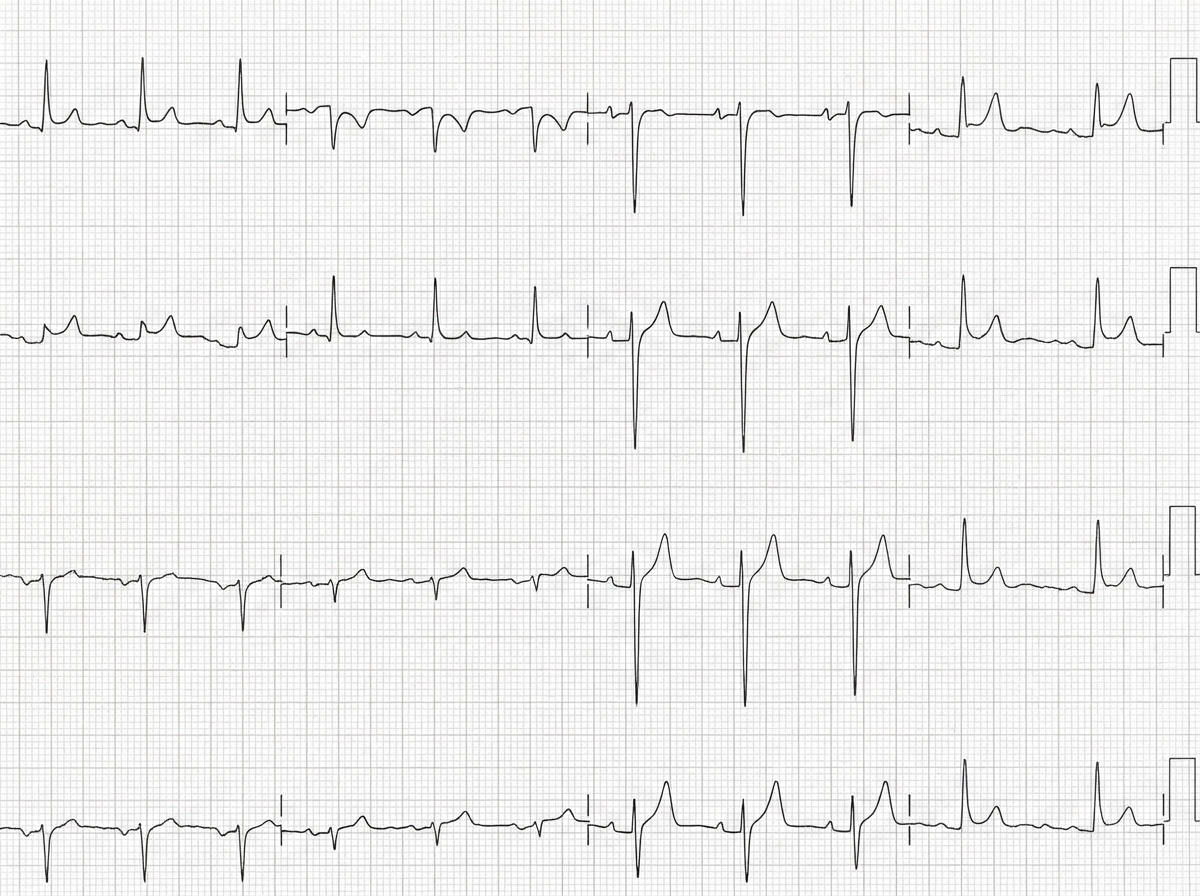
A 50-year-old man with a history of stage 4 kidney disease was admitted to the hospital for an elective hemicolectomy. His past medical history is significant for severe diverticulitis. After the procedure he becomes septic and was placed on broad spectrum antibiotics. On morning rounds, he appear weak and complains of fatigue and nausea. His words are soft and he has difficulty answering questions. His temperature is 38.9°C (102.1°F), heart rate is 110/min, respiratory rate is 15/min, blood pressure 90/65 mm Hg, and saturation is 89% on room air. On physical exam, his mental status appears altered. He has a bruise on his left arm that spontaneously appeared overnight. His cardiac exam is positive for a weak friction rub. Blood specimens are collected and sent for evaluation. An ECG is performed (see image). What therapy will this patient most likely receive next?
A 37-year-old man is brought to the emergency department by ambulance after a motor vehicle accident. He suffered multiple deep lacerations and experienced significant blood loss during transport. In the emergency department, his temperature is 98.6°F (37°C), blood pressure is 102/68 mmHg, pulse is 112/min, and respirations are 22/min. His lacerations are sutured and he is given 2 liters of saline by large bore intravenous lines. Which of the following changes will occur in this patient's cardiac physiology due to this intervention?
A 53-year-old diabetic man with cellulitis of the right lower limb presents to the emergency department because of symptoms of fever and chills. His pulse is 122/min, the blood pressure is 76/50 mm Hg, the respirations are 26/min, and the temperature is 40.0°C (104.0°F). His urine output is < 0.5mL/kg/h. He has warm peripheral extremities. The hemodynamic status of the patient is not improving in spite of the initiation of adequate fluid resuscitation. He is admitted to the hospital. Which of the following is the most likely laboratory profile?
Which of the following physiologic changes decreases pulmonary vascular resistance (PVR)?
A 27-year-old man is brought to the emergency department 30 minutes after being shot in the abdomen during a violent altercation. His temperature is 36.5°C (97.7°F), pulse is 118/min and regular, and blood pressure is 88/65 mm Hg. Examination shows cool extremities. Abdominal examination shows a 2.5-cm entrance wound in the left upper quadrant at the midclavicular line, below the left costal margin. Focused ultrasound shows free fluid in the left upper quadrant. Which of the following sets of hemodynamic changes is most likely in this patient? Cardiac output (CO) | Pulmonary capillary wedge pressure (PCWP) | Systemic vascular resistance (SVR) | Central venous pressure (CVP)
A 57-year-old man is admitted to the burn unit after he was brought to the emergency room following an accidental fire in his house. His past medical history is unknown due to his current clinical condition. Currently, his blood pressure is 75/40 mmHg, pulse rate is 140/min, and respiratory rate is 17/min. The patient is subsequently intubated and started on aggressive fluid resuscitation. A Swan-Ganz catheter is inserted to clarify his volume status. Which of the following hemodynamic parameters would you expect to see in this patient?
A 17-year-old previously healthy, athletic male suddenly falls unconscious while playing soccer. His athletic trainer comes to his aid and notes that he is pulseless. He begins performing CPR on the patient until the ambulance arrives but the teenager is pronounced dead when the paramedics arrived. Upon investigation of his primary care physician's office notes, it was found that the child had a recognized murmur that was ruled to be "benign." Which of the following conditions would have increased the intensity of the murmur?
A 35-year-old woman is brought to the emergency department 45 minutes after being rescued from a house fire. On arrival, she appears confused and has shortness of breath. The patient is 165 cm (5 ft 5 in) tall and weighs 55 kg (121 lb); BMI is 20 kg/m2. Her pulse is 125/min, respirations are 29/min, and blood pressure is 105/65 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 97%. Examination shows second and third-degree burns over the anterior surfaces of the chest and abdomen, and the anterior surface of the upper extremities. There is black debris in the mouth and nose. There are coarse breath sounds over the lung bases. Cardiac examination shows no murmurs, rubs, or gallop. Femoral and pedal pulses are palpable bilaterally. Which of the following is the most appropriate fluid regimen for this patient according to the Parkland formula?
A 7-year-old boy is brought to the emergency room because of severe, acute diarrhea. He is drowsy with a dull, lethargic appearance. He has sunken eyes, poor skin turgor, and dry oral mucous membranes and tongue. He has a rapid, thready pulse with a systolic blood pressure of 60 mm Hg and his respirations are 33/min. His capillary refill time is 6 sec. He has had no urine output for the past 24 hours. Which of the following is the most appropriate next step in treatment?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
