Empiric antimicrobial therapy — MCQs

An 18-year-old female college student is brought to the emergency department by ambulance for a headache and altered mental status. The patient lives with her boyfriend who is with her currently. He states she had not been feeling well for the past day and has vomited several times in the past 12 hours. Lumbar puncture is performed in the emergency room and demonstrates an increased cell count with a neutrophil predominance and gram-negative diplococci on Gram stain. The patient is started on vancomycin and ceftriaxone. Which of the following is the best next step in management?
A 22-year-old female is brought to the emergency department by her roommate with a one day history of fever and malaise. She did not feel well after class the previous night and has been in her room since then. She has not been eating or drinking due to severe nausea. Her roommate checked on her one hour ago and was alarmed to find a fever of 102°F (38.9°C). On physical exam temperature is 103°F (40°C), blood pressure is 110/66 mmHg, pulse is 110/min, respirations are 23/min, and pulse oximetry is 98% on room air. She refuses to move her neck and has a rash on her trunk. You perform a lumbar puncture and the CSF analysis is shown below. Appearance: Cloudy Opening pressure: 180 mm H2O WBC count: 150 cells/µL (93% PMN) Glucose level: < 40 mg/dL Protein level: 50 mg/dL Gram stain: gram-negative diplococci Based on this patient's clinical presentation, which of the following should most likely be administered?
A 59-year-old woman comes to the emergency department because of a 2-day history of worsening fever, chills, malaise, productive cough, and difficulty breathing. Three days ago, she returned from a trip to South Africa. She has type 2 diabetes mellitus, hypertension, and varicose veins. Her current medications include metformin, lisinopril, and atorvastatin. Her temperature is 39.4°C (102.9°F), pulse is 102/minute, blood pressure is 94/68 mm Hg, and respirations are 31/minute. Pulse oximetry on 2 L of oxygen via nasal cannula shows an oxygen saturation of 91%. Examination reveals decreased breath sounds and dull percussion over the left lung base. The skin is very warm and well-perfused. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 11.6 g/dL Leukocyte count 15,400/mm3 platelet count 282,000/mm3 Serum Na+ 144 mEq/L Cl- 104 mEq/L K+ 4.9 mEq/L Creatinine 1.5 mg/dL Blood and urine for cultures are obtained. Intravenous fluid resuscitation is begun. Which of the following is the next best step in management?
Five days after being admitted to the hospital for a scald wound, a 2-year-old boy is found to have a temperature of 40.2°C (104.4°F). He does not have difficulty breathing, cough, or painful urination. He initially presented one hour after spilling a pot of boiling water on his torso while his mother was cooking dinner. He was admitted for fluid resuscitation, nutritional support, pain management, and wound care, and he was progressing well until today. He has no other medical conditions. Other than analgesia during this hospital stay, he does not take any medications. He appears uncomfortable but not in acute distress. His pulse is 150/min, respirations are 41/min, and blood pressure is 90/50 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 99%. Examination shows uneven, asymmetrical scalding covering his anterior torso in arrow-like patterns with surrounding erythema and purulent discharge. The remainder of the examination shows no abnormalities. His hemoglobin is 13.4 g/dL, platelet count is 200,000/mm3, and leukocyte count is 13,900/mm3. Which of the following is the most appropriate initial pharmacological treatment for this patient?
Three days after admission to the hospital following a motor vehicle accident, a 45-year-old woman develops a fever. A central venous catheter was placed on the day of admission for treatment of severe hypotension. Her temperature is 39.2°C (102.5°F). Examination shows erythema surrounding the catheter insertion site at the right internal jugular vein. Blood cultures show gram-positive, catalase-positive cocci that have a high minimum inhibitory concentration when exposed to novobiocin. Which of the following is the most appropriate pharmacotherapy?
A 62-year-old man is brought to the emergency department from a senior-care facility after he was found with a decreased level of consciousness and fever. His personal history is relevant for colorectal cancer that was managed with surgical excision of the tumor. Upon admission, he is found to have a blood pressure of 130/80 mm Hg, a pulse of 102/min, a respiratory rate of 20/min, and a body temperature 38.8°C (101.8°F). There is no rash on physical examination; he is found to have neck rigidity, confusion, and photophobia. There are no focal neurological deficits. A head CT is normal without mass or hydrocephalus. A lumbar puncture was performed and cerebrospinal fluid (CSF) is sent to analysis while ceftriaxone and vancomycin are started. Which of the following additional antimicrobials should be added in the management of this patient?
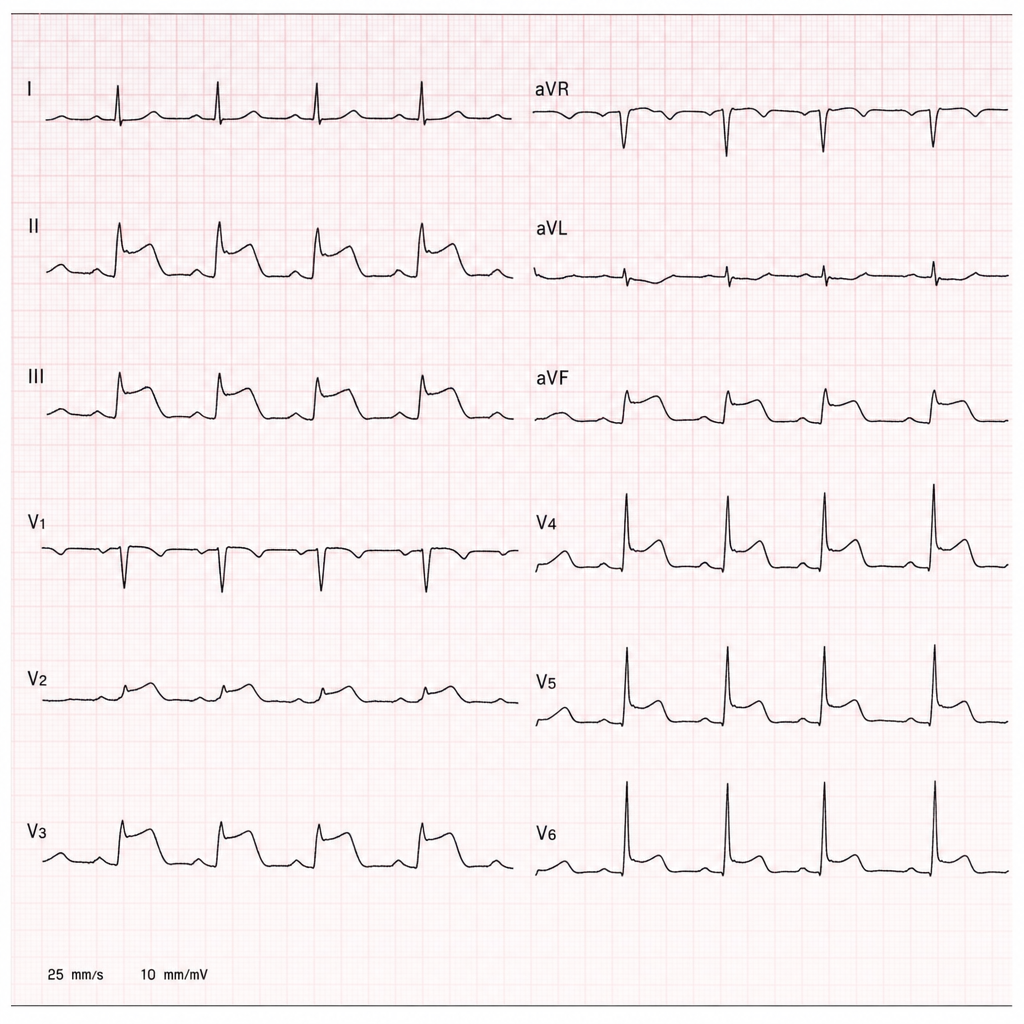
A 58-year-old man with hypertension and hyperlipidemia is brought to the emergency department by ambulance after collapsing at home. His wife states he complained of sudden severe chest pain radiating to the left arm 40 minutes ago, then became diaphoretic and lost consciousness briefly. On arrival, BP is 88/60 mmHg, HR 112 bpm, RR 22/min, SpO2 94% on room air. The ECG shown demonstrates 4 mm ST-segment elevation in leads II, III, and aVF with reciprocal changes in I and aVL. IV access is established, aspirin 325 mg has been given, and oxygen is being administered. The nearest percutaneous coronary intervention-capable facility is 25 minutes away. Which of the following is the most appropriate next step?
A 38-year-old previously healthy woman develops septic shock from necrotizing fasciitis of the lower extremity. Despite three debridements, broad-spectrum antibiotics (vancomycin, meropenem, clindamycin), IVIG, and aggressive critical care support, she develops refractory shock requiring norepinephrine 1.2 mcg/kg/min, vasopressin 0.04 units/min, and epinephrine 0.1 mcg/kg/min. Lactate is 15 mmol/L. Surgical team recommends hemipelvectomy as last option for source control. Family is devastated. ICU team notes SOFA score of 18. Synthesize an approach to management and decision-making.
A 52-year-old woman with septic shock from intra-abdominal infection undergoes emergency exploratory laparotomy for perforated diverticulitis with fecal peritonitis. Surgery reveals extensive contamination requiring damage control approach. Postoperatively, she requires norepinephrine 0.8 mcg/kg/min plus vasopressin 0.04 units/min, has lactate of 8.5 mmol/L, temperature 35.2°C, INR 2.8, pH 7.18, and base deficit -12. Planned return to OR is in 48 hours. Evaluate the priority interventions to optimize outcome.
A 70-year-old man with recently diagnosed small cell lung cancer presents with septic shock from pneumonia. After initial resuscitation, he requires norepinephrine 0.6 mcg/kg/min and has a lactate of 7.8 mmol/L. His SOFA score is 14. The family requests 'everything be done,' but the patient had previously told his oncologist he would not want prolonged intensive care if his cancer prognosis was poor. Staging shows extensive-stage disease. The ICU team debates goals of care. What represents the most ethically appropriate approach to decision-making?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
