Beta-blockers, ACE-I/ARBs, statins — MCQs

A 55-year-old man comes to the physician because of a 4-month history of episodic, pressure-like chest pain. The chest pain occurs when he is walking up stairs and improves with rest. He has hypertension and type 2 diabetes mellitus. His father died from a myocardial infarction at the age of 50 years. Current medications include hydrochlorothiazide and metformin. His pulse is 85/min, respirations are 12/min, and blood pressure is 140/90 mm Hg. Cardiac examination shows normal heart sounds without any murmurs, rubs, or gallops. An ECG shows high amplitude of the S wave in lead V3. An exercise stress test is performed but stopped after 4 minutes because the patient experiences chest pain. An ECG obtained during the stress test shows sinus tachycardia and ST-segment depressions in leads V1–V4. Which of the following is the most appropriate long-term pharmacotherapy to reduce the frequency of symptoms in this patient?
A 62-year-old man comes to the physician for an annual health maintenance examination. He has a history of stable angina, gout, and hypertension. His medications include lisinopril and aspirin. He has smoked a pack of cigarettes daily for 20 years. He drinks 5–6 beers on the weekends. His blood pressure is 150/85 mm Hg. Laboratory studies show a total cholesterol of 276 mg/dL with an elevated low-density lipoprotein (LDL) concentration and low high-density lipoprotein (HDL) concentration. Administration of which of the following agents is the most appropriate next step in management?
A 55-year-old man comes to the physician because of intermittent palpitations that occur when he is stressed, exercising, or when he drinks alcohol. Physical examination shows an irregularly irregular pulse. An ECG shows irregular QRS complexes without any discrete P waves. Pharmacotherapy with carvedilol is initiated for his condition. Compared to treatment with propranolol, which of the following adverse effects is most likely?
A 72-year-old man presents to the outpatient clinic today. He has New York Heart Association class III heart failure. His current medications include captopril 20 mg, furosemide 40 mg, potassium chloride 10 mg twice daily, rosuvastatin 20 mg, and aspirin 81 mg. He reports that he generally feels well and has not had any recent worsening of his symptoms. His blood pressure is 132/85 mm Hg and heart rate is 84/min. Physical examination is unremarkable except for trace pitting edema of the bilateral lower extremities. What other medication should be added to his heart failure regimen?
A 71-year-old African American man diagnosed with high blood pressure presents to the outpatient clinic. In the clinic, his blood pressure is 161/88 mm Hg with a pulse of 88/min. He has had similar blood pressure measurements in the past, and you initiate captopril. He presents back shortly after initiation with extremely swollen lips, tongue, and face. After captopril is discontinued, what is the most appropriate step for the management of his high blood pressure?
A 73-year-old man presents to the outpatient clinic complaining of chest pain with exertion. He states that resting for a few minutes usually resolves the chest pain. Currently, he takes 81 mg of aspirin daily. He has a blood pressure of 127/85 mm Hg and heart rate of 75/min. Physical examination reveals regular heart sounds and clear lung sounds bilateral. Which medication regimen below should be added?
A 60-year-old patient is at his physician’s office for a routine health maintenance exam. The patient has a past medical history of osteoarthritis in his right knee and GERD that is well-controlled with over the counter medication. On a fasting lipid profile, he is found to have high cholesterol. The patient is started on daily atorvastatin to reduce his risk of cardiovascular disease. What is the major apolipoprotein found on the lipoprotein most directly affected by his statin medication?
A 56-year-old patient developed excruciating chest discomfort in the past 72 hours, relieved by GTN spray. Troponin I is normal, and the ECG shows features of left ventricular hypertrophy (LVH) with T wave flattening. The patient is already on statins, aspirin, and metoprolol 50 mg . What is the next best step in management?
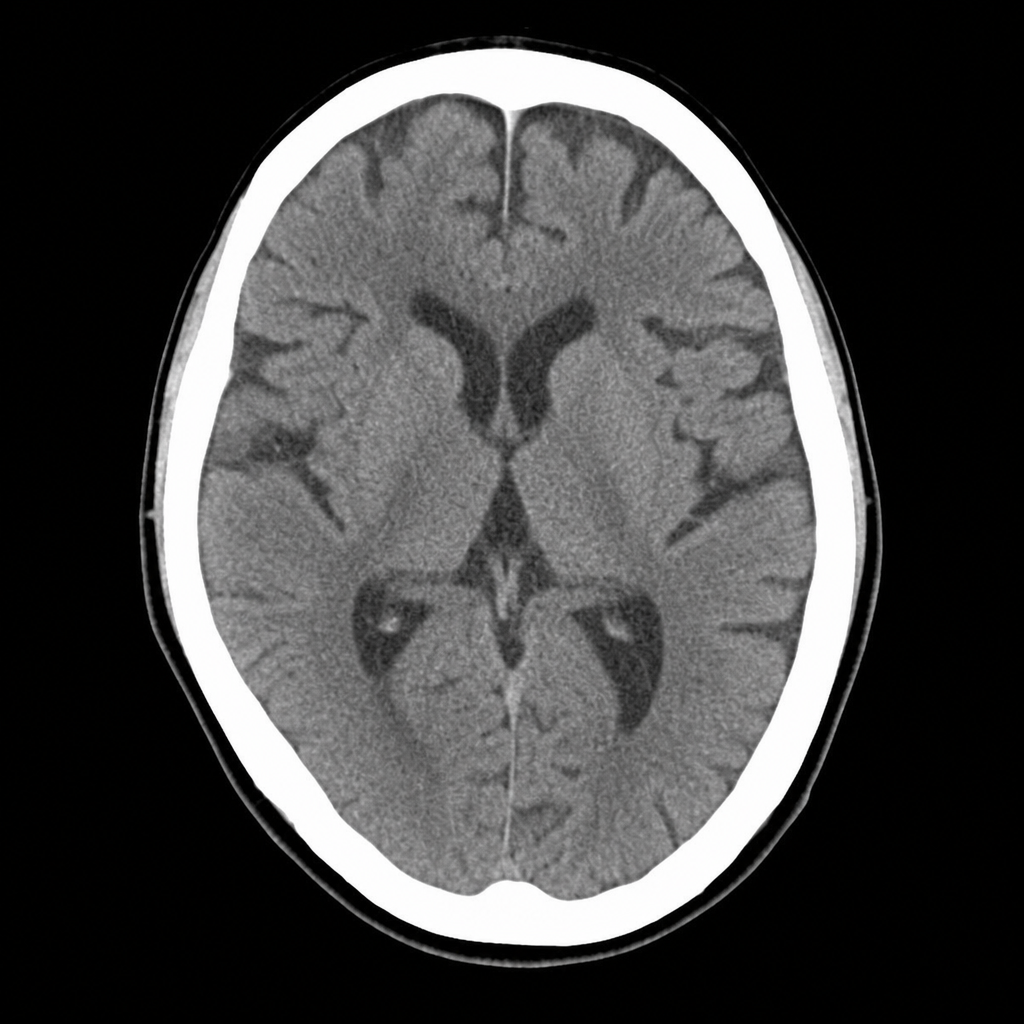
A 67-year-old man with hypertension and type 2 diabetes is brought to the ED by his wife, who noticed he developed sudden right-sided facial droop and slurred speech approximately 2 hours ago. On arrival, blood pressure is 188/104 mmHg, heart rate 82 bpm, oxygen saturation 97% on room air. Neurological examination reveals right facial weakness, dysarthria, and mild right arm drift. NIHSS score is 7. A non-contrast CT head is performed and shown above. No hemorrhage, early infarct signs, or mass lesion is identified. The patient takes metformin and lisinopril; no anticoagulants. Which of the following is the most appropriate immediate next step?
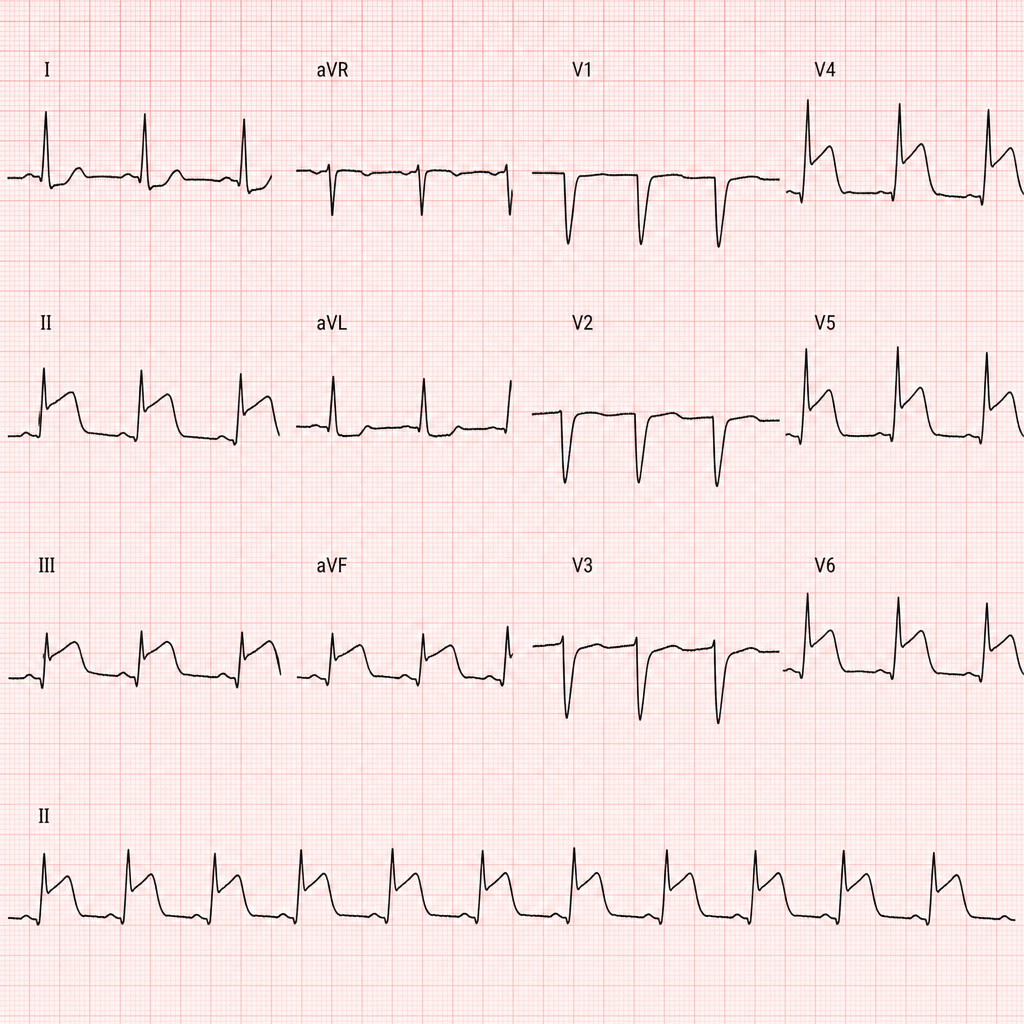
A 67-year-old man with hypertension and hyperlipidemia presents to the emergency department with 45 minutes of crushing substernal chest pain radiating to his left arm. He is diaphoretic and pale. Vital signs: BP 88/60 mmHg, HR 112 bpm, RR 20/min, SpO2 94% on room air. PCI is immediately available. An ECG is obtained and shown above. Two large-bore IVs are placed. Which of the following is the most appropriate immediate next step?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
