Respiratory failure management — MCQs

A 63-year-old man presents to the clinic with fever accompanied by shortness of breath. The symptoms developed a week ago and have been progressively worsening over the last 2 days. He reports his cough is productive of thick, yellow sputum. He was diagnosed with chronic obstructive pulmonary disease 3 years ago and has been on treatment ever since. He quit smoking 10 years ago but occasionally experiences shortness of breath along with chest tightness that improves with the use of an inhaler. However, this time the symptoms seem to be more severe and unrelenting. His temperature is 38.6°C (101.4°F), the respirations are 21/min, the blood pressure is 100/60 mm Hg, and the pulse is 105/min. Auscultation reveals bilateral crackles and expiratory wheezes. His oxygen saturation is 95% on room air. According to this patient’s history, which of the following should be the next step in the management of this patient?
A 21-year-old man presents to his physician because he has been feeling increasingly tired and short of breath at work. He has previously had these symptoms but cannot recall the diagnosis he was given. Chart review reveals the following results: Oxygen tension in inspired air = 150 mmHg Alveolar carbon dioxide tension = 50 mmHg Arterial oxygen tension = 71 mmHg Respiratory exchange ratio = 0.80 Diffusion studies reveal normal diffusion distance. The patient is administered 100% oxygen but the patient's blood oxygen concentration does not improve. Which of the following conditions would best explain this patient's findings?
An 8-year-old girl is brought to the emergency department by her parents with severe difficulty in breathing for an hour. She is struggling to breathe. She was playing outside with her friends, when she suddenly fell to the ground, out of breath. She was diagnosed with asthma one year before and has since been on treatment for it. At present, she is sitting leaning forward with severe retractions of the intercostal muscles. She is unable to lie down. Her parents mentioned that she has already taken several puffs of her inhaler since this episode began but without response. On physical examination, her lungs are hyperresonant to percussion and there is decreased air entry in both of her lungs. Her vital signs show: blood pressure 110/60 mm Hg, pulse 110/min, respirations 22/min, and a peak expiratory flow rate (PEFR) of 50%. She is having difficulty in communicating with the physician. Her blood is sent for evaluation and a chest X-ray is ordered. Her arterial blood gas reports are as follows: PaO2 50 mm Hg pH 7.38 PaCO2 47 mm Hg HCO3 27 mEq/L Which of the following is the most appropriate next step in management?
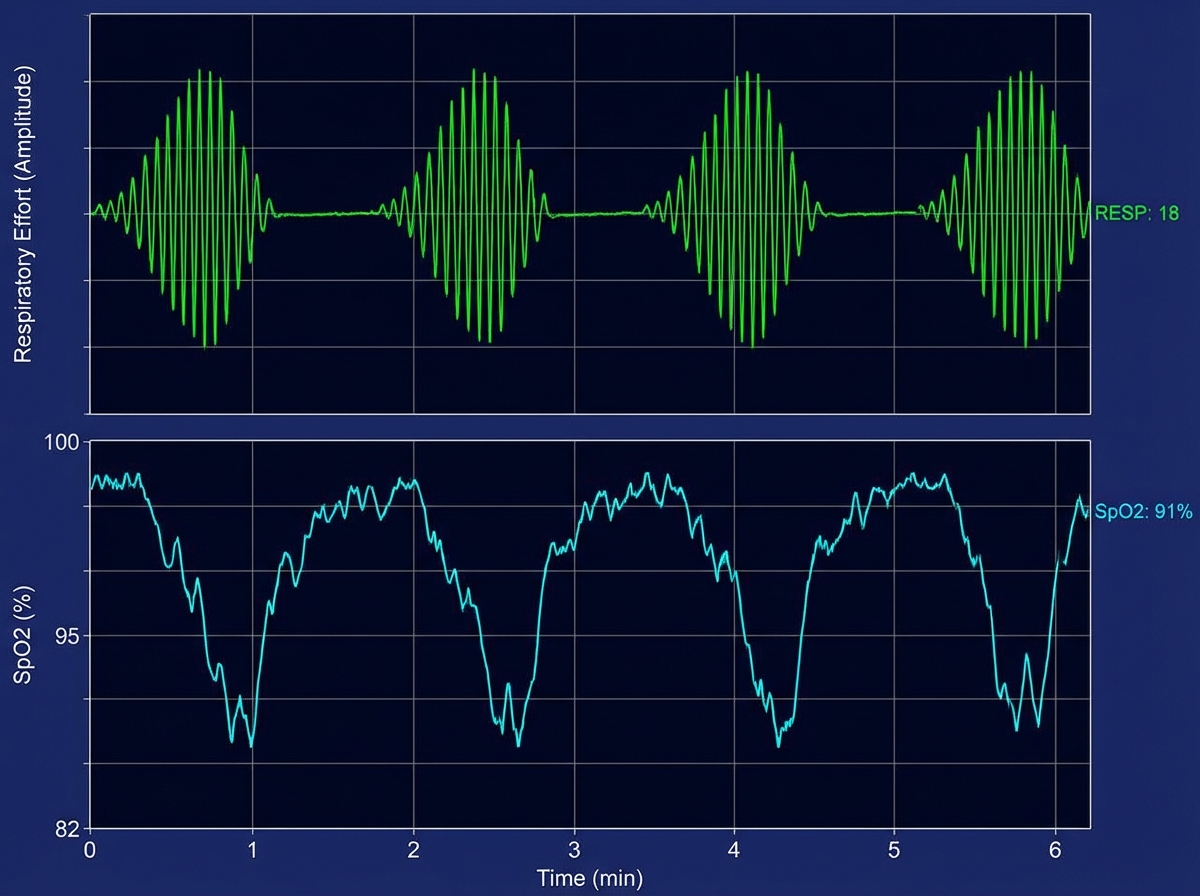
A 66-year-old man is brought to the emergency department because of shortness of breath and confusion. His pulse is 98/min, and blood pressure is 109/73 mm Hg. He is oriented to person but not time or place. A graph of his breathing pattern and oxygen saturation is shown. Which of the following additional findings is most likely present in this patient?
A 62-year-old man is brought to the emergency department because of progressive shortness of breath, mild chest pain on exertion, and a cough for 2 days. One week ago, he had a low-grade fever and nasal congestion. He has hypertension but does not adhere to his medication regimen. He has smoked one pack of cigarettes daily for 30 years and drinks 3–4 beers daily. His temperature is 37.1°C (98.8°F), pulse is 125/min, respirations are 29/min, and blood pressure is 145/86 mm Hg. He is in moderate respiratory distress while sitting. Pulmonary examination shows reduced breath sounds bilaterally. There is scattered wheezing over all lung fields. There is inward displacement of his abdomen during inspiration. Arterial blood gas analysis shows: pH 7.29 PCO2 63 mm Hg PO2 71 mm Hg HCO3- 29 mEq/L O2 saturation 89% Which of the following is the most likely cause of this patient's symptoms?
A 63-year-old man is brought to the emergency department, 30 minutes after being involved in a high-speed motor vehicle collision. He is obtunded on arrival. He is intubated and mechanical ventilation is begun. The ventilator is set at a FiO2 of 60%, tidal volume of 440 mL, and positive end-expiratory pressure of 4 cm H2O. On the third day of intubation, his temperature is 37.3°C (99.1°F), pulse is 91/min, and blood pressure is 103/60 mm Hg. There are decreased breath sounds over the left lung base. Cardiac examination shows no abnormalities. The abdomen is soft and not distended. Arterial blood gas analysis shows: pH 7.49 pCO2 29 mm Hg pO2 73 mm Hg HCO3- 20 mEq/L O2 saturation 89% Monitoring shows a sudden increase in the plateau airway pressure. An x-ray of the chest shows deepening of the costophrenic angle on the left side. Which of the following is the most appropriate next step in management?
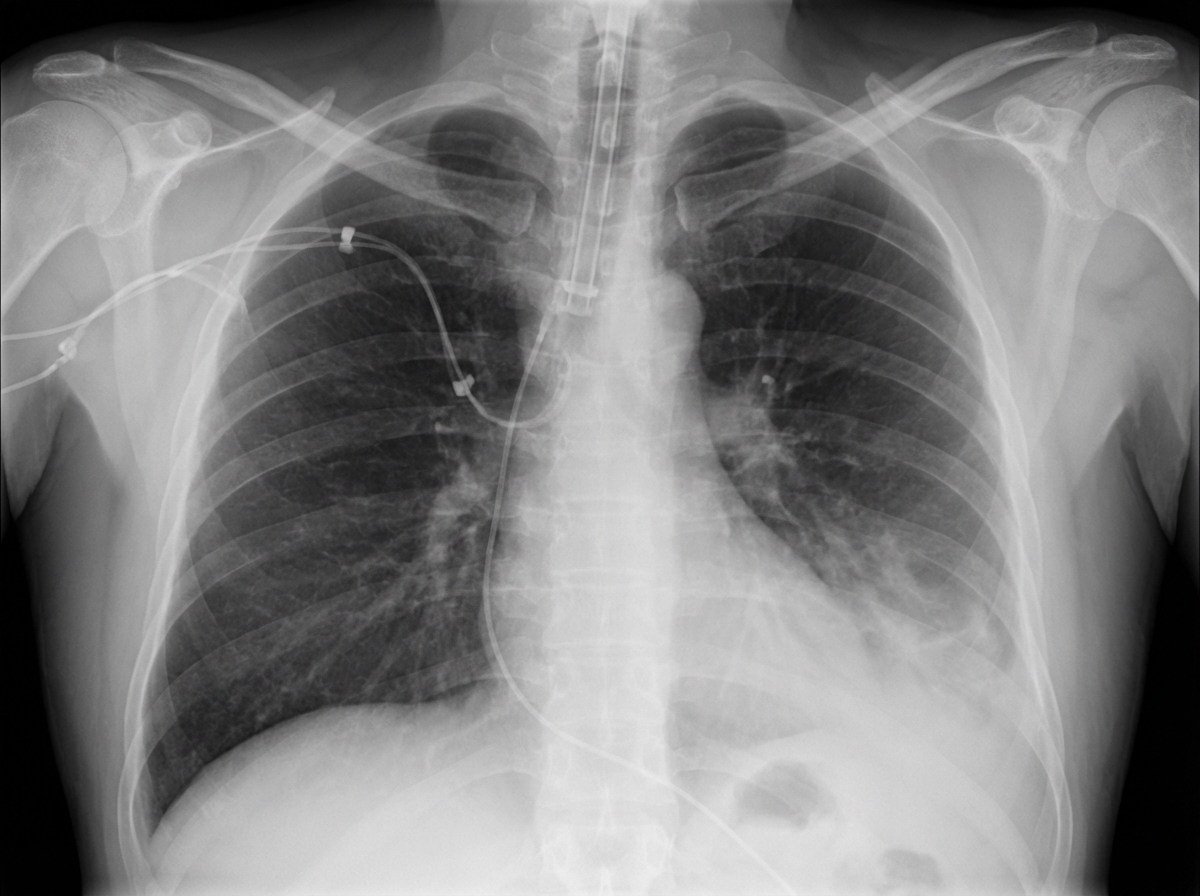
In which of the following pathological states would the oxygen content of the trachea resemble the oxygen content in the affected alveoli?
A 27-year-old man with an unknown past medical history is brought to the emergency department acutely intoxicated. The patient was found passed out in a park covered in vomit and urine. His temperature is 99.0°F (37.2°C), blood pressure is 107/68 mm Hg, pulse is 120/min, respiratory rate is 13/min, and oxygen saturation is 95% on room air. Physical exam is notable for wheezing in all lung fields without any crackles. The patient is started on 2L/min nasal cannula oxygen and IV fluids. His laboratory values are notable for an AST of 200 U/L and an ALT of 100 U/L. An initial chest radiograph is unremarkable. Which of the following is the most likely explanation for this patient's pulmonary symptoms?
For evaluating the functioning of a health center, which is the most important determinant for assessing clinical management?
A 56-year-old woman is brought to the emergency department after falling on her outstretched hand. Her wrist is clearly deformed by fracture and is painful to palpation. Her wrist and finger motion is limited due to pain. After treatment and discharge, her final total cost is $25,000. Her health insurance plan has a $3,000 copayment for emergency medical visits after the annual deductible of $20,000 is met and before 20% co-insurance applies. Previously this year, she had 2 visits to the emergency department for asthma attacks, which cost her $3,500 and $4,500 respectively. She has had no other medical costs during this period. Given that she has no previous balance due, which of the following must she pay out of pocket for her current visit to the emergency department?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
