Inflammatory myopathies — MCQs

A 35-year-old woman presents for evaluation of symmetric proximal muscle weakness. The patient also presents with a blue-purple discoloration of the upper eyelids accompanied by rashes on the knuckles, as shown in the picture below. What is the most likely cause?
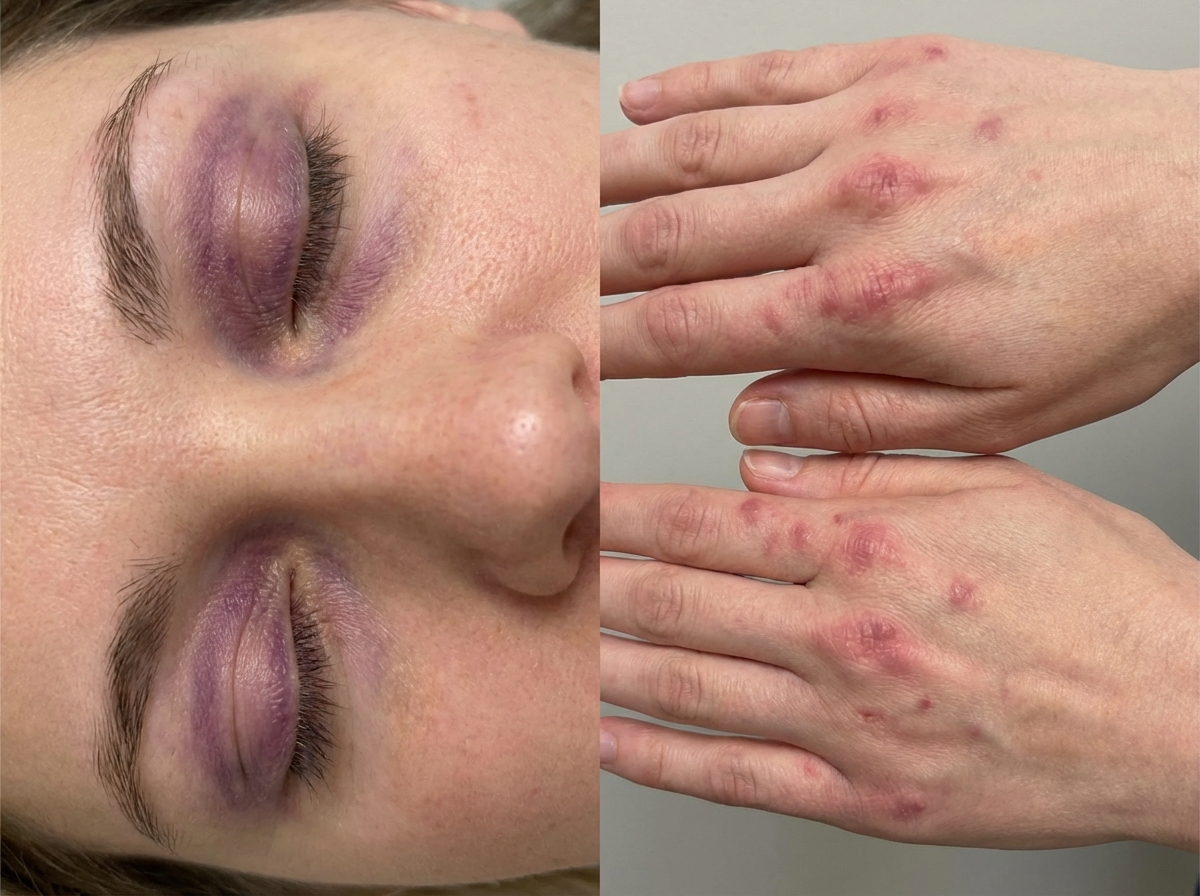
A 47-year-old woman comes to the physician because of body aches for the past 9 months. She also has stiffness of the shoulders and knees that is worse in the morning and tingling in the upper extremities. Examination shows marked tenderness over the posterior neck, bilateral mid trapezius, and medial aspect of the left knee. A complete blood count and erythrocyte sedimentation rate are within the reference ranges. Which of the following is the most likely diagnosis?
A 48-year-old woman comes to the physician because of a 6-month history of muscle stiffness, myalgia, and a 7-kg (15-lb) weight gain. Her last menstrual period was 4 months ago. Physical examination shows cold, dry skin, and proximal muscle weakness. Deep tendon reflexes are 2+ bilaterally, with delayed relaxation. The creatine kinase level is 2,940 U/L. Which of the following is the most appropriate next step in diagnosis?
A 42-year-old man presents to clinic complaining of increasing difficulty climbing stairs and standing up from sitting in his chair. On exam you perceive his strength to be 5/5 distally, but only 3/5 in proximal muscle groups bilaterally. There is a distinctive rash on his upper eyelids and around his eyes. Examination of the fingers is most likely to reveal which of the following?
A 33-year-old woman comes to the clinic for a follow-up visit after recently starting high dose corticosteroids for a newly diagnosed autoimmune condition. She was first evaluated a month ago due to fatigue, muscle weakness, and a scaly rash on both hands. On examination, muscle strength was rated 2 out of 5 in the upper extremities. Creatine kinase-MB was elevated, and anti-Jo-1 antibodies were observed. A muscle biopsy later showed perimysial inflammation and treatment was initiated. Today, the patient says that her symptoms have not improved despite treatment with corticosteroids. It is agreed upon to initiate methotrexate with the hopes of achieving better symptom control. Which of the following is most often associated with this patient’s condition?
A 32-year-old woman comes to the physician because of increasing muscle weakness in her shoulders and legs for 6 weeks. She is unable to climb stairs or comb her hair. She has also had difficulty swallowing food for the past week. Her symptoms do not improve with rest. Physical examination shows normal muscle tone. There is bilateral weakness of the iliopsoas, hamstring, deltoid, and biceps muscles. Deep tendon reflexes are 2+ bilaterally. Sensation to pinprick, temperature, and vibration is intact. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 10.7 g/dL Leukocyte count 10.800/mm3 Erythrocyte sedimentation rate 100 mm/h Serum Glucose 60 mg/dL Creatine kinase 7047 U/L Lactate dehydrogenase 2785 U/L Thyroid-stimulating hormone 4.0 μU/mL Which of the following is the most appropriate next step in management?
A 13-year-old girl is admitted to the hospital due to muscle weakness, pain, and arthralgia in her wrist joints. The patient says, "I am having trouble walking home after school, especially climbing steep hills." She also complains of malaise. On physical examination, a heliotrope rash is observed around her eyes, and multiple hyperkeratotic, flat, red papules with central atrophy are present on the back of the metacarpophalangeal and interphalangeal joints. Deposits of calcium are also noted on the pads of her fingers. Her serum creatine kinase levels are elevated. Which of the following antibodies is most likely to be found in this patient?
A 38-year-old woman presents with progressive muscle weakness. The patient says that symptoms onset a couple of weeks ago and have progressively worsened. She says she hasn’t been able to lift her arms to comb her hair the past few days. No significant past medical history and no current medications. Family history is significant for her mother with scleroderma and an aunt with systemic lupus erythematosus (SLE). On physical examination, strength is 2 out of 5 in the upper extremities bilaterally. There is an erythematous area, consisting of alternating hypopigmentation and hyperpigmentation with telangiectasias, present on the extensor surfaces of the arms, the upper chest, and the neck in a ‘V-shaped’ distribution. Additional findings are presented in the exhibit (see image). Laboratory tests are significant for a positive antinuclear antibody (ANA) and elevated creatinine phosphokinase. Which of the following is the most appropriate first-line treatment for this patient?
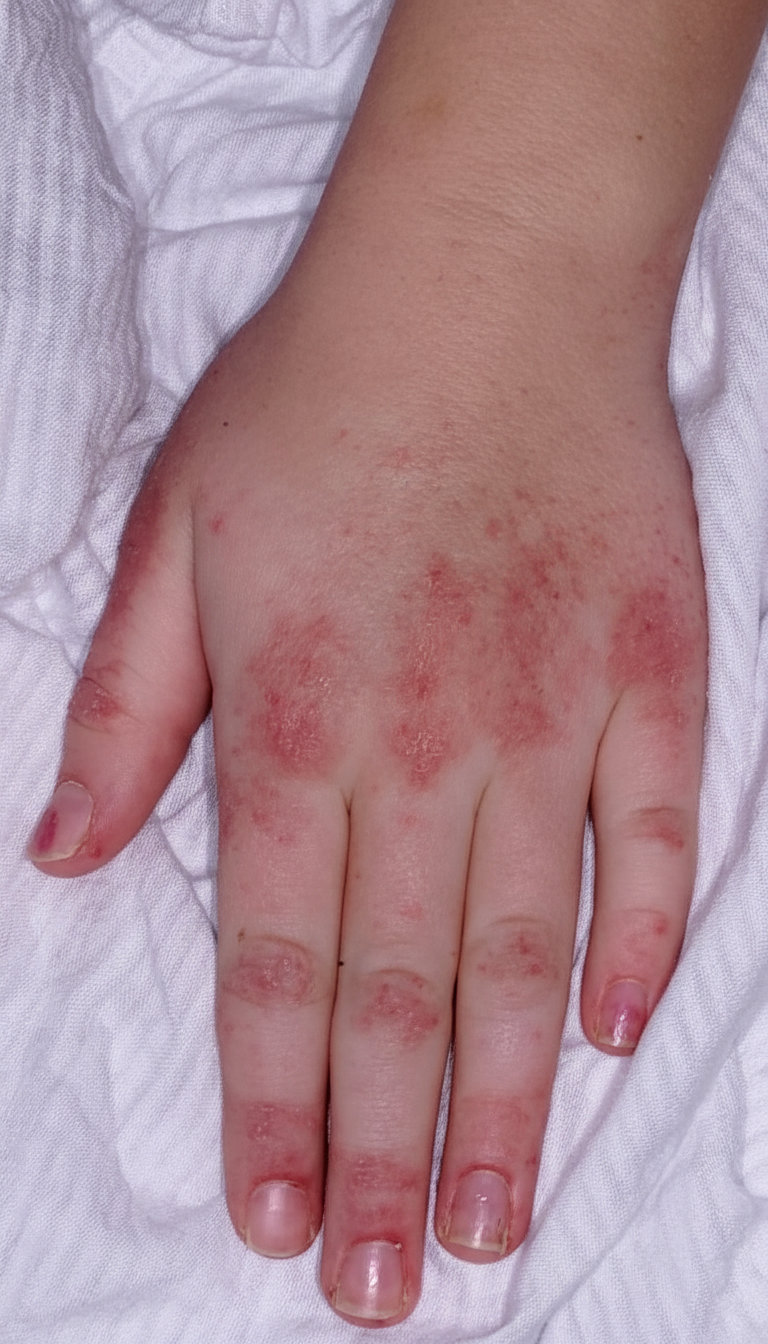
A 45-year-old woman presents to the clinic complaining of weakness that has progressively worsened over the past 2 weeks. She states that she has a hard time lifting both her arms but that they function normally. She notes no history of trauma or other deficits. On examination, that patient has 2/5 muscle strength on shoulder shrug and arm abduction bilaterally, but all other neurological exam findings are normal. You notice some skin changes and ask the patient about them. She states that she has had a rash around her eyes as well as on her lower face, going down to her neck and chest. She notes that the rashes started around the same time as the weakness began. Labs are drawn and a complete blood count and basic metabolic panel are normal. Which of the following is the most likely diagnosis?
A 56-year-old woman presents to the emergency department with muscle weakness. She reports her symptoms have progressively worsened over the course of 2 weeks and are most significant in her lower extremities. She also notices increased urinary frequency. Approximately 1 month ago she was diagnosed with a calcium phosphate nephrolithiasis. Medical history is significant for rheumatoid arthritis diagnosed approximately 10 years ago treated with methotrexate, and type II diabetes mellitus treated with metformin. Her temperature is 98.6°F (37°C), blood pressure is 138/92 mmHg, pulse is 92/min, and respirations are 17/min. On physical exam, there is mild tenderness to palpation of the metacarpophalangeal and proximal interphalangeal joints. There is 4/5 power throughout the lower extremity. Laboratory testing is shown. Serum: Na+: 137 mEq/L Cl-: 106 mEq/L K+: 2.9 mEq/L HCO3-: 18 mEq/L Glucose: 115 mg/dL Creatinine: 1.0 mg/dL Urine pH: 5.6 Which of the following is the best next step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
