Liver disease — MCQs

On this page
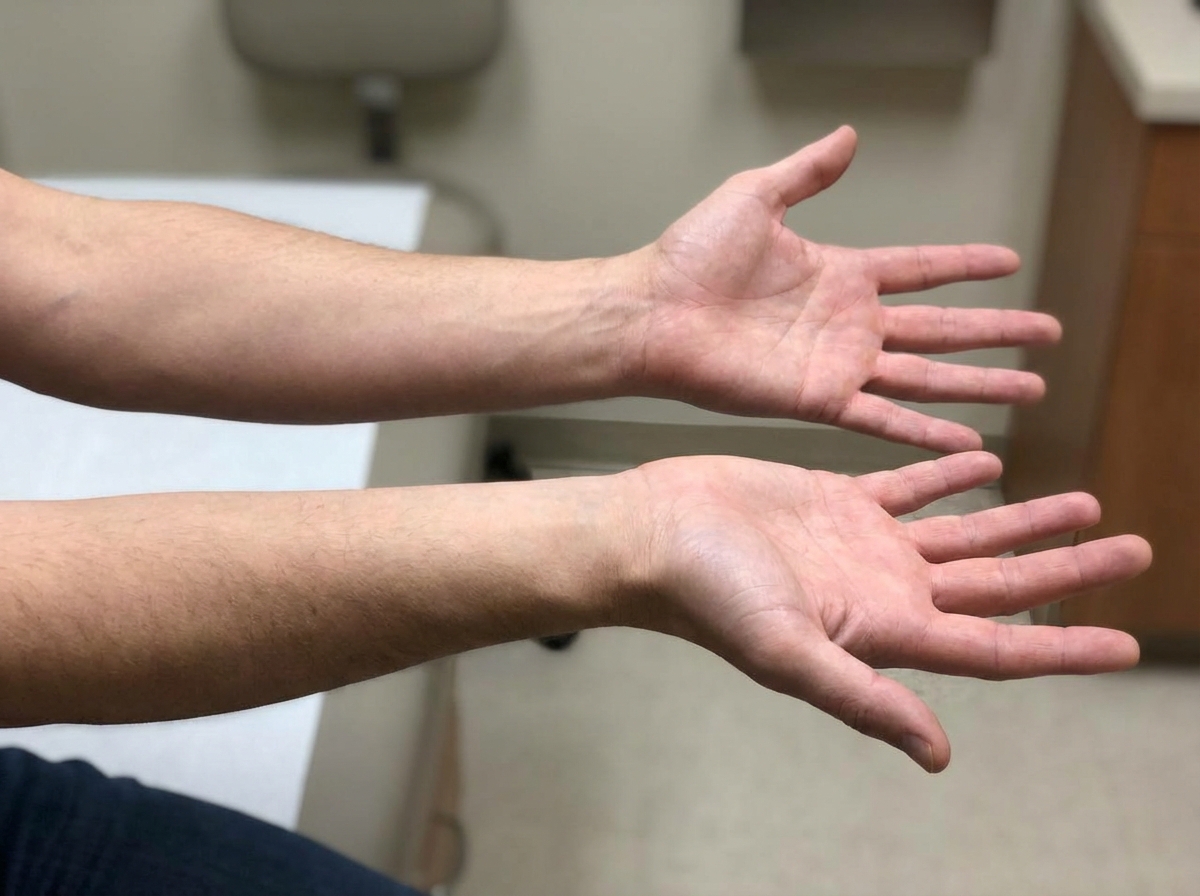
A 56-year-old male with a history of hepatitis C cirrhosis status post TIPS procedure is brought in by his wife to the emergency department because he has been acting disoriented, slurring his speech, and sleeping throughout the day. On arrival the patient is afebrile and his vital signs are pulse is 87/min, blood pressure is 137/93 mmHg, and respirations are 12/min with shallow breaths. Examination reveals a jaundiced male who appears older than stated age. Abdominal exam is positive for a fluid wave and shifting dullness to percussion. You note enlarged breasts, decreased facial hair, 3+ patellar reflexes bilaterally, and the following in the upper extremity (Image A). Paracentesis reveals ascitic fluid with neutrophil counts of < 100 cells/mcL. Serum creatinine is 1.0 and BUN is 15. Which of the following is the next best step in management?
A 52-year-old unconscious man is brought to the emergency department. He was found unresponsive on the sidewalk in the snow. He is recognized by the staff as a local homeless man and IV drug user. Rapid warming procedures are initiated. At physical examination, he is dirty and disheveled and unrousable with a blood pressure of 100/76 mm Hg and a temperature of 37.2°C (99°F). He is thin with apparent weight loss. Both arms have indications of recent IV injection stigmata. A head MRI reveals multiple hyperintense signals in the meninges with multiple tiny contrast-enhancing lesions in the cerebellum and cerebral cortex. A chest X-ray is within normal limits. Mild dilatation of the ventricles is also appreciated. Cerebrospinal fluid (CSF) analysis reveals: CSF opening pressure 25 cm H20 CSF total leukocyte count 580/mm3 Lymphocytes 90% Neutrophils 10% CSF protein 176 mg/dL CSF glucose 21 mg/dL A specimen stains are positive for acid-fast bacilli. CSF culture is pending. Appropriate antibacterial medication is initiated. Which of the following is true regarding the immediate future management of this patient?
A 58-year-old man with liver cirrhosis presents to his primary care physician complaining of increased abdominal girth and early satiety. He drinks 2–4 glasses of wine with dinner and recalls having had abnormal liver enzymes in the past. Vital signs include a temperature of 37.1°C (98.7°F), blood pressure of 110/70 mm Hg, and a pulse of 75/min. Physical examination reveals telangiectasias, mild splenomegaly, palpable firm liver, and shifting dullness. Liver function is shown: Total bilirubin 3 mg/dL Aspartate aminotransferase (AST) 150 U/L Alanine aminotransferase (ALT) 70 U/L Total albumin 2.5 g/dL Abdominal ultrasonography confirms the presence of ascites. Diagnostic paracentesis is performed and its results are shown: Polymorphonuclear cell count 10 cells/mm Ascitic protein 1 g/dL Which of the following best represents the mechanism of ascites in this patient?
A 49-year-old man is brought to the emergency department by his wife because he is vomiting blood. His wife reports that he has been nauseous for the past day and that he has had 2 episodes of vomiting bright red blood over the past 2 hours. He has never experienced this before. He has not had any bloody stool, melena, or abdominal pain. He was diagnosed with alcoholic cirrhosis 6 months ago. He drank approximately 1 liter of vodka over the past day, which is typical for him. He takes no medications. He is confused and disoriented to place and time. Physical examination shows ascites. Vital signs are within normal limits. His hemoglobin concentration is 9.5 g/dL. Intravenous fluid resuscitation is begun. He starts to vomit bright red blood again intermittently, which continues for 10 minutes. When vital signs are measured again, his pulse is 95/min and blood pressure is 109/80 mm/Hg. Which of the following is the most appropriate initial step in management?
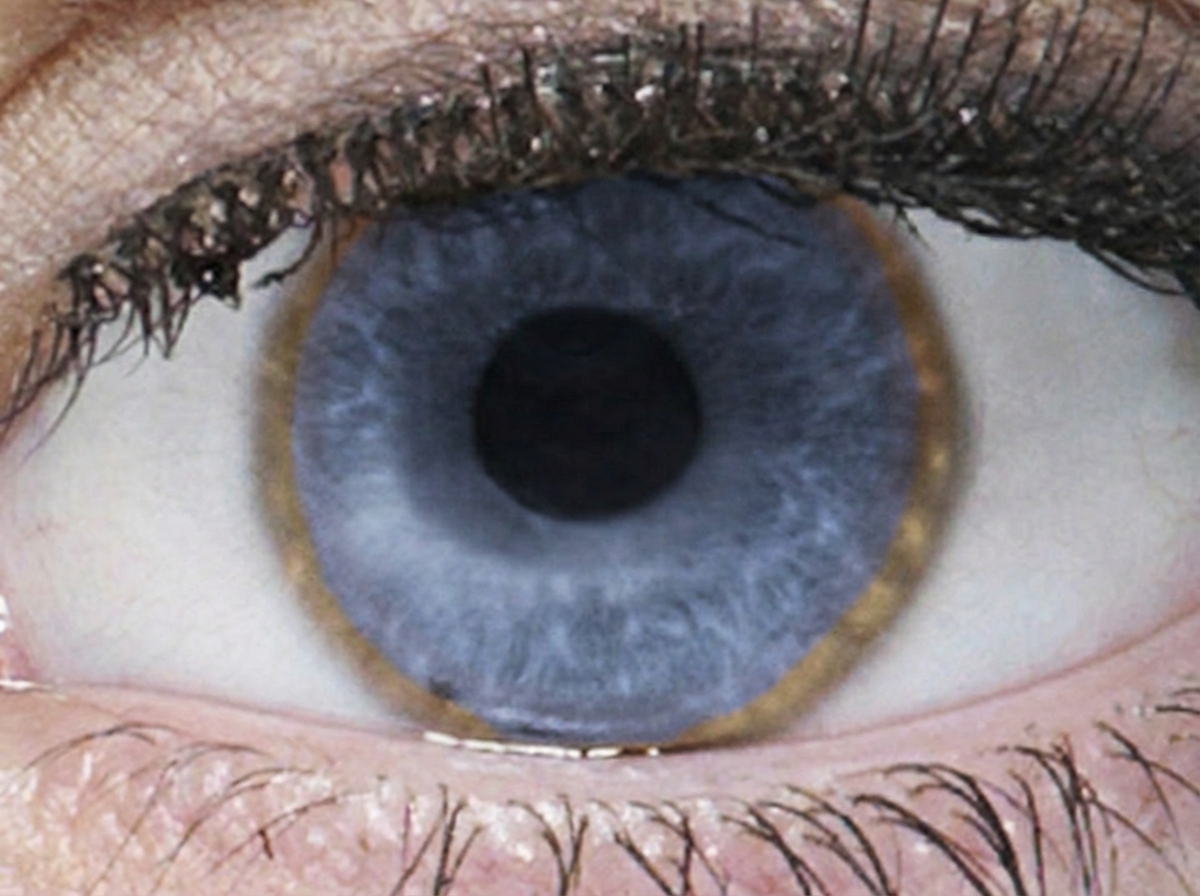
A 28-year-old woman is brought to the physician because of progressive difficulty walking, slowed speech, and a tremor for the past 5 months. Her grandfather died of bleeding esophageal varices at the age of 42 years. She does not drink alcohol. She is alert and oriented but has a flat affect. Her speech is slurred and monotonous. Examination shows a broad-based gait and a low-frequency tremor of her left hand. Abdominal examination shows hepatosplenomegaly. A photograph of the patient's right eye is shown. Further evaluation of this patient is most likely to show which of the following findings?
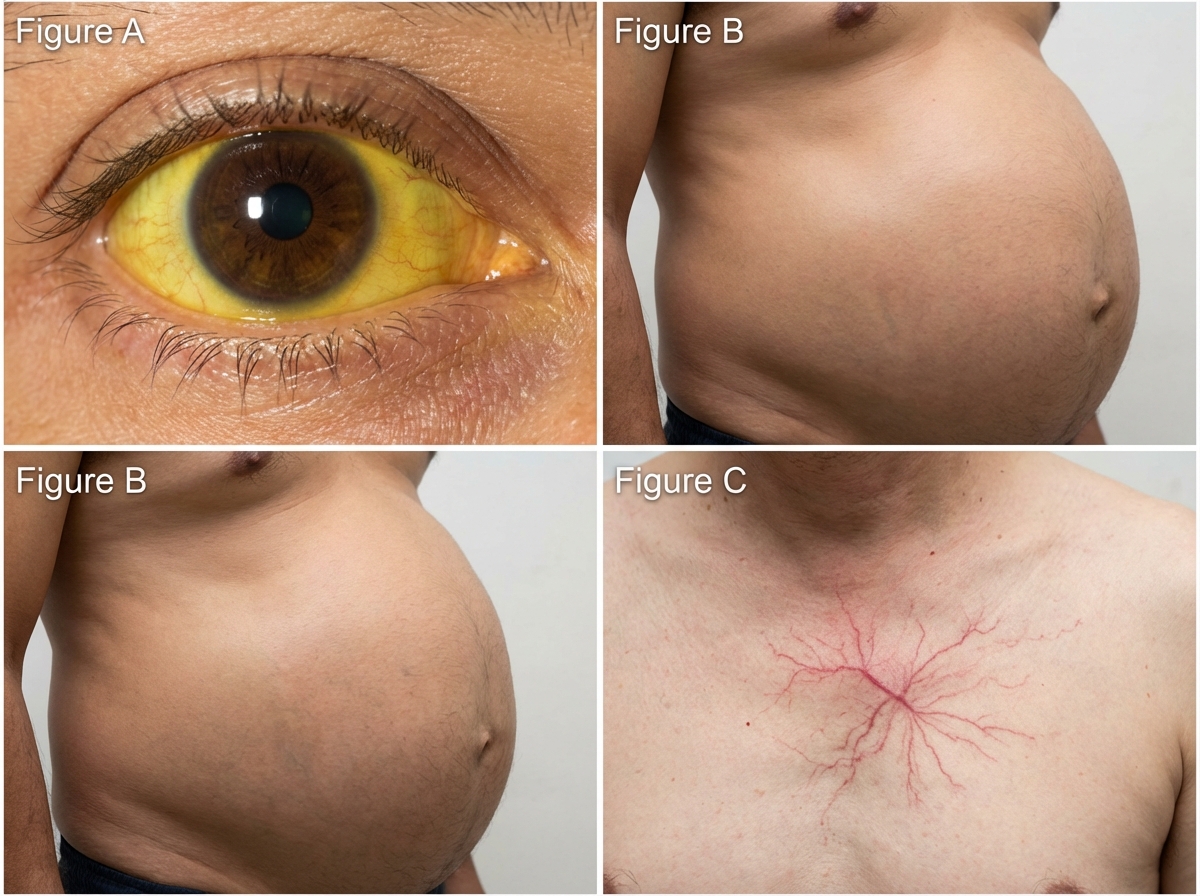
A 64-year-old man who has not seen a physician in over 20 years presents to your office complaining of recently worsening fatigue and weakness, a decreased appetite, distended abdomen, and easy bruising. His family history is notable for a mother with Hashimoto's thyroiditis, a sister with lupus and a brother with type II diabetes. On further questioning, the patient discloses a history of prior alcoholism as well as intravenous drug use, though he currently only smokes a pack per day of cigarettes. On physical exam, you note the following findings (see Figures A-C) as well as several ecchymoses and telangiectasias. As the patient has not seen a physician in many years, you obtain the following laboratory studies: Leukocyte count: 4,100/mm^3 Hemoglobin: 9.6 g/dL Platelet count: 87,000/mm^3 Prothrombin time (PT): 21.0 seconds International Normalized Ratio (INR): 1.8 Serum: Creatinine: 1.7 mg/dL Total bilirubin: 3.2 mg/dL Aspartate aminotransferase (AST): 225 U/L Alanine aminotransferase (ALT): 103 U/L Alkaline phosphatase: 162 U/L Albumin: 2.6 g/dL Serum thyroxine (T4): 3.1 µg/dL Thyroid-stimulating hormone (TSH): 3.4 µU/mL What is the cause of this patient’s low serum thyroxine?
A 57-year-old woman comes to the physician for a routine health maintenance examination. She has well-controlled type 2 diabetes mellitus, for which she takes metformin. She is 163 cm (5 ft 4 in) tall and weighs 84 kg (185 lb); BMI is 31.6 kg/m2. Her blood pressure is 140/92 mm Hg. Physical examination shows central obesity, with a waist circumference of 90 cm. Laboratory studies show: Fasting glucose 94 mg/dl Total cholesterol 200 mg/dL High-density lipoprotein cholesterol 36 mg/dL Triglycerides 170 mg/dL Without treatment, this patient is at greatest risk for which of the following conditions?
A 27-year-old man with an unknown past medical history is brought to the emergency department acutely intoxicated. The patient was found passed out in a park covered in vomit and urine. His temperature is 99.0°F (37.2°C), blood pressure is 107/68 mm Hg, pulse is 120/min, respiratory rate is 13/min, and oxygen saturation is 95% on room air. Physical exam is notable for wheezing in all lung fields without any crackles. The patient is started on 2L/min nasal cannula oxygen and IV fluids. His laboratory values are notable for an AST of 200 U/L and an ALT of 100 U/L. An initial chest radiograph is unremarkable. Which of the following is the most likely explanation for this patient's pulmonary symptoms?
A 48-year-old woman comes to the physician because of a 6-month history of excessive fatigue and a 1-month history of progressively increasing generalized pruritus. She has hypothyroidism, for which she receives thyroid replacement therapy. Physical examination shows jaundice. The liver is palpated 4 cm below the right costal margin. Serum studies show a direct bilirubin concentration of 2.9 mg/dL, alkaline phosphatase activity of 580 U/L, and increased titers of antimitochondrial antibodies and anti-thyroid peroxidase antibodies. Which of the following is the most likely cause of this patient's condition?
A 53-year-old man comes to the physician because of a 3-month history of a nonpruritic rash, fatigue, and decreased urination. Physical examination shows multiple erythematous, purpuric papules on his trunk and extremities that do not blanch when pressed. Serum creatinine is elevated and urinalysis shows red blood cell casts and protein. Serum complement levels are decreased. Renal biopsy shows subendothelial immune complex deposits with granular immunofluorescence and tram-track basement membrane splitting. Further laboratory evaluation of this patient is most likely to show the presence of which of the following antibodies?
Practice by Chapter
Viral hepatitis (A, B, C, D, E)
Practice Questions
Alcoholic liver disease
Practice Questions
Non-alcoholic fatty liver disease
Practice Questions
Drug-induced liver injury
Practice Questions
Autoimmune hepatitis
Practice Questions
Cirrhosis management
Practice Questions
Portal hypertension complications
Practice Questions
Ascites diagnosis and management
Practice Questions
Hepatic encephalopathy
Practice Questions
Spontaneous bacterial peritonitis
Practice Questions
Hepatorenal syndrome
Practice Questions
Hepatocellular carcinoma
Practice Questions
Liver transplantation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
