Liver disease — MCQs

On this page
A 30-year-old woman presents to the office with chief complaints of skin pigmentation and fragility of the extensor sides of both hands for a month. The lesions are progressive and are not directly sensitive to light. The patient is otherwise healthy and only uses an oral contraceptive. There is no skin disease or similar skin symptoms in family members. She consumes 1 glass of wine twice a week. Dermatological examination reveals erosions, erythematous macules, pigmentation, and atrophic scarring. Blood analysis reveals elevated CRP (34 mg/L), AST (91 U/L), ALT (141 U/L), and serum ferritin (786 ng/mL compared to the normal value of 350 ng/mL). Her BMI is 21 kg/m2. Urine porphyrin test results are negative. Autoimmune laboratory analysis, hepatic panel, and HIV serology are negative with a normal liver ultrasound. Genetic analysis shows a homozygous missense mutation of the HFE gene. What could be the long-term effect of her condition to her liver?
A 28-year-old man presents to the office with complaints of malaise, anorexia, and vomiting for the past 2 weeks. He also says that his urine is dark. The past medical history is unremarkable. The temperature is 36.8°C (98.2°F), the pulse is 72/min, the blood pressure is 118/63 mm Hg, and the respiratory rate is 15/min. The physical examination reveals a slightly enlarged, tender liver. No edema or spider angiomata are noted. Laboratory testing showed the following: HBsAg Positive IgM anti-HBc < 1:1,000 Anti-HBs Negative HBeAg Positive Anti-HBe Negative HBV DNA 2.65 × 10⁹ IU/L Alpha-fetoprotein 125 ng/mL What is the most likely cause of this patient's condition?
A 44-year-old man with HIV comes to the physician for a routine follow-up examination. He has been noncompliant with his antiretroviral medication regimen for several years. He appears chronically ill and fatigued. CD4+ T-lymphocyte count is 180/mm³ (N ≥ 500). Further evaluation of this patient is most likely to show which of the following findings?
A 55-year-old man presents to the emergency department with hematemesis that started 1 hour ago but has subsided. His past medical history is significant for cirrhosis with known esophageal varices which have been previously banded. His temperature is 97.5°F (36.4°C), blood pressure is 114/64 mmHg, pulse is 130/min, respirations are 12/min, and oxygen saturation is 98% on room air. During the patient's physical exam, he begins vomiting again and his heart rate increases with a worsening blood pressure. He develops mental status changes and on exam he opens his eyes and flexes his arms only to sternal rub and is muttering incoherent words. Which of the following is the most appropriate next step in management?
A 61-year-old man comes to the physician because of fatigue and a 5-kg (11-lb) weight loss over the past 6 months. He experimented with intravenous drugs during his 20s and has hepatitis C. His father died of colon cancer. He has smoked one pack of cigarettes daily for 35 years. Physical examination shows scleral icterus and several telangiectasias on the abdomen. The liver is firm and nodular. Laboratory studies show: Hemoglobin 10.9 g/dL Mean corpuscular volume 88 μm3 Leukocyte count 10,400/mm3 Platelet count 260,000/mm3 Ultrasonography of the liver is shown. Which of the following additional findings is most likely?
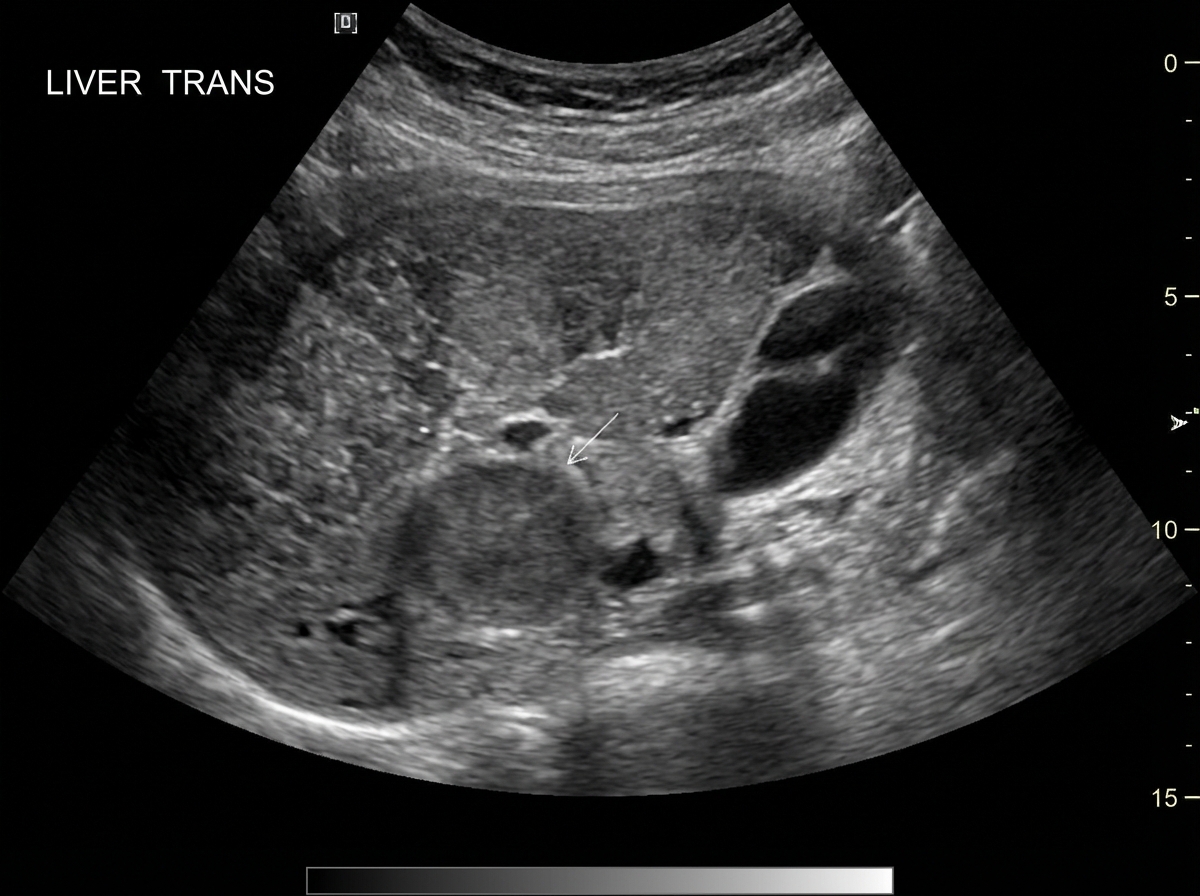
A 45-year-old man comes to the physician for a routine health maintenance examination. He feels well. He has type 2 diabetes mellitus. There is no family history of serious illness. He works as an engineer at a local company. He does not smoke. He drinks one glass of red wine every other day. He does not use illicit drugs. His only medication is metformin. He is 180 cm (5 ft 11 in) tall and weighs 100 kg (220 lb); BMI is 31 kg/m2. His vital signs are within normal limits. Examination shows a soft, nontender abdomen. The liver is palpated 2 to 3 cm below the right costal margin. Laboratory studies show an aspartate aminotransferase concentration of 100 U/L and an alanine aminotransferase concentration of 130 U/L. Liver biopsy shows hepatocyte ballooning degeneration, as well as inflammatory infiltrates with scattered lymphocytes, neutrophils, and Kupffer cells. Which of the following is the most likely diagnosis?
A 45-year-old man comes to the physician because of a 6-month history of increasing fatigue and reduced libido. He also complains of joint pain in both of his hands. He has a history of hypertension that is controlled with enalapril. He does not smoke or use illicit drugs. He drinks 2–3 beers on the weekends. His vital signs are within normal limits. Physical examination shows a strongly-tanned patient and decreased size of the testes. The second and third metacarpophalangeal joints of both hands are tender to palpation and range of motion is limited. The liver is palpated 2 to 3 cm below the right costal margin. Laboratory studies show: Ferritin 2500 μg/L Aspartate aminotransferase 70 U/L Alanine aminotransferase 80 U/L Glucose 250 mg/dL This patient is at greatest risk for developing which of the following complications?
A 59-year-old man with chronic hepatitis C infection comes to the physician because of a 2-week history of ankle pain and nonpruritic skin lesions on his legs. He does not recall recent trauma or injury. He has not received treatment for hepatitis. Examination shows diffuse, violaceous lesions on both lower extremities. The lesions are 4–7 mm in size, slightly raised, and do not blanch with pressure. These skin lesions are best classified as which of the following?
A 45-year-old man comes to the physician because of bright red blood in his stool for 5 days. He has had no pain during defecation and no abdominal pain. One year ago, he was diagnosed with cirrhosis after being admitted to the emergency department for upper gastrointestinal bleeding. He has since cut down on his drinking and consumes around 5 bottles of beer daily. Examination shows scleral icterus and mild ankle swelling. Palpation of the abdomen shows a fluid wave and shifting dullness. Anoscopy shows enlarged bluish vessels above the dentate line. Which of the following is the most likely source of bleeding in this patient?
A 52-year-old man comes to the physician because of progressive abdominal distention and weight gain over the last 2 months. He was diagnosed with alcoholic liver cirrhosis with large ascites 1 year ago. He has congestive heart failure with a depressed ejection fraction related to his alcohol use. For the last 6 months, he has abstained from alcohol and has followed a low-sodium diet. His current medications include propranolol, spironolactone, and furosemide. His temperature is 36.7°C (98°F), pulse is 90/min, and blood pressure is 109/56 mm Hg. Physical examination shows reddening of the palms, telangiectasias on the face and trunk, and prominent blood vessels around the umbilicus. The abdomen is tense and distended; there is no abdominal tenderness. On percussion of the abdomen, there is dullness that shifts when the patient moves from the supine to the right lateral decubitus position. When the patient stretches out his arms with the wrists extended, a jerky, flapping motion of the hands is seen. Mental status examination shows a decreased attention span. Serum studies show: Sodium 136 mEq/L Creatinine 0.9 mg/dL Albumin 3.6 mg/dL Total bilirubin 1.9 mg/dL INR 1.0 Which of the following is the most appropriate next step in treatment?
Practice by Chapter
Viral hepatitis (A, B, C, D, E)
Practice Questions
Alcoholic liver disease
Practice Questions
Non-alcoholic fatty liver disease
Practice Questions
Drug-induced liver injury
Practice Questions
Autoimmune hepatitis
Practice Questions
Cirrhosis management
Practice Questions
Portal hypertension complications
Practice Questions
Ascites diagnosis and management
Practice Questions
Hepatic encephalopathy
Practice Questions
Spontaneous bacterial peritonitis
Practice Questions
Hepatorenal syndrome
Practice Questions
Hepatocellular carcinoma
Practice Questions
Liver transplantation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
