Liver disease — MCQs

On this page
A 42-year-old woman presents with pruritus and progressive weakness for the past 3 months. She says she feels excessively tired during the daytime and is losing interest in activities that used to be fun. The patient reports a history of heavy alcohol use and drinks around 20 ounces per week. Laboratory studies show: Proteins 6.5 g/dL Albumin 4.5 g/dL Globulin 1.9 g/dL Bilirubin 5.8 mg/dL Serum alanine aminotransferase (ALT) 86 U/L Serum aspartate transaminase (AST) 84 U/L Serum alkaline phosphatase (ALP) 224 U/L Antinuclear antibody (ANA) positive Antimitochondrial antibody (AMA) positive anti-HBs positive anti-HBc negative Which is the most likely diagnosis in this patient?
A 48-year-old man is brought to the emergency department by his wife because of a 3-day history of increasing confusion and lethargy. He complains of decreased urine output and abdominal pain for the past month. Two months ago, he was hospitalized for pyelonephritis and treated with ceftriaxone. He has a history of chronic hepatitis C. He does not take any medications. He appears pale and irritable. His temperature is 37°C (98.6°F), pulse is 90/min, and blood pressure is 98/60 mm Hg. On mental status examination, he is oriented to person but not to time or place. Physical examination shows scleral icterus and jaundice. There is 2+ pitting edema of the lower extremities. The abdomen is distended with a positive fluid wave. Laboratory studies show: Hemoglobin 10.1 g/dL Leukocyte count 4300/mm3 Platelet count 89,000/mm3 Prothrombin time 19 sec Serum Urea nitrogen 71 mg/dL Glucose 99 mg/dL Creatinine 3.5 mg/dL ALT 137 mg/dL AST 154 mg/dL Urinalysis shows no abnormalities. The FeNa is < 1%. Ultrasound of the kidneys is unremarkable. Intravenous fluids are administered for 36 hours but do not improve urine output. Which of the following is the most likely cause of the kidney dysfunction in this patient?
A 24-year-old woman arrives to an urgent care clinic for "eye discoloration." She states that for the past 3 days she has had the “stomach flu” and has not been eating much. Today, she reports she is feeling better, but when she woke up "the whites of [her] eyes were yellow." She denies fever, headache, palpitations, abdominal pain, nausea, vomiting, and diarrhea. She was recently diagnosed with polycystic ovary syndrome during a gynecology appointment 2 weeks ago for irregular menses. Since then, she has been taking a daily combined oral contraceptive. She takes no other medications. Her temperature is 98.6°F (37°C), blood pressure is 120/80 mmHg, and pulse is 76/min. Body mass index is 32 kg/m^2. On physical examination, there is scleral icterus and mild jaundice. Liver function tests are drawn, as shown below: Alanine aminotransferase (ALT): 19 U/L Aspartate aminotransferase (AST): 15 U/L Alkaline phosphatase: 85 U/L Albumin: 4.0 g/dL Total bilirubin: 12 mg/dL Direct bilirubin: 10 mg/dL Prothrombin time: 13 seconds If a liver biopsy were to be performed and it showed a normal pathology, which of the following would be the most likely diagnosis?
A 45-year-old man is brought to the emergency department because of a 1-day history of malaise and abdominal pain. Six weeks ago, he had vomiting and watery diarrhea for 2 days that resolved without treatment. Twelve weeks ago, he underwent orthotopic liver transplantation for alcoholic cirrhosis. At the time of discharge, his total serum bilirubin concentration was 1.0 mg/dL. He stopped drinking alcohol one year ago. His current medications include daily tacrolimus, prednisone, valganciclovir, and trimethoprim-sulfamethoxazole. His temperature is 37.7°C (99.9°F), pulse is 95/min, and blood pressure is 150/80 mm Hg. He appears uncomfortable and has mild jaundice. Examination shows scleral icterus. The abdomen is soft and tender to deep palpation over the right upper quadrant, where there is a well-healed surgical scar. His leukocyte count is 2500/mm3, serum bilirubin concentration is 2.6 mg/dL, and serum tacrolimus concentration is within therapeutic range. Which of the following is the next appropriate step in diagnosis?
A 69-year-old man with aggressive metastatic cholangiocarcinoma presents after the second round of chemotherapy. He has suffered a great deal of pain from the metastasis to his spine, and he is experiencing side effects from the cytotoxic chemotherapy drugs. Imaging shows no change in the tumor mass and reveals the presence of several new metastatic lesions. The patient is not willing to undergo any more chemotherapy unless he gets something for pain that will “knock him out”. High-dose opioids would be effective, in his case, but carry a risk of bradypnea and sudden respiratory failure. Which of the following is the most appropriate next step in management?
A 30-year-old man presents to clinic. He was born in southeast Asia and immigrated to the US three years ago. He has a history of chronic hepatitis C which he contracted from intravenous drug use. He reports that he has been receiving treatment for his hepatitis C, but unfortunately has started using heroin again. The patient was seen in the clinic last week and had blood work done. His results are as follows: HBsAg - negative; HBsAb - negative; HBcAb - negative. In addition to encouraging the patient to seek treatment for his heroin addiction, what else should be done at this health visit for general health maintenance?
A 53-year-old man comes to the physician because of a 3-month history of a nonpruritic rash. He has been feeling more tired than usual and occasionally experiences pain in his wrists and ankles. He does not smoke or drink alcohol. His temperature is 37.6°C (99.7°F), pulse is 98/min, respirations are 18/min, and blood pressure is 130/75 mm Hg. Physical examination shows multiple, erythematous, purpuric papules on his trunk and extremities that do not blanch when pressed. The remainder of the examination shows no abnormalities. The patient's hemoglobin is 14 g/dL, leukocyte count is 9,500/mm3, and platelet count is 228,000/mm3. Urinalysis and liver function tests are within normal limits. The test for rheumatoid factor is positive. Serum ANA is negative. Serum complement levels are decreased. Serum protein electrophoresis and immunofixation shows increased gammaglobulins with pronounced polyclonal IgM and IgG bands. Testing for cryoglobulins shows no precipitate after 24 hours. Chest x-ray and ECG show no abnormalities. Which of the following is the most appropriate next step in management?
A 46-year-old man comes to the physician for a follow-up examination. Two weeks ago, he underwent laparoscopic herniorrhaphy for an indirect inguinal hernia. During the procedure, a black liver was noted. He has a history of intermittent scleral icterus that resolved without treatment. Serum studies show: Aspartate aminotransferase 30 IU/L Alanine aminotransferase 35 IU/L Alkaline phosphatase 47 mg/dL Total bilirubin 1.7 mg/dL Direct bilirubin 1.1 mg/dL Which of the following is the most likely diagnosis?
A 59-year-old man presents to his primary care physician for fatigue. In general, he has been in good health; however, he recently has experienced some weight loss, abdominal pain, and general fatigue. He has a past medical history of anxiety, diabetes, a fracture of his foot sustained when he tripped, and a recent cold that caused him to miss work for a week. His current medications include metformin, insulin, buspirone, vitamin D, calcium, and sodium docusate. His temperature is 99.5°F (37.5°C), blood pressure is 150/100 mmHg, pulse is 90/min, respirations are 18/min, and oxygen saturation is 98% on room air. Physical exam reveals a calm gentleman. A mild systolic murmur is heard in the left upper sternal region. The rest of the physical exam is within normal limits. Laboratory values are ordered as seen below. Hemoglobin: 12 g/dL Hematocrit: 36% Leukocyte count: 66,500/mm^3 with normal differential Platelet count: 177,000/mm^3 Leukocyte alkaline phosphatase: elevated Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L BUN: 20 mg/dL Glucose: 120 mg/dL Creatinine: 1.1 mg/dL Ca2+: 10.9 mEq/L AST: 12 U/L ALT: 10 U/L Which of the following is the most likely diagnosis?
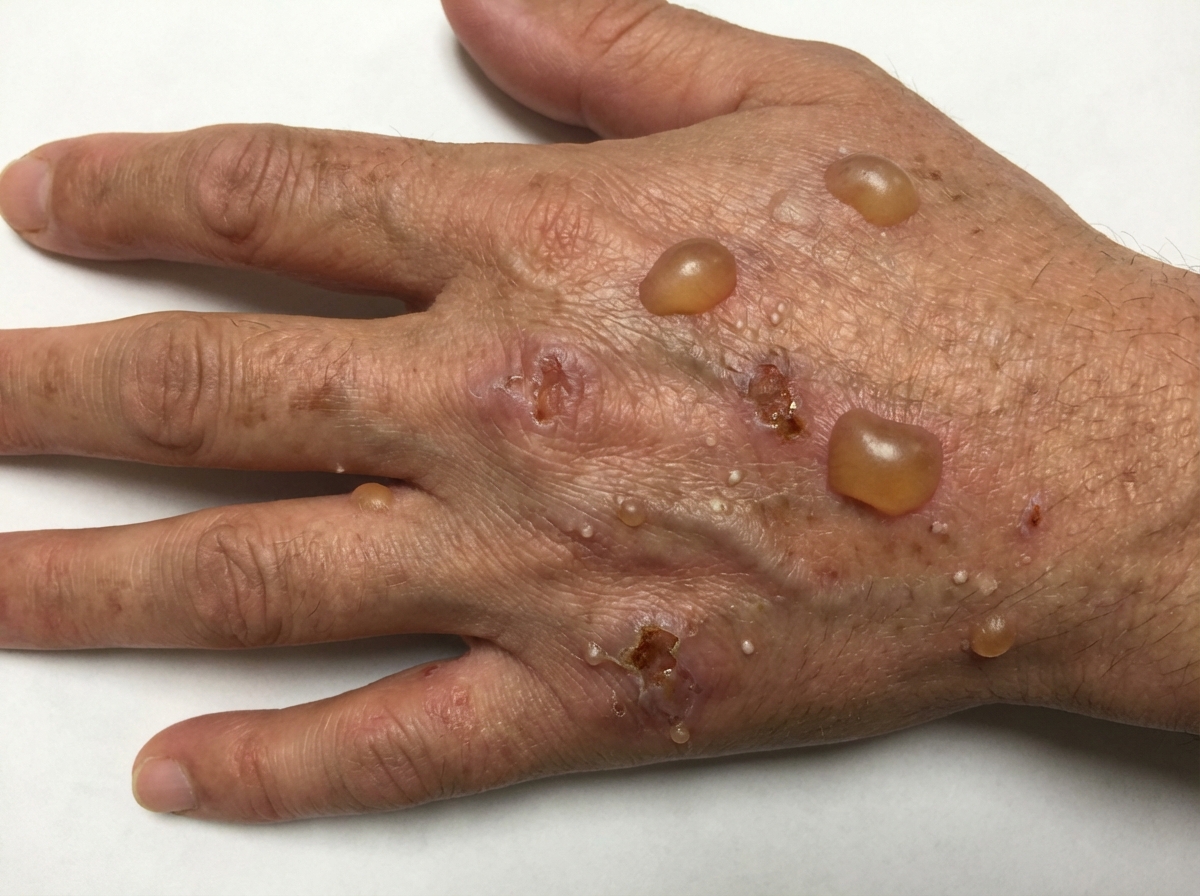
A 42-year-old woman comes to the physician with a rash on the dorsal surfaces of her hands and feet for the past month. The rash began as blisters that developed a few days after she had been sunbathing on the beach. Photographs of the rash are shown. She has no history of similar symptoms, takes no medications, and has no history of recent travels. She has consumed excess alcohol several times over the past 2 months. Her temperature is 37.1°C (98.8°F). The remainder of the physical examination shows no abnormalities. Laboratory studies show elevated plasma porphyrins, with normal urinary 5-aminolevulinic acid and porphobilinogen. Which of the following is the most appropriate next step in management?
Practice by Chapter
Viral hepatitis (A, B, C, D, E)
Practice Questions
Alcoholic liver disease
Practice Questions
Non-alcoholic fatty liver disease
Practice Questions
Drug-induced liver injury
Practice Questions
Autoimmune hepatitis
Practice Questions
Cirrhosis management
Practice Questions
Portal hypertension complications
Practice Questions
Ascites diagnosis and management
Practice Questions
Hepatic encephalopathy
Practice Questions
Spontaneous bacterial peritonitis
Practice Questions
Hepatorenal syndrome
Practice Questions
Hepatocellular carcinoma
Practice Questions
Liver transplantation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
