Liver disease — MCQs

On this page
A 52-year-old man presents to his primary care physician for generalized pain. The patient states that he feels like his muscles and bones are in constant pain. This has persisted for the past several weeks, and his symptoms have not improved with use of ibuprofen or acetaminophen. The patient has a past medical history of alcohol abuse, repeat episodes of pancreatitis, constipation, and anxiety. He has a 22 pack-year smoking history. His temperature is 99.5°F (37.5°C), blood pressure is 140/95 mmHg, pulse is 70/min, respirations are 15/min, and oxygen saturation is 99% on room air. On physical exam, you note generalized tenderness/pain of the patient's extremities. Abdominal exam reveals normoactive bowel sounds and is non-tender. Dermatologic exam is unremarkable. Laboratory values are ordered as seen below. Hemoglobin: 12 g/dL Hematocrit: 36% Leukocyte count: 7,500/mm^3 with normal differential Platelet count: 147,000/mm^3 Serum: Na+: 138 mEq/L Cl-: 100 mEq/L K+: 4.2 mEq/L HCO3-: 24 mEq/L BUN: 20 mg/dL Glucose: 99 mg/dL Creatinine: 1.0 mg/dL Ca2+: 10.2 mg/dL Alkaline phosphatase: 252 U/L Lipase: 30 U/L AST: 12 U/L ALT: 10 U/L Which of the following is associated with this patient's condition?
A 32-year-old man comes to the physician for a follow-up examination. He has a 2-month history of increasing generalized fatigue and severe pruritus. He has hypertension and ulcerative colitis which was diagnosed via colonoscopy 5 years ago. Current medications include lisinopril and rectal mesalamine. He is sexually active with 2 female partners and uses condoms inconsistently. His temperature is 37.3°C (99.1°F), pulse is 86/min, and blood pressure is 130/84 mm Hg. Examination shows scleral icterus and multiple scratch marks on the trunk and extremities. The lungs are clear to auscultation. The abdomen is soft and nontender. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 11.5 g/dL Leukocyte count 7500/mm3 Platelet count 280,000/mm3 Serum Na+ 138 mEq/L Cl- 101 mEq/L K+ 4.7 mEq/L Urea nitrogen 18 mg/dL Glucose 91 mg/dL Creatinine 0.8 mg/dL Bilirubin Total 1.5 mg/dL Direct 0.9 mg/dL Alkaline phosphatase 460 U/L AST 75 U/L ALT 78 U/L Anti-nuclear antibody negative Antimitochondrial antibodies negative Abdominal ultrasound shows thickening of the bile ducts and focal bile duct dilatation. Which of the following is the most likely diagnosis?
A 48-year-old man is brought to the emergency department by his wife 20 minutes after she witnessed him vigorously shaking for about 1 minute. During this episode, he urinated on himself. He feels drowsy and has nausea. He has a history of chronic alcoholism; he has been drinking 15 beers daily for the past 3 days. Before this time, he drank 8 beers daily. His last drink was 2 hours ago. He appears lethargic. His vital signs are within normal limits. Physical and neurologic examinations show no other abnormalities. On mental status examination, he is confused and not oriented to time. Laboratory studies show: Hematocrit 44.0% Leukocyte count 12,000/mm3 Platelet count 320,000/mm3 Serum Na+ 112 mEq/L Cl- 75 mEq/L K+ 3.8 mEq/L HCO3- 13 mEq/L Urea nitrogen 6 mEq/L Creatinine 0.6 mg/dL Albumin 2.1 g/dL Glucose 80 mg/dL Urgent treatment for this patient's current condition puts him at increased risk for which of the following adverse events?
A 50-year-old woman presents with esophageal varices, alcoholic cirrhosis, hepatic encephalopathy, portal hypertension, and recent onset confusion. The patient’s husband does not recall her past medical history but knows her current medications and states that she is quite disciplined about taking them. Current medications are spironolactone, labetalol, lactulose, and furosemide. Her temperature is 38.3°C (100.9°F), heart rate is 115/min, blood pressure is 105/62 mm Hg, respiratory rate is 12/min, and oxygen saturation is 96% on room air. On physical examination, the patient is disoriented, lethargic, and poorly responsive to commands. A cardiac examination is unremarkable. Lungs are clear to auscultation. The abdomen is distended, tense, and mildly tender. Mild asterixis is present. Neurologic examination is normal. The digital rectal examination reveals guaiac negative stool. Laboratory findings are significant for the following: Basic metabolic panel Unremarkable Platelet count 95,500/µL Leukocyte count 14,790/µL Hematocrit 33% (baseline is 30%) Which of the following would most likely be of diagnostic value in this patient?
A 46-year-old man comes to the emergency department because of a 10-day history of right upper quadrant abdominal pain. He has also been feeling tired and nauseous for the past 6 weeks. On examination, scleral icterus is present. Abdominal examination shows tenderness to palpation in the right upper quadrant. The liver edge is palpated 2 cm below the right costal margin. Laboratory studies show: Aspartate aminotransferase 1780 U/L Alanine aminotransferase 2520 U/L Hepatitis A IgM antibody Negative Hepatitis B surface antigen Negative Hepatitis B surface antibody Negative Hepatitis B core IgM antibody Positive Hepatitis C antibody Positive Hepatitis C RNA Negative Which of the following is the best course of action for this patient?
A 48-year-old woman comes to the emergency department because of a photosensitive blistering rash on her hands, forearms, and face for 3 weeks. The lesions are not itchy. She has also noticed that her urine has been dark brown in color recently. Twenty years ago, she was successfully treated for Coats disease of the retina via retinal sclerotherapy. She is currently on hormonal replacement therapy for perimenopausal symptoms. Her aunt and sister have a history of a similar skin lesions. Examination shows multiple fluid-filled blisters and oozing erosions on the forearms, dorsal side of both hands, and forehead. There is hyperpigmented scarring and patches of bald skin along the sides of the blisters. Laboratory studies show a normal serum ferritin concentration. Which of the following is the most appropriate next step in management to induce remission in this patient?
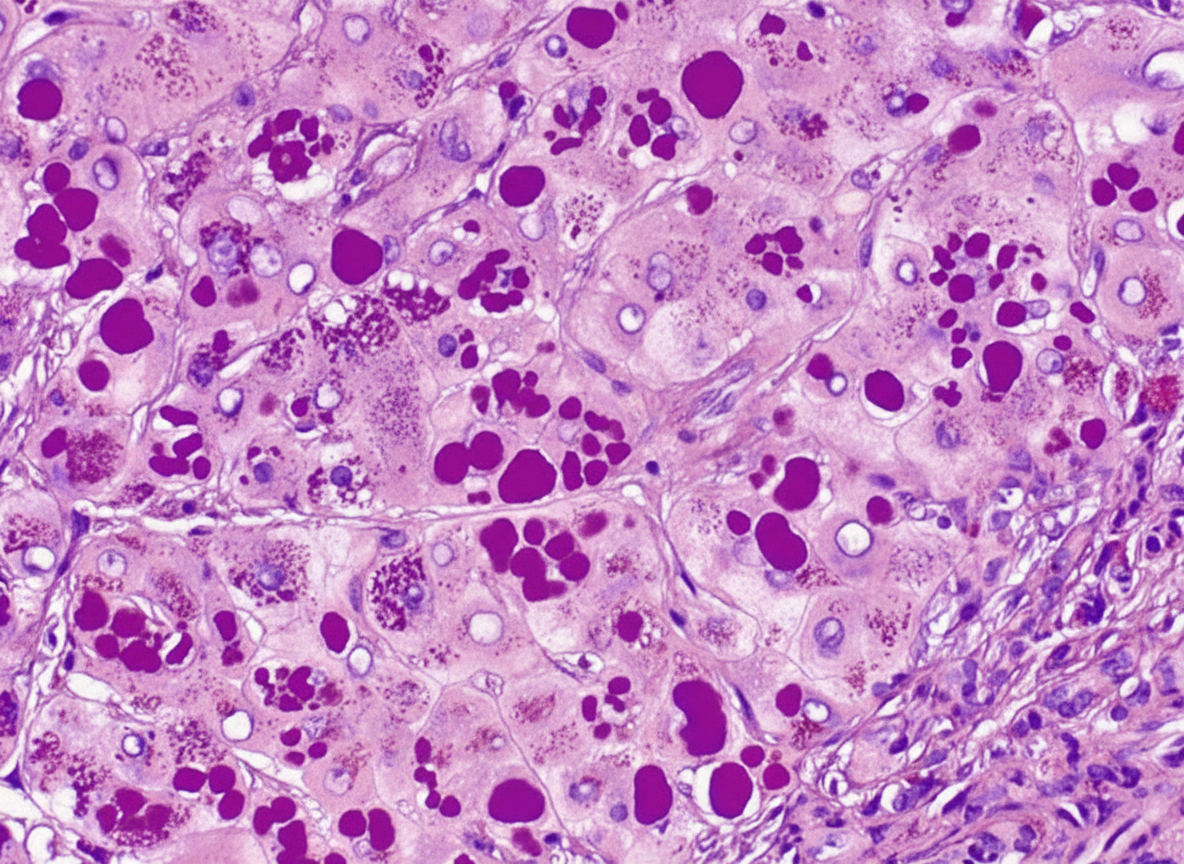
A previously healthy 36-year-old man comes to the physician for a yellow discoloration of his skin and dark-colored urine for 2 weeks. He does not drink any alcohol. Physical examination shows jaundice. Abdominal and neurologic examinations show no abnormalities. Serum studies show increased levels of alanine aminotransferase (ALT) and aspartate aminotransferase (AST). A liver biopsy is performed and a photomicrograph after periodic acid-Schiff-staining is shown. Which of the following is the most likely additional finding in this patient?
Practice by Chapter
Viral hepatitis (A, B, C, D, E)
Practice Questions
Alcoholic liver disease
Practice Questions
Non-alcoholic fatty liver disease
Practice Questions
Drug-induced liver injury
Practice Questions
Autoimmune hepatitis
Practice Questions
Cirrhosis management
Practice Questions
Portal hypertension complications
Practice Questions
Ascites diagnosis and management
Practice Questions
Hepatic encephalopathy
Practice Questions
Spontaneous bacterial peritonitis
Practice Questions
Hepatorenal syndrome
Practice Questions
Hepatocellular carcinoma
Practice Questions
Liver transplantation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
