Liver disease — MCQs

On this page
A 45-year-old homeless man is brought to the emergency department by the police. He was found intoxicated and passed out in a library. The patient has a past medical history of IV drug abuse, diabetes, alcohol abuse, and malnutrition. The patient has been hospitalized previously for multiple episodes of pancreatitis and sepsis. Currently, the patient is minimally responsive and only withdraws his extremities in response to painful stimuli. His temperature is 99.5°F (37.5°C), blood pressure is 90/48 mmHg, pulse is 150/min, respirations are 17/min, and oxygen saturation is 95% on room air. Physical exam is notable for tachycardia, a diastolic murmur at the left lower sternal border, and bilateral crackles on pulmonary exam. The patient is started on IV fluids, vancomycin, and piperacillin-tazobactam. Laboratory values are ordered as seen below. Hemoglobin: 9 g/dL Hematocrit: 30% Leukocyte count: 11,500/mm^3 with normal differential Platelet count: 297,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.0 mEq/L HCO3-: 28 mEq/L BUN: 33 mg/dL Glucose: 60 mg/dL Creatinine: 1.7 mg/dL Ca2+: 9.7 mg/dL PT: 20 seconds aPTT: 60 seconds AST: 1,010 U/L ALT: 950 U/L The patient is admitted to the medical floor. Five days later, the patient's neurological status has improved. His temperature is 99.5°F (37.5°C), blood pressure is 130/90 mmHg, pulse is 90/min, respirations are 11/min, and oxygen saturation is 99% on room air. Laboratory values are repeated as seen below. Hemoglobin: 10 g/dL Hematocrit: 32% Leukocyte count: 9,500/mm^3 with normal differential Platelet count: 199,000/mm^3 Serum: Na+: 140 mEq/L Cl-: 102 mEq/L K+: 4.3 mEq/L HCO3-: 24 mEq/L BUN: 31 mg/dL Glucose: 100 mg/dL Creatinine: 1.6 mg/dL Ca2+: 9.0 mg/dL PT: 40 seconds aPTT: 90 seconds AST: 150 U/L ALT: 90 U/L Which of the following is the best description of this patient’s current status?
A 17-year-old man presents to his primary care physician with a bilateral tremor of the hands. He is a senior in high school and during the year, his grades have plummeted to the point that he is failing. He says his memory is now poor, and he has trouble focusing on tasks. His behavior has changed in the past 6 months, in that he has frequent episodes of depression, separated by episodes of bizarre behavior, including excessive alcohol drinking and shoplifting. His parents have started to suspect that he is using street drugs, which he denies. His handwriting has become very sloppy. His parents have noted slight slurring of his speech. Family history is irrelevant. Physical examination reveals upper extremity tremors, mild dystonia of the upper extremities, and mild incoordination involving his hands. The patient’s eye is shown. Which of the following best represents the etiology of this patient illness?
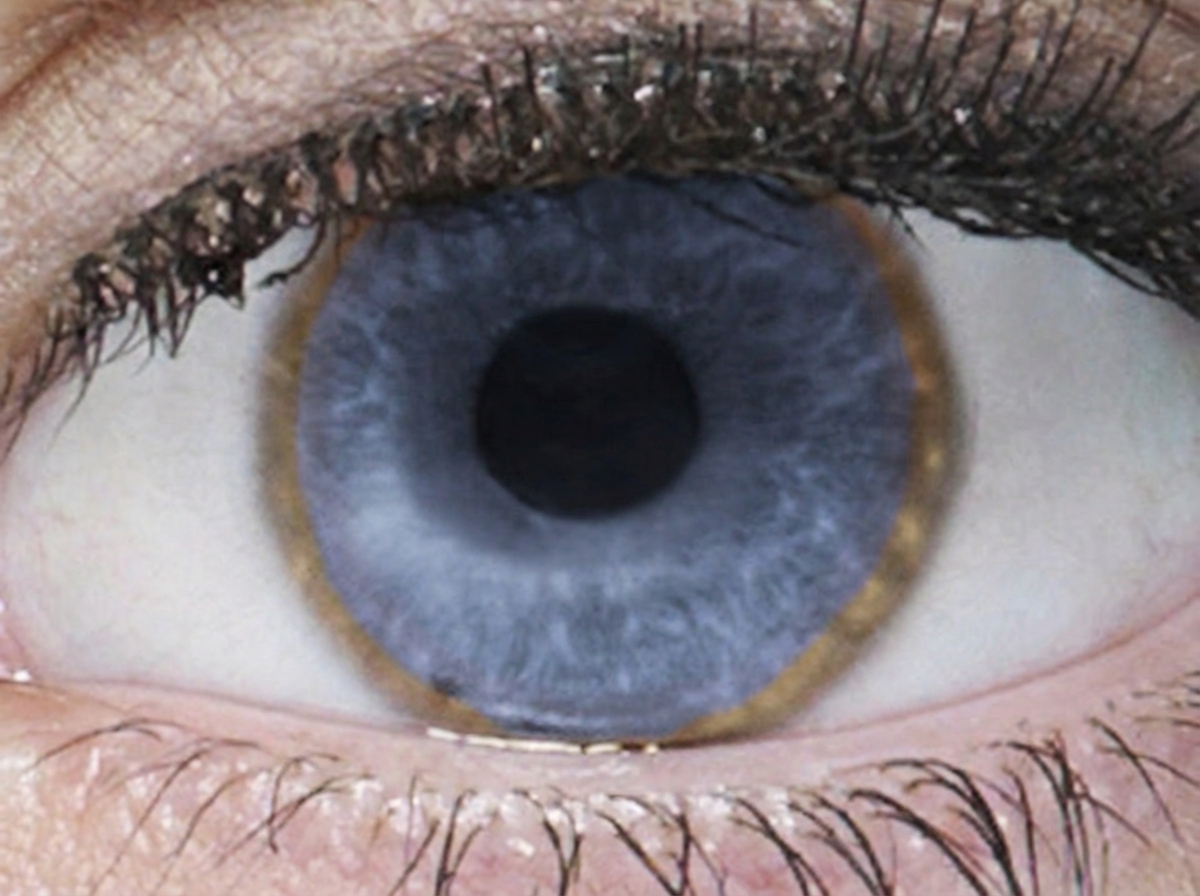
A 48-year-old man with a history of diabetes mellitus presents to his primary care physician with lethargy, joint pain, and impotence. Lab evaluation is notable for a ferritin of 1400 ug/L (nl <300 ug/L), increased total iron, increased transferrin saturation, and decreased total iron binding capacity. All of the following are true regarding this patient's condition EXCEPT:
A 71-year-old woman comes to the physician because of an 8-month history of fatigue. Laboratory studies show a hemoglobin concentration of 13.3 g/dL, a serum creatinine concentration of 0.9 mg/dL, and a serum alkaline phosphatase concentration of 100 U/L. Laboratory evaluation of which of the following parameters would be most helpful in determining the cause of this patient's symptoms?
A 47-year-old woman comes to the physician because of a 3-week history of generalized fatigue, mild fever, abdominal pain, and nausea. She attended the state fair over a month ago, where she tried a number of regional foods, and wonders if it might have been caused by something she ate. She has also noticed darkening of her urine, which she attributes to not drinking enough water recently. She has type 2 diabetes mellitus. She drinks 1–2 beers daily. She works as nursing assistant in a rehabilitation facility. Current medications include glyburide, sitagliptin, and a multivitamin. She appears tired. Her temperature is 38.1°C (100.6°F), pulse is 99/min, and blood pressure is 110/74 mm Hg. Examination shows mild scleral icterus. The liver is palpated 2–3 cm below the right costal margin and is tender. Laboratory studies show: Hemoglobin 10.6 g/dL Leukocyte count 11600/mm3 Platelet count 221,000/mm3 Serum Urea nitrogen 26 mg/dL Glucose 122 mg/dL Creatinine 1.3 mg/dL Bilirubin 3.6 mg/dL Total 3.6 mg/dL Direct 2.4 mg/dL Alkaline phosphatase 72 U/L AST 488 U/L ALT 798 U/L Hepatitis A IgG antibody (HAV-IgG) positive Hepatitis B surface antigen (HBsAg) positive Hepatitis B core IgG antibody (anti-HBc) positive Hepatitis B envelope antigen (HBeAg) positive Hepatitis C antibody (anti-HCV) negative Which of the following is the most likely diagnosis?
A 32-year-old woman comes to the emergency department for a 2-week history of right upper quadrant abdominal pain. She has also been feeling tired and nauseous for the past 5 weeks. She has a history of depression and suicidal ideation. She is a social worker for an international charity foundation. She used intravenous illicit drugs in the past but quit 4 months ago. Her only medication is sertraline. Her temperature is 37.8°C (100.0°F), pulse is 100/min, and blood pressure is 128/76 mm Hg. She is alert and oriented. Scleral icterus is present. Abdominal examination shows tenderness to palpation in the right upper quadrant. The liver edge is palpated 3 cm below the right costal margin. There is no rebound tenderness or guarding. The abdomen is non-distended and the fluid wave test is negative. She is able to extend her arms with wrists in full extension and hold them steady without flapping. Laboratory studies show: Hemoglobin 13.8 g/dL Leukocytes 13,700/mm3 Platelets 165,000/mm3 Prothrombin time 14 seconds Partial thromboplastin time 35 seconds Serum: Total bilirubin 4.8 mg/dL Direct bilirubin 1.3 mg/dL Aspartate aminotransferase 1852 U/L Alanine aminotransferase 2497 U/L Urea nitrogen 21 mg/dL Creatinine 1.2 mg/dL Hepatitis A IgM antibody Negative Hepatitis B surface antigen Negative Hepatitis B surface antibody Negative Hepatitis B core IgM antibody Positive Hepatitis C antibody Positive Hepatitis C RNA Negative Urine beta-hCG Negative Which of the following is the most appropriate next step in management?
A 53-year-old woman presents to your office with several months of fatigue and abdominal pain. The pain is dull in character and unrelated to meals. She has a history of type 2 diabetes mellitus and rheumatoid arthritis for which she is taking ibuprofen, methotrexate, and metformin. She has 2-3 drinks on the weekends and does not use tobacco products. On physical examination, there is mild tenderness to palpation in the right upper quadrant. The liver span is 15 cm at the midclavicular line. Laboratory results are as follows: Serum: Na+: 135 mEq/L Cl-: 100 mEq/L K+: 3.7 mEq/L HCO3-: 24 mEq/L BUN: 13 mg/dL Creatinine: 1.0 mg/dL Alkaline phosphatase: 100 U/L AST: 70 U/L ALT: 120 U/L Bilirubin (total): 0.5 mg/dL Bilirubin (conjugated): 0.1 mg/dL Amylase: 76 U/L What is the most likely cause of her clinical presentation?
A 44-year-old man comes to the physician because of a 2-week history of lower extremity swelling and frothy urine. He has a history of chronic hepatitis C infection. Physical examination shows 3+ pitting edema of the lower legs and ankles. Further evaluation of this patient is most likely to show which of the following?
A 71-year-old man is brought to the emergency department by his daughter after she found him to be extremely confused at home. She says that he appeared to be fine in the morning; however, upon returning home, she found that he was slumped in his chair and was hard to arouse. She was worried that he may have taken too many medications and rushed him to the emergency department. His past medical history is significant for bipolar disorder and absence seizures. He does not smoke and drinks 4 alcoholic beverages per night on average. On physical exam, he is found to have a flapping tremor of his hands, pitting ankle edema, and gynecomastia. He does not appear to have any focal neurologic deficits. Which of the following lab findings would most likely be seen in this patient?
A 20-year-old man, who was previously healthy, is taken to the emergency department due to agitation during the past 24 hours. During the past week, his family members noticed a yellowish coloring of his skin and eyes. He occasionally uses cocaine and ecstasy, and he drinks alcohol (about 20 g) on weekends. The patient also admits to high-risk sexual behavior and does not use appropriate protection. Physical examination shows heart rate of 94/min, respiratory rate of 13/min, temperature of 37.0°C (98.6°F), and blood pressure of 110/60 mm Hg. The patient shows psychomotor agitation, and he is not oriented to time and space. Other findings include asterixis, jaundice on the skin and mucous membranes, and epistaxis. The rest of the physical examination is normal. The laboratory tests show: Hemoglobin 16.3 g/dL Hematocrit 47% Leukocyte count 9,750/mm3 Neutrophils 58% Bands 2% Eosinophils 1% Basophils 0% Lymphocytes 24% Monocytes 2% Platelet count 365,000/mm3 Bilirubin 25 mg/dL AST 600 IU/L ALT 650 IU/L TP activity < 40% INR 1.5 What is the most likely diagnosis?
Practice by Chapter
Viral hepatitis (A, B, C, D, E)
Practice Questions
Alcoholic liver disease
Practice Questions
Non-alcoholic fatty liver disease
Practice Questions
Drug-induced liver injury
Practice Questions
Autoimmune hepatitis
Practice Questions
Cirrhosis management
Practice Questions
Portal hypertension complications
Practice Questions
Ascites diagnosis and management
Practice Questions
Hepatic encephalopathy
Practice Questions
Spontaneous bacterial peritonitis
Practice Questions
Hepatorenal syndrome
Practice Questions
Hepatocellular carcinoma
Practice Questions
Liver transplantation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
