Liver disease — MCQs

On this page
A 25-year-old man presents to the office for a 3-day history of fever and fatigue. Upon further questioning, he says that he also had constant muscular pain, headaches, and fever during these days. He adds additional information by giving a history of regular unprotected sexual relationship with multiple partners. He is a non-smoker and drinks alcohol occasionally. The heart rate is 102/min, respiratory rate is 18/min, temperature is 38.0°C (100.4°F), and blood pressure is 120/80 mm Hg. On physical examination, he is icteric and hepatosplenomegaly is evident with diffuse muscular and abdominal tenderness particularly in the right upper quadrant. The serologic markers show the following pattern: Anti-HAV IgM negative HBsAg positive Anti-HBs negative IgM anti-HBc positive Anti-HCV negative Anti-HDV negative What is the most likely diagnosis?
A 35-year-old man presents with erectile dysfunction. Past medical history is significant for diabetes mellitus diagnosed 5 years ago, managed with insulin, and for donating blood 6 months ago. The patient denies any history of smoking or alcohol use. He is afebrile, and his vital signs are within normal limits. Physical examination shows a bronze-colored hyperpigmentation on the dorsal side of the arms bilaterally. Nocturnal penile tumescence is negative. Routine basic laboratory tests are significant for a moderate increase in glycosylated hemoglobin and hepatic enzymes. Which of the following is the most likely diagnosis in this patient?
A 46-year-old man comes to the clinic complaining of abdominal pain for the past month. The pain comes and goes and is the most prominent after meals. He reports 1-2 episodes of black stools in the past month, a 10-lbs weight loss, fevers, and a skin rash on his left arm. A review of systems is negative for any recent travel, abnormal ingestion, palpitations, nausea/vomiting, diarrhea, or constipation. Family history is significant for a cousin who had liver failure in his forties. His past medical history is unremarkable. He is sexually active with multiple partners and uses condoms intermittently. He admits to 1-2 drinks every month and used to smoke socially during his teenage years. His laboratory values are shown below: Serum: Na+: 138 mEq/L Cl-: 98 mEq/L K+: 3.8 mEq/L HCO3-: 26 mEq/L BUN: 10 mg/dL Glucose: 140 mg/dL Creatinine: 2.1 mg/dL Thyroid-stimulating hormone: 3.5 µU/mL Ca2+: 10 mg/dL AST: 53 U/L ALT: 35 U/L HBsAg: Positive Anti-HBc: Positive IgM anti-HBc: Positive Anti-HBs: Negative What findings would you expect to find in this patient?
A 54-year-old man with known end-stage liver disease from alcoholic cirrhosis presents to the emergency department with decreased urinary output and swelling in his lower extremities. His disease has been complicated by ascites and hepatic encephalopathy in the past. Initial laboratory studies show a creatinine of 1.73 mg/dL up from a previous value of 1.12 one month prior. There have been no new medication changes, and no recent procedures performed. A diagnostic paracentesis is performed that is negative for infection, and he is admitted to the hospital for further management and initiated on albumin. Two days later, his creatinine has risen to 2.34 and he is oliguric. Which of the following is the most definitive treatment for this patient's condition?
A 62-year-old man is brought to the emergency department for the evaluation of intermittent bloody vomiting for the past 2 hours. He has had similar episodes during the last 6 months that usually stop spontaneously within an hour. The patient is not aware of any medical problems. He has smoked one pack of cigarettes daily for 30 years but quit 10 years ago. He drinks half a liter of vodka daily. He appears pale and diaphoretic. His temperature is 37.3°C (99.1°F), pulse is 100/min, respirations are 20/min, and blood pressure is 105/68 mm Hg. Cardiac examination shows no murmurs, rubs, or gallops. There is increased abdominal girth. On percussion of the abdomen, the fluid-air level shifts when the patient moves from the supine to the right lateral decubitus position. The edge of the liver is palpated 2 cm below the costal margin. His hemoglobin concentration is 10.3 g/dL, leukocyte count is 4,200/mm3, and platelet count is 124,000/mm3. Intravenous fluids and octreotide are started. Which of the following is the most appropriate next step in the management of this patient?
A 47-year-old man is brought to the emergency department by police. He was forcibly removed from a bar for lewd behavior. The patient smells of alcohol, and his speech is slurred and unintelligible. The patient has a past medical history of alcohol abuse, obesity, diabetes, and Wernicke encephalopathy. The patient's currently prescribed medications include insulin, metformin, disulfiram, atorvastatin, a multi-B-vitamin, and lisinopril; however, he is non-compliant with his medications. His temperature is 98.5°F (36.7°C), blood pressure is 150/97 mmHg, pulse is 100/min, respirations are 15/min, and oxygen saturation is 96% on room air. Physical exam is notable for a palpable liver edge 2 cm inferior to the rib cage and increased abdominal girth with a positive fluid wave. Laboratory values are ordered and return as below: Hemoglobin: 10 g/dL Hematocrit: 33% Leukocyte count: 7,500 cells/mm^3 with normal differential Platelet count: 245,000/mm^3 Serum: Na+: 136 mEq/L Cl-: 102 mEq/L K+: 4.1 mEq/L HCO3-: 24 mEq/L BUN: 24 mg/dL Glucose: 157 mg/dL Creatinine: 1.5 mg/dL Ca2+: 9.6 mg/dL Which of the following are the most likely laboratory values that would be seen in this patient in terms of aspartate aminotransferase (AST), alanine aminotransferase (ALT) and gamma-glutamyl transferase (GGT) (in U/L)?
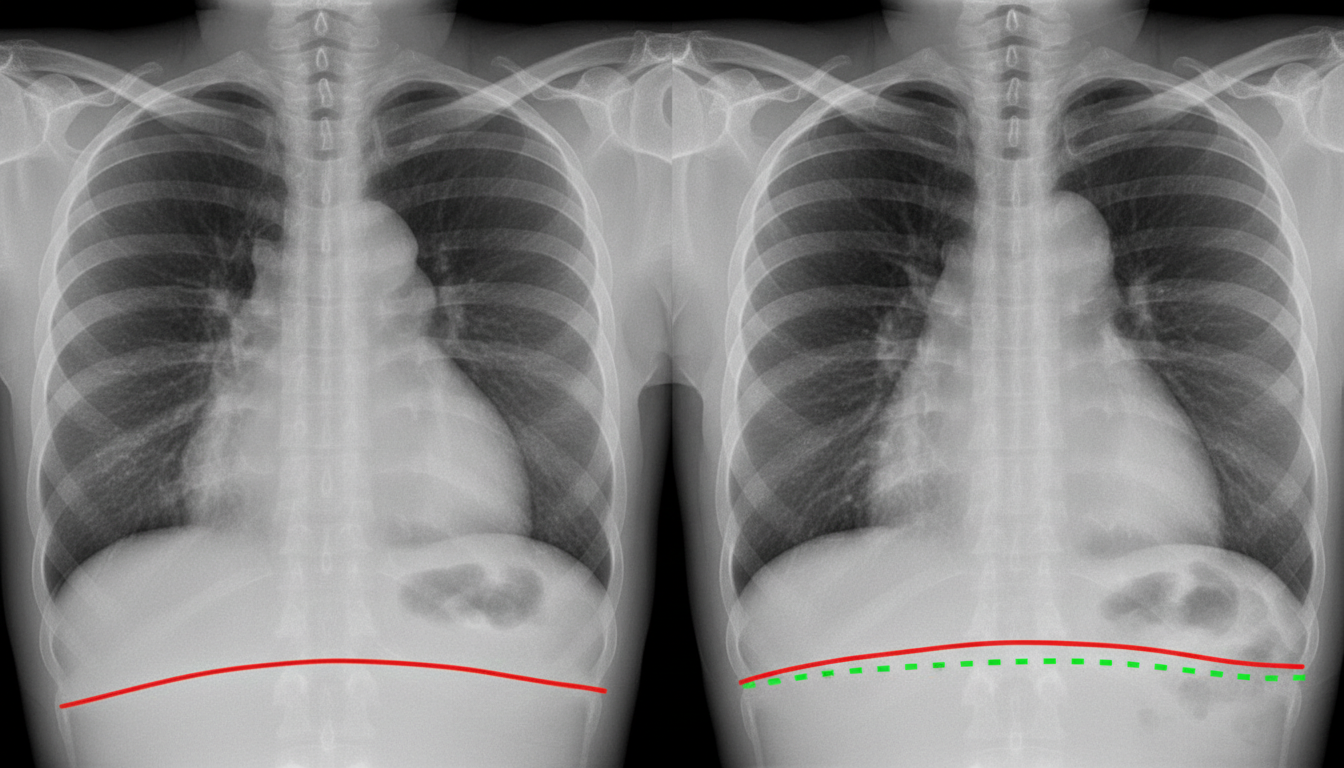
A 28-year-old patient presents to the hospital complaining of progressively worsening dyspnea and a dry cough. Radiographic imaging is shown below. Pulmonary function testing (PFT's) reveals a decreased FEV1 and FEV1/FVC, but an increased TLC. The patient states that he does not smoke. Which of the following conditions is most consistent with the patient's symptoms?
A 44-year-old woman presents to the emergency department with jaundice and diffuse abdominal pain. She denies any previous medical problems and says she does not take any medications, drugs, or supplements. Her temperature is 97.6°F (36.4°C), blood pressure is 133/87 mmHg, pulse is 86/min, respirations are 22/min, and oxygen saturation is 100% on room air. Physical exam is notable for sclera which are icteric and there is tenderness to palpation over the right upper quadrant. Laboratory studies are ordered as seen below. Hepatitis B surface antigen: Positive Hepatitis B surface antibody: Negative Hepatitis B core antibody IgM: Negative Hepatitis B core antibody IgG: Positive Hepatitis B E antigen: Positive Hepatitis B E antibody (anti-HBe): Negative Which of the following is the most likely diagnosis?
A 22-year-old student presents to the college health clinic with a 1-week history of fever, sore throat, nausea, and fatigue. He could hardly get out of bed this morning. There are no pets at home. He admits to having recent unprotected sex. The vital signs include: temperature 38.3°C (101.0°F), pulse 72/min, blood pressure 118/63 mm Hg, and respiratory rate 15/min. On physical examination, he has bilateral posterior cervical lymphadenopathy, exudates over the palatine tonsil walls with soft palate petechiae, an erythematous macular rash on the trunk and arms, and mild hepatosplenomegaly. What is the most likely diagnosis?
A 45-year-old man is brought to the physician for a follow-up examination. Three weeks ago, he was hospitalized and treated for spontaneous bacterial peritonitis. He has alcoholic liver cirrhosis and hypothyroidism. His current medications include spironolactone, lactulose, levothyroxine, trimethoprim-sulfamethoxazole, and furosemide. He appears ill. His temperature is 36.8°C (98.2°F), pulse is 77/min, and blood pressure is 106/68 mm Hg. He is oriented to place and person only. Examination shows scleral icterus and jaundice. There is 3+ pedal edema and reddening of the palms bilaterally. Breast tissue appears enlarged, and several telangiectasias are visible over the chest and back. Abdominal examination shows dilated tortuous veins. On percussion of the abdomen, the fluid-air level shifts when the patient moves from lying supine to right lateral decubitus. Breath sounds are decreased over both lung bases. Cardiac examination shows no abnormalities. Bilateral tremor is seen when the wrists are extended. Genital examination shows reduced testicular volume of both testes. Digital rectal examination and proctoscopy show hemorrhoids. Which of the following potential complications of this patient's condition is the best indication for the placement of a transjugular intrahepatic portosystemic shunt (TIPS)?
Practice by Chapter
Viral hepatitis (A, B, C, D, E)
Practice Questions
Alcoholic liver disease
Practice Questions
Non-alcoholic fatty liver disease
Practice Questions
Drug-induced liver injury
Practice Questions
Autoimmune hepatitis
Practice Questions
Cirrhosis management
Practice Questions
Portal hypertension complications
Practice Questions
Ascites diagnosis and management
Practice Questions
Hepatic encephalopathy
Practice Questions
Spontaneous bacterial peritonitis
Practice Questions
Hepatorenal syndrome
Practice Questions
Hepatocellular carcinoma
Practice Questions
Liver transplantation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
